Abstract
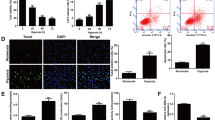
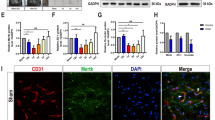
Therapy targeting the neurovascular unit may provide effective neuroprotection against neonatal hypoxia–ischemia (HI). We hypothesized that the peripheral injection of hypoxia-preconditioned human umbilical vein endothelial cells (HUVECs) following HI protects against neurovascular damage and provides long-term neuroprotection in a postpartum (P) day-7 rat pup model. Compared with normoxic HUVECs, hypoxic HUVECs showed enhanced migration and angiogenesis in vitro and had augmented migration effects into the brain when administered intraperitoneally in vivo after HI. Moreover, 24 and 72 h post-HI, the hypoxic HUVECs group but not the normoxic HUVECs or culture-medium groups had significantly higher preservation of microvessels and neurons, and attenuation of blood–brain barrier damage than the normal-saline group. Compared to control or normal-saline groups, only the hypoxic HUVECs group had no impaired foot steps and showed a significant reduction of brain area loss at P42. Next-generation sequencing showed hypoxia-induced upregulation and downregulation of 209 and 215 genes in HUVECs, respectively. Upstream regulator analysis by ingenuity pathway analysis (IPA) identified hypoxia-inducible factor 1-alpha as the key predicted activated transcription regulator. After hypoxia, 12 genes (ADAMTS1, EFNA1, HIF1A, LOX, MEOX2, SELE, VEGFA, VEGFC, CX3CL1, HMMR, SDC, and SERPINE) associated with migration and/or angiogenesis were regulated in HUVECs. In addition, 6 genes (VEGFA, VEGFC, NTN4, TGFA, SERPINE1, and CX3CL1) involved in the survival of endothelial and neuronal cells were also markedly altered in hypoxic HUVECs. Thus, cell therapy by using hypoxic HUVECs that enhance migration and neurovascular protection may provide an effective therapeutic strategy for treating neonatal asphyxia.








Similar content being viewed by others
References
Ferriero DM (2004) Neonatal brain injury. N Engl J Med 351(19):1985–1995. https://doi.org/10.1056/NEJMra041996
Johnston MV, Fatemi A, Wilson MA, Northington F (2011) Treatment advances in neonatal neuroprotection and neurointensive care. Lancet Neurol 10(4):372–382. https://doi.org/10.1016/S1474-4422(11)70016-3
Gluckman PD, Wyatt JS, Azzopardi D, Ballard R, Edwards AD, Ferriero DM, Polin RA, Robertson CM et al (2005) Selective head cooling with mild systemic hypothermia after neonatal encephalopathy. Lancet 365(9460):663–670. https://doi.org/10.1016/S0140-6736(05)17946-X
Shankaran S, Laptook AR, Ehrenkranz RA, Tyson JE, McDonald SA, Donovan EF, Fanaroff AA, Poole WK et al (2005) Whole-body hypothermia for neonates with hypoxic-ischemic encephalopathy. N Engl J Med 353(15):1574–1584. https://doi.org/10.1056/NEJMcps050929
Azzopardi DV, Strohm B, Edwards AD, Dyet L, Halliday HL, Juszczak E, Kapellou O, Levene M et al (2009) Moderate hypothermia to treat perinatal asphyxial encephalopathy. N Engl J Med 361(14):1349–1358. https://doi.org/10.1056/NEJMoa0900854
Shankaran S, Pappas A, McDonald SA, Vohr BR, Hintz SR, Yolton K, Gustafson KE, Leach TM et al (2012) Childhood outcomes after hypothermia for neonatal encephalopathy. N Engl J Med 366(22):2085–2092. https://doi.org/10.1056/NEJMoa1112066
Azzopardi D, Strohm B, Marlow N, Brocklehurst P, Deierl A, Eddama O, Goodwin J, Halliday HL et al (2014) Effects of hypothermia for perinatal asphyxia on childhood outcomes. N Engl J Med 371(2):140–149. https://doi.org/10.1056/NEJMoa1315788
Quaegebeur A, Lange C, Carmeliet P (2011) The neurovascular link in health and disease: molecular mechanisms and therapeutic implications. Neuron 71(3):406–424. https://doi.org/10.1016/j.neuron.2011.07.013
Hawkins BT, Davis TP (2005) The blood-brain barrier/neurovascular unit in health and disease. Pharmacol Rev 57(2):173–185. https://doi.org/10.1124/pr.57.2.4
Lee HT, Chang YC, YF T et al (2009) VEGF-A/VEGFR-2 signaling leading to camp response element-binding protein phosphorylation is a shared pathway underlying the protective effect of preconditioning on neurons and endothelial cells. J Neurosci 29(14):4356–4368. https://doi.org/10.1523/JNEUROSCI.5497-08.2009
Moretti R, Pansiot J, Bettati D et al (2015) Blood-brain barrier dysfunction in disorders of the developing brain. Front Neurosci 9:40
Lee BF, Wang LW, Lin SH, Jhuo TJ, Chiu NT, Huang CC, Hsia CC, Shen LH (2012) Tc-99m-HL91 imaging in early detection of neuronal injury in a neonatal rat model of hypoxic ischemia. Crit Care Med 40(6):1930–1938. https://doi.org/10.1097/CCM.0b013e31824e1883
Hsu YC, Chang YC, Lin YC, Sze CI, Huang CC, Ho CJ (2014) Cerebral microvascular damage occurs early after hypoxia-ischemia via nNOS activation in neonatal brain. J Cereb Blood Flow & Metab 34(4):668–676. https://doi.org/10.1038/jcbfm.2013.244
Tam SJ, Watts RJ (2010) Connecting vascular and nervous system development: angiogenesis and the blood-brain barrier. Ann Rev Neurosci 33(1):379–408. https://doi.org/10.1146/annurev-neuro-060909-152829
Tu YF, Lu PJ, Huang CC (2012) Moderate dietary restriction reduces p53-mediated neurovascular damage and microglia activation after hypoxic ischemia in neonatal brain. Stroke 43:491–498
Mouhieddine TH, Kobeissy FH, Itani M, Nokkari A, Wang KK (2014) Stem cells in neuroinjury and neurodegenerative disorders: challenges and future neurotherapeutic prospects. Neural Regen Res 9(9):901–906. https://doi.org/10.4103/1673-5374.133129
Titomanlio L, Kavelaars A, Dalous J, Mani S, el Ghouzzi V, Heijnen C, Baud O, Gressens P (2011) Stem cell therapy for neonatal brain injury: perspectives and challenges. Ann Neurol 70(5):698–712. https://doi.org/10.1002/ana.22518
Aleynik A, Gernavage KM, Mourad YSH, Sherman LS, Liu K, Gubenko YA, Rameshwar P (2014) Stem cell delivery of therapies for brain disorders. Clinical and Translational Medicine 3(1):24. https://doi.org/10.1186/2001-1326-3-24
Wu CC, Chen YC, Chang YC et al (2013) Human umbilical vein endothelial cells protect against hypoxic-ischemic damage in neonatal brain via SDF-1/CXCR4. Stroke 44:1402–1409
Cruz FF, Rocco PRM (2015) Hypoxic preconditioning enhances mesenchymal stromal cell lung repair capacity. Stem Cell Res Ther 6(1):130. https://doi.org/10.1186/s13287-015-0120-3
Jiang YZ, Li Y, Wang K, Dai CF, Huang SA, Chen DB, Zheng J (2014) Distinic roles of HIF1A in endothelial adaptations to physiological and ambient oxygen. Mol Cell Endocrinol 391(1-2):60–67. https://doi.org/10.1016/j.mce.2014.04.008
Baudin B, Bruneel A, Bosselut N, Vaubourdolle M (2007) A protocol for isolation and culture of human umbilical vein endothelial cells. Nat Protoc 2(3):481–485. https://doi.org/10.1038/nprot.2007.54
Izuta H, Chikaraishi Y, Shimazawa M, Mishima S, Hara H (2009) 10-Hydroxy-2-decenoic acid, a major fatty acid from royal jelly, inhibits VEGF-induced angiogenesis in human umbilical vein endothelial cells. Evid Based Complement Alternat Med 6(4):489–494. https://doi.org/10.1093/ecam/nem152
Koyanagi S, Tanigawa N, Nakagawa H, Soeda S, Shimeno H (2003) Oversulfation of fucoidan enhances its anti-angiogenic and antitumor activities. Biochem Pharmacol 65(2):173–179. https://doi.org/10.1016/S0006-2952(02)01478-8
Li J, Cubbon RM, Wilson LA, Amer MS, McKeown L, Hou B, Majeed Y, Tumova S et al (2011) Orai1 and CRAC channel dependence of VEGF-activated Ca2+ entry and endothelial tube formation. Circ Res 108(10):1190–1198. https://doi.org/10.1161/CIRCRESAHA.111.243352
Tu YF, Jiang ST, Chow YH et al (2016) Insulin receptor substrate-1 activation mediated p53 downregulation protects against hypoxic-ischemia in the neonatal brain. Mol Neurobiol 53:3658–3669
Germanò A, Caffo M, Angileri FF et al (2007) NMDA receptor antagonist felbamate reduces behavioral deficits and blood-brain barrier permeability changes after experimental subarachnoid hemorrhage in the rat. J Neurotrauma 24(4):732–744. https://doi.org/10.1089/neu.2006.0181
Hung PL, Huang CC, DG T et al (2013) Thyroxin treatment protects against white matter injury in the immature brain via brain-derived neurotrophic factor. Stroke 44(8):2275–2283. https://doi.org/10.1161/STROKEAHA.113.001552
Paxinos G, Watson C (1986) The rat brain in stereotaxic coordinates. Academic Press, New York
Bouras C, Kövari E, Herrmann FR, Rivara CB, Bailey TL, von Gunten A, Hof PR, Giannakopoulos P (2006) Stereologic analysis of microvascular morphology in the elderly: Alzheimer disease pathology and cognitive status. J Neuropathol Exp Neurol 65(3):235–244. https://doi.org/10.1097/01.jnen.0000203077.53080.2c
Liu H, Liu S, Li Y, Wang X, Xue W, Ge G, Luo X (2012) The role of SDF-1-CXCR4/ CXCR7 axis in the therapeutic effects of hypoxia-preconditioned mesenchymal stem cells for renal ischemia/reperfusion injury. PLoS One 7(4):e34608. https://doi.org/10.1371/journal.pone.0034608
Wei N, SP Y, Gu X et al (2013) Delayed intranasal delivery of hypoxic-preconditioned bone marroe mesenchymal stem cells enhanced cell homing and therapeutic benefits after ischemic stroke in mice. Cell Transplant 22(6):977–991. https://doi.org/10.3727/096368912X657251
Yu X, Lu C, Liu H, Rao S, Cai J, Liu S, Kriegel AJ, Greene AS et al (2013) Hypoxic preconditioning with cobalt of bone marrow mesenchymal stem cells improves cell migration and enhances therapy for treatment of ischemic acute kidney injury. PLoS One 8(5):e62703. https://doi.org/10.1371/journal.pone.0062703
Chacko SM, Ahmed S, Selvendiran K, Kuppusamy ML, Khan M, Kuppusamy P (2010) Hypoxic preconditioning induces the expression of prosurvival and proangiogenic markers in mesenchymal stem cells. Am J Physiol Cell Physiol 299(6):C1562–C1570. https://doi.org/10.1152/ajpcell.00221.2010
Tsai CC, Yew TL, Yang DC, Huang WH, Hung SC (2012) Benefits of hypoxic culture on bone marrow multipotent stromal cells. Am J Blood Res 2(3):148–159
Yu Y, RX W, Gao LN et al (2016) Stromal cell-derived factor-1-directed bone marrow mesenchymal stem cell migration in response to inflammatory and/or hypoxic stimuli. Cell Adhes Migr 8:1–18
Eichmann A, Simons M (2005) VEGF signaling inside vascular endothelial cells and beyond. Curr Opin Cell Biol 24:188–193
Cheng N, Brantley DM, Liu H, Lin Q, Enriquez M, Gale N, Yancopoulos G, Cerretti DP et al (2002) Blockade of EphA receptor tyrosine kinase activation inhibits vascular endothelial cell growth factor-induced angiogenesis. Mol Cancer Res 1(1):2–11
Hunter SG, Zhuang G, Brantley-Sieders D, Swat W, Cowan CW, Chen J (2006) Essential role of Vav family guanine nucleotide exchange factors in EphA receptor-mediated angiogenesis. Mol Cell Biol 26(13):4830–4842. https://doi.org/10.1128/MCB.02215-05
Baker AM, Bird D, Welti JC, Gourlaouen M, Lang G, Murray GI, Reynolds AR, Cox TR et al (2013) Lysyl oxidase plays a critical role in endothelial cell stimulation to drive tumor angiogenesis. Cancer Res 73(2):583–594. https://doi.org/10.1158/0008-5472.CAN-12-2447
Kumar P, Amin MA, Harlow LA, Polverini PJ, Koch AE (2003) Src and phosphatidylinositol 3–kinase mediate soluble E-selectin–induced angiogenesis. Blood 101(10):3960–3968. https://doi.org/10.1182/blood-2002-04-1237
Namiki A, Brogi E, Kearney M, Kim EA, Wu T, Couffinhal T, Varticovski L, Isner JM (1995) Hypoxia induces vascular endothelial growth factor in cultured human endothelial cells. J Biol Chem 270(52):31189–31195. https://doi.org/10.1074/jbc.270.52.31189
Forsythe JA, Jiang BH, Iyer NV, Agani F, Leung SW, Koos RD, Semenza GL (1996) Activation of vascular endothelial growth factor gene transcription by hypoxia-inducible factor 1. Mol Cell Biol 16(9):4604–4613. https://doi.org/10.1128/MCB.16.9.4604
Borentain P, Carmona S, Mathieu S, Jouve E, el-Battari A, Gérolami R (2016) Inhibition of E-selectin expression on the surface of endothelial cells inhibits hepatocellular carcinoma growth by preventing tumor angiogenesis. Cancer Chemother Pharmacol 77(4):847–856. https://doi.org/10.1007/s00280-016-3006-x
Hatipoglu OF, Hirohata S, Cilek MZ (2009) ADAMTS1 is a unique hypoxic early response gene expressed by endothelial cells. J Biol Chem 284(24):16325–16333. https://doi.org/10.1074/jbc.M109.001313
Patel S, Leal AD, Gorski DH (2005) The homeobox gene Gax inhibits angiogenesis through inhibition of nuclear factor-kappaB-dependent endothelial cell gene expression. Cancer Res 65(4):1414–1424. https://doi.org/10.1158/0008-5472.CAN-04-3431
Zhang J, Li X, Chai S, Wang X (2015) Neuroprotective effect of lentivirus mediated VEGF on rat model with cerebral ischemic injury. Int J Clin Exp Med 8(3):4094–4100
Horie N, Pereira MP, Niizuma K, Sun G, Keren-Gill H, Encarnacion A, Shamloo M, Hamilton SA et al (2011) Transplanted stem cell-secreted vascular endothelial growth factor effects poststroke recovery, inflammation, and vascular repair. Stem Cells 29(2):274–285. https://doi.org/10.1002/stem.584
Larrieu-Lahargue F, Welm AL, Thomas KR, Li DY (2010) Netrin-4 induces lymphangiogenesis in vivo. Blood 115(26):5418–5426. https://doi.org/10.1182/blood-2009-11-252338
Viñals F, Pouysségur J (2001) Transforming growth factor beta1 (TGF-beta1) promotes endothelial cell survival during in vitro angiogenesis via an autocrine mechanism implicating TGF-alpha signaling. Mol Cell Biol 21(21):7218–7230. https://doi.org/10.1128/MCB.21.21.7218-7230.2001
Cheng Q, Zhang Z, Zhang S, Yang H, Zhang X, Pan J, Weng L, Sha D et al (2015) Human umbilical cord mesenchymal stem cells protect against ischemic brain injury in mouse by regulating peripheral immunoinflammation. Brain Res 1594:293–304. https://doi.org/10.1016/j.brainres.2014.10.065
Jeon H, Kim JH, Kim JH et al (2012) Plasminogen activator inhibitor type 1 regulates microglial motility and phagocytic activity. J Neuroinflammation 9:149
Yang D, Nemkul N, Shereen A, Jone A, Dunn RS, Lawrence DA, Lindquist D, Kuan CY (2009) Therapeutic administration of plasminogen activator inhibitor-1 prevents hypoxic-ischemic brain injury in newborns. J Neurosci 29(27):8669–8674. https://doi.org/10.1523/JNEUROSCI.1117-09.2009
Yang D, Sun YY, Nemkul N, Baumann JM, Shereen A, Dunn RS, Wills-Karp M, Lawrence DA et al (2013) Plasminogen activator inhibitor-1 mitigates brain injury in a rat model of infection-sensitized neonatal hypoxia–ischemia. Cereb Cortex 23(5):1218–1229. https://doi.org/10.1093/cercor/bhs115
Yang D, Sun YY, Lin X, Baumann JM, Warnock M, Lawrence DA, Kuan CY (2013) Taming neonatal hypoxic-ischemic brain injury by intranasal delivery of plasminogen activator inhibitor-1. Stroke 44(9):2623–2627. https://doi.org/10.1161/STROKEAHA.113.001233
Hughes PM, Botham MS, Frentzel S, Mir A, Perry VH (2002) Expression of fractalkine (CX3CL1) and its receptor, CX3CR1, during acute and chronic inflammation in the rodent CNS. Glia 37(4):314–327. https://doi.org/10.1002/glia.10037
Limatola C, Ransohoff RM (2014) Modulating neurotoxicity through CX3CL1/CX3CR1 signaling. Front Cell Neurosci 8:229
Suzuki M, El-Hage N, Zou S, Hahn YK, Sorrell ME, Sturgill JL, Conrad DH, Knapp PE et al (2011) Fractalkine/CX3CL1 protects striatal neurons from synergistic morphine and HIV-1 Tat-induced dendritic losses and death. Mol Neurodegener 6(1):78. https://doi.org/10.1186/1750-1326-6-78
Noda M, Doi Y, Liang J, Kawanokuchi J, Sonobe Y, Takeuchi H, Mizuno T, Suzumura A (2011) Fractalkine attenuates excito-neurotoxicity via microglial clearance of damaged neurons and antioxidant enzyme heme oxygenase-1 expression. J Biol Chem 286(3):2308–2319. https://doi.org/10.1074/jbc.M110.169839
Acknowledgments
This study was supported by grants from the Ministry of Science and Technology (103-2314-B-038-062-MY3 and 104-2314-B-006-093-MY3) of Taiwan. We acknowledge Wallace Academic Editing (www.editing.tw) for editing this manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors have no conflicts of interest to declare.
Research Involving Animals
This study was approved by the Institutional Animal Care Committee of National Cheng Kung University’s.
Informed Consent
Not indicated
Electronic Supplementary Material
ESM 1
(XLSX 22 kb).
Rights and permissions
About this article
Cite this article
Lee, YC., Chang, YC., Wu, CC. et al. Hypoxia-Preconditioned Human Umbilical Vein Endothelial Cells Protect Against Neurovascular Damage After Hypoxic Ischemia in Neonatal Brain. Mol Neurobiol 55, 7743–7757 (2018). https://doi.org/10.1007/s12035-018-0867-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-018-0867-5