Abstract
Purpose of Review
Tropical infections may present with primary hepatobiliary manifestations mimicking other liver diseases. Gastroenterologists and hepatologists practicing in endemic regions must be aware of appropriate diagnostic testing and treatment of these infections.
Recent Findings
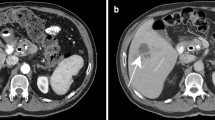
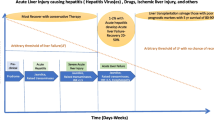
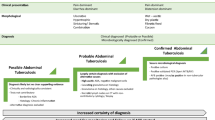
Tropical infections like dengue, malaria, scrub typhus, and leptospirosis can mimic viral hepatitis, but certain subtle clues like ongoing fever after the onset of jaundice, hepatomegaly in the setting of acute liver failure-like presentation, preserved coagulation parameters, and multi-system involvement help in suspecting the diagnosis. Infections like localized hepatic tuberculosis, amebic liver abscess, and hydatid disease should be included in the differentials of space-occupying lesions in the liver parenchyma. Hepatosplenic schistosomiasis may mimic other causes of portal hypertension.
Summary
A high index of suspicion is required to include tropical infections in the differential diagnoses of patients with liver diseases. They are more likely to occur in individuals residing in the tropics, or with a travel history to these regions.

Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
• Prahraj D, Anand AC. Tropical liver diseases: an overview. Clin Liver Dis. 2021;18:138–42. Seminal review discussing tropical liver diseases.
Samanta J, Sharma V. Dengue and its effects on liver. World J Clin Cases. 2015;3:125–31.
Kulkarni AV, Choudhury AK, Premkumar M, Jain P, Gupta E, Sarin SK. Spectrum, manifestations and outcomes of dengue infection in individuals with and without liver disease. J Clin Transl Hepatol. 2019;7:106–11.
Seneviratne SL, Malavige GN, de Silva HJ. Pathogenesis of liver involvement during dengue viral infections. Trans R Soc Trop Med Hyg. 2006;100:608–14.
Devarbhavi H, Ganga D, Menon M, Kothari K, Singh R. Dengue hepatitis with acute liver failure: clinical, biochemical, histopathological characteristics and predictors of outcome. J Gastroenterol Hepatol. 2020;35:1223–8.
Jha AK, Nijhawan S, Rai RR, Nepalia S, Jain P, Suchismita A. Etiology, clinical profile, and inhospital mortality of acute-on-chronic liver failure: a prospective study. Indian J Gastroenterol. 2013;32:108–14.
Raafat N, Blacksell SD, Maude RJ. A review of dengue diagnostics and implications for surveillance and control. Trans R Soc Trop Med Hyg. 2019;113:653–60.
Galante A, Adeyi O, Lau L, Humar A, Galvin Z, Selzner N, et al. Liver transplantation for acute liver failure due to dengue fever. Hepatology. 2019;70:1863–5.
Izmirly AM, Alturki SO, Alturki SO, Connors J, Haddad EK. Challenges in dengue vaccines development: pre-existing infections and cross-reactivity. Front Immunol. 2020;11:1055. [cited 2023 Dec 31];11. Available from: https://pubmed.ncbi.nlm.nih.gov/32655548/
Angelin M, Sjölin J, Kahn F, Ljunghill Hedberg A, Rosdahl A, Skorup P, et al. Qdenga® — a promising dengue fever vaccine; can it be recommended to non-immune travelers? Travel Med Infect Dis. 2023;54:102598.
• Anand AC, Puri P. Jaundice in malaria. J Gastroenterol Hepatol. 2005;20:1322–32. Important review article discussing the pathogenesis of liver involvement in malaria.
Murthy GL, Sahay RK, Sreenivas DV, Sundaram C, Shantaram V. Hepatitis in falciparum malaria. Trop Gastroenterol. 1998;19:152–4.
Anand AC, Ramji C, Narula AS, Singh W. Malarial hepatitis: a heterogeneous syndrome? Natl Med J India. 1992;5:59–62.
Bhalla A, Suri V, Singh V. Malarial hepatopathy. J Postgrad Med. 2006;52:315–20.
Goljan J, Nahorski W, Felczak-Korzybska I, Górski J, Myjak P. Liver injury in the course of malaria. Int Marit Health. 2000;51:30–9.
Joshi YK, Tandon BN, Acharya SK, Babu S, Tandon M. Acute hepatic failure due to Plasmodium falciparum liver injury. Liver. 1986;6:357–60.
Devarbhavi H, Alvares JF, Kumar KS. Severe falciparum malaria simulating fulminant hepatic failure. Mayo Clin Proc. 2005;80:355–8.
Ghoshal UC, Somani S, Chetri K, Akhtar P, Aggarwal R, Naik SR. Plasmodium falciparum and hepatitis E virus co-infection in fulminant hepatic failure. Indian J Gastroenterol. 2001;20:111.
Treatment of severe malaria — UpToDate [Internet]. [cited 2023 May 6]. Available from: https://www.uptodate.com/contents/treatment-of-severe-malaria?search=treatment%20of%20complicated%20malaria&source=search_result&selectedTitle=1~150&usage_type=default&display_rank=1
Levett PN. Leptospirosis. Clin Microbiol Rev. 2001;14:296–326.
Moola S, Beri D, Salam A, Jagnoor J, Teja A, Bhaumik S. Leptospirosis prevalence and risk factors in India: evidence gap maps. Trop Doct. 2021;51:415–21.
Gupta N, Wilson W, Ravindra P. Leptospirosis in India: a systematic review and meta-analysis of clinical profile, treatment and outcomes. Infez Med. 2023;31:290–305.
De Brito T, da Silva AMG, Abreu PAE. Pathology and pathogenesis of human leptospirosis: a commented review. Rev Inst Med Trop Sao Paulo. 2018;60:e23.
Wysocki J, Liu Y, Shores N. Leptospirosis with acute liver injury. Proc (Bayl Univ Med Cent). 2014;27:257–8.
Philip N, Affendy NB, Masri SN, Yuhana MY, Than LTL, Sekawi Z, et al. Combined PCR and MAT improves the early diagnosis of the biphasic illness leptospirosis. PLoS One. 2020;15:e0239069.
Luce-Fedrow A, Lehman ML, Kelly DJ, Mullins K, Maina AN, Stewart RL, et al. A review of scrub typhus (Orientia tsutsugamushi and related organisms): then, now, and tomorrow. Trop Med Infect Dis. 2018;3:8.
Gaba S, Gaba N, Gupta M, Sharma S. Hepatic and renal profile of scrub typhus patients at a tertiary care center in India. Cureus. 2020;12:e7925.
Rathi P, Siddiqui KA, Shah P. Scrub typhus-related hepatotoxicity: the Indian scenario. Trop Doct. 2021;51:228–31.
Kanno A, Yamada M, Murakami K, Torinuki W. Liver involvement in Tsutsugamushi disease. Tohoku J Exp Med. 1996;179:213–7.
Chung J-H, Lim S-C, Yun N-R, Shin S-H, Kim C-M, Kim D-M. Scrub typhus hepatitis confirmed by immunohistochemical staining. World J Gastroenterol. 2012;18:5138–41.
Gaba S, Sharma S, Gaba N, Gupta M. Scrub typhus leading to acute liver failure in a pregnant patient. Cureus. 2020;12:e10191.
Pongponratn E, Maneerat Y, Chaisri U, Wilairatana P, Punpoowong B, Viriyavejakul P, et al. Electron-microscopic examination of Rickettsia tsutsugamushi-infected human liver. Trop Med Int Health. 1998;3:242–8.
Koh GCKW, Maude RJ, Paris DH, Newton PN, Blacksell SD. Diagnosis of scrub typhus. Am J Trop Med Hyg. 2010;82:368–70.
•• Varghese GM, Dayanand D, Gunasekaran K, Kundu D, Wyawahare M, Sharma N, et al. Intravenous doxycycline, azithromycin, or both for severe scrub typhus. N Engl J Med. 2023;388:792–803. Recent randomised controlled trial from India showing superioriy of combination of doxycycline and azithromycin for severe scrub typhus.
. Alvarez SZ. Hepatobiliary tuberculosis. J Gastroenterol Hepatol. 1998;13:833–9. Seminal review article discussing the myriad presentations of tubercular liver involvement.
Elhence A, Shalimar. Hepatic tuberculosis: a wolf in sheep’s clothing. J Clin Exp Hepatol. 2021;11:521.
Chaudhary P. Hepatobiliary tuberculosis. Ann Gastroenterol. 2014;27:207–11.
Alvarez SZ, Sollano JD. ERCP in hepatobiliary tuberculosis. Gastrointest Endosc. 1998;47:100–4.
Sharma SK, Ryan H, Khaparde S, Sachdeva KS, Singh AD, Mohan A, et al. Index-TB guidelines: guidelines on extrapulmonary tuberculosis for India. Indian J Med Res. 2017;145:448–63.
Dhiman RK, Saraswat VA, Rajekar H, Reddy C, Chawla YK. A guide to the management of tuberculosis in patients with chronic liver disease. J Clin Exp Hepatol. 2012;2:260–70.
Hughes MA, Petri WA. Amebic liver abscess. Infect Dis Clin. 2000;14:565–82.
Kumar R, Priyadarshi RN, Anand U. Management of ruptured amoebic liver abscess: can we afford surgical drainage today? Frontline Gastroenterol. 2020;12:695.
Sharma MP, Dasarathy S, Verma N, Saksena S, Shukla DK. Prognostic markers in amebic liver abscess: a prospective study. Am J Gastroenterol. 1996;91:2584–8.
Noordin R, Yunus MH, Saidin S, Mohamed Z, Fuentes Corripio I, Rubio JM, et al. Multi-laboratory evaluation of a lateral flow rapid test for detection of amebic liver abscess. Am J Trop Med Hyg. 2020;103:2233–8.
Pandey S, Gupta GK, Wanjari SJ, Nijhawan S. Comparative study of tinidazole versus metronidazole in treatment of amebic liver abscess: a randomized control trial. Indian J Gastroenterol. 2018;37:196–201.
Sharma MP, Rai RR, Acharya SK, Ray JC, Tandon BN. Needle aspiration of amoebic liver abscess. BMJ. 1989;299:1308–9.
Kumar R, Ranjan A, Narayan R, Priyadarshi RN, Anand U, Null S. Evidence-based therapeutic dilemma in the management of uncomplicated amebic liver abscess: a systematic review and meta-analysis. Indian J Gastroenterol. 2019;38:498–508.
Khuroo MS, Zargar SA, Mahajan R. Hepatobiliary and pancreatic ascariasis in India. Lancet. 1990;335:1503–6.
•• Khuroo MS, Rather AA, Khuroo NS, Khuroo MS. Hepatobiliary and pancreatic ascariasis. World J Gastroenterol. 2016;22:7507–17. Important review article discussing hepatobiliary ascariasis.
Khuroo MS, Zargar SA, Mahajan R, Bhat RL, Javid G. Sonographic appearances in biliary ascariasis. Gastroenterology. 1987;93:267–72.
Hashmi MA, De JK. Biliary ascariasis on magnetic resonance cholangiopancreatography. J Glob Infect Dis. 2009;1:144–5.
Epidemiology and control of echinococcosis — UpToDate [Internet]. [cited 2023 May 7]. Available from: https://www.uptodate.com/contents/epidemiology-and-control-of-echinococcosis?search=echinococcosis&topicRef=5669&source=see_link
Echinococcosis: clinical manifestations and diagnosis — UpToDate [Internet]. [cited 2023 May 7]. Available from: https://www.uptodate.com/contents/echinococcosis-clinical-manifestations-and-diagnosis?search=echinococcosis&source=search_result&selectedTitle=1~55&usage_type=default&display_rank=1
• Khuroo MS. Percutaneous drainage in hepatic hydatidosis—the PAIR technique: concept, technique, and results. J Clin Exp Hepatol. 2021;11:592–602. Seminal review discussing the evolution of the technique of PAIR for hydatid disease.
Frider B, Larrieu E, Odriozola M. Long-term outcome of asymptomatic liver hydatidosis. J Hepatol. 1999;30:228–31.
Ozaslan E, Bayraktar Y. Endoscopic therapy in the management of hepatobiliary hydatid disease. J Clin Gastroenterol. 2002;35:160–74.
Gogia N, Sharma R, Gamangatti S, Seenu V, Madhusudhan KS, Parshad R. Hepatic hydatid cysts with biliary, and peritoneal rupture and transdiaphragmatic migration. Trop Gastroenterol. 2006;27:93–6.
Khuroo MS, Dar MY, Yattoo GN, Zargar SA, Javaid G, Khan BA, et al. Percutaneous drainage versus albendazole therapy in hepatic hydatidosis: a prospective, randomized study. Gastroenterology. 1993;104:1452–9.
Khuroo MS, Wani NA, Javid G, Khan BA, Yattoo GN, Shah AH, et al. Percutaneous drainage compared with surgery for hepatic hydatid cysts. N Engl J Med. 1997;337:881–7.
Brunetti E, Kern P, Vuitton DA. Writing Panel for the WHO-IWGE. Expert consensus for the diagnosis and treatment of cystic and alveolar echinococcosis in humans. Acta Trop. 2010;114:1–16.
Biswas SN, Kulkarni A, Jain M, Chaudhary N, Ghoshal UC. Intra-biliary rupture of hepatic hydatid cyst: an uncommon presentation of a common disease. Indian J Gastroenterol. 2021;40:445–7.
McManus DP, Dunne DW, Sacko M, Utzinger J, Vennervald BJ, Zhou X-N. Schistosomiasis. Nat Rev Dis Primers. 2018;4:13.
Kali A. Schistosome infections: an Indian perspective. J Clin Diagn Res. 2015;9:DE01–4.
Gray DJ, Ross AG, Li Y-S, McManus DP. Diagnosis and management of schistosomiasis. BMJ. 2011;342:d2651.
Author information
Authors and Affiliations
Contributions
Credit Authorship statement: AE: Writing original draft, review and editing. S: Writing original draft, review and editing, visualization and conception
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no competing interests.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Elhence, A., Shalimar Liver and Tropical Infections. Curr Hepatology Rep (2024). https://doi.org/10.1007/s11901-024-00648-5
Accepted:
Published:
DOI: https://doi.org/10.1007/s11901-024-00648-5