Abstract
Purpose
The current meta-analysis aimed to evaluate the association of thyroid dysfunction and autoimmunity with gestational diabetes mellitus (GDM).
Methods
A comprehensive search from PubMed, Embase, MEDLINE, and Cochrane databases until November 2020 was conducted. Fixed-effect model was used to combine the results when I2 was <50%. Random-effect model was used to summarize the results when I2 was >50%.
Results
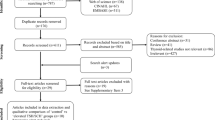
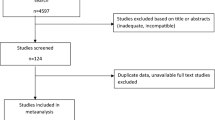
A total of 44 studies were included in the meta-analysis. Low FT4 levels were closely related with GDM in the first and second trimesters of gestation. Hypothyroxinemia (OR: 1.45; 95% CI: 1.25, 1.68; P < 0.00001), overt (OR: 1.80; 95% CI: 1.73, 1.86; P < 0.00001), and subclinical (OR: 1.54; 95% CI: 1.03, 2.30; P = 0.03) hypothyroidism, overt hyperthyroidism (OR: 1.49; 95% CI: 1.09, 2.04; P = 0.01), and positive thyroid antibodies (OR: 1.49; 95% CI: 1.07, 2.07; P < 0.00001) were observed significantly associated with the risk of GDM. Pregnant women with subclinical hyperthyroidism were less likely to develop GDM (OR: 0.62; 95% CI: 0.39, 0.97; P = 0.04).
Conclusions
Thyroid dysfunction and positive thyroid antibodies were associated with the risk of GDM. Our findings suggest that pregnant women with these thyroid diseases may be offered screening for GDM comprehensively.



Similar content being viewed by others
References
J. He, X. Chen, Y. Wang, Y. Liu, J. Bai, The experiences of pregnant women with gestational diabetes mellitus: a systematic review of qualitative evidence. Rev. Endocr. Metab. Disord. (2020). https://doi.org/10.1007/s11154-020-09610-4
L. Guariguata, U. Linnenkamp, J. Beagley, D.R. Whiting, N.H. Cho, Global estimates of the prevalence of hyperglycaemia in pregnancy. Diabetes Res. Clin. Pract. 103(2), 176–185 (2014). https://doi.org/10.1016/j.diabres.2013.11.003
M.G. Dalfrà, S. Burlina, G.G. Del Vescovo, A. Lapolla, Genetics and epigenetics: new insight on gestational diabetes mellitus. Front. Endocrinol. 11, 602477 (2020). https://doi.org/10.3389/fendo.2020.602477
E.V. Preston, C. Eberle, F.M. Brown, T. James-Todd, Climate factors and gestational diabetes mellitus risk—a systematic review. Environ. Health 19(1), 112 (2020). https://doi.org/10.1186/s12940-020-00668-w
L.L. Gong, H. Liu, L.H. Liu, Relationship between hypothyroidism and the incidence of gestational diabetes: a meta-analysis. Taiwan. J. Obstet. Gynecol. 55(2), 171–175 (2016). https://doi.org/10.1016/j.tjog.2016.02.004
U.Y. Sert, G.N. Buyuk, Y. Engin Ustun, A.S. Ozgu Erdinc, Is there any relationship between thyroid function abnormalities, thyroid antibodies and development of gestational diabetes mellitus (GDM) in pregnant women? Medeni. Med. J. 35(3), 195–201 (2020). https://doi.org/10.5222/mmj.2020.29964
Y. Kemkem, D. Nasteska, A. de Bray, P. Bargi-Souza, R.A. Peliciari-Garcia, A. Guillou, P. Mollard, D.J. Hodson, M. Schaeffer, Maternal hypothyroidism in mice influences glucose metabolism in adult offspring. Diabetologia 63(9), 1822–1835 (2020). https://doi.org/10.1007/s00125-020-05172-x
L. Gu, J. Yang, Y. Gong, Y. Ma, S. Yan, Y. Huang, Y. Wang, Y. Peng, Lower free thyroid hormone levels are associated with high blood glucose and insulin resistance; these normalize with metabolic improvement of type 2 diabetes. J. Diabetes (2020). https://doi.org/10.1111/1753-0407.13118
D. Luo, X. Wan, J. Liu, T. Tong, Optimally estimating the sample mean from the sample size, median, mid-range, and/or mid-quartile range. Stat. Methods Med. Res. 27(6), 1785–1805 (2018). https://doi.org/10.1177/0962280216669183
X. Wan, W. Wang, J. Liu, T. Tong, Estimating the sample mean and standard deviation from the sample size, median, range and/or interquartile range. BMC Med. Res. Methodol. 14, 135 (2014). https://doi.org/10.1186/1471-2288-14-135
J. Araya, A. Rodriguez, K. Lagos-SanMartin, D. Mennickent, S. Gutiérrez-Vega, B. Ortega-Contreras, B. Valderrama-Gutiérrez, M. Gonzalez, M. Farías-Jofré, E. Guzmán-Gutiérrez, Maternal thyroid profile in first and second trimester of pregnancy is correlated with gestational diabetes mellitus through machine learning. Placenta 103, 82–85 (2020). https://doi.org/10.1016/j.placenta.2020.10.015
K. Huang, Y. Xu, S. Yan, T. Li, Y. Xu, P. Zhu, F. Tao, Isolated effect of maternal thyroid-stimulating hormone, free thyroxine and antithyroid peroxidase antibodies in early pregnancy on gestational diabetes mellitus: a birth cohort study in China. Endocr. J. 66(3), 223–231 (2019). https://doi.org/10.1507/endocrj.EJ18-0340
S. Rawal, M.Y. Tsai, S.N. Hinkle, Y. Zhu, W. Bao, Y. Lin, P. Panuganti, P.S. Albert, R.C.W. Ma, C. Zhang, A longitudinal study of thyroid markers across pregnancy and the risk of gestational diabetes. J. Clin. Endocrinol. Metab. 103(7), 2447–2456 (2018). https://doi.org/10.1210/jc.2017-02442
S. Yang, F.T. Shi, P.C. Leung, H.F. Huang, J. Fan, Low thyroid hormone in early pregnancy is associated with an increased risk of gestational diabetes mellitus. J. Clin. Endocrinol. Metab. 101(11), 4237–4243 (2016). https://doi.org/10.1210/jc.2016-1506
Y. Zhang, X. Dai, S. Yang, C. Zhang, M. Han, H.F. Huang, J. Fan, Maternal low thyroxin levels are associated with adverse pregnancy outcomes in a Chinese population. 12(5), e0178100 (2017). https://doi.org/10.1371/journal.pone.0178100
S. Gorar, G.B. Abanonu, A. Uysal, O. Erol, A. Unal, S. Uyar, A.H. Cekin, Comparison of thyroid function tests and blood count in pregnant women with versus without gestational diabetes mellitus. J. Obstet. Gynaecol. Res. 43(5), 848–854 (2017). https://doi.org/10.1111/jog.13280
E. Vitacolonna, A. Lapolla, B. Di Nenno, A. Passante, I. Bucci, C. Giuliani, D. Cerrone, F. Capani, F. Monaco, G. Napolitano, Gestational diabetes and thyroid autoimmunity. Int. J. Endocrinol. 2012, 867415 (2012). https://doi.org/10.1155/2012/867415
F. Li, Y. Hu, J. Zeng, L. Zheng, P. Ye, D. Wei, D. Chen, Analysis of risk factors related to gestational diabetes mellitus. Taiwan. J. Obstet. Gynecol. 59(5), 718–722 (2020). https://doi.org/10.1016/j.tjog.2020.07.016
N. Yuan, J. Sun, Z. Li, S. Chai, X. Zhang, L. Ji, Relationship between anti-thyroid peroxidase antibody positivity and pregnancy-related and fetal outcomes in Euthyroid women: a single-center cohort study. BMC Pregnancy Childbirth 20(1), 491 (2020). https://doi.org/10.1186/s12884-020-03176-4
H. Ying, Y.P. Tang, Y.R. Bao, X.J. Su, X. Cai, Y.H. Li, D.F. Wang, Maternal TSH level and TPOAb status in early pregnancy and their relationship to the risk of gestational diabetes mellitus. Endocrine 54(3), 742–750 (2016). https://doi.org/10.1007/s12020-016-1022-6
J.E. Haddow, W.Y. Craig, L.M. Neveux, G.E. Palomaki, G. Lambert-Messerlian, F.D. Malone, M.E. D’Alton, Free thyroxine during early pregnancy and risk for gestational diabetes. PLoS ONE 11(2), e0149065 (2016). https://doi.org/10.1371/journal.pone.0149065
P. Kumru, E. Erdogdu, R. Arisoy, O. Demirci, A. Ozkoral, C. Ardic, A.A. Ertekin, S. Erdogan, N.N. Ozdemir, Effect of thyroid dysfunction and autoimmunity on pregnancy outcomes in low risk population. Arch. Gynecol. Obstet. 291(5), 1047–1054 (2015). https://doi.org/10.1007/s00404-014-3533-9
L.M. Chen, Q. Zhang, G.X. Si, Q.S. Chen, E.L. Ye, L.C. Yu, M.M. Peng, H. Yang, W.J. Du, C. Zhang, X.M. Lu, Associations between thyroid autoantibody status and abnormal pregnancy outcomes in euthyroid women. Endocrine 48(3), 924–928 (2015). https://doi.org/10.1007/s12020-014-0420-x
P. Karakosta, D. Alegakis, V. Georgiou, T. Roumeliotaki, E. Fthenou, M. Vassilaki, D. Boumpas, E. Castanas, M. Kogevinas, L. Chatzi, Thyroid dysfunction and autoantibodies in early pregnancy are associated with increased risk of gestational diabetes and adverse birth outcomes. J. Clin. Endocrinol. Metab. 97(12), 4464–4472 (2012). https://doi.org/10.1210/jc.2012-2540
T. Männistö, M. Vääräsmäki, A. Pouta, A.L. Hartikainen, A. Ruokonen, H.M. Surcel, A. Bloigu, M.R. Järvelin, E. Suvanto, Thyroid dysfunction and autoantibodies during pregnancy as predictive factors of pregnancy complications and maternal morbidity in later life. J. Clin. Endocrinol. Metab. 95(3), 1084–1094 (2010). https://doi.org/10.1210/jc.2009-1904
P. Montaner, L. Juan, R. Campos, L. Gil, R. Corcoy, Is thyroid autoimmunity associated with gestational diabetes mellitus? Metabolism 57(4), 522–525 (2008). https://doi.org/10.1016/j.metabol.2007.11.015
R. Negro, A. Schwartz, R. Gismondi, A. Tinelli, T. Mangieri, A. Stagnaro-Green, Thyroid antibody positivity in the first trimester of pregnancy is associated with negative pregnancy outcomes. J. Clin. Endocrinol. Metab. 96(6), E920–924 (2011). https://doi.org/10.1210/jc.2011-0026
S. Nazarpour, F. Ramezani Tehrani, M. Simbar, M. Tohidi, S. Minooee, M. Rahmati, F. Azizi, Effects of levothyroxine on pregnant women with subclinical hypothyroidism, negative for thyroid peroxidase antibodies. J. Clin. Endocrinol. Metab. 103(3), 926–935 (2018). https://doi.org/10.1210/jc.2017-01850
J. Li, J. Shen, L. Qin, Effects of levothyroxine on pregnancy outcomes in women with thyroid dysfunction: a meta-analysis of randomized controlled trials. Altern. Ther. Health Med. 23(2), 49–58 (2017)
M. Pradhan, B. Anand, N. Singh, M. Mehrotra, Thyroid peroxidase antibody in hypothyroidism: it’s effect on pregnancy. J. Matern.-Fetal Neonatal Med. 26(6), 581–583 (2013). https://doi.org/10.3109/14767058.2012.745498
X. Su, Y. Zhao, Z. Cao, Y. Yang, T. Duan, J. Hua, Association between isolated hypothyroxinaemia in early pregnancy and perinatal outcomes. Endocr. Connect. 8(4), 435–441 (2019). https://doi.org/10.1530/ec-19-0088
J.E. Haddow, W.Y. Craig, L.M. Neveux, H.R. Haddow, G.E. Palomaki, G. Lambert-Messerlian, F.D. Malone, M.E. D’Alton, Implications of high free thyroxine (FT4) concentrations in euthyroid pregnancies: the FaSTER trial. J. Clin. Endocrinol. Metab. 99(6), 2038–2044 (2014). https://doi.org/10.1210/jc.2014-1053
J. Cleary-Goldman, F.D. Malone, G. Lambert-Messerlian, L. Sullivan, J. Canick, T.F. Porter, D. Luthy, S. Gross, D.W. Bianchi, M.E. D’Alton, Maternal thyroid hypofunction and pregnancy outcome. Obstet. Gynecol. 112(1), 85–92 (2008). https://doi.org/10.1097/AOG.0b013e3181788dd7
F.M. Breathnach, J. Donnelly, S.M. Cooley, M. Geary, F.D. Malone, Subclinical hypothyroidism as a risk factor for placental abruption: evidence from a low-risk primigravid population. Aust. N. Z. J. Obstet. Gynaecol. 53(6), 553–560 (2013). https://doi.org/10.1111/ajo.12131
L. Chen, H. Yang, E. Ye, Z. Lin, M. Peng, H. Lin, L. Yu, Z. Cai, X. Lu, Insignificant effect of isolated hypothyroxinemia on pregnancy outcomes during the first and second trimester of pregnancy. Front. Endocrinol. 11, 528146 (2020). https://doi.org/10.3389/fendo.2020.528146
M. Zhou, M. Wang, J. Li, X. Luo, M. Lei, Effects of thyroid diseases on pregnancy outcomes. Exp. Ther. Med. 18(3), 1807–1815 (2019). https://doi.org/10.3892/etm.2019.7739
X. Gong, A. Liu, Y. Li, H. Sun, Y. Li, C. Li, X. Yu, C. Fan, Z. Shan, W. Teng, The impact of isolated maternal hypothyroxinemia during the first and second trimester of gestation on pregnancy outcomes: an intervention and prospective cohort study in China. J. Endocrinol. Investig. 42(5), 599–607 (2019). https://doi.org/10.1007/s40618-018-0960-7
M. Aburezq, F. AlAlban, M. Alabdulrazzaq, H. Badr, Risk factors associated with gestational diabetes mellitus: the role of pregnancy-induced hypertension and physical inactivity. Pregnancy Hypertens. 22, 64–70 (2020). https://doi.org/10.1016/j.preghy.2020.07.010
S.S. Fatima, R. Rehman, Z. Butt, M. Asif Tauni, T. Fatima Munim, B. Chaudhry, T.A. Khan, Screening of subclinical hypothyroidism during gestational diabetes in Pakistani population. J. Matern.-Fetal Neonatal Med. 29(13), 2166–2170 (2016). https://doi.org/10.3109/14767058.2015.1077513
H. Shahbazian, N. Shahbazian, M. Rahimi Baniani, L. Yazdanpanah, S.M. Latifi, Evaluation of thyroid dysfunction in pregnant women with gestational and pre-gestational diabetes. Pak. J. Med. Sci. 29(2), 638–641 (2013). https://doi.org/10.12669/pjms.292.2862
T. Männistö, P. Mendola, J. Grewal, Y. Xie, Z. Chen, S.K. Laughon, Thyroid diseases and adverse pregnancy outcomes in a contemporary US cohort. J. Clin. Endocrinol. Metab. 98(7), 2725–2733 (2013). https://doi.org/10.1210/jc.2012-4233
S. Hoseini, S. Hantoushzadeh, S. Shoar, Evaluating the extent of pregravid risk factors of gestational diabetes mellitus in women in tehran. Iran. Red. Crescent Med. J. 13(6), 407–414 (2011)
M.T. Sahu, V. Das, S. Mittal, A. Agarwal, M. Sahu, Overt and subclinical thyroid dysfunction among Indian pregnant women and its effect on maternal and fetal outcome. Arch. Gynecol. Obstet. 281(2), 215–220 (2010). https://doi.org/10.1007/s00404-009-1105-1
T. Barišić, V. Mandić, A. Vasilj, D. Tiric, Higher levels of thyrotropin in pregnancy and adverse pregnancy outcomes. J. Matern.-Fetal Neonatal Med. 32(17), 2883–2888 (2019). https://doi.org/10.1080/14767058.2018.1451509
S. Turunen, M. Vääräsmäki, T. Männistö, A.L. Hartikainen, A.M. Lahesmaa-Korpinen, M. Gissler, E. Suvanto, Pregnancy and perinatal outcome among hypothyroid mothers: a population-based cohort study. Thyroid 29(1), 135–141 (2019). https://doi.org/10.1089/thy.2018.0311
Y. Zhang, W. Sun, S. Zhu, Y. Huang, Y. Huang, Y. Gao, J. Zhang, H. Yang, X. Guo, The impact of thyroid function and TPOAb in the first trimester on pregnancy outcomes: a retrospective study in peking. J. Clin. Endocrinol. Metab. 105(3) (2020). https://doi.org/10.1210/clinem/dgz167
B.D. Cakmak, U.A. Turker, M. Temur, E. Ustunyurt, Pregnancy outcomes of antibody negative and untreated subclinical hypothyroidism. J. Obstet. Gynaecol. Res. 45(4), 810–816 (2019). https://doi.org/10.1111/jog.13925
S. Furukawa, K. Miyakawa, J. Shibata, M. Iwashita, Women with subclinical hypothyroidism are at low risk of poor pregnancy outcome in Japan. Tohoku J. Exp. Med. 242(3), 167–172 (2017). https://doi.org/10.1620/tjem.242.167
L.M. Chen, W.J. Du, J. Dai, Q. Zhang, G.X. Si, H. Yang, E.L. Ye, Q.S. Chen, L.C. Yu, C. Zhang, X.M. Lu, Effects of subclinical hypothyroidism on maternal and perinatal outcomes during pregnancy: a single-center cohort study of a Chinese population. PLoS ONE 9(10), e109364 (2014). https://doi.org/10.1371/journal.pone.0109364
D.B. Nelson, B.M. Casey, D.D. McIntire, F.G. Cunningham, Subsequent pregnancy outcomes in women previously diagnosed with subclinical hypothyroidism. Am. J. Perinatol. 31(1), 77–84 (2014). https://doi.org/10.1055/s-0033-1334457
C.M. Tudela, B.M. Casey, D.D. McIntire, F.G. Cunningham, Relationship of subclinical thyroid disease to the incidence of gestational diabetes. Obstet. Gynecol. 119(5), 983–988 (2012). https://doi.org/10.1097/AOG.0b013e318250aeeb
N. Arbib, E. Hadar, O. Sneh-Arbib, R. Chen, A. Wiznitzer, R. Gabbay-Benziv, First trimester thyroid stimulating hormone as an independent risk factor for adverse pregnancy outcome. J. Matern.-Fetal Neonatal Med. 30(18), 2174–2178 (2017). https://doi.org/10.1080/14767058.2016.1242123
N. Aggarawal, V. Suri, R. Singla, S. Chopra, P. Sikka, V.N. Shah, A. Bhansali, Pregnancy outcome in hyperthyroidism: a case control study. Gynecol. Obstet. Investig. 77(2), 94–99 (2014). https://doi.org/10.1159/000357615
C. Li, S. Peng, X. Zhang, X. Xie, D. Wang, J. Mao, X. Teng, Z. Shan, W. Teng, The urine iodine to creatinine as an optimal index of iodine during pregnancy in an iodine adequate area in China. J. Clin. Endocrinol. Metab. 101(3), 1290–1298 (2016). https://doi.org/10.1210/jc.2015-3519
V.J. Pop, V. Ormindean, A. Mocan, M. Meems, M. Broeren, J.K. Denollet, W.M. Wiersinga, A. Bunevicius, Maternal cognitive function during pregnancy in relation to hypo- and hyperthyroxinemia. Clin. Endocrinol. 91(6), 824–833 (2019). https://doi.org/10.1111/cen.14107
T.I.M. Korevaar, A. Derakhshan, P.N. Taylor, M. Meima, L. Chen, S. Bliddal, D.M. Carty, M. Meems, B. Vaidya, B. Shields, F. Ghafoor, P.V. Popova, L. Mosso, E. Oken, E. Suvanto, A. Hisada, J. Yoshinaga, S.J. Brown, J. Bassols, J. Auvinen, W.M. Bramer, A. López-Bermejo, C. Dayan, L. Boucai, M. Vafeiadi, E.N. Grineva, A.S. Tkachuck, V.J.M. Pop, T.G. Vrijkotte, M. Guxens, L. Chatzi, J. Sunyer, A. Jiménez-Zabala, I. Riaño, M. Murcia, X. Lu, S. Mukhtar, C. Delles, U. Feldt-Rasmussen, S.M. Nelson, E.K. Alexander, L. Chaker, T. Männistö, J.P. Walsh, E.N. Pearce, E.A.P. Steegers, R.P. Peeters, Association of thyroid function test abnormalities and thyroid autoimmunity with preterm birth: a systematic review and meta-analysis. JAMA 322(7), 632–641 (2019). https://doi.org/10.1001/jama.2019.10931
K.A. Toulis, A. Stagnaro-Green, R. Negro, Maternal subclinical hypothyroidsm and gestational diabetes mellitus: a meta-analysis. Endocr. Pract. 20(7), 703–714 (2014). https://doi.org/10.4158/ep13440.ra
A. Al-Khaldi, S. Sultan, The expression of sirtuins, superoxide dismutase, and lipid peroxidation status in peripheral blood from patients with diabetes and hypothyroidism. 19(1), 19 (2019). https://doi.org/10.1186/s12902-019-0350-y
E. Carmeli, A. Bachar, S. Barchad, M. Morad, J. Merrick, Antioxidant status in the serum of persons with intellectual disability and hypothyroidism: a pilot study. Res. Dev. Disabil. 29(5), 431–438 (2008). https://doi.org/10.1016/j.ridd.2007.08.001
A. Haribabu, V.S. Reddy, C. Pallavi, A.R. Bitla, A. Sachan, P. Pullaiah, V. Suresh, P.V. Rao, M.M. Suchitra, Evaluation of protein oxidation and its association with lipid peroxidation and thyrotropin levels in overt and subclinical hypothyroidism. Endocrine 44(1), 152–157 (2013). https://doi.org/10.1007/s12020-012-9849-y
Y. Han, L.J. Mao, X. Ge, K. Huang, S.Q. Yan, L.L. Ren, S.Q. Hong, H. Gao, J. Sheng, Y.Y. Xu, W.J. Pan, P. Zhu, J.H. Hao, D.F. Zhu, F.B. Tao, Thyroid autoantibodies in pregnancy are associated with hypertensive disorders of pregnancy: Ma'anshan Birth Cohort Study. 88(6), 928–935 (2018). https://doi.org/10.1111/cen.13590
M. Yang, C. Du, Y. Wang, J. Liu, CD19(+)CD24(hi)CD38(hi) regulatory B cells are associated with insulin resistance in type I Hashimoto’s thyroiditis in Chinese females. Exp. Ther. Med. 14(4), 3887–3893 (2017). https://doi.org/10.3892/etm.2017.4925
Funding
The study was funded by Natural Science Foundation of China (Grant Nos. 81670763 and 81471050).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Luo, J., Wang, X., Yuan, L. et al. Association of thyroid disorders with gestational diabetes mellitus: a meta-analysis. Endocrine 73, 550–560 (2021). https://doi.org/10.1007/s12020-021-02712-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-021-02712-2