Abstract
Background
Hepatocellular cancer (HCC) typically arises in the background of cirrhosis. The epidemiology of HCC has changed in recent years due to availability of newer antivirals, changing life-styles and greater possibility for early detection. We undertook a multicentric national sentinel surveillance for liver cirrhosis and HCC to assess the attributable risk factors for the development of HCC, both with and without a background of cirrhosis.
Methods
Data from January 2017 till August 2022 from hospital-based records of eleven participating centers were included. Diagnosed cases of cirrhosis [radiological (multiphase and/or histopathological] and HCC [as per AASLD 2018] were included. History of significant alcohol intake was elicited by AUDIT-C questionnaire.
Results
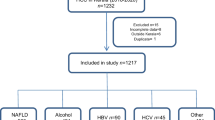
Altogether 5798 enrolled patients were assessed, of which 2664 patients had HCC. The mean age was 58.2 ± 11.7 years and 84.3% (n = 2247) were males. Diabetes was found in over a third of those with HCC (n = 1032;39.5%). The most common etiology of HCC was NAFLD (n = 927;35.5%) followed by viral hepatitis B and C and harmful levels of alcohol. Among those with HCC, 27.9% (n = 744) had no cirrhosis. Higher proportion of cirrhotic HCC patients had alcohol as an etiological factor as compared to non-cirrhotic (17.5 vs. 4.7%, p ≤ 0.001). NAFLD was an etiological factor for a higher proportion of non-cirrhotic HCC patients as compared to cirrhotic HCC (48.2 vs. 30.6%, p ≤0.001). Diabetics more commonly had non-cirrhotic HCC (50.5 vs. 35.2%). The following factors were associated with an occurrence of cirrhotic HCC: male gender (OR 1.372 and 95% CI 1.070–1.759), age above 60 years (OR 1.409 and 95% CI 1.176–1.689), HBV (OR 1.164 and 95% CI 0.928–1.460), HCV (OR 1.228 and 95 CI 0.964–1.565) and harmful consumption of alcohol (OR 3.472 and 95% CI 2.388–5.047). The adjusted odds of non-cirrhotic patients having NAFLD was 1.553 (95% CI 1.290–1.869).
Conclusion
This large multi-centric study demonstrates that NAFLD is the most important risk factor for development of both cirrhotic and non-cirrhotic HCC in India and has overtaken viral hepatitis. Awareness campaigns and large-scale screening are required to reduce the high burden of NAFLD-related HCC in India.


Similar content being viewed by others
Data availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- HCC:
-
Hepato-cellular carcinoma
- AASLD:
-
American Association for the Study of Liver Diseases
- AUDIT-C:
-
Alcohol use disorders identification test-concise
- NAFLD:
-
Non-alcoholic fatty liver disease
- HBV:
-
Hepatitis B virus
- HCV:
-
Hepatitis C virus
- ILBS:
-
Institute of Liver and Biliary Sciences
- CT:
-
Computed tomography
- MRI:
-
Magnetic resonance imaging
- OPD:
-
Outpatient department
- IPD:
-
Inpatient department
- IBM:
-
International business machines
- SPSS:
-
Statistical package for the social sciences
- IQR:
-
Interquartile range
- AFLD:
-
Alcoholic fatty liver disease
References
Schuppan D, Afdhal NH. Liver Cirrhosis. Lancet 2008;371(9615):838–851
Altekruse SF, Devesa SS, Dickie LA, McGlynn KA, Kleiner DE. Histological classification of liver and intrahepatic bile duct cancers in SEER registries. J Registry Manag 2011;38:201–205
EASL–EORTC Clinical Practice Guideline Management of hepatocellular carcinoma. J Hepatol 2012;56:908–943
Paul SB, Chalamalasetty B, Vishnubatla S. Clinical profile, etiology and therapeutic outcome in 324 hepatocellular cancer in India. Oncology 2009;77:162–171
Thomas London W, Petrick JL, McGlynn KA. Liver cancer. In Thun M, Linet MS, Cerhan JR, Haiman CA, Schottenfeld D, editors., Cancer epidemiology and prevention. 4th ed. Oxford University Press; 2018. 635–660
Marengo A, Rosso C, Bugianesi E. Liver cancer: connections with obesity, fatty liver, and cirrhosis. Annu Rev Med 2016;67:103–117
Sulkowski MS, Gardiner DF, Rodriguez-Torres M, Reddy KR, Hassanein T, Jacobson I, et al. Daclatasvir plus sofosbuvir for previously treated or untreated chronic HCV infection. N Engl J Med 2014;370:211–221
Younossi Z, Stepanova M, Ong JP, Jacobson IM, Bugianesi E, Duseja A, et al. Nonalcoholic steatohepatitis is the fastest growing cause of hepatocellular carcinoma in liver transplant candidates. Clin Gastroenterol Hepatol 2019;17:748–755
Marrero JA, Kulik LM, Sirlin CB, Zhu AX, Finn RS, Abecassis MM, et al. Diagnosis, staging, and management of hepatocellular carcinoma: 2018 practice guidance by the american association for the study of liver diseases. Hepatology 2018;68:723–750
Bush K, Kivlahan DR, McDonell MB, Fihn SD, Bradley KA. The AUDIT alcohol consumption questions (AUDIT-C): an effective brief screening test for problem drinking. Ambulatory Care Quality Improvement Project (ACQUIP). Alcohol Use Disorders Identification Test. Arch Intern Med 1998;158(16):1789–1795. https://doi.org/10.1001/archinte.158.16.1789
Kumar R, Saraswat MK, Sharma BC, Sakhuja P, Sarin SK. Characteristics of hepatocellular carcinoma in India: a retrospective analysis of 191 cases. QJM 2008;101:479–485
Sherman M. Hepatocellular carcinoma: epidemiology, surveillance, and diagnosis. Semin Liver Dis 2010;30:3–16
Zhu RX, Seto WK, Lai CL, Yuen MF. Epidemiology of hepatocellular carcinoma in the Asia-Pacific Region. Gut Liver 2016;10:332–339
Tham J, Goh TL, Barclay S, Priest M, Forrest E, Fraser A, et al. P221 Non-cirrhotic vs. Cirrhotic HCC: comparison between patient characteristics, aetiology and outcomes. Gut 2021;70:157–158
Castán A, Navarro Y, Sarría L, Larrosa R, Serradilla M, Serrablo A. Radiological diagnosis of hepatocellular carcinoma in non-cirrhotic patients. Hepatoma Res 2017;3:1
Trevisani F, Frigerio M, Santi V, Grignaschi A, Bernardi M. Hepatocellular carcinoma in non-cirrhotic liver: a reappraisal. Dig Liver Dis 2010;42:341–347
Kumar M, Kumar R, Hissar SS, Saraswat MK, Sharma BC, Sakhuja P, et al. Risk factors analysis for hepatocellular carcinoma in patients with and without cirrhosis: a case-control study of 213 hepatocellular carcinoma patients from India. J Gastroenterol Hepatol 2007;22:1104–1111
Sarin SK, Thakur V, Guptan RC, Saigal S, Malhotra V, Thyagarajan SP, et al. Profile of hepatocellular carcinoma in India: an insight into the possible etiologic associations. J Gastroenterol Hepatol 2001;16:666–673
Sanyal AJ, Yoon SK, Lencioni R. The etiology of hepatocellular carcinoma and consequences for treatment. Oncologist 2010;15(Suppl 4):14–22
Chayanupatkul M, Omino R, Mittal S, Kramer JR, Richardson P, El-Serag HB, et al. 12 the risk factors of hepatocellular carcinoma (HCC) in non-cirrhotic chronic hepatitis B patients in United States Veterans. Gastroenterology 2016;150:S4
el-Refaie A, Savage K, Bhattacharya S, Khakoo S, Harrison TJ, el-Batanony M, et al. HCV-associated hepatocellular carcinoma without cirrhosis. J Hepatol 1996;24:277–285
Nash KL, Woodall T, Brown AS, Davies SE, Alexander GJ. Hepatocellular carcinoma in patients with chronic hepatitis C virus infection without cirrhosis. World J Gastroenterol 2010;16:4061–4065
Alotaibi AS, Alghamdi W, Marotta P, Qumosani K. A266 hepatocellular carcinoma prevalence in non-cirrhotic hepatitis C patients. J Can Assoc Gastroenterol 2018;1:383–384
Perumpail RB, Liu A, Wong RJ, Ahmed A, Harrison SA. Pathogenesis of hepatocarcinogenesis in non-cirrhotic nonalcoholic fatty liver disease: potential mechanistic pathways. World J Hepatol 2015;7:2384–2388
Piñero F, Pages J, Marciano S, Fernández N, Silva J, Anders M, et al. Fatty liver disease, an emerging etiology of hepatocellular carcinoma in Argentina. World J Hepatol 2018;10:41–50
Alexander J, Torbenson M, Wu TT, Yeh MM. Non-alcoholic fatty liver disease contributes to hepatocarcinogenesis in non-cirrhotic liver: a clinical and pathological study. J Gastroenterol Hepatol 2013;28:848–854
Margini C, Dufour JF. The story of HCC in NAFLD: from epidemiology, across pathogenesis, to prevention and treatment. Liver Int 2016;36:317–324
Balakrishnan M, El-Serag HB. Editorial: NAFLD-related hepatocellular carcinoma—increasing or not? With or without cirrhosis? Aliment Pharmacol Ther 2018;47:437–438
Mancina RM, Dongiovanni P, Petta S, Pingitore P, Meroni M, Rametta R, et al. The MBOAT7-TMC4 variant rs641738 increases risk of nonalcoholic fatty liver disease in individuals of European descent. Gastroenterology 2016;150(5):1219–1230
Donati B, Dongiovanni P, Romeo S, Meroni M, McCain M, Miele L, et al. MBOAT7 rs641738 variant and hepatocellular carcinoma in non-cirrhotic individuals. Sci Rep 2017;7(1):4492
Papatheodoridi AM, Chrysavgis L, Koutsilieris M, Chatzigeorgiou A. The role of senescence in the development of nonalcoholic fatty liver disease and progression to nonalcoholic steatohepatitis. Hepatology 2020;71:363–374
Bhatti HBA, Sheikh EAA, Mahmud SU, Zeeshan S, Khan NY, Zia HH, et al. Clinical profile and treatment of hepatocellular carcinoma: a single-center experience. South Asian J Cancer 2021;10(2):76–80
Saini N, Bhagat A, Sharma S, Duseja A, Chawla Y. Evaluation of clinical and biochemical parameters in hepatocellular carcinoma: experience from an Indian center. Clin Chim Acta 2006;371:183–186
Sood A, Midha V, Goyal O, Goyal P, Sood N, Sharma SK. Profile of hepatocellular carcinoma in a tertiary care hospital in Punjab in northern India. Indian J Gastroenterol 2014;33:35–40
Pal S, Ramachandran J, Kurien RT, Eapen A, Ramakrishna B, Keshava SN, et al. Hepatocellular carcinoma continues to be diagnosed in the advanced stage: profile of hepatocellular carcinoma in a tertiary care hospital in South India. Trop Doct 2013;43:25–26
David D, Raghavendran A, Goel A, Bharath Kumar C, Kodiatte TA, Burad D, et al. Risk factors for non-alcoholic fatty liver disease are common in patients with non-B non-C hepatocellular carcinoma in India. Indian J Gastroenterol 2017;36:373–379
Musunuri B, Shetty S, Bhat G, Udupa K, Pai A. Profile of patients with hepatocellular carcinoma: an experience from a tertiary care center in India. Indian J Gastroenterol 2022;41(2):127–134. https://doi.org/10.1007/s12664-021-01209-0
Acknowledgements
We appreciate the efforts of all the collaborators for WHOCC study titled ‘Surveillance of Etiological factors for Cirrhosis and Hepatocellular Carcinoma’.
Funding
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data analysis and first draft was done by TP. SKS commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
Tushar Prabhakar, Kanica Kaushal, Manya Prasad, Ekta Gupta, Ajit Sood, Ajay K. Jain, Akash Shukla, Ashish Goel, Ajay Duseja, Anoop Saraya, Samir Shah, Guresh Kumar, Shiv Kumar Sarin have no relevant financial or non-financial interests to disclose.
Ethical approval
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2008 (5). Informed consent was waived off due to the record review and surveillance mode of data collection. Institutional Ethics Committee allowed the same (No. IEC/2020/73/NA06).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Prabhakar, T., Kaushal, K., Prasad, M. et al. Etiologic fractions in patients of hepatocellular carcinoma in India with and without a background of cirrhosis: a multi-centric study. Hepatol Int 17, 745–752 (2023). https://doi.org/10.1007/s12072-023-10498-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12072-023-10498-w