Abstract
Purpose
Upper airway injury and sympathetic activation may be related to the forces applied during laryngoscopy. We compared the applied forces during laryngoscopy using direct and indirect visualization of a standardized mannequin glottis.
Methods
Force transducers were applied to the concave surface of a GlideScope T-MAC Macintosh-style video laryngoscope that can also be used as a conventional direct-view laryngoscope. Thirty-four anesthesiologists performed four laryngoscopies (two direct and two indirect views) on an Ambu mannequin in a randomized sequence. During each laryngoscopy, participants were instructed to obtain views corresponding to > 80% and 50% of the glottic opening aperture. Peak and impulse forces were measured for each view.
Results
To achieve a 50% glottic opening view, the top 10th percentile force was higher with direct vs indirect laryngoscopy in terms of peak (difference, 9.1 newton; 99% confidence interval [CI], 7.4 to 13.9) and impulse (difference, 56.4 newton·sec; 99% CI, 49.0 to 81.7) forces. To achieve >80% view of the glottic opening, median force was higher with direct vs indirect laryngoscopy in terms of peak (difference, 3.6 newton; 99% CI, 1.6 to 7.3) and impulse (difference, 20.4 newton·sec; 99% CI, 11.7 to 35.1) forces.
Conclusions
In this mannequin study, lower forces applied during indirect vs direct laryngoscopy may reflect an advantage of video laryngoscopy, but additional studies using patients are required to confirm the clinical implications of these findings.
Résumé
Objectif
Les lésions aux voies aériennes supérieures et l’activation du système sympathique pourraient être dues aux forces appliquées pendant la laryngoscopie. Nous avons comparé les forces appliquées pendant une laryngoscopie avec visualisation directe vs indirecte d’une glotte standardisée sur mannequin.
Méthode
Des transducteurs ont été appliqués à la surface concave d’un vidéolaryngoscope de type Macintosh GlideScope T-MAC, un dispositif qui peut également être utilisé comme laryngoscope conventionnel avec visualisation directe. Trente-quatre anesthésiologistes ont chacun réalisé quatre laryngoscopies (deux visualisations directes et deux indirectes) sur un mannequin Ambu en suivant une séquence randomisée. Pendant chaque laryngoscopie, les participants avaient pour consigne d’obtenir des vues correspondant à > 80 % et 50 % de l’ouverture glottique. Les forces maximales et impulsions ont été mesurées pour chaque visualisation.
Résultats
Pour obtenir une visualisation à 50 % de l’ouverture glottique, le 10e percentile maximal était plus élevé en cas de laryngoscopie directe qu’en cas de laryngoscopie indirecte tant au maximum de la force (différence, 9,1 newton; intervalle de confiance [IC] 99 %, 7,4 à 13,9) qu’à l’impulsion (différence, 56,4 newton·sec; IC 99 %, 49,0 à 81,7). Pour obtenir une visualisation à > 80 % de l’ouverture glottique, la médiane était également plus élevée en cas de laryngoscopie directe qu’en cas de laryngoscopie indirecte, tant au maximum de la force (différence, 3,6 newton; intervalle de confiance [IC] 99 %, 1,6 à 7,3) qu’à l’impulsion (différence, 20,4 newton·sec; IC 99 %, 11,7 à 35,1).
Conclusion
Dans cette étude sur mannequin, les forces et impulsions moins prononcées appliquées pendant la laryngoscopie indirecte plutôt que directe pourraient refléter un avantage de la vidéolaryngoscopie, mais des études supplémentaires sur patient sont nécessaires afin de confirmer les implications cliniques de ces résultats.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
During laryngoscopy, a displacement force is applied to the base of the tongue. This helps achieve a laryngeal view of the vocal cords that enables oral intubation. Laryngoscopy can cause airway trauma. It is also a well-recognized sympathetic trigger associated with increased plasma catecholamine concentration, blood pressure, and heart rate.1,2,3,4
Decreasing the force applied during laryngoscopy may help reduce these negative events. Direct laryngoscopy requires displacement of oropharyngeal tissues to achieve a straight line-of-sight of the glottis. Indirect (video) laryngoscopy presents the view obtained from the video camera, located distally on the laryngoscope blade. This potentially requires less tissue displacement. It was previously described that laryngoscopy forces applied to both mannequins5 and patients6,7 using a hyperangulated GlideScope blade (Verathon, Bothell, WA, USA) were lower than those applied with a Macintosh (direct) laryngoscope.
Recently, a new video laryngoscope model, the GlideScope® Titanium™ Macintosh-style blade (T-MAC™), was introduced. It has the familiar look and feel of a conventional Macintosh blade and can be used for both indirect and direct laryngoscopy.
The rationale for this mannequin study was to compare the forces applied during direct and indirect laryngoscopy, using the same laryngoscope on the same airway to obtain a standardized glottic view. We postulated that with the GlideScope T-MAC, more force would be required during direct compared with indirect laryngoscopy to produce the same view of the glottis.
Methods
Ethical approval for this study (Number 16-5213-AE) was provided by the Toronto Academic Health Sciences Network Research Ethics Committee, Toronto, Canada in September 2016. Written informed consent was obtained from all participants.
Anesthesia staff and fellows in the Department of Anesthesia and Pain Management at Toronto General Hospital were invited to take part in this study. Inclusion criteria were active participation in operating-room based provision of adult anesthesia care, and experience with video laryngoscopy (> 25 intubations).
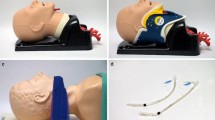
Three sessions of data collection were performed between December 2016 and February 2017. Participants were asked to obtain standardized laryngoscopic views of the Ambu® Airway Man mannequin (Ballerup, Denmark) glottis. Use of a mannequin airway eliminated anatomical variability, enabling us to present a standardized airway to multiple laryngoscopists. Participants were provided with a schematic depiction (Fig. 1) of 100%, 80%, and 50% view of the glottic opening for reference, and were asked to achieve a percent of glottic opening view of 50% and > 80%8 using direct and indirect laryngoscopy. Each participant was given the opportunity to practice and adjust the mannequin height prior to their recorded laryngoscopy attempts. External laryngeal manipulation was provided by an available “assistant” on request. With each participant, the sequencing of direct vs indirect laryngoscopy, and percentage of glottic opening view was randomized by a computer-generated block of events. The list of sequences was created before the study and each sequence was inserted into an opaque envelope that was sequentially numbered and sealed. At the beginning of the simulation, a researcher opened an envelope and asked the participant to perform as indicated in the sequence. During direct laryngoscopy, the video screen was turned away from the participant to ensure the glottic view was achieved only by direct laryngoscopy. For video laryngoscopy, participants were instructed to view only the video screen. Participants indicated verbally when they had achieved a 50% or > 80% view of the glottis and then inserted an endotracheal tube (size 7.0, cuffed) fitted with a Mallinckrodt™ Satin Slip® intubating stylet (Mallinckrodt™, Medtronic, Minneapolis, MN, USA) into the glottic opening (intubation confirmed on video screen). During laryngoscopy, force measurements were obtained from three FlexiForce Sensors (A201-25; Tekscan Inc., Boston, MA, USA) attached with double-sided adhesive to the distal concave surface of a size 3 GlideScope Titanium T-MAC blade (Fig. 2). The sensors are composed of thin (0.02 mm, 9.53 mm2), printed piezo-resistive strips that continuously measure the force with a response time of < 5 μsec and a linearity error of ± 3%. A dome-shaped plastic “puck” with a diameter of 0.91 cm was glued to each sensor as described in our previous study.5 The sensors were connected to a Tekscan Economical Load and Force (ELF™) measurement system and were calibrated prior to each of the three data collection sessions. Force was measured at each of the three sensors throughout laryngoscopy and intubation at intervals of 0.125 sec using the Tekscan ELF™ data capture software. Measurement started when the laryngoscope passed between the incisors of the mannequin and ceased as the endotracheal tube passed between the vocal cords. The participants were blinded to the force measurements. Participants were told that their attempts would be timed but that the times would not be analyzed.
The forces measured by the three sensors were summated and were not individually analyzed. According to previous studies,5,6,7 peak force (the maximum force recorded, expressed as newton [N]) and impulse force (integral of total force over time for laryngoscopy, expressed as newton·second [NS]) were calculated. Median and top 10th percentile values were calculated as relevant indicators of each force index, and median and top 10th percentile values (with confidence intervals [CI]) of the paired differences between direct and indirect laryngoscopy were used for comparisons. We assessed the top 10th percentile difference in forces to represent the maximum difference in applied forces. Because of coverage error of bootstrap CIs for quantiles in small samples, empirical bootstrap 99% CIs were calculated (functions “boot” and “boot.ci” of the R package “boot”) using re-sampling with replacement to create 1,000 samples of the same size as the original. Any CI (for the difference between direct and indirect laryngoscopy) not including zero indicated a statistically significant difference. Statistical analysis was performed using R 3.5 (R Foundation for Statistical Computing, Vienna, Austria).9 No statistical power calculation was conducted prior to the study, as we were unable to predict the magnitude of difference in forces applied during laryngoscopy. A convenience sample size of 34 participants was chosen in view of our previous experience with this study design.5
Results
Complete data sets were obtained from 25/34 participants. With eight participants, one of the sensors became disconnected or failed to provide data during the study, which prevented complete force data analysis during laryngoscopy. One participant stated that visual impairment prevented him from assessing the glottic view.
For the 50% percentage of glottic opening task, the median and the top 10th percentile for applied forces are reported in Table 1. There was no detectable median difference in peak or impulse force between direct and indirect laryngoscopy to obtain a view of 50% glottic opening (peak: 1.7 N; 99% CI, -3.6 to 8.2; impulse force, 15.1 NS; 99% CI, -9.6 to 41.9). Nevertheless, the top 10th percentile differences between direct and indirect laryngoscopy forces to obtain a 50% glottic view were greater than zero (peak, 91.0 N; 99% CI, 7.4 to 13.9; impulse force, 56.4 NS; 99% CI, 49.0 to 81.7; Table 1).
To obtain a view of > 80% of the glottic opening, the median difference in peak and impulse forces were greater than zero (peak: 3.6 N; 99% CI, 1.6 to 7.3; impulse force: 20.4 NS; 99% CI, 11.7 to 35.1). To obtain a view of > 80% of the glottic opening, the top 10th percentile difference in forces was greater than zero for the peak force (10.3 N; 99% CI, 8.8 to 15.6) but not for the impulse force (41.3 NS; 99% CI, -13.1 to 53.7) (Table 2).
External laryngeal manipulation was not requested by any participant. There were no failed intubation attempts and no laryngoscopy exceeded 95 sec. The dataset for impulse and peak forces for each laryngoscopy is available as an eTable (see Electronic Supplementary Material).
Discussion
The literature supports several advantages to video laryngoscopy compared with direct laryngoscopy, such as improved laryngeal view, reduced incidence of failed intubation, a higher chance of first-time success, and facilitation of training.10,11,12 In previous studies, we showed that the GlideScope hyperangulated blade required less applied force in mannequins12 and patients6,7 than a Macintosh-style laryngoscope. The findings of this study extend the advantages, showing that less force was required during indirect compared with direct laryngoscopy using the same Macintosh-style device. Previous studies showed large variability in applied force during laryngoscopy,6,13 implying that applied force can be reduced. Unfortunately, our study was not designed to evaluate such extent of variability.
There is a significant relationship between the intensity of the laryngoscopy stimulus and the maximal hemodynamic and catecholamine response.4 Even routine intubation produces measurable airway injury.14,15 These effects are further exacerbated in the presence of inadequate neuromuscular relaxation, anesthetic depth,16 or when performing laryngoscopy in a patient with a difficult airway.17 Clinicians focused on securing the airway may be unaware of the forces they are applying or the implications of using forces greater than necessary. Our findings support the use of indirect viewing over direct laryngoscopy when using the GlideScope T-MAC to reduce the required force. We acknowledge that the magnitude of force difference in our study has uncertain clinical relevance. Nevertheless, the forces used in this mannequin closely approximated those applied to human subjects in a previous study.5 Since laryngoscopy induces an impulse-dependent rise in cardiovascular stress,4 we believe that any reduction in force is desirable to minimize the potential for patient harm.
This study has some limitations that should be considered. First, we can only speculate about its relevance to patients because the study was performed on a mannequin.18,19,20 Nevertheless, this allowed us to eliminate the anatomical variability among patients. Second, the participants were aware that we were measuring force applied during laryngoscopy, and this might have biased their performance. Nevertheless, we asked the participants to use the laryngoscope as they would in their clinical practice, and they were blinded to the measured applied forces. Third, the study was not designed to evaluate the variability of forces applied between participants nor the factors (including level of experience) that may influence it. Future studies are needed to address these questions. Interestingly, despite being presented with an identical task, the range of forces applied varied by as much as tenfold. This suggests that there are opportunities to improve laryngoscopy technique. In particular, laryngoscopists should consider the glottic view required for a successful intubation. For example, a 50% view (or less) of the glottic opening may be entirely adequate for intubating purposes, obviating the need to use more force to achieve a greater percentage of glottic opening view. Finally, our results should be interpreted with caution given the limited sample size and the number of outcome measures.
In conclusion, in this mannequin study, higher median forces were applied with direct vs indirect laryngoscopy to achieve > 80% view of the glottic opening. For the top 10th percentile force differences, higher forces were applied with direct vs indirect laryngoscopy when aiming to achieve a view of 50% of the glottic opening. This may represent a desirable advantage of video laryngoscopy, but more clinical studies are required to verify the clinical implications of our findings.
References
Prys-Roberts C, Greene LT, Miloche R, Foex P. Studies of anaesthesia in relation to hypertension. II. Haemodynamic consequences of induction and endotracheal intubation. Br J Anaesth 1971; 43: 531-47.
Shribman AJ, Smith G, Achola KJ. Cardiovascular and catecholamine responses to laryngoscopy with and without tracheal intubation. Br J Anaesth 1987; 59: 295-9.
Derbyshire DR, Chmielewski A, Fell D, Vater M, Achola K, Smith G. Plasma catecholamine responses to tracheal intubation. Br J Anaesth 1983; 55: 855-60.
Hassan HG, El-Sharkawy TY, Renck H, Mansour G, Fouda A. Hemodynamic and catecholamine responses to laryngoscopy with vs. without endotracheal intubation. Acta Anaesthesiol Scand 1991; 35: 442-7.
Lee C, Russell T, Firat M, Cooper RM. Forces generated by Macintosh and GlideScope® laryngoscopes in four airway-training manikins. Anaesthesia 2013; 68: 492-6.
Russell T, Khan S, Elman J, Katznelson R, Cooper RM. Measurement of forces applied during Macintosh direct laryngoscopy compared with GlideScope® videolaryngoscopy. Anaesthesia 2012; 67: 626-31.
Cordovani D, Russell T, Wee W, Suen A, Cooper RM. Measurement of forces applied using a Macintosh direct laryngoscope compared with a Glidescope video laryngoscope in patients with predictors of difficult laryngoscopy: a randomised controlled trial. Eur J Anaesthesiol 2019; 36: 221-6.
Levitan RM, Hollander JE, Ochroch EA. A grading system for direct laryngoscopy. Anaesthesia 1999; 54: 1009-10.
R Core Team. R: A language and environment for statistical computing. R Foundation for Statistical Computing, Vienna, Austria, 2018. Available from URL: https://www.R-project.org/ (accessed November 2019).
Arulkumaran N, Lowe J, Ions R, Mendoza M, Bennett V, Dunser MW. Videolaryngoscopy versus direct laryngoscopy for emergency orotracheal intubation outside the operating room: a systematic review and meta-analysis. Br J Anaesth 2018; 120: 712-24.
Kelly FE, Cook TM, Boniface N, Hughes J, Seller C, Simpson T. Videolaryngoscopes confer benefits in human factors in addition to technical skills. Br J Anaesth 2015; 115: 132-3.
Russell T, Lee C, Firat M, Cooper RM. A comparison of the forces applied to a manikin during laryngoscopy with the GlideScope and Macintosh laryngoscopes. Anaesth Intensive Care 2011; 39: 1098-102.
Hastings RH, Hon ED, Nghiem C, Wahrenbrock EA. Force and torque vary between laryngoscopists and laryngoscope blades. Anesth Analg 1996; 82: 462-8.
Tanaka A, Isono S, Ishikawa T, Sato J, Nishino T. Laryngeal resistance before and after minor surgery: endotracheal tube versus Laryngeal Mask Airway. Anesthesiology 2003; 99: 252-8.
Mencke T, Echternach M, Kleinschmidt S, et al. Laryngeal morbidity and quality of tracheal intubation: a randomized controlled trial. Anesthesiology 2003; 98: 1049-56.
Pandit JJ, Andrade J, Bogod DG, et al. 5th National Audit Project (NAP5) on accidental awareness during general anaesthesia: summary of main findings and risk factors. Br J Anaesth 2014; 113: 549-59.
Santoni BG, Hindman BJ, Puttlitz CM, et al. Manual in-line stabilization increases pressures applied by the laryngoscope blade during direct laryngoscopy and orotracheal intubation. Anesthesiology 2009; 110: 24-31.
Ward PA, Irwin MG. Man vs. manikin revisited - the ethical boundaries of simulating difficult airways in patients. Anaesthesia 2016; 71: 1399-403.
Mercer M. Respiratory failure after tracheal extubation in a patient with halo frame cervical spine immobilization–rescue therapy using the Combitube airway. Br J Anaesth 2001; 86: 886-91.
Yang JH, Kim YM, Chung HS, et al. Comparison of four manikins and fresh frozen cadaver models for direct laryngoscopic orotracheal intubation training. Emerg Med J 2010; 27: 13-6.
Author contributions
Joanna Gordon contributed to the design, acquisition, analysis, and interpretation of data and drafting of this article. Francesco Cavalli contributed to the analysis and interpretation of data and drafting the article. Vaughan Bertram contributed to the study conception and design; interpretation of data; and drafting the article. Matteo Parotto and Richard Cooper contributed to all aspects of this article including the conception and design; acquisition, analysis, and interpretation of data; and drafting the article.
Conflicts of interest
None. Richard M. Cooper is an unpaid consultant to Verathon.
Funding statement
This study was conducted with departmental resources.
Editorial responsibility
This submission was handled by Dr. Steven Backman, Associate Editor, Canadian Journal of Anesthesia.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is accompanied by an editorial. Please see Can J Anesth 2020; 67: this issue.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Gordon, J.K., Bertram, V.E., Cavallin, F. et al. Direct versus indirect laryngoscopy using a Macintosh video laryngoscope: a mannequin study comparing applied forces. Can J Anesth/J Can Anesth 67, 515–520 (2020). https://doi.org/10.1007/s12630-020-01583-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12630-020-01583-x