Abstract
Infection by dengue virus is common in tropical countries. Hepatic involvement in dengue can range from asymptomatic elevation of transaminases to life-threatening acute liver failure (ALF). Dengue-related ALF (DALF) is responsible for significant morbidity and mortality, especially in Southeast Asia. However, there is a scarcity of literature on DALF, necessitating a thorough examination of its clinical determinants and management strategies. All relevant studies related to DALF were reviewed until December 2023. Case reports, case series and studies reporting ALF in dengue infection were included. Demographics, clinical profiles, management and outcomes of DALF cases were analyzed, which revealed a predominance of DALF incidence in pediatric patients (1.1% to 15.8%) and an upward trend over the years, particularly in India. The proportion of ALF cases attributable to dengue was also higher among pediatric ALF patients (6.7% to 34.3%). Age ≤ 40 years, persistent nausea, vomiting and elevated serum bilirubin and alkaline phosphatase (ALP) with aspartate aminotransferase (AST) > 1000 IU/mL within the first five days of illness, more than 10% of atypical lymphocytes in peripheral blood, platelet count of < 50,000/cu·mm, severe hepatitis at presentation and baseline model for end-stage liver disease (MELD) > 15 were the risk factors for the development of DALF. Histopathological features of DALF included multi-lobular hepatic necrosis, steatosis and occasional cholestasis. Mortality in DALF ranged from 0% to 80%; admission pH and lactate strongly predicted mortality, while mortality was found to be significantly higher in patients with cirrhosis. N-Acetyl cysteine (NAC) has been used as a treatment modality with varying results. There is limited evidence regarding the use of extra-corporeal support systems, while candidate selection for liver transplantation (LT) in DALF remains poorly defined.
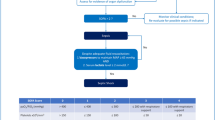
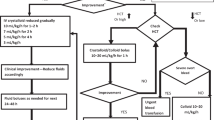
Graphical Abstract

Similar content being viewed by others
Data Availability
None.
References
Phanitchat T, Zhao B, Haque U, et al. Spatial and temporal patterns of dengue incidence in northeastern Thailand 2006–2016. BMC Infect Dis. 2019;19:743.
Thisyakorn U, Thisyakorn C. DENGUE: GLOBAL THREAT. Southeast Asian J Trop Med Public Health. 2015;46:3–10.
Dengue/DHF situation in India: National Center for Vector Borne Diseases Control.; 2023. Accessed: January 23, 2024.
Fernando S, Wijewickrama A, Gomes L, et al. Patterns and causes of liver involvement in acute dengue infection. BMC Infect Dis. 2016;16:319.
Leowattana W, Leowattana T. Dengue hemorrhagic fever and the liver. World J Hepatol. 2021;13:1968–76.
Chakravarti A, Arora R, Luxemburger C. Fifty years of dengue in India. Trans R Soc Trop Med Hyg. 2012;106:273–82.
Lawn SD, Tilley R, Lloyd G, et al. Dengue hemorrhagic fever with fulminant hepatic failure in an immigrant returning to Bangladesh. Clin Infect Dis. 2003;37:e1-4.
Subramanian V, Shenoy S, Joseph AJ. Dengue hemorrhagic fever and fulminant hepatic failure. Dig Dis Sci. 2005;50:1146–7.
Vinodh BN, Bammigatti C, Kumar A, Mittal V. Dengue fever with acute liver failure. J Postgrad Med. 2005;51:322–3.
Penafiel A, Devanand A, Tan HK, Eng P. Use of molecular adsorbent recirculating system in acute liver failure attributable to dengue hemorrhagic fever. J Intensive Care Med. 2006;21:369–71.
Gasperino J, Yunen J, Guh A, Tanaka KE, Kvetan V, Doyle H. Fulminant liver failure secondary to haemorrhagic dengue in an international traveller. Liver Int. 2007;27:1148–51.
Ling LM, Wilder-Smith A, Leo YS. Fulminant hepatitis in dengue haemorrhagic fever. J Clin Virol. 2007;38:265–8.
Giri S, Agarwal MP, Sharma V, Singh A. Acute hepatic failure due to dengue: a case report. Cases J. 2008;1:204.
Soundravally R, Narayanan P, Bhat BV, Soundraragavan J, Setia S. Fulminant hepatic failure in an infant with severe dengue infection. Indian J Pediatr. 2010;77:435–7.
Viswanathan S, Iqbal N, Anemon PP, Kumar GS. Fatal fulminant hepatic failure in a diabetic with primary dengue. J Trop Med. 2010;2010: 413561.
Vijayalakshmi AM, Devaprasath S. Fulminant hepatic failure in primary dengue infection. Indian Pediatr. 2010;47:280.
Jhamb R, Kashyap B, Ranga GS, Kumar A. Dengue fever presenting as acute liver failure–a case report. Asian Pac J Trop Med. 2011;4:323–4.
Lim G, Lee JH. N-acetylcysteine in children with dengue-associated liver failure: a case report. J Trop Pediatr. 2012;58:409–13.
Abeysekera RA, Illangasekera U, Jayalath T, Sandeepana AG, Kularatne SA. Successful use of intravenous N-acetylcysteine in dengue haemorrhagic fever with acute liver failure. Ceylon Med J. 2012;57:166–7.
Sedhain A, Adhikari S, Regmi S, Chaudhari SK, Shah M, Shrestha B. Fulminant hepatic failure due to dengue. Kathmandu Univ Med J (KUMJ). 2011;9:73–5.
Manoj EM, Ranasinghe G, Ragunathan MK. Successful use of N-acetyl cysteine and activated recombinant factor VII in fulminant hepatic failure and massive bleeding secondary to dengue hemorrhagic fever. J Emerg Trauma Shock. 2014;7:313–5.
Arora S, Nathaniel SD, Paul JC, Hansdak SG. Acute liver failure in dengue haemorrhagic fever. BMJ Case Rep. 2015;2015:bcr2015209443.
Abdulrahman B, Ahmed MH, Ramage J. Acute liver failure in a patient travelling from Asia: the other face of the coin of infectious disease. Gastroenterology Res. 2017;10:268–70.
Dalugama C, Gawarammana IB. Dengue hemorrhagic fever complicated with acute liver failure: a case report. J Med Case Rep. 2017;11:341.
Nazeer A, Rai AA, Luck NH, Tasneem AAY. Dengue hemorrhagic fever: arare cause of acute liver failure. J Coll Physicians Surg Pak. 2017;27:511–3.
Singh L, Singh A, Agarwal M, Mishra S. Is dengue emerging as important cause of acute liver failure in endemic regions? World J Clin Cases. 2017;5:303–6.
Samarasekara K, Munasinghe J. Dengue shock syndrome complicated with acute liver failure and kidney injury, infective endocarditis, and deep vein thrombosis: a case report. J Med Case Rep. 2018;12:321.
Galante A, Adeyi O, Lau L, et al. Liver transplantation for acute liver failure due to dengue fever. Hepatology. 2019;70:1863–5.
Suganthan N, Sakthilingham G, Kumanan T. Dengue fever complicated with acute liver failure: a case report of expanded dengue syndrome and literature review. SAGE Open Med Case Rep. 2020;8:2050313X20913428.
Chikkala BR, Pandey Y, Acharya R, et al. Living donor liver transplant for dengue-related acute liver failure: a case report. Exp Clin Transplant. 2021;19:163–6.
Arunpriyandan V, Sundaresan KT. Fulminant hepatic failure in dengue fever without plasma leakage: a case report. Cureus. 2022;14: e23964.
Gautam A, Singh H. Dengue fever with fulminant liver failure and fatal pulmonary alveolar hemorrhage: a case report. Cureus. 2022;14: e28302.
Gunasekera AM, Eranthaka U, Priyankara D, Kalupahana R. A rare case of acute liver failure with intrahepatic cholestasis due to dengue hemorrhagic fever: CytoSorb® and plasma exchange aided in the recovery: case report. BMC Infect Dis. 2022;22:938.
Thadchanamoorthy V, Dayasiri K. Expanded dengue syndrome presenting with acute liver failure, acute kidney injury, pancreatic involvement, coagulopathy, and multiple intracranial hemorrhages in a young child: a case report. J Med Case Rep. 2022;16:123.
Achhami E, Adhikari L, Shrestha S, Shrestha AB. Acute liver failure in a young patient with dengue shock syndrome: a case report. Ann Med Surg (Lond). 2023;85:286–90.
Jeyabalan SV, Tay TR, Tan SY, Kumar R. Successful treatment of acute liver failure secondary to dengue fever using low-volume plasma exchange. Singapore Med J. 2023. https://doi.org/10.4103/singaporemedj.SMJ-2021-165
Roy A, Sarkar D, Chakraborty S, Chaudhuri J, Ghosh P, Chakraborty S. Profile of hepatic involvement by dengue virus in dengue infected children. N Am J Med Sci. 2013;5:480–5.
Laoprasopwattana K, Jundee P, Pruekprasert P, Geater A. Outcome of severe dengue viral infection-caused acute liver failure in Thai children. J Trop Pediatr. 2016;62:200–5.
Mohan N, Goyal D, Sakshi K, Perumal V. Profile of dengue hepatitis in children from India and its correlation with WHO dengue case classification. Asian Pac J Trop Dis. 2017;7:327–31. https://doi.org/10.12980/apjtd.7.2017D6-430.
Prasad D, Bhriguvanshi A. Clinical profile, liver dysfunction and outcome of dengue infection in children: a prospective observational study. Pediatr Infect Dis J. 2020;39:97–101.
Dogra S, Kumar K, Malhotra S, Jerath N, Sibal A. Acute liver failure in dengue: a common but overlooked entity in pediatric patients in tropical countries. J Pediatr Gastroenterol Nutr. 2023;76:149–53.
Nguyen TT, Nguyen DT, Vo TT, et al. Associations of obesity and dengue-associated mortality, acute liver failure and mechanical ventilation in children with dengue shock syndrome. Medicine (Baltimore). 2023;102:e36054.
Kumarasena RS, Niriella MA, Ranawaka CK, et al. Predicting acute liver failure in dengue infection. Ceylon Med J. 2016;61:35–6.
Kye Mon K, Nontprasert A, Kittitrakul C, Tangkijvanich P, Leowattana W, Poovorawan K. Incidence and clinical outcome of acute liver failure caused by dengue in a hospital for tropical diseases. Am J Trop Med Hyg. 2016;95:1338–44.
Iqtadar S, Akbar N, Huma N, Randhawa FA. Profile of hepatic involvement in dengue infections in adult Pakistani population. Pak J Med Sci. 2017;33:963–7.
Devarbhavi H, Ganga D, Menon M, Kothari K, Singh R. Dengue hepatitis with acute liver failure: clinical, biochemical, histopathological characteristics and predictors of outcome. J Gastroenterol Hepatol. 2020;35:1223–8.
Kulkarni AV, Choudhury AK, Premkumar M, Jain P, Gupta E, Sarin SK. Spectrum, manifestations and outcomes of dengue infection in individuals with and without liver disease. J Clin Transl Hepatol. 2019;7:106–11.
Kumar R, Bhushan D, Anand U. Acute liver failure in dengue present some peculiar features. J Clin Exp Hepatol. 2019;9:416–7.
Teerasarntipan T, Chaiteerakij R, Komolmit P, Tangkijvanich P, Treeprasertsuk S. Acute liver failure and death predictors in patients with dengue-induced severe hepatitis. World J Gastroenterol. 2020;26:4983–95.
Prajapati R, Mehta R, Kabrawala M, et al. Dengue hepatitis: Incidence, spectrum and outcome. Indian J Gastroenterol. 2023;42:355–60.
Alam R, Rukunuzzaman M, Nahid KL. Hepatic involvement in childhood dengue infection. Egypt Liv J. 2023;13:45.
Poovorawan Y, Hutagalung Y, Chongsrisawat V, Boudville I, Bock HL. Dengue virus infection: a major cause of acute hepatic failure in Thai children. Ann Trop Paediatr. 2006;26:17–23.
Kumar R, Tripathi P, Tripathi S, Kanodia A, Venkatesh V. Prevalence of dengue infection in north Indian children with acute hepatic failure. Ann Hepatol. 2008;7:59–62.
Chongsrisawat V, Hutagalung Y, Poovorawan Y. Liver function test results and outcomes in children with acute liver failure due to dengue infection. Southeast Asian J Trop Med Public Health. 2009;40:47–53.
Alam S, Lal BB, Khanna R, Sood V, Rawat D. Acute liver failure in infants and young children in a specialized pediatric liver centre in India. Indian J Pediatr. 2015;82:879–83.
Getsuwan S, Lertudomphonwanit C, Tanpowpong P, et al. Etiologies, prognostic factors, and outcomes of pediatric acute liver failure in Thailand. Pediatr Gastroenterol Hepatol Nutr. 2020;23:539–47.
Amatya P, Kapalavai SK, Deep A, et al. Pediatric acute liver failure: an experience of a pediatric intensive care unit from resource limited settings. Front Pediatr. 2022;10:956699.
Deepak NA, Patel ND. Differential diagnosis of acute liver failure in India. Ann Hepatol. 2006;5:150–6.
Jain J, Jain M. Acute liver failure in tropical infections- thinking beyond viral hepatitis! Trop Doct. 2023;53:137–9.
Tan SS, Bujang MA. The clinical features and outcomes of acute liver failure associated with dengue infection in adults: a case series. Braz J Infect Dis. 2013;17:164–9.
Lum LC, Lam SK, George R, Devi S. Fulminant hepatitis in dengue infection. Southeast Asian J Trop Med Public Health. 1993;24:467–71.
Zafarullah M, Li WQ, Sylvester J, Ahmad M. Molecular mechanisms of N-acetylcysteine actions. Cell Mol Life Sci. 2003;60:6–20.
Rank N, Michel C, Haertel C, et al. N-acetylcysteine increases liver blood flow and improves liver function in septic shock patients: results of a prospective, randomized, double-blind study. Crit Care Med. 2000;28:3799–807.
Mumtaz K, Azam Z, Hamid S, et al. Role of N-acetylcysteine in adults with non-acetaminophen-induced acute liver failure in a center without the facility of liver transplantation. Hepatol Int. 2009;3:563–70.
Kumarasena RS, Mananjala Senanayake S, Sivaraman K, et al. Intravenous N-acetylcysteine in dengue-associated acute liver failure. Hepatol Int. 2010;4:533–4.
Senanayake MP, Jayamanne MD, Kankananarachchi I. N-acetylcysteine in children with acute liver failure complicating dengue viral infection. Ceylon Med J. 2013;58:80–2.
Sriphongphankul H, Liabsuetrakul T, Osatakul S. Clinical outcomes of children diagnosed dengue-associated acute liver failure with or without N-acetylcysteine treatment: a retrospective cohort study. J Trop Pediatr. 2021;67:fmab039.
Dissanayake DMDIB, Gunaratne WMSN, Kumarihamy KWMPP, Kularatne SAM, Kumarasiri PVR. Use of intravenous N-acetylcysteine in acute severe hepatitis due to severe dengue infection: a case series. BMC Infect Dis. 2021;21:978.
Pless G, Sauer IM. Bioartificial liver: current status. Transplant Proc. 2005;37:3893–5.
Kjaergard LL, Liu J, Als-Nielsen B, Gluud C. Artificial and bioartificial support systems for acute and acute-on-chronic liver failure: a systematic review. JAMA. 2003;289:217–22.
Mitzner SR, Stange J, Klammt S, Peszynski P, Schmidt R, Nöldge-Schomburg G. Extracorporeal detoxification using the molecular adsorbent recirculating system for critically ill patients with liver failure. J Am Soc Nephrol. 2001;12:S75-82.
Trepatchayakorn S, Chaijitraruch N, Chongsrisawat V, Chanakul A, Kongkiattikul L, Samransamruajkit R. Therapeutic plasma exchange with continuous renal replacement therapy for pediatric acute liver failure: a case series from Thailand. Indian J Crit Care Med. 2021;25:812–6.
Deep A, Stewart CE, Dhawan A, Douiri A. Effect of continuous renal replacement therapy on outcome in pediatric acute liver failure. Crit Care Med. 2016;44:1910–9.
Ankawi G, Neri M, Zhang J, Breglia A, Ricci Z, Ronco C. Extracorporeal techniques for the treatment of critically ill patients with sepsis beyond conventional blood purification therapy: the promises and the pitfalls. Crit Care. 2018;22:262.
Chris-Olaiya A, Kapoor A, Ricci KS, Lindenmeyer CC. Therapeutic plasma exchange in liver failure. World J Hepatol. 2021;13:904–15.
Thanh NT, Dat NT, Thinh TN, et al. Therapeutic plasma exchange and continuous renal replacement therapy in pediatric dengue-associated acute liver failure: a case series from Vietnam. Transfus Apher Sci. 2023;62:103617.
Vo LT, Do VC, Trinh TH, Vu T, Nguyen TT. Combined therapeutic plasma exchange and continuous renal replacement therapy in children with dengue-associated acute liver failure and shock syndrome: single-center cohort from Vietnam. Pediatr Crit Care Med. 2023;24:818–28.
Dengue: Guidelines for Diagnosis, Treatment, Prevention and Control: New Edition. Geneva: World Health Organization. 2009.
Prince HE, Matud JL. Estimation of dengue virus IgM persistence using regression analysis. Clin Vaccine Immunol. 2011;18:2183–5.
De Paula SO, Fonseca BA. Dengue: a review of the laboratory tests a clinician must know to achieve a correct diagnosis. Braz J Infect Dis. 2004;8:390–8.
Author information
Authors and Affiliations
Contributions
Conceptualization: SG, DLP; data curation: SG, PA, AV, DLP; formal analysis: SG, PA, DLP; funding acquisition: N/A; investigation: SG, PA, AV, DLP; methodology: SG, DLP; project administration: SG, DLP; resources: SG, PA, AV, DLP; software: SG; supervision; SG, DLP; validation: SG, DLP; visualization: SG, PA; roles/writing—original draft: SG, PA, DLP; writing—review and editing: SG, PA, AV, DLP.
Corresponding author
Ethics declarations
Conflict of interest
SG, PA, AV and DLP declare no competing interests.
Ethical approval and consent to participate
NA for scoping review.
Human ethics
No human subjects participated in the study.
Consent for publication
NA.
Disclaimer
The authors are solely responsible for the data and the content of the paper. In no way, the Honorary Editor-in-Chief, Editorial Board Members, or the the Indian Society of Gastroenterology, printer/publishers are responsible for the results/findings and content of this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Giri, S., Anirvan, P., Vaidya, A. et al. Dengue-related acute liver failure—A scoping review. Indian J Gastroenterol (2024). https://doi.org/10.1007/s12664-024-01570-w
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12664-024-01570-w