Abstract
Purpose of Review
Porphyrias constitute a group of rare metabolic disorders that result in a deficiency of the heme biosynthetic pathway and lead to the accumulation of metabolic intermediaries. Patients with porphyria can experience recurrent neurovisceral attacks which are characterized by neuropathic abdominal pain and acute gastrointestinal symptoms, including nausea, vomiting, and constipation. Depending on the type of porphyria, patients can present with cutaneous manifestations, such as severe skin photosensitivity, chronic hemolysis, or evidence of neurologic dysfunction, including alterations in consciousness, neurovascular involvement, seizures, transient sensor-motor symptoms, polyneuropathy, and behavioral abnormalities.
Recent Findings
More recently, cases of posterior reversible encephalopathy syndrome, cerebral vasoconstriction, and acute flaccid paralysis have also been described. While the exact pathogenic mechanisms linking the accumulation of abnormal heme biosynthetic intermediaries to neurologic manifestations have not been completely elucidated, it has been proposed that these manifestations are more common than previously thought and can result in permanent neurologic injury.
Summary
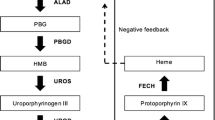
This article reviews the basic principles of heme synthesis as well as the pathogenic mechanism of disease, presentation, and treatment of acute hepatic porphyrias with emphasis on those with neurologic manifestations.

Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Yasuda M, Chen B, Desnick RJ. Recent advances on porphyria genetics: inheritance, penetrance & molecular heterogeneity, including new modifying/causative genes. Mol Genet Metab. 2019;128:320–31.
Puy H, Gouya L, Deybach J. Porphyrias. Lancet. 2010;375:924–37.
Szlendak U, Bykowska K, Lipniacka A. Clinical, biochemical and molecular characteristics of the main types of porphyria. Adv Clin Exp Med. 2016;25:361–8.
Phillips JD. Heme biosynthesis and the porphyrias. Mol Genet Metab. 2019;128:164–77 (• This publication provides a detailed description of the biochemistry of heme.).
Pischik E, Kazakov V, Kauppinen R. Is screening for urinary porphobilinogen useful among patients with acute polyneuropathy or encephalopathy? J Neurol. 2008;255:974–9.
Suh Y, Gandhi J, Seyam O, Jiang W, Joshi G, Smith NL, Ali KS. Neurological and neuropsychiatric manifestations of porphyria. Int J Neurosci. 2019;129:1226–33.
Silveira DC, Bashir M, Daniel J, Lucena MH, Bonpietro F. Acute intermittent porphyria presenting with posterior reversible encephalopathy syndrome and lateralized periodic discharges plus fast activity on EEG. Epilepsy Behav Case Rep. 2016;6:58–60.
Takata T, Kume K, Kokudo Y, Ikeda K, Kamada M, Touge T, Deguchi K, Masaki T. Acute intermittent porphyria presenting with posterior reversible encephalopathy syndrome, accompanied by prolonged vasoconstriction. Intern Med. 2017;56:713–7.
Anderson R, Patel V, Sheikh-Bahaei N, Liu CSJ, Rajamohan AG, Shiroishi MS, Kim PE, Go JL, Lerner A, Acharya J. Posterior reversible encephalopathy syndrome (PRES): pathophysiology and neuro-imaging. Front Neurol. 2020;11:463.
Zheng X, Liu X, Wang Y, Zhao R, Qu L, Pei H, Tuo M, Zhang Y, Song Y, Ji X, et al. Acute intermittent porphyria presenting with seizures and posterior reversible encephalopathy syndrome: two case reports and a literature review. Medicine (Baltimore). 2018;97: e11665.
Zhao B, Wei Q, Wang Y, Chen Y, Shang H. Posterior reversible encephalopathy syndrome in acute intermittent porphyria. Pediatr Neurol. 2014;51:457–60.
Rasheed F, Mehdi QS, Bhatti S, Khan MMA. Posterior reversible encephalopathy syndrome in a patient with variegate porphyria: a case report. Cureus . 2018;10.
Hagemann G, Ugur T, Witte OW, Fitzek C. Recurrent posterior reversible encephalopathy syndrome (PRES). J Hum Hypertens. 2004;18:287–9.
Pilato F, Distefano M, Calandrelli R. Posterior reversible encephalopathy syndrome and reversible cerebral vasoconstriction syndrome: clinical and radiological considerations. Front Neurol. 2020;11:34.
Mullin S, Platts A, Randhawa K, Watts P. Cerebral vasospasm and anterior circulation stroke secondary to an exacerbation of hereditary corproporphyria. Pract Neurol. 2012;12:384–7.
Bastide L, Legros B, Rampal N, Gilmore EJ, Hirsch LJ, Gaspard N. Clinical correlates of periodic discharges and nonconvulsive seizures in posterior reversible encephalopathy syndrome (PRES). Neurocrit Care. 2018;29:481–90.
Dawit S, Bhatt SK, Das DM, Pines AR, Shiue HJ, Goodman BP, Drazkowski JF, Sirven JI. Nonconvulsive status epilepticus secondary to acute porphyria crisis. Epilepsy Behav Case Rep. 2019;11:43–6.
Tran TPY, Leduc K, Savard M, Dupré N, Rivest D, Nguyen DK. Acute porphyria presenting as epilepsia partialis continua. Case Rep Neurol. 2013;5:116–24.
Bonkovsky HL, Dixon N, Rudnick S. Pathogenesis and clinical features of the acute hepatic porphyrias (AHPs). Mol Genet Metab. 2019;128:213–8.
Jaramillo-Calle DA, Solano JM, Rabinstein AA, Bonkovsky HL. Porphyria-induced posterior reversible encephalopathy syndrome and central nervous system dysfunction. Mol Genet Metab. 2019;128:242–53.
Price RS, Kasner SE. Hypertension and hypertensive encephalopathy. Handb Clin Neurol. 2014;119:161–7.
Alqwaifly M, Bril V, Dodig D. Acute intermittent porphyria: a report of 3 cases with neuropathy. CRN. 2019;11:32–6.
Mutluay B, Köksal A, Çelık RGG, Bülbül HH. A case of acute intermittent porphyria mimicking Guillain-Barré syndrome. Noro Psikiyatr Ars. 2019;56:311–2.
Rad N, Beydoun SR. Porphyria-induced recurrent quadriplegia misdiagnosed as Guillain-Barré syndrome. US Neurol. 2020;16:66.
Barraza G, Serranova T, Herrero C, Casanova-Mollá J, To-Figueras J, Herranz J, Valls-Solé J. Brainstem dysfunction in variegate porphyria. Muscle Nerve. 2012;46:426–33.
Spiritos Z, Salvador S, Mosquera D, Wilder J. Acute intermittent porphyria: current perspectives and case presentation. TCRM. 2019;15:1443–51.
Nabin A, Thapa LJ, Paudel R, Rana PVS. Acute intermittent porphyria with SIADH and fluctuating dysautonomia. Kathmandu Univ Med J. 2012;10:96–9.
Baumann K, Kauppinen R. Long-term follow-up of acute porphyria in female patients: update of clinical outcome and life expectancy. Mol Genet Metab Rep. 2022;30: 100842 (•• Large database of porphyria cases with long-term follow-up providing insight into frequency of complications.).
Ricci A, Di Pierro E, Marcacci M, Ventura P. Mechanisms of neuronal damage in acute hepatic porphyrias. Diagnostics (Basel). 2021;11:2205 (• Detailed description of the pathogenic mechanisms associated with neuronal damage in porphyrias.).
Hermes-Lima M, Castilho RF, Valle VG, Bechara EJ, Vercesi AE. Calcium-dependent mitochondrial oxidative damage promoted by 5-aminolevulinic acid. Biochim Biophys Acta. 1992;1180:201–6.
Emanuelli T, Pagel FW, Porciúncula LO, Souza DO. Effects of 5-aminolevulinic acid on the glutamatergic neurotransmission. Neurochem Int. 2003;42:115–21.
Müller WE, Snyder SH. delta-Aminolevulinic acid: influences on synaptic GABA receptor binding may explain CNS symptoms of porphyria. Ann Neurol. 1977;2:340–2.
Russell VA, Lamm MC, Taljaard JJ. Inhibition of Na+, K+-ATPase activity by delta-aminolevulinic acid. Neurochem Res. 1983;8:1407–15.
Lin CS-, Krishnan AV, Lee M, Zagami AS, You H, Yang C, Bostock H, Kiernan MC. Nerve function and dysfunction in acute intermittent porphyria. Brain . 2008;131:2510–2519.
Bredt DS, Hwang PM, Snyder SH. Localization of nitric oxide synthase indicating a neural role for nitric oxide. Nature. 1990;347:768–70.
•• The drug database for acute porphyria. Available at: http://www.drugs-porphyria.org/. Accessed April 11, 2022. (Updated database containing safety of drugs in porphyria.)
•• American Porphyria Foundation Drug Database. Available at: https://porphyriafoundation.org/drugdatabase/. Accessed Apr 11, 2022. (Updated database containing safety of drugs in porphyria.)
Vidaurre J, Gedela S, Yarosz S. Antiepileptic drugs and liver disease. Pediatr Neurol. 2017;77:23–36.
Syed YY. Givosiran: a review in acute hepatic porphyria. Drugs. 2021;81:841–8.
Stein P, Badminton M, Barth J, Rees D, Stewart MF. Best practice guidelines on clinical management of acute attacks of porphyria and their complications. Ann Clin Biochem. 2013;50:217–23.
Bissell DM, Anderson KE, Bonkovsky HL. Porphyria. N Engl J Med. 2017;377:862–72.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Kyle Wylie and Fernando D. Testai each declare no potential conflicts of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Neurology of Systemic Diseases
Rights and permissions
About this article
Cite this article
Wylie, K., Testai, F.D. Neurological Manifestations of Acute Porphyrias. Curr Neurol Neurosci Rep 22, 355–362 (2022). https://doi.org/10.1007/s11910-022-01205-7
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11910-022-01205-7