Abstract
Purpose of review
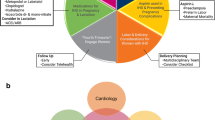
We review recent literature regarding coronary artery disease in pregnant women or women desiring pregnancy. This includes preconception counseling, prenatal care, labor and delivery, management of acute events in pregnancy, and postpartum care.
Recent findings
The pregnancy outcomes for women with coronary artery disease and their babies correlate with the degree of recovery from the initial event, coronary revascularization, and current maternal cardiac status. Preconception care includes assessment of cardiac function and management of cardiac medications. Prenatal care includes monitoring for recurrent events and planning for delivery. Delivery planning includes minimizing cardiac ischemia during labor, monitoring for cardiac events, and modifying medications. Postpartum care consists of assessing for recurrent events, assessing medications for compatibility with lactation, and contraception counseling.
Summary
Management is optimized when performed by an interdisciplinary team including Obstetrics, Maternal-Fetal Medicine, Cardiology, and Anesthesiology.
Similar content being viewed by others
References and Recommended Reading
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Gelson E, Gatzoulis MA, Steer P, Johnson MR. Heart disease--why is maternal mortality increasing? BJOG. 2009;116(5):609–11. https://doi.org/10.1111/j.1471-0528.2008.02082.x.
• Smilowitz NR, Gupta N, Guo Y, Zhong J, Weinberg CR, Reynolds HR, et al. Acute myocardial infarction during pregnancy and the puerperium in the United States. Mayo Clin Proc. 2018;93(10):1404–14. https://doi.org/10.1016/j.mayocp.2018.04.019 Discusses epidemiology of MI in pregnancy.
Kealey A. Coronary artery disease and myocardial infarction in pregnancy: a review of epidemiology, diagnosis, and medical and surgical management. Can J Cardiol. 2010;26(6):185–9. https://doi.org/10.1016/s0828-282x(10)70397-4.
•• ACOG. practice bulletin no. 212: pregnancy and heart disease. Obstet Gynecol. 2019;133(5):e320–e56 Guideline for management of CAD in pregnancy.
Codsi E, Tweet MS, Rose CH, Arendt KW, Best PJ, Hayes SN. Spontaneous coronary artery dissection in pregnancy: what every obstetrician should know. Obstet Gynecol. 2016;128(4):731–8. https://doi.org/10.1097/AOG.0000000000001630.
Paratz ED, Kao C, MacIsaac AI, Somaratne J, Whitbourn R. Evolving management and improving outcomes of pregnancy-associated spontaneous coronary artery dissection (P-SCAD): a systematic review. Int J Cardiol Heart Vasc. 2018;18:1–6. https://doi.org/10.1016/j.ijcha.2017.12.001.
Pierce T, Hovnanian M, Hedgire S, Ghoshhajra B. Imaging of cardiovascular disease in pregnancy and the peripartum period. Curr Treat Options Cardiovasc Med. 2017;19(12):94. https://doi.org/10.1007/s11936-017-0593-8.
Resnik R, Lockwood CJ, Moore TR, Greene MF, Copel JA, Silver RM. Creasy and Resnik's maternal-fetal medicine : principles and practice. Eighth edition. ed. Philadephia: Elsevier; 2019.
Burchill LJ, Lameijer H, Roos-Hesselink JW, Grewal J, Ruys TP, Kulikowski JD, et al. Pregnancy risks in women with pre-existing coronary artery disease, or following acute coronary syndrome. Heart. 2015;101(7):525–9. https://doi.org/10.1136/heartjnl-2014-306676.
Karalis DG, Hill AN, Clifton S, Wild RA. The risks of statin use in pregnancy: a systematic review. J Clin Lipidol. 2016;10(5):1081–90.
Edison RJ, Muenke M. Mechanistic and epidemiologic considerations in the evaluation of adverse birth outcomes following gestational exposure to statins. Am J Med Genet A. 2004;131(3):287–98.
• Esteve-Valverde E, Ferrer-Oliveras R, Gil-Aliberas N, Baraldès-Farré A, Llurba E, Alijotas-Reig J. Pravastatin for preventing and treating preeclampsia: a systematic review. Obstet Gynecol Surv. 2018;73(1):40–55 Reconsideration of statins in pregnancy.
Al-Aqeedi RF, Al-Nabti AD. Drug-eluting stent implantation for acute myocardial infarction during pregnancy with use of glycoprotein IIb/IIIa inhibitor, aspirin and clopidogrel. J Invasive Cardiol. 2008;20(5):E146–9.
Cooper WO, Hernandez-Diaz S, Arbogast PG, Dudley JA, Dyer S, Gideon PS, et al. Major congenital malformations after first-trimester exposure to ACE inhibitors. N Engl J Med. 2006;354(23):2443–51. https://doi.org/10.1056/NEJMoa055202.
Ain DL, Narula J, Sengupta PP. Cardiovascular imaging and diagnostic procedures in pregnancy. Cardiol Clin. 2012;30(3):331–41.
Vigorito C, Giordano A, Ferraro P, Acanfora D, De Caprio L, Naddeo C, et al. Hemodynamic effects of magnesium sulfate on the normal human heart. Am J Cardiol. 1991;67(16):1435–7.
Horlocker TT, Wedel DJ, Benzon H, Brown DL, Enneking FK, Heit JA, et al. Regional anesthesia in the anticoagulated patient: defining the risks (the second ASRA Consensus Conference on Neuraxial Anesthesia and Anticoagulation). Reg Anesth Pain Med. 2003;28(3):172–97.
Anderson PO. Anticoagulants and breastfeeding. Breastfeed Med. 2017;12(2):77–8.
Squibb B-M. Plavix (clopidogrel) prescribing information. Available at packageinserts bms com/pi/pi_plavix pdf (Accessed 1 April 2015). 2013.
Tsang K, Hartmark-Hill JR. Ticagrelor (Brilinta) for secondary prevention of thrombotic events following acute coronary syndrome. Am Fam Physician. 2013;88(12):821–2.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Anna Natenzon declares that she has no conflict of interest. Bruce Morris declares that he has no conflict of interest. Joshua Schulman-Marcus declares that he has no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Coronary Artery Disease
Rights and permissions
About this article
Cite this article
Natenzon, A., Morris, B. & Schulman-Marcus, J. An Update on Coronary Artery Disease in Pregnancy. Curr Treat Options Cardio Med 23, 16 (2021). https://doi.org/10.1007/s11936-020-00893-z
Accepted:
Published:
DOI: https://doi.org/10.1007/s11936-020-00893-z