Abstract
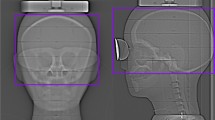
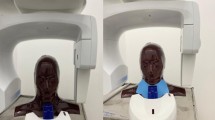
This study aimed to determine the placement distance, number, and position of the bismuth shield for developing a lens protective device for cone-beam computed tomography (CBCT). To determine the dose reduction rate, the lens doses were measured using an anthropomorphic head phantom and a real-time dosimeter. The image quality assessment was determined by analyzing the change in the pixel value, caused by the bismuth shield, and the artifact index was calculated from the pixel value and image noise within various regions of interest in the head phantom. When the distance between the bismuth shield and the subject was increased, the image quality deteriorated less, but there was also a decrease in the lens dose reduction rate. Upon changing the number of bismuth shields from 1-ply to 2-ply, the dose reduction rate increased; however, there was a decrease in the image quality. Additionally, placing the bismuth shield outside of the subject improved the dose reduction rate without deteriorating the image quality. The optimum placement conditions of the bismuth shield were concluded as follows: positioned outside, placed 10 mm from the surface of the subject, and used a 1-ply bismuth shield. When these placement conditions were used, the lens dose reduction rate was 26.9 ± 0.36% (right–left average) for the “bismuth shield: separate”. The protective device developed in this study will contribute to radiation dose reduction in CBCT scans.
















Similar content being viewed by others
References
Chida K, Inaba Y, Saito H, Ishibashi T, Takahashi S, Kohzuki M, et al. Radiation dose of interventional radiology system using a flat-panel detector. Am J Roentgenol. 2009;193:1680–5.
Chida K, Kaga Y, Haga Y, Kataoka N, Kumasaka E, Meguro T, et al. Occupational dose in interventional radiology procedures. Am J Roentgenol. 2013;200:138–41.
Chida K, Ohno T, Kakizaki S, Takegawa M, Yuuki H, Nakada M, et al. Radiation dose to the pediatric cardiac catheterization and intervention patient. Am J Roentgenol. 2010;195:1175–9.
Chida K, Saito H, Otani H, Kohzuki M, Takahashi S, Yamada S, et al. Relationship between fluoroscopic time, dose-area product, body weight, and maximum radiation skin dose in cardiac interventional procedures. Am J Roentgenol. 2006;186:774–8.
Chida K, Takahashi T, Ito D, Shimura H, Takeda K, Zuguchi M. Clarifying and visualizing sources of staff-received scattered radiation in interventional procedures. Am J Roentgenol. 2011;197:W900–3.
Ishii H, Chida K, Satsurai K, Haga Y, Kaga Y, Abe M, et al. A phantom study to determine the optimal placement of eye dosemeters on interventional cardiology staff. Radiat Prot Dosimetry. 2019;185:409–13.
Kawauchi S, Moritake T, Hayakawa M, Hamada Y, Sakuma H, Yoda S, et al. Estimation of maximum entrance skin dose during cerebral angiography. Nihon Hoshasen Gijutsu Gakkai Zasshi (in Japanese). 2015;71:746–57.
Matsunaga Y, Chida K, Kondo Y, Kobayashi K, Kobayashi M, Minami K, et al. Diagnostic reference levels and achievable doses for common computed tomography examinations: results from the Japanese nationwide dose survey. Br J Radiol. 2019;92:20180290.
Moritake T, Hayakawa M, Matsumaru Y, Takigawa T, Koguchi Y, Miyamoto Y, et al. Precise mapping system of entrance skin dose during endovascular embolization for cerebral aneurysm. Radiat Meas. 2011;46:2103–6.
Sánchez RM, Vañó E, Fernández JM, Rosati S, López-Ibor L. Radiation doses in patient eye lenses during interventional neuroradiology procedures. AJNR Am J Neuroradiol. 2016;37:402–7.
Kawauchi S, Chida K, Moritake T, Matsumaru Y, Hamada Y, Sakuma H, et al. Estimation of patient lens dose associated with C-arm cone-beam computed tomography usage during interventional neuroradiology. Radiat Prot Dosimetry. 2019;184:138–47.
Irie K, Murayama Y, Saguchi T, Ishibashi T, Ebara M, Takao H, et al. Dynact soft-tissue visualization using an angiographic C-arm system: initial clinical experience in the operating room. Neurosurgery. 2008;62:266–72.
Kanayama S, Hara T, Hamada Y, Matsumaru Y. Potential of 80-kV high-resolution cone-beam CT imaging combined with an optimized protocol for neurological surgery. Neuroradiology. 2015;57:155–62.
Struffert T, Richter G, Engelhorn T, Doelken M, Goelitz P, Kalender WA, et al. Visualisation of intracerebral haemorrhage with flat-detector CT compared to multislice CT: results in 44 cases. Eur Radiol. 2009;19:619–25.
Tsuruta W, Matsumaru Y, Hamada Y, Hayakawa M, Kamiya Y. Analysis of closed-cell intracranial stent characteristics using cone-beam computed tomography with contrast material. Neurol Med Chir (Tokyo). 2013;53:403–8.
Stewart FA, Akleyev AV, Hauer-Jensen M, Hendry JH, Kleiman NJ, MacVittie TJ, Aleman BM, Edgar AB, Mabuchi K, Muirhead CR, Shore RE, Wallace WH. ICRP publication 118: ICRP statement on tissue reactions and early and late effects of radiation in normal tissues and organs-threshold doses for tissue reactions in a radiation protection context. Ann ICRP. 2012;41:1–322.
Endo M, Haga Y, Sota M, Tanaka A, Otomo K, Murabayashi Y, et al. Evaluation of novel X-ray protective eyewear in reducing the eye dose to interventional radiology physicians. J Radiat Res. 2021;62:414–9.
Haga Y, Chida K, Kaga Y, Sota M, Meguro T, Zuguchi M. Occupational eye dose in interventional cardiology procedures. Sci Rep. 2017;7:569.
Kato M, Chida K, Ishida T, Toyoshima H, Yoshida Y, Yoshioka S, et al. Occupational radiation exposure of the eye in neurovascular interventional physician. Radiat Prot Dosimetry. 2019;185:151–6.
Wang C, Nguyen G, Toncheva G, Jiang X, Ferrell A, Smith T, et al. Evaluation of patient effective dose of neurovascular imaging protocols for C-arm cone-beam CT. AJR Am J Roentgenol. 2014;202:1072–7.
Kawauchi S, Chida K, Moritake T, Hamada Y, Matsumaru Y, Tsuruta W, et al. Treatment of internal carotid aneurysms using pipeline embolization devices: measuring the radiation dose of the patient and determining the factors affecting it. Radiat Prot Dosimetry. 2020;3:389.
Ciarmatori A, Nocetti L, Mistretta G, Zambelli G, Costi T. Reducing absorbed dose to eye lenses in head CT examinations: the effect of bismuth shielding. Australas Phys Eng Sci Med. 2016;39:583–9.
Colletti PM, Micheli OA, Lee KH. To shield or not to shield: application of bismuth breast shields. Am J Roentgenol. 2013;200:503–7.
Hopper KD. Orbital, thyroid, and breast superficial radiation shielding for patients undergoing diagnostic CT. Semin Ultrasound CT MR. 2002;23:423–7.
Hopper KD, Neuman JD, King SH, Kunselman AR. Radioprotection to the eye during CT scanning. AJNR Am J Neuroradiol. 2001;22:1194–8.
Kim JS, Kwon SM, Kim JM, Yoon SW. New organ-based tube current modulation method to reduce the radiation dose during computed tomography of the head: evaluation of image quality and radiation dose to the eyes in the phantom study. Radiol Med. 2017;122:601–8.
McLaughlin DJ, Mooney RB. Dose reduction to radiosensitive tissues in CT. Do commercially available shields meet the users’ needs? Clin Radiol. 2004;59:446–50.
Mehnati P, Malekzadeh R, Sooteh MY. Use of bismuth shield for protection of superficial radiosensitive organs in patients undergoing computed tomography: a literature review and meta-analysis. Radiol Phys Technol. 2019;12:6–25.
Nikupaavo U, Kaasalainen T, Reijonen V, Ahonen SM, Kortesniemi M. Lens dose in routine head CT: comparison of different optimization methods with anthropomorphic phantoms. Am J Roentgenol. 2015;204:117–23.
Raissaki M, Perisinakis K, Damilakis J, Gourtsoyiannis N. Eye-lens bismuth shielding in paediatric head CT: artefact evaluation and reduction. Pediatr Radiol. 2010;40:1748–54.
Wang J, Duan X, Christner JA, Leng S, Grant KL, McCollough CH. Bismuth shielding, organ-based tube current modulation, and global reduction of tube current for dose reduction to the eye at head CT. Radiology. 2012;262:191–8.
Kawauchi S, Chida K, Moritake T, Hamada Y, Tsuruta W. Radioprotection of eye lens using protective material in neuro cone-beam computed tomography: Estimation of dose reduction rate and image quality. Phys Med. 2021;82:192–9.
Liao YL, Lai NK, Tyan YS, Tsai HY. Bismuth shield affecting CT image quality and radiation dose in adjacent and distant zones relative to shielding surface: a phantom study. Biomed J. 2019;42:343–51.
Chida K, Kato M, Inaba Y, Kobayashi R, Nakamura M, Abe Y, et al. Real-time patient radiation dosimeter for use in interventional radiology. Phys Med. 2016;32:1475–8.
Inaba Y, Chida K, Murabayashi Y, Endo M, Otomo K, Zuguchi M. An initial investigation of a wireless patient radiation dosimeter for use in interventional radiology. Radiol Phys Technol. 2020;13:321–6.
Inaba Y, Nakamura M, Chida K, Zuguchi M. Effectiveness of a novel real-time dosimeter in interventional radiology: a comparison of new and old radiation sensors. Radiol Phys Technol. 2018;11:445–50.
Inaba Y, Nakamura M, Zuguchi M, Chida K. Development of novel real-time radiation systems using 4-channel sensors. Sensors (Basel). 2020;20:2741.
Kato M, Chida K, Nakamura M, Toyoshima H, Terata K, Abe Y. New real-time patient radiation dosimeter for use in radiofrequency catheter ablation. J Radiat Res. 2019;60:215–20.
Nakamura M, Chida K, Zuguchi M. Red emission phosphor for real-time skin dosimeter for fluoroscopy and interventional radiology. Med Phys. 2014;41:101913.
Nakamura M, Chida K, Zuguchi M. Novel dosimeter using a nontoxic phosphor for real-time monitoring of patient radiation dose in interventional radiology. Am J Roentgenol. 2015;205:W202–6.
Dong Y, Shi AJ, Wu JL, Wang RX, Sun LF, Liu AL, et al. Metal artifact reduction using virtual monochromatic images for patients with pedicle screws implants on CT. Eur Spine J. 2016;25:1754–63.
Kuya K, Shinohara Y, Kato A, Sakamoto M, Kurosaki M, Ogawa T. Reduction of metal artifacts due to dental hardware in computed tomography angiography: assessment of the utility of model-based iterative reconstruction. Neuroradiology. 2017;59:231–5.
Lin XZ, Miao F, Li JY, Dong HP, Shen Y, Chen KM. High-definition CT Gemstone spectral imaging of the brain: initial results of selecting optimal monochromatic image for beam-hardening artifacts and image noise reduction. J Comput Assist Tomogr. 2011;35:294–7.
Kim DJ, Park MK, Jung DE, Kang JH, Kim BM. Radiation dose reduction without compromise to image quality by alterations of filtration and focal spot size in cerebral angiography. Korean J Radiol. 2017;18:722–8.
Acknowledgements
This study was supported by JSPS KAKENHI Grant No: JP19K17183. This study was partly supported by a research award grant from the Japanese Society of Radiological Technology, Tokyo branch.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Research involving human participants
This article does not contain any studies with human participants.
Research involving animals
This article does not contain any studies involving animals.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Kawauchi, S., Chida, K., Hamada, Y. et al. Lens dose reduction with a bismuth shield in neuro cone-beam computed tomography: an investigation on optimum shield device placement conditions. Radiol Phys Technol 15, 25–36 (2022). https://doi.org/10.1007/s12194-021-00644-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12194-021-00644-0