Abstract
Background
Oral submucous fibrosis (OSMF) is a habit related potentially malignant disorder seen mainly in South Asian people. The malignancy arising from OSMF has been regarded as low grade with better outcome. The present study was orchestrated to histochemically analyze collagen and elastic fibres in OSMF without dysplasia, OSMF with dysplasia and OSMF turning malignant.
Materials and Methods
100 cases (80 cases and 20 healthy controls) were included after obtaining clearance from ethical committee. All cases were subjected to Van Gieson staining for collagen and a novel simple method for elastic fibres (Orcein staining). Data were analyzed using SPSS software.
Results
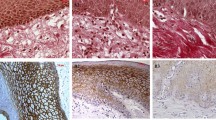
Controls showed haphazard arrangement of collagen and elastic fibres. The collagen bundles were parallelly arranged in OSMF without dysplasia and OSMF with dysplasia; the collagen was however haphazard in cases of OSMF turning malignant. As with collagen, elastic fibres were also haphazardly arranged in the control group; in contrast, the elastic fibres were predominantly arranged in a criss-cross pattern in the other study groups. The difference in orientation and density among the groups was statistically significant.
Conclusion
With advancement of stage there is increased collagenization of OSMF, as the condition acquires dysplastic changes and turns malignant, microenvironment alters resulting in increased activity of collagenases. However, the arrangement of more resistant elastic fibres depicts the better outcome, once OSMF shows malignant transformation, limiting locoregional and distant spread.



Similar content being viewed by others
References
Parola M, Pinzani M (2019) Liver fibrosis: pathophysiology, pathogenetic targets and clinical issues. Mol Aspects Med 65:37–55
Noble PW, Barkauskas CE, Jiang D (2012) Pulmonary fibrosis: patterns and perpetrators. J Clin Invest 122(8):2756–2762
Pindborg JJ, Sirsat SM (1966) Oral submucous fibrosis. Oral Surg Oral Med Oral Pathol 22(6):764–779
Sirsat SM, Pindborg JJ (1967) The vascular response in early and advanced oral submucous fibrosis. Acta Pathol Microbiol Scand 70(2):179–184
Sirsat SM, Pindborg JJ (1967) Subepithelial changes in oral submucous fibrosis. Acta Pathol Microbiol Scand 70(2):161–173
Pandiar D, Krishnan RP, Ramani P, Anand R, Sarode S (2023) Oral submucous fibrosis and the malignancy arising from it, could best exemplify the concepts of cuproplasia and cuproptosis. J Stomatol Oral Maxillofac Surg 124(1S):101368
Pandiar D, Shameena P (2014) Immunohistochemical expression of CD34 and basic fibroblast growth factor (bFGF) in oral submucous fibrosis. J Oral Maxillofac Pathol 18(2):155–161
Utsunomiya H, Tilakaratne WM, Oshiro K, Maruyama S, Suzuki M, Ida-Yonemochi H et al (2005) Extracellular matrix remodeling in oral submucous fibrosis: its stage-specific modes revealed by immunohistochemistry and in situ hybridization. J Oral Pathol Med 34(8):498–507
Chaturvedi P, Vaishampayan SS, Nair S, Nair D, Agarwal JP, Kane SV et al (2013) Oral squamous cell carcinoma arising in background of oral submucous fibrosis: a clinicopathologically distinct disease. Head Neck 35(10):1404–1409
Sarode SC, Sarode GS (2013) Better grade of tumor differentiation of oral squamous cell carcinoma arising in background of oral submucous fibrosis. Med Hypotheses 81(4):540–543
Gadbail AR, Korde S, Chaudhary MS, Sarode SC, Gondivkar SM, Dande R et al (2020) Ki67, CD105, and α-SMA expression supports biological distinctness of oral squamous cell carcinoma arising in the background of oral submucous fibrosis. Asian Pac J Cancer Prev 21(7):2067–2074
Kujan O, Mello FW, Warnakulasuriya S (2021) Malignant transformation of oral submucous fibrosis: a systematic review and meta-analysis. Oral Dis 27(8):1936–1946
Murthy V, Mylonas P, Carey B, Yogarajah S, Farnell D, Addison O et al (2022) Malignant transformation rate of oral submucous fibrosis: a systematic review and meta-analysis. J Clin Med 11(7):1793
Cai X, Yao Z, Liu G, Cui L, Li H, Huang J (2019) Oral submucous fibrosis: a clinicopathological study of 674 cases in China. J Oral Pathol Med 48(4):321–325
Angadi PV, Rekha KP (2011) Oral submucous fibrosis: a clinicopathologic review of 205 cases in indians. Oral Maxillofac Surg 15(1):15–19
Gadbail AR, Chaudhary M, Gawande M, Hande A, Sarode S, Tekade SA et al (2017) Oral squamous cell carcinoma in the background of oral submucous fibrosis is a distinct clinicopathological entity with better prognosis. J Oral Pathol Med 46(6):448–453
Pandiar D, Ramani P, Krishnan RP, Thamilselvan S, Viswasini DR (2022) Spindle cell squamous cell carcinoma of alveolus with heterologous mesenchymal differentiation and synchronous contralateral buccal squamous cell carcinoma in a background of oral submucous fibrosis: recapitulation of embryonic plasticity? Oral Oncol 124:105476
Ganganna K, Shetty P, Shroff SE (2012) Collagen in histologic stages of oral submucous fibrosis: a polarizing microscopic study. J Oral Maxillofac Pathol 16(2):162–166
Chiu CJ, Chang ML, Chiang CP, Hahn LJ, Hsieh LL, Chen CJ (2002) Interaction of collagen-related genes and susceptibility to betel quid-induced oral submucous fibrosis. Cancer Epidemiol Biomarkers Prev 11(7):646–653
Kuo MY, Chen HM, Hahn LJ, Hsieh CC, Chiang CP (1995) Collagen biosynthesis in human oral submucous fibrosis fibroblast cultures. J Dent Res 74(11):1783–1788
Smitha B, Donoghue M (2011) Clinical and histopathological evaluation of collagen fiber orientation in patients with oral submucous fibrosis. J Oral Maxillofac Pathol 15(2):154–160
Tilakaratne WM, Klinikowski MF, Saku T, Peters TJ, Warnakulasuriya S (2006) Oral submucous fibrosis: review on aetiology and pathogenesis. Oral Oncol 42(6):561–568
Gray ST, Wilkins RJ, Yun K (1992) Interstitial collagenase gene expression in oral squamous cell carcinoma. Am J Pathol 141(2):301–306
Mashhadiabbas F, Mahjour F, Mahjour SB, Fereidooni F, Hosseini FS (2012) The immunohistochemical characterization of MMP-2, MMP-10, TIMP-1, TIMP-2, and podoplanin in oral squamous cell carcinoma. Oral Surg Oral Med Oral Pathol Oral Radiol 114(2):240–250
Mishev G, Deliverska E, Hlushchuk R, Velinov N, Aebersold D, Weinstein F et al (2014) Prognostic value of matrix metalloproteinases in oral squamous cell carcinoma. Biotechnol Biotechnol Equip 28(6):1138–1149
Bishen KA, Radhakrishnan R, Satyamoorthy K (2008) The role of basic fibroblast growth factor in oral submucous fibrosis pathogenesis. J Oral Pathol Med 37(7):402–411
Funding
The authors have not disclosed any funding.
Author information
Authors and Affiliations
Contributions
DP: acquisition of data, conception and design, analysis and interpretation of data, and drafting of the manuscript; AE: acquisition of data and histochemical procedures, review; RPK: acquisition of images and final revision of the article.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Ethical Approval
Ethical approval was granted by the Institutional Human Ethics Committee (IHEC/SDC/FACULTY/22/OPATH/217).
Informed Consent
For retrospective study formal consent is not required.
Additional information
Publisher’s Note
Springer nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Pandiar, D., Aswani, E. & Krishnan, R.P. Qualitative Assessment of Collagen and Elastic Fibers in Oral Submucous Fibrosis (OSMF), OSMF with Dysplasia and Oral Squamous Cell Carcinoma Arising from OSMF: A Histochemical Study. Head and Neck Pathol 17, 932–939 (2023). https://doi.org/10.1007/s12105-023-01591-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12105-023-01591-5