Abstract
Purpose of review
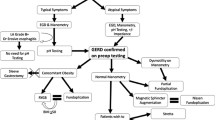
Endoscopic intervention is one of the therapeutic modalities that are currently available for GERD. Endoscopic treatment for GERD has been recently positioned as an alternative for chronic medical therapy or anti-reflux surgery. Patients who are candidates for these procedures include those with typical symptoms of GERD, low-grade erosive esophagitis (Los Angeles A and B), abnormal esophageal acid exposure if normal endoscopy, small hiatal hernia (< 3 cm), and partial or complete response to PPI treatment. This review will highlight the present and emerging data available about current and new endoscopic therapeutic modalities for GERD.
Recent findings
Presently, there are three endoscopic techniques that are approved for GERD, including the Stretta procedure, transoral incisionless fundoplication (TIF), and Medigus ultrasonic surgical endostapler (MUSE). Overall, all endoscopic techniques for GERD have reported excellent control of GERD-related symptoms, improvement of health-related quality of life, durability, and safety. However, the quality of evidence to support these claims varies greatly from one procedure to the other. Furthermore, there is an important discrepancy between improvement of subjective clinical parameters versus objective clinical parameters. There is a growing interest in positioning the endoscopic techniques in patient’s post-bariatric surgery, after peroral endoscopic myotomy (POEM), and in those who also require hiatal hernia repair. There are several new endoscopic interventions for GERD that are currently under investigation.
Summary
Endoscopic techniques are currently part of our therapeutic armamentarium for GERD. Criticism about their limited effect on objective clinical endpoints has tempered the enthusiasm of patients and physicians alike about their therapeutic value. However, endoscopic therapy for GERD is here to stay as more patients are looking for alternatives to medical and surgical therapy.





Similar content being viewed by others
References and Recommended Reading
El-Serag HB, et al. Update on the epidemiology of gastro-oesophageal reflux disease: a systematic review. Gut. 2014;63(6):871–80.
Sandhu DS, Fass R. Current trends in the management of gastroesophageal reflux disease. Gut Liver. 2018;12(1):7–16.
Shaheen NJ, et al. The burden of gastrointestinal and liver diseases, 2006. Am J Gastroenterol. 2006;101(9):2128–38.
Lagergren J, et al. Symptomatic gastroesophageal reflux as a risk factor for esophageal adenocarcinoma. N Engl J Med. 1999;340(11):825–31.
Ness-Jensen E, et al. Lifestyle intervention in gastroesophageal reflux disease. Clin Gastroenterol Hepatol. 2016;14(2):175–82 e1–3.
Banerjee S, et al. Effect of concomitant use of clopidogrel and proton pump inhibitors after percutaneous coronary intervention. Am J Cardiol. 2011;107(6):871–8.
Girgis CM, Sher D, Seibel MJ. Atypical femoral fractures and bisphosphonate use. N Engl J Med. 2010;362(19):1848–9.
Heidelbaugh JJ, Goldberg KL, Inadomi JM. Adverse risks associated with proton pump inhibitors: a systematic review. Gastroenterol Hepatol. 2009;5(10):725–34.
Kellokumpu I, et al. Quality of life following laparoscopic Nissen fundoplication: assessing short-term and long-term outcomes. World J Gastroenterol. 2013;19(24):3810–8.
Grant A, et al. The effectiveness and cost-effectiveness of minimal access surgery amongst people with gastro-oesophageal reflux disease—a UK collaborative study. The Reflux Trial Health Technol Assess. 2008;12(31):1–181 iii-iv.
Galmiche JP, et al. Laparoscopic antireflux surgery vs esomeprazole treatment for chronic GERD: the LOTUS randomized clinical trial. JAMA. 2011;305(19):1969–77.
Shibli F, Kitayama Y, Fass R. Novel therapies for gastroesophageal reflux disease: beyond proton pump inhibitors. Curr Gastroenterol Rep. 2020;22(4):16.
Nabi Z, Reddy DN. Endoscopic management of gastroesophageal reflux disease: revisited. Clin Endosc. 2016;49(5):408–16.
Fass R. Endoscopic approaches for the treatment of gastroesophageal reflux disease. Gastroenterol Hepatol. 2019;15(10):555–7.
Sandhu DS and Fass R, Stretta therapy in the management of gastroesophageal reflux disease (GERD). Ann Esophagus, 2019. 2.
Sowa P, Samarasena JB. Nonablative radiofrequency treatment for gastroesophageal reflux disease (STRETTA). Gastrointest Endosc Clin N Am. 2020;30(2):253–65.
Jackman WM, et al. Catheter ablation of accessory atrioventricular pathways (Wolff-Parkinson-White syndrome) by radiofrequency current. N Engl J Med. 1991;324(23):1605–11.
Utley DS, et al. Augmentation of lower esophageal sphincter pressure and gastric yield pressure after radiofrequency energy delivery to the gastroesophageal junction: a porcine model. Gastrointest Endosc. 2000;52(1):81–6.
Chang K and Utley D. Endoscopic ultrasound (EUS) in-vivo assessment of radiofrequency (RF) energy delivery to the gastroesophageal (GE) junction in a porcine model. in GASTROINTESTINAL ENDOSCOPY. 2001. MOSBY, INC 11830 WESTLINE INDUSTRIAL DR, ST LOUIS, MO 63146–3318 USA.
Lidums I, et al. Control of transient lower esophageal sphincter relaxations and reflux by the GABA(B) agonist baclofen in normal subjects. Gastroenterology. 2000;118(1):7–13.
Auyang ED, et al. SAGES clinical spotlight review: endoluminal treatments for gastroesophageal reflux disease (GERD). Surg Endosc. 2013;27(8):2658–72.
Vaezi MF, Shaheen NJ, Muthusamy VR. State of evidence in minimally invasive management of gastroesophageal reflux: findings of a scoping review. Gastroenterology. 2020.
Triadafilopoulos G, et al. The Stretta procedure for the treatment of GERD: 6 and 12 month follow-up of the U.S. open label trial. Gastrointest Endosc. 2002;55(2):149–56.
Corley DA, et al. Improvement of gastroesophageal reflux symptoms after radiofrequency energy: a randomized, sham-controlled trial. Gastroenterology. 2003;125(3):668–76.
Aziz AM, et al. A prospective randomized trial of sham, single-dose Stretta, and double-dose Stretta for the treatment of gastroesophageal reflux disease. Surg Endosc. 2010;24(4):818–25.
Coron E, et al. Clinical trial: radiofrequency energy delivery in proton pump inhibitor-dependent gastro-oesophageal reflux disease patients. Aliment Pharmacol Ther. 2008;28(9):1147–58.
Arts J, et al. A double-blind sham-controlled study of the effect of radiofrequency energy on symptoms and distensibility of the gastro-esophageal junction in GERD. Am J Gastroenterol. 2012;107(2):222–30.
Perry KA, Banerjee A, Melvin WS. Radiofrequency energy delivery to the lower esophageal sphincter reduces esophageal acid exposure and improves GERD symptoms: a systematic review and meta-analysis. Surg Laparosc Endosc Percutan Tech. 2012;22(4):283–8.
Lipka S, Kumar A, Richter JE. No evidence for efficacy of radiofrequency ablation for treatment of gastroesophageal reflux disease: a systematic review and meta-analysis. Clin Gastroenterol Hepatol. 2015;13(6):1058–67 e1.
Fass R, et al. Systematic review and meta-analysis of controlled and prospective cohort efficacy studies of endoscopic radiofrequency for treatment of gastroesophageal reflux disease. Surg Endosc. 2017;31(12):4865–82.
Zerbib F, et al. Randomised clinical trial: oesophageal radiofrequency energy delivery versus sham for PPI-refractory heartburn. Aliment Pharmacol Ther. 2020;52(4):637–45.
He S, et al. Stretta procedure versus proton pump inhibitors for the treatment of nonerosive reflux disease: a 6-month follow-up. Medicine (Baltimore). 2020;99(3):e18610.
Noar M, Squires P, Khan S. Radiofrequency energy delivery to the lower esophageal sphincter improves gastroesophageal reflux patient-reported outcomes in failed laparoscopic Nissen fundoplication cohort. Surg Endosc. 2017;31(7):2854–62.
Guerron D, Portenier D. A case series on gastroesophageal reflux disease and the bariatric patients: Stretta therapy as a non-surgical option. Bariatric Times. 2016;13(11):18–20.
Khidir N, et al. Initial Experience of endoscopic radiofrequency waves delivery to the lower esophageal sphincter (Stretta procedure) on symptomatic gastroesophageal reflux disease post-sleeve gastrectomy. Obes Surg. 2018;28(10):3125–30.
Mattar SG, et al. Treatment of refractory gastroesophageal reflux disease with radiofrequency energy (Stretta) in patients after Roux-en-Y gastric bypass. Surg Endosc. 2006;20(6):850–4.
Fass R. An overview of transoral incisionless fundoplication and magnetic sphincter augmentation for GERD. Gastroenterol Hepatol (N Y). 2017;13(1):50–2.
Ihde GM. The evolution of TIF: transoral incisionless fundoplication. Ther Adv Gastroenterol. 2020;13:1756284820924206.
Chang KJ, Bell R. Transoral incisionless fundoplication. Gastrointest Endosc Clin. 2020;30(2):267–89.
Horgan S, Pellegrini CA. Surgical treatment of gastroesophageal reflux disease. Surg Clin North Am. 1997;77(5):1063–82.
Ihde GM, Besancon K, Deljkich E. Short-term safety and symptomatic outcomes of transoral incisionless fundoplication with or without hiatal hernia repair in patients with chronic gastroesophageal reflux disease. Am J Surg. 2011;202(6):740–6 discussion 746–7.
Rinsma NF, et al. Effect of transoral incisionless fundoplication on reflux mechanisms. Surg Endosc. 2014;28(3):941–9.
Sami Trad K. Transoral incisionless fundoplication: current status. Curr Opin Gastroenterol. 2016;32(4):338–43.
Cadière GB, et al. Endoluminal fundoplication by a transoral device for the treatment of GERD: a feasibility study. Surg Endosc. 2008;22(2):333–42.
Cadière GB, et al. Antireflux transoral incisionless fundoplication using EsophyX: 12-month results of a prospective multicenter study. World J Surg. 2008;32(8):1676–88.
Cadière GB, et al. Two-year results of a feasibility study on antireflux transoral incisionless fundoplication using EsophyX. Surg Endosc. 2009;23(5):957–64.
Witteman BP, et al. Transoral incisionless fundoplication for treatment of gastroesophageal reflux disease in clinical practice. Surg Endosc. 2012;26(11):3307–15.
Huang X, et al. Efficacy of transoral incisionless fundoplication (TIF) for the treatment of GERD: a systematic review with meta-analysis. Surg Endosc. 2017;31(3):1032–44.
Jain D, Singhal S. Transoral incisionless fundoplication for refractory gastroesophageal reflux disease: where do we stand? Clin Endosc. 2016;49(2):147–56.
Testoni PA, Mazzoleni G, Testoni SG. Transoral incisionless fundoplication for gastro-esophageal reflux disease: techniques and outcomes. World J Gastrointest Pharmacol Ther. 2016;7(2):179–89.
Hunter JG, et al. Efficacy of transoral fundoplication vs omeprazole for treatment of regurgitation in a randomized controlled trial. Gastroenterology. 2015;148(2):324–33 e5.
Witteman BP, et al. Randomized controlled trial of transoral incisionless fundoplication vs. proton pump inhibitors for treatment of gastroesophageal reflux disease. Am J Gastroenterol. 2015;110(4):531–42.
Håkansson B, et al. Randomised clinical trial: transoral incisionless fundoplication vs. sham intervention to control chronic GERD. Aliment Pharmacol Ther. 2015;42(11–12):1261–70.
Testoni PA, et al. Long-term efficacy of transoral incisionless fundoplication with Esophyx (Tif 2.0) and factors affecting outcomes in GERD patients followed for up to 6 years: a prospective single-center study. Surg Endosc. 2015;29(9):2770–80.
Stefanidis G, et al. Long-term benefit of transoral incisionless fundoplication using the esophyx device for the management of gastroesophageal reflux disease responsive to medical therapy. Dis Esophagus. 2017;30(3):1–8.
Richter JE, et al. Efficacy of laparoscopic Nissen fundoplication vs transoral incisionless fundoplication or proton pump inhibitors in patients with gastroesophageal reflux disease: a systematic review and network meta-analysis. Gastroenterology. 2018;154(5):1298–308 e7.
Trad KS, et al. Transoral fundoplication offers durable symptom control for chronic GERD: 3-year report from the TEMPO randomized trial with a crossover arm. Surg Endosc. 2017;31(6):2498–508.
Trad KS, et al. The TEMPO Trial at 5 years: transoral fundoplication (TIF 2.0) is safe, durable, and cost-effective. Surg Innov. 2018;25(2):149–57.
Kahrilas PJ, et al. Transoral esophagogastric fundoplication provides quality-of-life improvement and sustained symptom and esophageal ph control: a randomized, sham-controlled, crossover trial: 1666. Am J Gastroenterol. 2015;110:S710.
Testoni PA, et al. Transoral incisionless fundoplication with EsophyX for gastroesophageal reflux disease: clinical efficacy is maintained up to 10 years. Endosc Int Open. 2019;7(5):E647–54.
Ihde GM 2nd, et al. pH Scores in Hiatal Repair with Transoral Incisionless Fundoplication. JSLS. 2019;23(1):e2018.00087.
Janu P, et al. Laparoscopic hiatal hernia repair followed by transoral incisionless fundoplication with EsophyX device (HH + TIF): efficacy and safety in two community hospitals. Surg Innov. 2019;26(6):675–86.
Gisi C, et al. Efficacy and patient satisfaction of single-session transoral incisionless fundoplication and laparoscopic hernia repair. Surg Endosc. 2020;35(2):921–7.
Repici A, et al. GERD after per-oral endoscopic myotomy as compared with Heller’s myotomy with fundoplication: a systematic review with meta-analysis. Gastrointest Endosc. 2018;87(4):934–43 e18.
Marano L, et al. Surgery or peroral esophageal myotomy for achalasia: a systematic review and meta-analysis. Medicine (Baltimore). 2016;95(10):e3001.
Schlottmann F, et al. Laparoscopic Heller myotomy versus Peroral Endoscopic Myotomy (POEM) for Achalasia: a systematic review and meta-analysis. Ann Surg. 2018;267(3):451–60.
Brewer Gutierrez OI, Benias PC, Khashab MA. Same-session per-oral endoscopic myotomy followed by transoral incisionless fundoplication in achalasia: are we there yet? Am J Gastroenterol. 2020;115(2):162.
Haito Chavez Y, et al. Transoral incisionless endoscopic fundoplication guided by impedance planimetry to treat severe GERD symptoms after per-oral endoscopic myotomy. Gastrointest Endosc. 2017;85(1):254–5.
Kumta NA, et al. Transoral incisionless fundoplication for treatment of refractory GERD after peroral endoscopic myotomy. Gastrointest Endosc. 2015;81(1):224–5.
Tyberg A, et al. Transoral incisional fundoplication for reflux after peroral endoscopic myotomy: a crucial addition to our arsenal. Endosc Int Open. 2018;6(5):E549–52.
Zacherl J, et al. Endoscopic anterior fundoplication with the Medigus Ultrasonic Surgical Endostapler (MUSE™) for gastroesophageal reflux disease: 6-month results from a multi-center prospective trial. Surg Endosc. 2015;29(1):220–9.
Thosani N, et al. Endoscopic anti-reflux devices (with videos). Gastrointest Endosc. 2017;86(6):931–48.
Kim HJ, et al. Long-term follow-up results of endoscopic treatment of gastroesophageal reflux disease with the MUSE™ endoscopic stapling device. Surg Endosc. 2016;30(8):3402–8.
Roy-Shapira A, et al. Trans-oral anterior fundoplication: 5-year follow-up of pilot study. Surg Endosc. 2015;29(12):3717–21.
Nabi Z, Reddy DN. Update on endoscopic approaches for the management of gastroesophageal reflux disease. Gastroenterol Hepatol (N Y). 2019;15(7):369–76.
Weitzendorfer M, et al. Clinical feasibility of a new full-thickness endoscopic plication device (GERDx™) for patients with GERD: results of a prospective trial. Surg Endosc. 2018;32(5):2541–9.
Weitzendorfer M, et al. Interim report of a prospective trial on the clinical efficiency of a new full-thickness endoscopic plication device for patients with GERD: impact of changed suture material. Surg Laparosc Endosc Percutan Tech. 2017;27(3):163–9.
Hedberg HM, Kuchta K, Ujiki MB. First experience with banded anti-reflux mucosectomy (ARMS) for GERD: feasibility, safety, and technique (with video). J Gastrointest Surg. 2019;23(6):1274–8.
Inoue H, et al. Anti-reflux mucosectomy for gastroesophageal reflux disease in the absence of hiatus hernia: a pilot study. Ann Gastroenterol. 2014;27(4):346–51.
Benias PC, et al. Initial experience with a novel resection and plication (RAP) method for acid reflux: a pilot study. Endosc Int Open. 2018;6(4):E443–9.
Yoo IK, et al. Anti-reflux mucosectomy using a cap-assisted endoscopic mucosal resection method for refractory gastroesophageal disease: a prospective feasibility study. Surg Endosc. 2020;34(3):1124–31.
Seleem WM, Hanafy AS, Mohamed SI. Endoscopic management of refractory gastroesophageal reflux disease. Scand J Gastroenterol. 2018;53(4):390–7.
Hu HQ, et al. Peroral endoscopic cardial constriction in gastroesophageal reflux disease. Medicine (Baltimore). 2018;97(15):e0169.
Inoue H, et al. Anti-reflux mucosal ablation (ARMA) as a new treatment for gastroesophageal reflux refractory to proton pump inhibitors: a pilot study. Endosc Int Open. 2020;8(2):E133–8.
Tanabe M, et al. 878 Clinical outcomes of endoscopic anti-reflux treatment methods; Anti-Reflux Mucosectomy (ARMS) and Anti-Reflux Mucosal Ablation (ARMA). Gastrointest Endosc. 2020;91(6):AB72.
Hernández Mondragón OV, et al. Clinical feasibility of a new antireflux ablation therapy on gastroesophageal reflux disease (with video). Gastrointest Endosc. 2020;92(6):1190–201.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Human and animal rights and informed consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Endoscopy
Rights and permissions
About this article
Cite this article
Shibli, F., Fass, R. Endoscopic Anti-Reflux Procedures: Ready for Clinical Use?. Curr Treat Options Gastro 19, 399–420 (2021). https://doi.org/10.1007/s11938-021-00351-0
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11938-021-00351-0