Abstract
Background
In areas without convenient access to dermatology care, primary care providers (PCPs) serve as an important patient resource for early skin cancer detection. To determine the most effective strategy for skin cancer detection training in PCPs, we conducted a systematic review of educational interventions and performed a meta-analysis on sensitivity and specificity outcomes in PCPs.
Objectives
To summarize data on skin cancer sensitivity and specificity outcomes for PCP-targeted training programs and diagnostic algorithms. Our PCP cohort included practicing physicians, trainee physicians, and advanced practice practitioners.
Methods
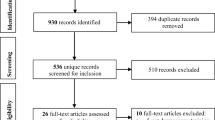
A literature search was performed in MEDLINE, Embase, Web of Science, and the Cochrane Library for relevant English-language articles published worldwide from 2000 onward. Results were screened for eligibility, and overlapping datasets were reconciled. Data extracted included the educational intervention, diagnostic algorithm, and outcomes of interest (sensitivity and specificity). Outcomes were pooled across interventions that taught the same diagnostic algorithm. A bivariate model was fit to compare different interventions/algorithms. This review followed the PRISMA guidelines.
Results
In total, 21 articles were included in this review, encompassing over 58,610 assessments of skin lesions by about 1529 participants worldwide. Training programs that implemented the triage-amalgamated dermoscopic algorithm (TADA) demonstrated high pooled sensitivity (91.7%) and high pooled specificity (81.4%) among PCPs.
Conclusions and Relevance
Overall, this systematic review and meta-analysis showed that dermoscopy training in PCPs was generally associated with gains in skin cancer sensitivity without loss of specificity. Clinically, this correlates with fewer skin cancers overlooked by PCPs and fewer excisions of benign lesions.


Similar content being viewed by others
Data Availability
All data compiled and analyzed in this review has been made available to the reader.
Change history
27 August 2022
A Correction to this paper has been published: https://doi.org/10.1007/s13187-022-02217-0
References
US Department of Health and Human Services (2014) The surgeon general’s call to action to prevent skin cancer. Office of the Surgeon General (US), Washington (DC). Skin cancer as a major public health problem. Available from: https://www.ncbi.nlm.nih.gov/books/NBK247164/
Rogers HW, Weinstock MA, Feldman SR, Coldiron BM (2015) Incidence estimate of nonmelanoma skin cancer (keratinocyte carcinomas) in the U.S. population, 2012. JAMA Dermatol 151(10):1081–1086. https://doi.org/10.1001/jamadermatol.2015.1187
Siegel RL, Miller KD, Fuchs HE, Jemal A (2022) Cancer statistics, 2022. CA Cancer J Clin 72(1):7–33. https://doi.org/10.3322/caac.21708
Guy GP Jr, Machlin SR, Ekwueme DU, Yabroff KR (2015) Prevalence and costs of skin cancer treatment in the US, 2002–2006 and 2007–2011. Am J Prev Med 48(2):183–187. https://doi.org/10.1016/j.amepre.2014.08.036
Apalla Z, Lallas A, Sotiriou E, Lazaridou E, Ioannides D (2017) Epidemiological trends in skin cancer. Dermatol pract conceptual 7(2):1–6. https://doi.org/10.5826/dpc.0702a01
Howlader NNAM, Noone AM, Krapcho ME, Miller D, Brest A, Yu ME, Ruhl J, Tatalovich Z, Mariotto A, Lewis DR, Chen HS (2019) SEER cancer statistics review, 1975–2016. National Cancer Institute, p 1
Vaidya T, Zubritsky L, Alikhan A, Housholder A (2018) Socioeconomic and geographic barriers to dermatology care in urban and rural US populations. J Am Acad Dermatol 78(2):406–408. https://doi.org/10.1016/j.jaad.2017.07.050
Alghothani L, Jacks SK, Vander Horst A, Zirwas MJ (2012) Disparities in access to dermatologic care according to insurance type. Arch Dermatol 148(8):956–957. https://doi.org/10.1001/archdermatol.2012.804
Nelson KC, Swetter SM, Saboda K, Chen SC, Curiel-Lewandrowski C (2019) Evaluation of the number-needed-to-biopsy metric for the diagnosis of cutaneous melanoma: a systematic review and meta-analysis. JAMA Dermatol 155(10):1167–1174. https://doi.org/10.1001/jamadermatol.2019.1514
Perera E, Xu C, Manoharan S (2012) Real-life teledermatology cases. In: Soyer H, Binder M, Smith A, Wurm E (eds) Telemedicine in Dermatology. Springer, Berlin, Heidelberg. https://doi.org/10.1007/978-3-642-20801-0_15
Moore MM, Geller AC, Zhang Z et al (2006) Skin cancer examination teaching in US medical education. Arch Dermatol 142(4):439–444. https://doi.org/10.1001/archderm.142.4.439
Moher D, Liberati A, Tetzlaff J, Altman DG (2009) Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. BMJ 339:b2535. https://doi.org/10.1136/bmj.b2535
Ouzzani M, Hammady H, Fedorowicz Z, Elmagarmid A (2016) Rayyan—a web and mobile app for systematic reviews. Syst Rev 5(210):10. https://doi.org/10.1186/s13643-016-0384-4
Reitsma JB, Glas AS, Rutjes AW, Scholten RJ, Bossuyt PM, Zwinderman AH (2005) Bivariate analysis of sensitivity and specificity produces informative summary measures in diagnostic reviews. J Clin Epidemiol 58(10):982–990. https://doi.org/10.1016/j.jclinepi.2005.02.022
Harkemanne E, Baeck M, Tromme I (2021) Training general practitioners in melanoma diagnosis: A scoping review of the literature. BMJ Open 11(3):e043926. https://doi.org/10.1136/bmjopen-2020-043926
Najmi M, Brown AE, Harrington SR, Farris D, Sepulveda S, Nelson KC (2021) A systematic review and synthesis of qualitative and quantitative studies evaluating provider, patient, and health care system-related barriers to diagnostic skin cancer examinations. Arch Dermatol Res. https://doi.org/10.1007/s00403-021-02224-z
Bourne P, Rosendahl C, Keir J, Cameron A (2012) BLINCK-A diagnostic algorithm for skin cancer diagnosis combining clinical features with dermatoscopy findings. Dermatol Pract Conceptual 2(2):202a12. https://doi.org/10.5826/dpc.0202a12
Argenziano G, Puig S, Zalaudek I et al (2006) Dermoscopy improves accuracy of primary care physicians to triage lesions suggestive of skin cancer. J Clin Oncol 24(12):1877–1882. https://doi.org/10.1200/jco.2005.05.0864
Koelink CJ, Vermeulen KM, Kollen BJ et al (2014) Diagnostic accuracy and cost-effectiveness of dermoscopy in primary care: A cluster randomized clinical trial. J Eur Acad Dermatol Venereol 28(11):1442–1449. https://doi.org/10.1111/jdv.12306
Westerhoff K, McCarthy WH, Menzies SW (2000) Increase in the sensitivity for melanoma diagnosis by primary care physicians using skin surface microscopy. Br J Dermatol 143(5):1016–1020. https://doi.org/10.1046/j.1365-2133.2000.03836.x
Seiverling E, Ahrns H, Stevens K et al (2021) Dermoscopic lotus of learning: implementation and dissemination of a multimodal dermoscopy curriculum for primary care. Short Report. J Med Educ Curric Dev 8:1–4. https://doi.org/10.1177/2382120521989983
Susong JR, Ahrns HT, Daugherty A, Marghoob AA, Seiverling EV (2020) Evaluation of a virtual basic dermatology curriculum for dermoscopy by using the triage amalgamated dermoscopic algorithm for novice dermoscopists. J Am Acad Dermatol 83(2):590–592. https://doi.org/10.1016/j.jaad.2019.05.097
Rogers T, Marino ML, Dusza SW et al (2016) A clinical aid for detecting skin cancer: the triage amalgamated dermoscopic algorithm (TADA). J Am Board Fam Med 29(6):694–701. https://doi.org/10.3122/jabfm.2016.06.160079
Sawyers EA, Wigle DT, Marghoob AA, Blum A (2020) Dermoscopy training effect on diagnostic accuracy of skin lesions in Canadian family medicine physicians using the triage amalgamated dermoscopic algorithm. Dermatol Pract Conceptual 10(2):e2020035. https://doi.org/10.5826/dpc.1002a35
De Bedout V, Williams NM, Muñoz AM et al (2021) Skin cancer and dermoscopy training for primary care physicians: A pilot study. Dermatol Pract Conceptual 11(1):e2021145. https://doi.org/10.5826/dpc.1101a145
Bandic J, Kovacevic S, Karabeg R, Lazarov A, Opric D (2020) Teledermoscopy for skin cancer prevention: a comparative study of clinical and teledermoscopic diagnosis. Acta Informatica Medica 28(1):37–41. https://doi.org/10.5455/aim.2020.28.37-41
Secker LJ, Buis PA, Bergman W, Kukutsch NA (2017) Effect of a dermoscopy training course on the accuracy of primary care physicians in diagnosing pigmented lesions. Acta Derm Venereol 97(2):263–265. https://doi.org/10.2340/00015555-2526
Harkemanne E, Goublomme N, Sawadogo K, Tromme I (2020) Early melanoma detection in primary care: clinical recognition of melanoma is not enough, one must also learn the basics [online ahead of print]. J Cancer Educ. https://doi.org/10.1007/s13187-020-01897-w
Eide MJ, Asgari MM, Fletcher SW et al (2013) Effects on skills and practice from a web-based skin cancer course for primary care providers. J Am Board Fam Med 26(6):648–657. https://doi.org/10.3122/jabfm.2013.06.130108
Orfaly VE, Berry EG, Stoos ER et al (2021) Melanoma toolkit for early detection for primary care providers: a pilot study. Pigment Cell Melanoma Res 34(5):984–986. https://doi.org/10.1111/pcmr.12968
Beecher SM, Keogh C, Healy C (2018) Dedicated general practitioner education sessions can improve diagnostic capabilities and may have a positive effect on referral patterns for common skin lesions. Ir J Med Sci 187(4):959–963. https://doi.org/10.1007/s11845-018-1788-z
Badertscher N, Braun RP, Held U et al (2013) Diagnostic competence of Swiss general practitioners in skin cancer. Swiss Med Wkly 143:w13834. https://doi.org/10.4414/smw.2013.13834
Carli P, De Giorgi V, Crocetti E, Caldini L, Ressel C, Giannotti B (2005) Diagnostic and referral accuracy of family doctors in melanoma screening: effect of a short formal training. Eur J Cancer Prev 14(1):51–55. https://doi.org/10.1097/00008469-200502000-00007
Brochez L, Verhaeghe E, Bleyen L, Naeyaert JM (2001) Diagnostic ability of general practitioners and dermatologists in discriminating pigmented skin lesions. J Am Acad Dermatol 44(6):979–986. https://doi.org/10.1067/mjd.2001.113442
Bedlow AJ, Cliff S, Melia J, Moss SM, Seyan R, Harland CC (2000) Impact of skin cancer education on general practitioners’ diagnostic skills. Clin Exp Dermatol 25(2):115–118. https://doi.org/10.1046/j.1365-2230.2000.00590.x
Harris JM, Salasche SJ, Harris RB (2001) Can Internet-based continuing medical education improve physicians’ skin cancer knowledge and skills? J Gen Intern Med 16(1):50–56. https://doi.org/10.1111/j.1525-1497.2001.00615.x
Oliveria SA, Nehal KS, Christos PJ, Sharma N, Tromberg JS, Halpern AC (2001) Using nurse practitioners for skin cancer screening: a pilot study. Am J Prev Med 21(3):214–217. https://doi.org/10.1016/s0749-3797(01)00354-3
Prasad S, Black S, Chen HW et al (2022) Beliefs and barriers to care of primary care practitioners toward melanoma screening and education in rural Texas. J Am Acad Dermatol. https://doi.org/10.1016/j.jaad.2021.12.059
Pagnanelli G, Soyer HP, Argenziano G et al (2003) Diagnosis of pigmented skin lesions by dermoscopy: web-based training improves diagnostic performance of non-experts. Br J Dermatol 148(4):698–702. https://doi.org/10.1046/j.1365-2133.2003.05168.x
Herschorn A (2012) Dermoscopy for melanoma detection in family practice. Can Fam Physician 58(7):740-5-e372-8
Argenziano G, Puig S, Zalaudek I et al (2006) Dermoscopy improves accuracy of primary care physicians to triage lesions suggestive of skin cancer. J Clin Oncol 24(12):1877–1882. https://doi.org/10.1200/jco.2005.05.0864
Funding
This work is supported in part by the generous philanthropic contributions of the Lyda Hill Foundation to The University of Texas MD Anderson Cancer Center Moon Shots Program™. This work is also supported in part by a National Cancer Institute (NCI) Cancer Center Support Grant (Award No. P30 CA016672). The funding sources were not involved in the design or conduct of the study; the collection, management, analysis, or interpretation of the data; the preparation, review, or approval of the manuscript; or the decision to submit the manuscript for publication.
Author information
Authors and Affiliations
Contributions
KCN, NG, and TT contributed to the study conceptualization and design. Literature search was performed by KCN, DPF, NG, and TT. Study selection and data collection were performed by TT, NG, and KCN. Data analysis was performed by RLB, TT, and KCN. The first draft of the manuscript was written by TT and NG, and all authors commented on previous versions of the manuscript. All authors reviewed and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics Approval
This is a secondary review of literature which has been published. Ethics approval was not required.
Consent to Participate
This review of published literature did not directly involve any human subjects. In this study, informed consent was not required.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Ms. Nadeen Gonna and Ms. Tiffaney Tran shared co-first authorship.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Gonna, N., Tran, T., Bassett, R.L. et al. Sensitivity and Specificity for Skin Cancer Diagnosis in Primary Care Providers: a Systematic Literature Review and Meta-analysis of Educational Interventions and Diagnostic Algorithms. J Canc Educ 37, 1563–1572 (2022). https://doi.org/10.1007/s13187-022-02194-4
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13187-022-02194-4