Abstract
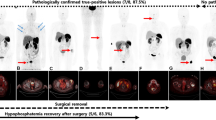
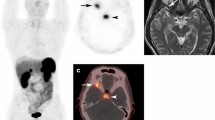
Tumour-induced osteomalacia is a rare paraneoplastic syndrome that manifests as chronic hypophosphataemia, non-specific bone pain and muscle weakness. It is generally caused by phosphaturic mesenchymal tumour (PMT), which is uncommonly associated with synchronous tumours. However, diagnosis is often delayed for several years due to the rarity, indolent growing nature and non-specific symptoms of the disease, often resulting in an overlook by clinicians during assessments. The patient initially presented with hypophosphataemia and generalised skeletal pain with multiple atraumatic fractures. Blood tests revealed serum calcium levels at the upper limit and extremely low inorganic phosphate levels. Herein, we report a case where two synchronous PMTs from two different sites were detected by ‘extended’ whole-body Ga-68 DOTATATE PET-CT, leading to remission of the disease after complete surgical removal. Early detection and diagnosis of PMT neoplasm is crucial, as complete surgical resection of this tumour is the only definitive treatment currently known. Upon excision, this curable disease will result in complete resolution of symptoms and blood parameters, leading to remission of the disease which significantly improves the patient’s quality of life. PMT often over-expresses somatostatin receptors (SSTR), predominantly subtype 2A, and Ga-68 DOTATATE PET-CT is a selective SSTR imaging that targets this characteristic over-expression in these tumours. The high diagnostic accuracy of Ga-68 DOTATATE PET-CT should be the primary imaging modality for full evaluation of this disease.


Similar content being viewed by others
References
Dadoniene J, Miglinas M, Miltiniene D, Vajauskas D, Seinin D, Butenas P, et al. Tumour-induced osteomalacia: a literature review and a case report. World J Surg Oncol. 2016;14:4.
Mc CR. Osteomalacia with Looser’s nodes (Milkman’s syndrome) due to a raised resistance to vitamin D acquired about the age of 15 years. Q J Med. 1947;16:33–46.
Ogose A, Hotta T, Emura I, Hatano H, Inoue Y, Umezu H, et al. Recurrent malignant variant of phosphaturic mesenchymal tumor with oncogenic osteomalacia. Skeletal Radiol. 2001;30:99–103.
Ghorbani-Aghbolaghi A, Darrow MA, Wang T. Phosphaturic mesenchymal tumor (PMT): exceptionally rare disease, yet crucial not to miss. Autops Case Rep. 2017;7:32–7.
Minisola S, Peacock M, Fukumoto S, Cipriani C, Pepe J, Tella SH, et al. Tumour-induced osteomalacia. Nat Rev Dis Primers. 2017;3:17044.
Tang D, Wang XM, Zhang YS, Mi XX. Oncogenic osteomalacia caused by a phosphaturic mesenchymal tumor of the femur: A case report. World J Clin Cases. 2019;7:2081–6.
Endo I, Fukumoto S, Ozono K, Namba N, Inoue D, Okazaki R, et al. Nationwide survey of fibroblast growth factor 23 (FGF23)-related hypophosphatemic diseases in Japan: prevalence, biochemical data and treatment. Endocr J. 2015;62:811–6.
Wu H, Bui MM, Zhou L, Li D, Zhang H, Zhong D. Phosphaturic mesenchymal tumor with an admixture of epithelial and mesenchymal elements in the jaws: clinicopathological and immunohistochemical analysis of 22 cases with literature review. Mod Pathol. 2019;32:189–204.
Ding J, Wang L, Zhang S, Li F, Huo L. Recurrent/Residual Intracranial Phosphaturic Mesenchymal Tumor Revealed on 68Ga-DOTATATE PET/CT. Clin Nucl Med. 2018;43:674–5.
Evans DJ, Azzopardi JG. Distinctive tumours of bone and soft tissue causing acquired vitamin-D-resistant osteomalacia. Lancet. 1972;1:353–4.
Weidner N, Santa Cruz D. Phosphaturicmesenchymal tumors. A polymorphous group causing osteomalacia or rickets. Cancer. 1987;59:1442–54.
Chong WH, Molinolo AA, Chen CC, Collins MT. Tumor-induced osteomalacia. Endocr Relat Cancer. 2011;18:R53-77.
Higley M, Beckett B, Schmahmann S, Dacey E, Foss E. Locally aggressive and multifocal phosphaturic mesenchymal tumors: two unusual cases of tumor-induced osteomalacia. Skeletal Radiol. 2015;44:1825–31.
Shenbaghavalli T, Harshavardhan JKG, Menon PG. A Rare Case of Phosphaturic Tumor/Oncogenic Osteomalacia - Diagnostic Challenges and Management Algorithm. J Orthop Case Rep. 2019;9:49–52.
Dutta D, Pandey RK, Gogoi R, Solanki N, Madan R, Mondal A, et al. Occult phosphaturic mesenchymal tumour of femur cortex causing oncogenic osteomalacia - diagnostic challenges and clinical outcomes. Endokrynol Pol. 2018;69:205–10.
Carpenter TO. Primary Disorders of Phosphate Metabolism. In: Feingold KR, Anawalt B, Boyce A, Chrousos G, Dungan K, Grossman A, et al., editors. Endotext[Internet]. South Dartmouth (MA): MDText.com, Inc.; 2000. https://www.ncbi.nlm.nih.gov/sites/books/NBK279172/?report=classic. Accessed 16 Jun 2020.
Marcucci G, Brandi ML. Congenital Conditions of Hypophosphatemia Expressed in Adults. Calcif Tissue Int. 2020. https://doi.org/10.1007/s00223-020-00695-2.
Bhattacharyya N, Chong WH, Gafni RI, Collins MT. Fibroblast growth factor 23: state of the field and future directions. Trends Endocrinol Metab. 2012;23:610–8.
Broski SM, Folpe AL, Wenger DE. Imaging features of phosphaturic mesenchymal tumors. Skeletal Radiol. 2019;48:119–27.
Singh D, Chopra A, Ravina M, Kongara S, Bhatia E, Kumar N, et al. Oncogenic osteomalacia: role of Ga-68 DOTANOC PET/CT scan in identifying the culprit lesion and its management. Br J Radiol. 2017;90:20160811.
Houang M, Clarkson A, Sioson L, Elston MS, Clifton-Bligh RJ, Dray M, et al. Phosphaturic mesenchymal tumors show positive staining for somatostatin receptor 2A (SSTR2A). Hum Pathol. 2013;44:2711–8.
Jan de Beur SM, Streeten EA, Civelek AC, McCarthy EF, Uribe L, Marx SJ, et al. Localisation of mesenchymaltumours by somatostatin receptor imaging. Lancet. 2002;359:761–3.
Ding J, Hu G, Wang L, Li F, Huo L. Increased Activity Due to Fractures Does Not Significantly Affect the Accuracy of 68Ga-DOTATATE PET/CT in the Detection of Culprit Tumor in the Evaluation of Tumor-Induced Osteomalacia. Clin Nucl Med. 2018;43:880–6.
El-Maouche D, Sadowski SM, Papadakis GZ, Guthrie L, Cottle-Delisle C, Merkel R, et al. (68)Ga-DOTATATE for Tumor Localization in Tumor-Induced Osteomalacia. J Clin Endocrinol Metab. 2016;101:3575–81.
Ho CL. Ga68-DOTA Peptide PET/CT to Detect Occult Mesenchymal Tumor-Inducing Osteomalacia: A Case Series of Three Patients. Nucl Med Mol Imaging. 2015;49:231–6.
Jadhav S, Kasaliwal R, Lele V, Rangarajan V, Chandra P, Shah H, et al. Functional imaging in primary tumour-induced osteomalacia: relative performance of FDG PET/CT vs somatostatin receptor-based functional scans: a series of nine patients. Clin Endocrinol (Oxf). 2014;81:31–7.
John JR, Hephzibah J, Oommen R, Shanthly N, Mathew D. Ga-68 DOTATATE Positron Emission Tomography-Computed Tomography Imaging in Oncogenic Osteomalacia: Experience from a Tertiary Level Hospital in South India. Indian J Nucl Med. 2019;34:188–93.
Paquet M, Gauthe M, Zhang Yin J, Nataf V, Belissant O, Orcel P, et al. Diagnostic performance and impact on patient management of (68)Ga-DOTA-TOC PET/CT for detecting osteomalacia-associated tumours. Eur J Nucl Med Mol Imaging. 2018;45:1710–20.
Zhang J, Zhu Z, Zhong D, Dang Y, Xing H, Du Y, et al. 68Ga DOTATATE PET/CT is an Accurate Imaging Modality in the Detection of Culprit Tumors Causing Osteomalacia. Clin Nucl Med. 2015;40:642–6.
Zhang S, Wang L, Wang T, Xing HQ, Huo L, Li F. [Value of (68)Ga-DOTA-TATE Positron Emission Tomography/Computed Tomography in the Localization of Culprit Tumors Causing Osteomalacia with Negative (99m)Tc-HYNIC-TOC Single Photo Emission Computed Tomography]. Zhongguo Yi XueKeXue Yuan XueBao. 2018;40:757–64.
Meyer M, Nicod Lalonde M, Testart N, Jreige M, Kamani C, Boughdad S, et al. Detection Rate of Culprit Tumors Causing Osteomalacia Using Somatostatin Receptor PET/CT: Systematic Review and Meta-Analysis. Diagnostics (Basel). 2019;10:2.
Kumar S, Diamond T. Lessons learnt from delayed diagnosis of FGF-23-producing tumour-induced osteomalacia and post-operative hungry bone syndrome. Bone Rep. 2020;12:100276.
Florenzano P, Gafni RI, Collins MT. Tumor-induced osteomalacia Bone Rep. 2017;7:90–7.
Ha S, Park S, Kim H, Go H, Lee SH, Choi JY, et al. Successful Localization Using (68)Ga-DOTATOC PET/CT of a Phosphaturic Mesenchymal Tumor Causing Osteomalacia in a Patient with Concurrent Follicular Lymphoma. Nucl Med Mol Imaging. 2018;52:462–7.
Annamalai AK, Sampathkumar K, Kane S, Shetty NS, Kulkarni S, Rangarajan V, et al. Needle(s) in the Haystack-Synchronous Multifocal Tumor-Induced Osteomalacia. J Clin Endocrinol Metab. 2016;101:390–3.
Acknowledgements
None.
Funding
This study was supported by funding from both Sunway Medical Centre and Sunway University (Funding No.: GRTEX-OTR-CBP-SMC-002–2019).
Author information
Authors and Affiliations
Contributions
Teik Hin Tan: Conceptualization and design; funding acquisition; analysis and interpretation of data; writing – review and revision; final approval of version for publication.
Ew-Jun Chen: Investigation; data acquisition and analysis; data curation; writing – original draft, review and editing.
Ming Tsuey Chew: Funding acquisition; investigation; writing – article draft, review and editing; final approval of version for publication.
Ping Ching Chye: Acquisition and interpretation of data; review of writing.
Ming Wong: Acquisition, interpretation and analysis of data; review of writing; final approval.
Corresponding author
Ethics declarations
Conflict of Interest
Teik Hin Tan, Ew-Jun Chen, Ming Tsuey Chew, Ping Ching Chye and Ming Wong declare that they have no conflict of interest.
Ethical Approval
All procedures performed in this study involving human participants were in accordance with the ethical standards of the institutional research committee and with the Helsinki declaration as revised in 2013 and its later amendments or comparable ethical standards.
Informed Consent
The institutional review board of our institute approved this retrospective study, and the requirement to obtain informed consent was waived.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Tan, T.H., Chen, EJ., Chew, M.T. et al. Extended Whole-body Ga-68 DOTATATE PET-CT in evaluating Tumour-Induced Osteomalacia: Case report and review of literature. Nucl Med Mol Imaging 55, 130–135 (2021). https://doi.org/10.1007/s13139-021-00695-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13139-021-00695-6