Abstract
Paracaval-originating cancers have been considered a contraindication for laparoscopic liver resection (LLR). This study aimed to explore the safety and feasibility of LLR in the treatment of paracaval-originating cancers. This study included 11 patients who underwent LLR and 20 who underwent open liver resection (OLR) for paracaval-originating cancers between May 2010 and November 2020. The outcomes of the procedures were retrospectively analyzed. There were no cases of perioperative death or conversion to laparotomy. The LLR group had an earlier postoperative feeding time, shorter postoperative hospital stay, and lower total bilirubin levels on the first day after surgery. No significant differences in the incidence of overall postoperative complications were noted between the LLR and OLR groups, but the incidence of grade IIIa complications was significantly higher in the LLR group than in the OLR group. Tumor recurrence occurred in 4 of 11 patients in the LLR group and in 11 of 20 patients in the OLR group. LLR for the treatment of paracaval-originating cancers is safe and feasible in selected patients.
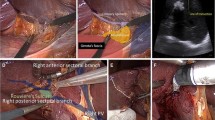
Graphic abstract


Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Kumon M (2017) Anatomical study of the caudate lobe with special reference to portal venous and biliary branches using corrosion liver casts and clinical application. Liver Cancer 6:161–170. https://doi.org/10.1159/000454682
Tuxun T, Aini A, Li YP, Apaer S, Zhang H, Li T, Aji T, Yimiti Y, Zhao JM, Shao YM, Wen H (2016) Systematic review of feasibility, safety and efficacy of ex situ liver resection and autotransplantation. Zhonghua Yi Xue Za Zhi 96:2251–2257. https://doi.org/10.3760/cma.j.issn.0376-2491.2016.28.011
Baker MA, Maley WR, Needleman L, Doria C (2015) Ex vivo resection of hepatic neoplasia and autotransplantation: a case report and review of the literature. J Gastrointest Surg 19:1169–1176. https://doi.org/10.1007/s11605-015-2806-3
Buell JF, Cherqui D, Geller DA, O’Rourke N, Iannitti D, Dagher I et al (2009) World consensus conference on laparoscopic surgery. The international position on laparoscopic liver surgery: the Louisville statement, 2008. Ann Surg 250:825–830. https://doi.org/10.1097/sla.0b013e3181b3b2d8
Fiorentini G, Ratti F, Cipriani F, Catena M, Paganelli M, Aldrighetti L (2018) Tips and tricks for a laparoscopic approach to paracaval liver segments. Ann Surg Oncol 25:1695–1698. https://doi.org/10.1245/s10434-018-6432-7
Liu F, Wei Y, Li B (2019) Laparoscopic isolated total caudate lobectomy for hepatocellular carcinoma located in the paracaval portion of the cirrhotic liver. Ann Surg Oncol 26:2980. https://doi.org/10.1245/s10434-019-07461-1
Iwashita Y, Uchida H, Endo Y, Yada K, Mori T, Ohta M, Inomata M (2016) Laparoscopic caudal approach for a small hepatocellular carcinoma located in the paracaval portion of a cirrhotic liver. Asian J Endosc Surg 9:204–207. https://doi.org/10.1111/ases.12273
Yoon YS, Han HS, Cho JY, Kim JH, Kwon Y (2013) Laparoscopic liver resection for centrally located tumors close to the hilum, major hepatic veins, or inferior vena cava. Surgery 153:502–509. https://doi.org/10.1016/j.surg.2012.10.004
Strasberg SM (2005) Nomenclature of hepatic anatomy and resections: a review of the Brisbane 2000 system. J Hepat Pancreat Surg 12:351–355. https://doi.org/10.1007/s00534-005-0999-7
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213. https://doi.org/10.1097/01.sla.0000133083.54934.ae
Nishigaki Y, Tomita E, Hayashi H, Suzuki Y, Iritani S, Kato T, Yamada T (2013) Efficacy and safety of radiofrequency ablation for hepatocellular carcinoma in the caudate lobe of the liver. Hepatol Res 43:467–474. https://doi.org/10.1111/j.1872-034X.2012.01095.x
Shibata T, Maetani Y, Ametani F, Kubo T, Itoh K, Konishi J (2002) Efficacy of nonsurgical treatments for hepatocellular carcinoma in the caudate lobe. Cardiovasc Interv Radiol 25:186–192. https://doi.org/10.1007/s00270-001-0111-x
Shimada M, Matsumata T, Maeda T, Yanaga K, Taketomi A, Sugimachi K (1994) Characteristics of hepatocellular carcinoma originating in the caudate lobe. Hepatology 19:911–915
Ishizawa T, Gumbs AA, Kokudo N, Gayet B (2012) Laparoscopic segmentectomy of the liver: from segment I to VIII. Ann Surg 256:959–964. https://doi.org/10.1097/SLA.0b013e31825ffed3
Afaneh C, Kluger MD (2013) Laparoscopic liver resection: lessons at the end of the second decade. Semin Liver Dis 33:226–235. https://doi.org/10.1055/s-0033-1351780
Schmelzle M, Krenzien F, Schöning W, Pratschke J (2020) Laparoscopic liver resection: indications, limitations, and economic aspects. Langenbecks Arch Surg 405:725–735. https://doi.org/10.1007/s00423-020-01918-8
Wang ZG, Lau W, Fu SY, Liu H, Pan ZY, Yang Y, Zhang J, Wu MC, Zhou WP (2015) Anterior hepatic parenchymal transection for complete caudate lobectomy to treat liver cancer situated in or involving the paracaval portion of the caudate lobe. J Gastrointest Surg 19:880–886. https://doi.org/10.1007/s11605-015-2793-4
Matsui Y, Terakawa N, Satoi S, Kaibori M, Kitade H, Takai S, Kwon AH, Kamiyama Y (2007) Postoperative outcomes in patients with hepatocellular carcinomas resected with exposure of the tumor surface: clinical role of the no-margin resection. Arch Surg 142:596–602. https://doi.org/10.1001/archsurg.142.7.596
Sakamoto Y, Nara S, Hata S, Yamamoto Y, Esaki M, Shimada K, Kosuge T (2011) Prognosis of patients undergoing hepatectomy for solitary hepatocellular carcinoma originating in the caudate lobe. Surgery 150:959–967. https://doi.org/10.1016/j.surg.2011.03.005
Lai EC, Ng IO, Ng MM, Lok AS, Tam PC, Fan ST, Choi TK, Wong J (1990) Long-term results of resection for large hepatocellular carcinoma: a multivariate analysis of clinicopathological features. Hepatology 11:815–818. https://doi.org/10.1002/hep.1840110516
Lockwood DS, Yeadon TM, Clouston AD, Crawford DG, Fawcett J, Callaghan SA, Gotley DC (2003) Tumor progression in hepatocellular carcinoma: relationship with tumor stroma and parenchymal disease. J Gastroenterol Hepatol 18:666–672. https://doi.org/10.1046/j.1440-1746.2003.03018.x
Ng IO, Lai EC, Fan ST, Ng MM, So MK (1995) Prognostic significance of pathologic features of hepatocellular carcinoma. A multivariate analysis of 278 patients. Cancer 76:2443–2448. https://doi.org/10.1002/1097-0142(19951215)76:12%3c2443::aid-cncr2820761207%3e3.0.co;2-f
Zervantonakis IK, Hughes-Alford SK, Charest JL, Condeelis JS, Gertler FB, Kamm RD (2012) Three-dimensional microfluidic model for tumor cell intravasation and endothelial barrier function. Proc Natl Acad Sci USA 109:13515–13520. https://doi.org/10.1073/pnas.1210182109
Yu W, Wang W, Rong W, Wang L, Xu Q, Wu F, Liu L, Wu J (2014) Adjuvant radiotherapy in centrally located hepatocellular carcinomas after hepatectomy with narrow margin (<1 cm): a prospective randomized study. J Am Coll Surg 218:381–392. https://doi.org/10.1016/j.jamcollsurg.2013.11.030
Qiu J, Wu H, Bai Y, Xu Y, Zhou J, Yuan H, Chen S, He Z, Zeng Y (2013) Mesohepatectomy for centrally located liver tumours. Br J Surg 100:1620–1626. https://doi.org/10.1002/bjs.9286
Fang C, An J, Bruno A et al (2020) Consensus recommendations of three-dimensional visualization for diagnosis and management of liver diseases. Hepatol Int 14:437–453. https://doi.org/10.1007/s12072-020-10052-y
Kaneko T, Kaneko K, Sugimoto H, Inoue S, Hatsuno T, Sawada K, Ando H, Nakao A (2000) Intrahepatic anastomosis formation between the hepatic veins in the graft liver of the living related liver transplantation: observation by Doppler ultrasonography. Transplantation 70:982–985. https://doi.org/10.1097/00007890-200009270-00018
Billingsley KG, Jarnagin WR, Fong Y, Blumgart LH (1998) Segment-oriented hepatic resection in the management of malignant neoplasms of the liver. J Am Coll Surg 187:471–481. https://doi.org/10.1016/s1072-7515(98)00231-2
Funding
This work was supported by Technology Innovation Project Foundation for Key Areas of the First Affiliated Hospital, Army Medical University, China (No. SWH2016ZDCX2015) and National Natural Science Foundation of China (81972303).
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection, and analysis were performed by SZ, TS, XW, and LC. The first draft of the manuscript was written by TS and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Ethical approval
The study was approved by the ethics committee of the Southwest Hospital of Army Medical University (KY2020125).
Informed consent
All patients signed informed consent forms before participating in the study.
Consent for publication
All patients agreed to have their clinical data published for scientific research.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Sun, T., Wang, X., Cao, L. et al. Laparoscopic liver resection for primary liver cancers originating in the paracaval portion of the caudate lobe: a preliminary retrospective analysis with 31 patients. Updates Surg 74, 547–555 (2022). https://doi.org/10.1007/s13304-021-01170-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13304-021-01170-9