Abstract
Insulin and insulin-like growth factor (IGF) signaling systems regulate breast cancer growth, progression, and metastasis. The insulin receptor substrates 1 and 2 (IRS1/2) transduce signaling from the type I IGF receptor (IGF-IR) and insulin receptor (InR) to mediate the biological effects of receptor activation. In breast cancer, IRS-1 plays a critical role in cancer cell proliferation while IRS-2 is associated with motility and metastasis. NT157, a small-molecule tyrphostin, downregulates IRS proteins in several model systems. In breast cancer cells, NT157 treatment suppressed IRS protein expression in a dose-dependent manner. Exposure to NT157 inhibited the activation of downstream signaling mediated by the IRS proteins. NT157 induced a MAPK-dependent serine phosphorylation of IRS proteins which resulted in disassociation between IRS proteins and their receptors resulting in IRS degradation. In estrogen receptor-α-positive (ERα+) breast cancer cells (MCF-7 and T47D), NT157 also resulted in cytoplasmic ERα downregulation likely because of disruption of an IRS-1-IGF-IR/InR/ERα complex. NT157 decreased S phase fraction, monolayer, and anchorage-independent growth after IGF/insulin treatment in ERα+ breast cancer cells. NT157 downregulation of IRS protein expression also sensitized ERα+ breast cancer cells to rapamycin. Moreover, NT157 inhibited the growth of tamoxifen-resistant ERα+ breast cancer cells. Given that both IGF-IR and InR play a role in cancer biology, targeting of IRS adaptor proteins may be a more effective strategy to inhibit the function of these receptors.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The insulin-like growth factor (IGF)/insulin signaling pathway has been implicated in the proliferation, migration, and survival of many human malignancies [1, 2]. Upon ligand binding, the type I IGF receptor (IGF-IR) and insulin receptor (InR) recruit the insulin receptor substrate (IRS) adaptor proteins to transduce signals to downstream signaling molecules and thereby regulate cellular biology. In breast cancers, IRS-1 and IRS-2 are the two major isoforms that mediate IGF/insulin signaling. The role of IRS-1/2 proteins in breast malignancies has been well documented: IRS-1 promotes tumor growth [3, 4], whereas IRS-2 stimulates motility [3, 5, 6].
The clinical trials for targeting IGF-IR have generally been disappointing. While several factors may account for the limited clinical activity, the disruption of endocrine homeostasis with resultant hyperinsulinemia could abrogate the effect of only inhibiting IGF-IR [7]. Recent clinical trials results show InR is more commonly expressed in endocrine-resistant breast cancer [8], while expression of IGF-IR is quite low. These data argue strongly that both IGF-IR and InR should be inhibited in breast cancer yet targeting of InR could be difficult due to accomplish because of effects on glucose homeostasis. However, targeting key signaling pathways downstream of both receptors, such as the IRS proteins, has appeal and could be another strategy for cancer treatment.
NT157 is a novel small-molecule tyrphostin targeting the IRS-1/2 proteins. Its efficacy and mechanism of action have been studied in models of melanoma [9] and prostate cancer in vitro and in vivo [10]. NT157 binds IGF-1R and indirectly downregulates IRS-1/2 proteins expressions by inducing the serine phosphorylation sites of these proteins, which sequentially causes the degradation and reduction of ligand-stimulated intracellular signaling activation, as well as suppression of cancer cell growth and metastasis. Recent data show NT157 also influences p38 MAPK and AXL [11] function in melanoma cells.
In our current study, we verify that NT157 caused IRS protein degradation by inducing serine phosphorylation of IRS and disassociation from IGF-IR and InR in breast cancer cells. We report a new mechanism of NT157 drug in estrogen receptor-positive (ERα+) breast cancer cell lines. Phosphorylation of IRS-1 induced by NT157 promoted the dissociation of ERα from IRS-1-IGF-IR/InR complex resulting in ERα degradation. We assess the efficacy of NT157 by characterizing its effects on onco-signaling suppression, growth inhibition, cell cycle arrest, and abolishment of migratory potential using various breast cancer subtypes. We also investigate the synergic therapeutic effects of NT157 in combination with rapamycin in treating breast cancer cells. Since NT157 inhibited IGF-IR and InR signaling, substrate inhibition may be exploited as a cancer therapy.
Materials and Methods
Reagents and Antibodies
Growth media and supplements were purchased from Invitrogen (Grand Island, NY). IGF-I was purchased from GroPep (Adelaide, Australia). IGF-II was purchased from Gemini (Woodland, CA). Insulin was purchased from Eli Lilly (Indianapolis, IN). LY294002, U0126, and actin antibody were purchased from Sigma-Aldrich (St. Louis, MO). Humanized anti-IGF-IR monoclonal antibody huEM164 was provided by Immunogen Inc. (Norwood, MA). BMS-754807 was provided by Bristol Myers Squibb (New Jersey, Marco Gottardis). Antibodies for phosphorylated AKT serine 473, total and phospho-IGF-IR, total and phosphorylated p44/42 (MAPK), phospho-p38 MAPK, total and phospho-IRS-1 (serine 636/639), phospho-S6K1, p21, p18, CDK2, CDK6, cyclin D1, cyclin D3, and PARP were purchased from Cell Signaling Technology (Beverly, MA). The IRS-2, total ERα, IGF-IRα, InRβ antibodies, and protein agarose A were purchased from Santa Cruz Biotechnology (Santa Cruz, CA). Horseradish peroxidase-conjugated anti-phosphotyrosine (PY-20) was purchased from BD Biosciences (San Jose, CA). Anti-rabbit and anti-mouse horseradish peroxidase-conjugated secondary antibodies were purchased from Pierce (Rockford, IL). NT157 compound was kindly provided by A. Levitzki (The Hebrew University of Jerusalem, Israel).
Cell Lines and Culture
MCF-7, T47D, and MDA-MB-231 cells were purchased from the ATCC (Manassas, VA) and cultured following ATCC’s instruction. Cell line authenticity is verified by STR analysis on an annual basis (Genetics Resources Core Facility, Johns Hopkins School of Medicine, Institute of Genetic Medicine). MCF-7L cells were kindly provided by C. Kent Osborne (Baylor College of Medicine) and maintained in improved MEM Richter’s modification medium (zinc option) supplemented with 5% FBS and 11.25 nmol/L insulin. MCF-7L were evaluated by comparative genomic hybridization (data not shown) and found to be nearly identical to the MCF-7 cells distributed by the ATCC. MCF-7L TamR and T47D TamR cells were generated as described [12]. All cells were grown at 37 °C in a humidified atmosphere containing 5% CO2.
Immunoblot
Cells were plated at a density of 3 × 105 in 60-mm diameter. Upon reaching 80% confluency, cells were switched to serum-free medium (SFM) for 24 h to synchronize cell status, after which treatments were added. Treated cells were washed twice with ice-cold phosphate buffered saline (PBS) on ice and lysed with TNESV lysis buffer of 50 mM Tris-Cl (pH 7.4), 1% Nonidet P-40, 2 mM EDTA (pH 8.0), 100 mM NaCl, 10 mM sodium orthovanadate, 1 mM phenylmethysulforny fluoride, and with proteases inhibitor cocktails. Lysates were centrifuged at 21,000 rpm for 30 min at 4 °C. Protein concentrations were measured using the bicinchoninic acid protein assay reagent kit (Pierce). Cellular protein (80 μg) was resuspended in 5× Laemmli loading buffer with 60 mg/ml DTT and was resolved by SDS-PAGE, transferred to nitrocellulose membrane, and immunoblotted according to manufacturer guidelines.
Immunoprecipitation
Total cellular lysates (500 μg) were incubated overnight with IGF-IRα or InRβ antibody at 4 °C followed by incubation with protein agarose A for 4 h at 4 °C. Samples were washed three times with TNESV buffer. 5× Laemmli loading buffer was added per immunoprecipitated sample and run on an 8% SDS-PAGE gel.
siRNA Transfection and Cell Stimulation
Cells were cultured in growth medium to reach confluency of 80% then were transfected with 25 nmol/L siRNA (siRNAs SMARTpool were purchased from Santa Cruz Biotechnology) using the TransIT-siQUEST transfection reagent (Mirus, Madison, WI) according to the manufacturer’s protocol. Forty-eight hours later, cells were washed twice with PBS and serum starved for another 24 h in SFM followed by treatments as indicated in the figure legends.
Reverse Transcription-Quantitative Real-Time Polymerase Chain Reaction
Cells were plated at a density of 2 × 105 in 6-well plates in growth media to reach 80% confluency then synchronized in SFM for 24 h followed by treatments indicated in the figure legends. Cellular RNA was isolated using TriPure Reagent according to the manufacturer (Roche, Belgium). For quality control and to determine concentration, a 260:280 ratio assay was conducted on a spectrophotometer. Forward and reverse primers were designed to target the following transcripts: IRS-1 5′-TCACAGCAGAATGAAGACC-3′ and 5′-CTACTGATGAGGAAGATATGAGG-3′; IRS-2 5′-TCGTGAAAGAGTGAAGATCTG-3′ and 5′-TCCAAACACAGTCATTGCT-3′; ESR1 5′-CCCAGGGAAGCTACTGTTTG-3′ and 5′-CTCCACCATGCCCTCTACAC-3′; CCND1 5′-AAACAGATCATCCGCAAACAC-3′ and 5′-GGTTCAGGCCTTGCACTG-3′; P21 5′-CAGGGGAGCAGGCTGAAG-3′ and 5′-GGATTAGGGCTTCCTCTTGG-3′; and RPLPO 5′-TGCTGATGGGCAAGAACAC-3′ and 5′-GAACACAAAGCCCACATTCC-3′. A total of 1 μg of RNA was reverse transcribed using the Transcriptor Reverse Transcriptase Kit, and quantitative PCR was conducted using the Universal SYBR Green Kit according to the manufacturer’s protocol (Roche) on an Eppendorf (Hamburg, Germany) Mastercycler Realplex4 machine. The relative concentration of mRNA was calculated using cycle threshold values that were derived from a standard curve and normalized to ribosomal protein, large, PO (RPLPO) as an internal control.
Monolayer Growth Assay
Cells were plated in 24-well plates at a density of 15,000 cells per well, allowed to attach overnight and starved in SFM for 24 h to synchronize cells. After 5 days of treatments, growth was assessed via the 3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide (MTT) assay. Fifty microliters of 5 mg/ml MTT solution in SFM were added to each well and incubated for 4 h at 37 °C. Media were aspirated, and formazan crystals were lysed with 500 μl of solubilization solution (95% dimethylsulfoxide + 5% improved minimal essential media). Absorbance was measured with a plate reader at 570 nm using a 650-nm differential filter to assess growth.
Anchorage-Independent Growth
A 1 ml layer of 1% Seaplaque-agarose (BioWhittaker, Rockland, ME) in 1.5% FBS-containing growth media was solidified into each well of a 6-well plate. The bottom layer was overlaid with 1 ml of a 1% top agar mixture for 12,000 cells per well with indicated treatments. All plates were incubated at 37 °C for 14 days. Colonies was counted on a light microscope with an ocular grid. Five random fields were counted per well and only colonies exceeding half of a grid square were scored.
Cell Cycle Analysis
Cells were typsinized, washed twice in ice-cold PBS, and fixed in 70% ice-cold ethanol − 20 °C overnight. Cell cycle analyses were performed on propidium iodide-stained nuclei by using an Accuri™ C6 flow cytometer (BD Biosciences, San Jose, CA). Single cells were gated, 10,000 events were collected and analyzed by FlowJo (Tree Star Inc., Ashland, OR) software.
Clinical Data Set Analysis
The relative mRNA expression of IRS-1 and IRS-2 in human breast tumor samples was determined by searching the Oncomine database (version 4.4.3, September 2012 data release. (www.oncomine.org) IRS-1 and IRS-2 mRNA expressions were queried in TCGA breast dataset using reporter A_32_P165472. For prognostic analyses, overall survival and distant metastasis-free survival, stratified by expression (all percentiles between the lower and upper quartiles were computed, and the best-performing threshold was used as a cutoff) of the gene of interest (IRS-1: 204686_s_at; IRS-2: 209184_s_at), were presented as Kaplan–Meier plots and tested for significance using log-rank tests. [13] TCGA BRCA RNASeqV2 and clinical patient data were downloaded on 7/1/2014. IRS-1, IRS-2, and ESR1 expression values were normalized by the expression of the housekeeping gene GAPDH. The Pearson correlations and linear regression were perfumed using R function cor and lm.
Statistical Analysis
All data except clinical data sets were analyzed with the unpaired Student’s t test with the use of Excel 2008 (Microsoft, Redmond, WA). A p value of < 0.05 was considered statistically significant (*p < 0.5, **p < 0.01, ***p < 0.001).
Results
NT157 Induced IRS Protein Degradation Through Serine Phosphorylation of IRS-1/2 in Multiple Breast Cancer Cell Lines
To evaluate the ability of NT157 to downregulate IRS-1 and IRS-2 proteins, breast cancer cell lines were incubated with increasing doses of NT157. NT157 reduced IRS1/2 levels while inducing serine phosphorylation of IRS-1/2 (serine 636/639). IGF-IRβ expression was not affected in both ERα+ and basal-like breast cancer cell lines (Fig. 1a top panels). NT157-induced IRS protein downregulation occurred after 4 h of drug exposure (Fig. S1). To evaluate the mechanism of IRS phosphorylation, cells were pretreated with small molecule inhibitors of downstream signaling pathways (Fig. 1a bottom panels). Only MEK inhibition by UO126 inhibited NT157’s ability to phosphorylate IRS proteins and partially rescued IRS protein levels. Inhibition of PI3K (LY294002) or IGF-IR (HuEM164 and BMS-754807) did not reverse the serine phosphorylation of IRS by NT157.
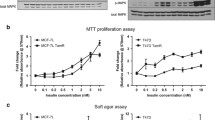
NT157 compound-induced IRS protein degradation through serine phosphorylation of IRS-1/2 in multiple breast cancer cell lines. a Top panels: MCF-7, T47D, and MDA-MB-231 cells were serum-starved overnight then treated with increasing concentrations of NT157 drug for 4 h. Cellular lysates were separated by SDS-PAGE and protein levels of IRS-1, IRS-2, phospho-serine IRS-1, IGF-IRβ, ERα, and actin were assessed by immunoblotting. Bottom panels: MCF-7, T47D, and MDA-MB-231 cells were serum-starved overnight then pretreated with huEM164 (164, 20 μg/ml, 24 h), BMS-754807 (BMS, 1 nM, 1 h), LY294002 (LY, 10 μM, 1 h), or UO126 (UO, 10 μM, 1 h). Protein levels of phospho-serine IRS1/2, phospho-SHC, and actin were determined by immunoblotting. b Top panels: expression analysis of IRS-1 and IRS-2 genes in TCGA breast cancer subtypes. Left: Box-whisker plot of IRS1 expression normalized to the housekeeping gene GAPDH in different breast cancer subtypes. Right: Box-whisker plots of normalized IRS-1 and IRS-2 expressions in ER-positive breast cancers. Bottom panel: scatter plot of ESR1 vs IRS-1 in ER-positive breast cancers. Straight line shows the best fit with a Pearson correlation factor of 0.3. c mRNA expressions of IRS-1 (left) and ESR1 (right) in a panel of breast cancer cell lines were determined by qRT-PCR. Data are mean ± SEM; all qRT-PCR results are representative of at least three independent triplicates experiments
NT157 Promoted Dissociation of IRS-1 and ERα with IGF-IR/InR in Breast Cancer Cells Resulting in IRS-1 and ERα Degradation
It has previously been shown that IRS-1 is an ERα+ target gene in breast cancer [14]. To study the relationship in available databases, Fig 1b shows that IRS-1 levels were higher in the ERα-positive tumors (luminal A and B) compared to ERα-negative breast cancers.
Since previous studies showed that IRS-1 and ERα formed a complex in the cytosol [15], we examined the effect of NT157 on ERα expression. In ERα+ cell lines, NT157 treatment downregulated total ERα expression (Fig. 1a top panels). Subcellular fractionation analysis further confirmed that NT157 specifically downregulated cytoplasmic ERα (Fig. 2a, left panel) in T47D cells. Ligand-induced ERα phosphorylation was also suppressed by NT157 treatment (Fig. 2a, right panel). Whether downregulation of ERα by NT157 further affected gene expression was then examined. After NT157 treatment, in ERα+ breast cancer cell lines, the ERα mRNA and mRNAs of two ERα-regulated genes IRS-1 [14, 16, 17] and CCND1 [15] were significantly suppressed (Fig. 2b, c), while non-ERα-regulated gene IRS-2 expression levels were not affected. In basal-like cell lines where ERα was not expressed, CCND1 and IRS-1 mRNA were not affected by NT157 (data not shown). To prove the mRNA level suppression was due to NT157’s effects on ERα, ERα+ breast cancer cells were transfected with both IRS-1 and IRS-2 siRNAs. Genetic downregulation of IRS proteins did not affect ERα mRNA or protein expression or ERα-regulated gene expression (Fig. S2) suggesting the possibility that NT157 resulted in ERα protein degradation by interfering with its interaction with IRS-1. Taken together, these data suggest that NT157’s predominant mechanism of action is stimulation of IRS protein degradation. However, the ability of NT157 to affect IRS-1 mRNA expression could also contribute to its biological effects.
NT157-induced ERα expression and function suppression. a Left panel: T47D cells were serum-starved overnight then treated with or without NT157 (3 μM) for 4 h. Cytoplasmic and nuclear ERα were extracted and assessed by immunoblotting. Right panel: MCF-7 and T47D cells were starved then pretreated with or without NT157 for 4 h following IGF-I (5 nM) stimulation for 15 min. Indicated protein levels were assessed by immunoblotting. b MCF-7 and T47D cells were serum-starved overnight then treated with or without 3 μM of NT157 drug for 4 h. Total RNA was isolated and reverse transcribed. IRS-1, IRS-2, and ESR1 levels were analyzed using qRT-PCR. Data were normalized to RPLP0 housekeeper gene. c MCF-7 cells were cultured in estrogen-depleted growth media for 2 days then serum-starved overnight. Cells were pretreated with NT157 (3 μM) for 4 h followed by 4 h of E2 (1 nM) stimulation. Total RNA was isolated and reverse transcribed. CCND1 levels were analyzed by qRT-PCR. Data were normalized to RPLP0 housekeeper gene. Data are mean ± SEM; results are representative of at least three independent triplicates experiments
IRS-1 protein forms complexes with IGF-IR/InR and ERα at the cell membrane [15] in normal mammary epithelial and breast cancer cell lines [18]. To determine if NT157 affected this complex, cell lysates were immunoprecipitated with IGF1R or InR antibodies. NT157 promoted the dissociation of IRS-1 from IGF-IR/IR as well as induced the dissociation of ERα from the IRS-1-IGF-IR/IR (Fig. 3a, left panel). Expression of IRS-1, ERα, and IGF-1R was similar in the full lysate regardless of NT157 treatment (Fig. 3a, right panel). The data above suggested a novel function of NT157 compound in ERα+ breast cancer cells.
NT157-induced dissociation of IGF-IR/IR and IRS-1-ERα complexes while not affecting major intracellular signaling cascades induced by short-term IGF-I treatment. a—Left panel: MCF-7 cells were serum-starved overnight then treated with indicated concentrations of NT157 drug for 2 h. 500 μg cellular protein was immunoprecipitated with IGF-IRα or InRβ. Protein levels of IRS-1 and ERα were determined by immunoblotting. Right panel: input to the immunoprecipitation was evaluated for IRS-1, IGF-1R, and ER after exposure of cells to 5 μM for 2 h. b MCF-7 cells were (1) serum-starved overnight, pretreated with 3 μM of NT157, then induced with or without 5 nM IGF-I for 10 min; (2) transfected by control or IRS1/2 siRNA for 48 h, starved overnight, then stimulated with or without 5 nM IGF-I. Protein levels of IRS-1, IRS-2, phospho-IGF-IR/IR, phospho-AKT, phospho-S6 K1, phospho-MAPK, and actin were assessed by immunoblotting
Downregulation of IRS Proteins in ERα+ Cancer Cells Does Not Affect Short-term IGF-I Treatment-Induced Signaling Transduction
In the presence of IGF-I, NT157 treatment eliminated the tyrosine phosphorylation of IRS1/2 (Fig. S3A) in response to IGF-I. Interestingly, neither downregulation of IRS proteins in ERα+ cells by NT157 treatment nor siRNA transfection attenuated activation of short-term IGF-I-induced signaling cascades (PI3K and MAPK) (Fig. 3b, S3B). Despite this lack of efficacy on signaling, data indicated that NT157 treatment suppressed cyclin D1 and induced p21 protein and mRNA expression in ERα+ breast cancer cell lines (Fig. 4a, b, and Fig. S4). Cyclin D1 is an estrogen-regulated gene, thus the degradation of ERα induced by NT157 reduced cyclin D1 expression. IGF-I-stimulated cyclin D1 was abolished by NT157 treatment in ERα+ cells (Fig. 4d). Downregulation of IRS proteins by siRNA did not affect IGF-I regulated cyclin D1 (Fig. S2A bottom panel), which indicated that suppression of IRS protein expression alone was not sufficient to inhibit IGF-I regulation of cyclin D1. NT157 disruption of the complex was required for maximal effect on cell cycle progression. Cell cycle analysis also revealed that NT157 treatment caused S phase arrest upon IGF/insulin system ligand stimulation (Fig. 4c). The unaltered upstream signaling pathway in ERα+ cancer cells may be due to compensation of other adaptor proteins, such as shc (Fig. 1a bottom panels and 4A).
NT157-inhibited cell cycle regulatory machinery. MCF-7 and T47D cells were serum-starved overnight then treated with indicated concentrations of NT157 for 4 h. a Protein levels of phospho-SHC, total-SHC, cyclin D1, p21, and actin were determined by immunoblotting. b Total RNA was isolated and reverse transcribed. CCND1 and p21 levels were analyzed using qRT-PCR. Data were normalized to RPLP0 housekeeper gene. c MCF-7 and T47D cells were serum-starved overnight, pretreated with or without 3 μM NT157, then induced with or without 5 nM IGF-I for 24 h. Cells were fixed then stained with propidum iodide. Cell cycle frequencies were determined by flow cytometry. d MCF-7 and T47D cells were serum-starved overnight, pretreated with or without 3 μM NT157 for 4 h, then stimulated with or without 5 nM IGF-I for 6 h. Protein levels of IRS-1, IRS-2, PARP, cyclin D1, p21, and actin were determined by immunoblotting. Data are mean ± SEM; results are representative of at least three independent triplicates experiments
NT157 Inhibited IGF/Insulin and 17β-Estradiol (E2) Induced Cell Proliferation in ERα+ Breast Cancer Cells
NT157 growth inhibitory effects in ERα+ breast cancer cell lines were further assessed. Both monolayer and anchorage-independent growth experiments showed that NT157 abolished IGF/insulin system ligands (IGF-I, IGF-II, and insulin) as well as E2-induced monolayer (Fig. 5a, S5B) and anchorage-independent growth (Fig. 5b). Moreover, parallel signaling experiments revealed that prolonged NT157 treatment resulted in suppressed PI3K signaling, decreased in total AKT level, downregulation of cyclin D1 expression, increased p21 expression, and enhanced activation of p38MAPK activation after ligand stimulation (Fig. 5c). Genetic suppression of IRS1/2 proteins also resulted in partial inhibition of ligand-induced growth (Fig. S6A) and attenuated PI3K pathway activation upon prolonged ligand stimulation but did not affect the cell cycle machinery (Fig. S6B). These data indicated that IRS proteins play a role in maintaining prolonged activation of PI3K pathway. NT157 treatment induced ERα degradation and further suppressed ligand stimulation of the cell cycle regulatory machinery in addition to IRS protein suppression. Therefore, NT157 inhibited ERα+ breast cancer cells by several different mechanisms and was more effective than genetic suppression methods.
NT157-inhibited IGF/insulin system ligand and E2-induced monolayer and anchorage-independent growth in ERα+ breast cancer cells. a MCF-7 and T47D were plated in 24-well plates, serum-starved overnight, and then treated with indicated treatments (IGF-I 5 nM, IGF-II 10 nM, insulin 10 nM, and E2 1 nM). Monolayer proliferation was evaluated using MTT assay, with results displayed as absorbance at 570 nm. b MCF-7 and T47D cells were serum-starved and treated with or without NT157 and ligands in 1% FBS in 0.45% agar and overlaid on 0.8% bottom agar. Colony growth in agarose was assessed after 14 days. Colonies formed were counted and averaged from 5 individual microscopic fields. Results displayed are the average number of colonies in 5 fields of 3 wells. c MCF-7 and T47D cells were serum-starved overnight, treated with or without NT157 and ligands for 24 h. Protein levels of IRS-1, IRS-2, phsopho-AKT, phospho-p38MAPK, cyclin D1, p21, and actin were determined by immunoblotting. Data are mean ± SEM; results are representative of at least three independent triplicates experiments
NT157 effects in two tamoxifen-resistant ERα+ breast cancer cell lines—MCF-7L TamR and T47D TamR [12, 19]—were also evaluated. These cells have reduced IRS-1 expression due to ERα functional suppression but retained similar expression levels of IRS-2 expression. Monolayer and anchorage-independent growth assays both indicated that NT157 blocked ligand-induced proliferation in TamR cells (Fig. S7). Thus, targeting IRS proteins by NT157 may also have therapeutic potential in treating endocrine-resistant breast cancers.
To investigate the specificity and toxicity of NT157 towards IRS proteins, immortalized breast epithelial cell line MCF10A, MCF-7L, and MCF-7L tamoxifen-resistant (TamR) cell lines were studied. MCF-7L TamR cells expressed significantly lower level of IRS-1 when compared to its parental cell line [12, 19]. The dose-response curves showed that MCF-7L cells were significantly more sensitive to NT157 treatment (Fig. S5A) than TamR cells. Concentrations of NT157 up to 2 μM did not affect MCF10A cells while this concentration suppressed monolayer growth of MCF-7L cells (Fig. S5A left). These data indicated that NT157 potently downregulates IRS proteins in multiple breast cancer cell lines and growth effects are associated with the level of IRS expression.
NT157 Compound Sensitized ERα+ Breast Cancer Cells to mTOR Inhibition
The mammalian target of rapamycin (mTOR) is a downstream effector of PI3K signaling. Inhibitors of mTOR are experimentally and clinically proven to have therapeutic effects in breast cancer [20, 21]. However, mTOR inhibitors suppress S6K1 activity. S6K1 functions to phosphorylate IRS proteins at serine sites resulting in IRS downregulation. Thus, mTOR inhibition results in disruption of a negative feedback loop to enhance levels of IRS expression [22], increase upstream receptor tyrosine kinase activation [23], and may result in resistance to this class of drugs. Therefore, NT157 could overcome the consequences of rapamycin upregulation of IRS and might improve cancer cell growth inhibition.
NT157 sensitized ERα+ cellular response to rapamycin treatment in both monolayer and colony formation in full media or IGF-I-treated conditions (Fig. 6a, b top panels). Immunoblot data also showed that rapamycin treatment alone caused upregulation of IRS proteins while NT157 suppressed this effect of rapamycin on IRS expression (Fig. 6b bottom panel). These data implicated that NT157 could be combined with rapalogs in the treatment of ERα+ breast cancers to avoid monotherapy induced resistance.
NT157 treatment sensitized ERα+ breast cancer cells to rapamycin. a Left panels: MCF-7 and T47D cells were plated then treated with indicated combinations for 5 days. Monolayer proliferation was evaluated by MTT assay. Right panels: MCF-7 and T47D cells were plated in 6-well plates treated with indicated combinations. Anchorage-independent growth was determined by colony formation in agarose after 14 days. b Top panels: MCF-7 and T47D cells were serum-starved overnight, treated with indicated combinations. Formed colonies were counted and analyzed after 14 days. Bottom panel: MCF-7 cells were treated with indicated combinations. Protein levels of IRS-1, IRS-2, IGF-IRβ, phospho-AKT, phospho-S6K1, phospho-p38MAPK, and actin were determined by immunoblotting. Data are mean ± SEM; results are representative of at least three independent triplicates experiments
Discussion
Preclinical and population data implicated IGF-IR’s critical roles in cancer biology and encouraged the development of anti-IGF-IR-targeted therapies. However, almost all IGF-IR monoclonal antibody (monotherapy or in combination with other therapies) clinical trials have failed to show clinical benefit in a significant number of patients [2, 24]. Because the IGF-IR inhibitors upregulate systemic insulin levels, disruption of InR signaling might be necessary to inhibit this highly homologous pathway [7]. This is especially true in patients with endocrine-resistant breast cancer as IR is the predominant receptor expressed in these tumors [8].
Our previous work showed that IRS proteins were the predominant adaptor proteins downstream of both IGF-IR/InR in breast cancer cells [4, 5] and IGF-IR/IR required the IRS proteins to transduce signaling as well as mediate biological outcomes in breast cancer models [3]. Disruption of IRS proteins might be a better strategy to inhibit both receptors’ signaling pathways. NT157 downregulation of IRS proteins resulted in dual receptor intracellular signaling inhibition in melanoma [9], prostate [10], and breast cancers.
In the current study, we tested NT157’s efficacy and mechanism in breast cancer cells, and we showed that NT157 induced the serine phosphorylation of IRS proteins, which resulted in the degradation of IRS. We also found that NT157 promoted the dissociation of ERα from IRS-IGF-IR/InR complex and resulted in ERα degradation. The cytoplasmic degradation of ERα further resulted in the ESR1-regulated gene suppression and inhibitory effects of the S phase cell cycle regulatory machinery. These findings were unique in ERα+ breast cancers. We also noticed that prolonged NT157 treatment also resulted in total AKT degradation. This was possibly due to extended ubiquitin-dependent mechanism [25] as the degradation of IRS proteins and ERα were believed to undergo this pathway [9]. NT157 also induces PARP cleavage in breast cancer cells (Fig. 4d) and caspase-mediated Akt cleavage [25] could also play a role in reducing Akt levels (Fig. 5c).
In the tamoxifen-resistant ERα+ breast cancer cells (details described previously [12]), NT157 also had inhibitory effects. Dual targeting of upstream signaling pathways and ERα might be superior to targeting a single pathway alone. The clinical approval of palbociclib and everolimus for treatment of ERα-expressing breast cancer demonstrates the value of developing inhibitors of these pathways in hormone-sensitive and -resistant cells. These encouraging results suggested that in hormone-resistant TamR cancers, targeting IRS proteins could be a therapeutic option.
Our study showed that rapamycin-treated ERα+ breast cancer cells had elevated IRS protein expression levels. Co-targeting IRS by NT157 resulted in improved growth inhibitory effects. A recent study showed that IGF-IR and IRS-1 were increased in crizotinib-treated anaplastic lymphoma receptor tyrosine kinase (ALK) fusion protein-positive lung cancer patients and co-targeting IGF-IR axis with ALK tyrosine kinase inhibitor resulted in therapeutic enhancement [26]. Another study demonstrated that targeting PI3K in hormone receptor breast tumors resulted in upregulation of ER function, which suggested that the necessity of co-targeting PI3K signaling pathway and ER in ER+ breast cancer patients [27]. NT157’s ability to disrupt IGF-IR/IR-IRS-1-ERα complex might make it a better drug to overcome hormone resistance. Recent data using phosphoproteomic profiling of A375 melanoma cells showed that multiple kinase signaling pathways are affected by NT157 including p38 MAPK, AXL, JNK and Src [11]. Thus, the drugs ability to disrupt IRS expression could result in biological effects important in its function.
Overall, our study emphasized the NT157 therapeutic potential as mono- and combination therapy in various breast cancer models. In addition, we, for the first time, revealed that NT157 also targeted ERα in ERα+ breast cancer cells. Targeting IRS protein could be useful alone or in combination with other therapies in many different subtypes of breast cancer.
References
Pollak M (2012) The insulin and insulin-like growth factor receptor family in neoplasia: an update. Nat Rev Cancer 12:159–169
Yang Y, Yee D (2012) Targeting insulin and insulin-like growth factor signaling in breast cancer. J Mammary Gland Biol Neoplasia 17:251–261
Byron SA, Horwitz KB, Richer JK, Lange CA, Zhang X, Yee D (2006) Insulin receptor substrates mediate distinct biological responses to insulin-like growth factor receptor activation in breast cancer cells. Br J Cancer 95:1220–1228
Jackson JG, White MF, Yee D (1998) Insulin receptor substrate-1 is the predominant signaling molecule activated by insulin-like growth factor-i, insulin, and interleukin-4 in estrogen receptor-positive human breast cancer cells. J Biol Chem 273:9994–10003
Jackson JG, Zhang X, Yoneda T, Yee D (2001) Regulation of breast cancer cell motility by insulin receptor substrate-2 (irs-2) in metastatic variants of human breast cancer cell lines. Oncogene 20:7318–7325
Mercado-Matos J, Clark JL, Piper AJ, Janusis J, Shaw LM (2017) Differential involvement of the microtubule cytoskeleton in insulin receptor substrate 1 (irs-1) and irs-2 signaling to akt determines the response to microtubule disruption in breast carcinoma cells. J Biol Chem 292:7806–7816
Yee D (2015) A tale of two receptors: insulin and insulin-like growth factor signaling in cancer. Clin Cancer Res 21:667–669
Gradishar WJ, Yardley DA, Layman R, Sparano JA, Chuang E, Northfelt DW, Schwartz GN, Youssoufian H, Tang S, Novosiadly R, Forest A, Nguyen TS, Cosaert J, Grebennik D, Haluska P (2016) Clinical and translational results of a phase ii, randomized trial of an anti-igf-1r (cixutumumab) in women with breast cancer that progressed on endocrine therapy. Clin Cancer Res 22:301–309
Reuveni H, Flashner-Abramson E, Steiner L, Makedonski K, Song R, Shir A, Herlyn M, Bar-Eli M, Levitzki A (2013) Therapeutic destruction of insulin receptor substrates for cancer treatment. Cancer Res 73:4383–4394
Ibuki N, Ghaffari M, Reuveni H, Pandey M, Fazli L, Azuma H, Gleave ME, Levitzki A, Cox ME (2014) The tyrphostin nt157 suppresses insulin receptor substrates and augments therapeutic response of prostate cancer. Mol Cancer Ther 13:2827–2839
Su SP, Flashner-Abramson E, Klein S, Gal M, Lee RS, Wu J, Levitzki A, Daly RJ (2018) Impact of the anticancer drug nt157 on tyrosine kinase signaling networks. Mol Cancer Ther 17:931–942
Fagan DH, Uselman RR, Sachdev D, Yee D (2012) Acquired resistance to tamoxifen is associated with loss of the type I insulin-like growth factor receptor: implications for breast cancer treatment. Cancer Res 72:3372–3380
Gyorffy B, Lanczky A, Eklund AC, Denkert C, Budczies J, Li Q, Szallasi Z (2010) An online survival analysis tool to rapidly assess the effect of 22,277 genes on breast cancer prognosis using microarray data of 1,809 patients. Breast Cancer Res Treat 123:725–731
Oesterreich S, Zhang P, Guler RL, Sun X, Curran EM, Welshons WV, Osborne CK, Lee AV (2001) Re-expression of estrogen receptor alpha in estrogen receptor alpha- negative mcf-7 cells restores both estrogen and insulin-like growth factor-mediated signaling and growth. Cancer Res 61:5771–5777
Tian J, Berton TR, Shirley SH, Lambertz I, Gimenez-Conti IB, DiGiovanni J, Korach KS, Conti CJ, Fuchs-Young R (2012) Developmental stage determines estrogen receptor alpha expression and non-genomic mechanisms that control igf-1 signaling and mammary proliferation in mice. J Clin Invest 122:192–204
Lee AV, Jackson JG, Gooch JL, Hilsenbeck SG, Coronado-Heinsohn E, Osborne CK, Yee D (1999) Enhancement of insulin-like growth factor signaling in human breast cancer: estrogen regulation of insulin receptor substrate-1 expression in vitro and in vivo. Mol Endocrinol 13:787–796
Molloy CA, May FE, Westley BR (2000) Insulin receptor substrate-1 expression is regulated by estrogen in the mcf-7 human breast cancer cell line. J Biol Chem 275:12565–12571
Song RX, Chen Y, Zhang Z, Bao Y, Yue W, Wang JP, Fan P, Santen RJ (2010) Estrogen utilization of igf-1-r and egf-r to signal in breast cancer cells. J Steroid Biochem Mol Biol 118:219–230
Yang Y, Yee D (2014) Igf-I regulates redox status in breast cancer cells by activating the amino acid transport molecule xC. Cancer Res 74:2295–2305
Wander SA, Hennessy BT, Slingerland JM (2011) Next-generation mtor inhibitors in clinical oncology: how pathway complexity informs therapeutic strategy. J Clin Invest 121:1231–1241
Vignot S, Faivre S, Aguirre D, Raymond E (2005) Mtor-targeted therapy of cancer with rapamycin derivatives. Ann Oncol 16:525–537
Tremblay F, Brule S, Hee Um S, Li Y, Masuda K, Roden M, Sun XJ, Krebs M, Polakiewicz RD, Thomas G, Marette A (2007) Identification of irs-1 ser-1101 as a target of s6k1 in nutrient- and obesity-induced insulin resistance. Proc Natl Acad Sci U S A 104:14056–14061
O’Reilly KE, Rojo F, She QB, Solit D, Mills GB, Smith D, Lane H, Hofmann F, Hicklin DJ, Ludwig DL, Baselga J, Rosen N (2006) mTOR inhibition induces upstream receptor tyrosine kinase signaling and activates Akt. Cancer Res 66:1500–1508
Yee D (2012) Insulin-like growth factor receptor inhibitors: baby or the bathwater? J Natl Cancer Inst 104:975–981
Liao Y, Hung MC (2010) Physiological regulation of Akt activity and stability. Am J Transl Res 2:19–42
Lovly CM, McDonald NT, Chen H, Ortiz-Cuaran S, Heukamp LC, Yan Y, Florin A, Ozretic L, Lim D, Wang L, Chen Z, Chen X, Lu P, Paik PK, Shen R, Jin H, Buettner R, Ansen S, Perner S, Brockmann M, Bos M, Wolf J, Gardizi M, Wright GM, Solomon B, Russell PA, Rogers TM, Suehara Y, Red-Brewer M, Tieu R, de Stanchina E, Wang Q, Zhao Z, Johnson DH, Horn L, Wong KK, Thomas RK, Ladanyi M, Pao W (2014) Rationale for co-targeting IGF-1R and ALK in ALK fusion-positive lung cancer. Nat Med 20:1027–1034
Bosch A, Li Z, Bergamaschi A, Ellis H, Toska E, Prat A, Tao JJ, Spratt DE, Viola-Villegas NT, Castel P, Minuesa G, Morse N, Rodon J, Ibrahim Y, Cortes J, Perez-Garcia J, Galvan P, Grueso J, Guzman M, Katzenellenbogen JA, Kharas M, Lewis JS, Dickler M, Serra V, Rosen N, Chandarlapaty S, Scaltriti M, Baselga J (2015) Pi3k inhibition results in enhanced estrogen receptor function and dependence in hormone receptor-positive breast cancer. Sci Transl Med 7:283ra251
Acknowledgements
The authors thank the assistance of the Flow Cytometry shared resource of the Masonic Cancer Center (P30 CA077598).
Funding
This study was supported by Komen for the Cure SAC110039 (DY), Mayo Clinic SPORE in Breast Cancer (NIH/NCI P50CA116201-06A1 - Ingle), and NIH/NCI Cancer Center Support Grant (2P30-CA077598 - Yee).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Electronic Supplementary Material
ESM 1
S1 NT157-induced IRS protein degradation was specific. MCF-7 cells were serum starved overnight then treated with 3 μM NT157 for the indicated time period. Protein levels of IRS-1, total ERα, and actin were determined by immunoblotting. S2 NT157 downregulated ER protein. Top panels: MCF-7 and T47D cells were transfected with 25 nM siRNA control or 25 nM siRNA IRS1/2 for 48 h. Total RNA was isolated and reverse transcribed. mRNA expressions of IRS-1, IRS-2, ESR1, CCND1, and p21 were determined by qRT-PCR. Bottom panel: MCF-7 cells were 1) serum starved overnight, pretreated with 3 μM of NT157 for 4 h, then induced with or without 5 nM IGF-I for 6 h; 2) transfected by control or IRS1/2 siRNA for 48 h, starved overnight, then stimulated with or without 5 nM IGF-I for 4 h. Protein levels of phospho-p38MAPK, cyclin D1, p21, ERα, and actin were assessed by immunoblotting. S3 Neither NT157 treatment nor genetic downregulation of IRS1 or IRS2 affected short term IGF-I stimulation induced PI3K and MAPK signaling. A. MCF-7 and T47D cells were starved overnight, pretreated with indicated dosages of NT157 drug for 4 h, and stimulated with or without 5 nM IGF-I for 10 min. Protein levels of IRS-1, py20, phospho-IGF-IR/IR, phospho-AKT, phospho-MAPK, total MAPK, and actin were determined by immunoblotting. B. MCF-7 and T47D cells were transfected with 25 nM siRNA control, siRNA IRS-1, or siRNA IRS-2 for 48 h. Cells were then serum starved overnight and treated with 5 nM IGF-I for 10 min. Protein levels of IRS-1, IRS-2, phospho-AKT, phospho-MAPK, and actin were determined by immunoblotting. S4 NT157 specifically suppressed cyclin D1 and induced p21 in MCF-7 cells. MCF-7 cells were starved overnight, pretreated with or without 3 μM NT157 drug for 4 h, then stimulated with or without 5 nM IGF-I for 6 h. Protein levels of IRS-1 cyclin D1, p21 CDK2, cyclin D3, CKD6, p18, and actin were determined by immunoblotting. S5 NT157 inhibited proliferation in ERα + breast cancer cells in a dose dependent manner. A. Left: MCF-7 L and MCF-7 L TamR cells were plated in 24 well plates and treated with indicated dosages of NT157 drug for 5 days. Monolayer proliferation was determined by MTT assay. Right: MCF-7 L and MCF-7 L TamR cells were plated in 6-well plates and treated with indicated dosages of NT157. Anchorage-independent growth was determined by colonies formation in agarose after 14 days. B. MCF-7 and T47D cells were serum starved overnight then treated with indicated treatment combination for 5 days. Monolayer proliferation was measured by MTT assay. Data are mean ± SEM; results are representative of at least three independent triplicates experiments. S6 Genetic downregulation of IRS1/2 partially suppressed proliferation and prolonged IGF-I induced PI3K activation in ERα + breast cancer cells. A. MCF-7 and T47D cells were transfected with 25 nM siRNA control or 25 nM siRNA IRS1/2 for 48 h. Cells were serum starved overnight then plated in 6-well plates and treated with IGF-I (5 nM), IGF-II (10 nM), insulin (10 nM), and E2 (1 nM). Anchorage-independent growth was determined by colonies formation in agarose after 14 days. B. MCF-7 cells were transfected with 25 nM siRNA control or 25 nM siRNA IRS1/2 for 48 h. Cells were starved overnight then plated in 6-well plates and treated with IGF-I (5 nM), IGF-II (10 nM), insulin (10 nM), and E2 (1 nM) for 24 h. Protein levels of IRS-1, IRS-2, phospho-AKT, cyclin D1, p21, and actin were determined by immunoblotting. Data are mean ± SEM; results are representative of at least three independent triplicates experiments. S7 NT157 inhibited ligand induced proliferation in tamoxifen resistant ERα + breast cancer cells. MCF-7 TamR and T47D TamR cells were 1) serum starved overnight then treated with indicated combinations. Monolayer proliferation was assessed by MTT assay after 5 days (left panels). 2) Starved overnight then treated with indicated combinations. Anchorage independent growth was determined by colonies formation in agarose after 14 days (right panels). Data are mean ± SEM; results are representative of at least three independent triplicates experiments.(PPTX 1491 kb).
Rights and permissions
About this article
Cite this article
Yang, Y., Chan, J.Y., Temiz, N.A. et al. Insulin Receptor Substrate Suppression by the Tyrphostin NT157 Inhibits Responses to Insulin-Like Growth Factor-I and Insulin in Breast Cancer Cells. HORM CANC 9, 371–382 (2018). https://doi.org/10.1007/s12672-018-0343-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12672-018-0343-8