Abstract
Purpose of the Review
Here, we review recent findings in the field of generating insulin-producing cells by pancreatic transcription factor (pTF)-induced liver transdifferentiation (TD). TD is the direct conversion of functional cell types from one lineage to another without passing through an intermediate stage of pluripotency. We address potential reasons for the restricted efficiency of TD and suggest modalities to overcome these challenges, to bring TD closer to its clinical implementation in autologous cell replacement therapy for insulin-dependent diabetes.
Recent Findings
Liver to pancreas TD is restricted to cells that are a priori predisposed to undergo the developmental process. In vivo, the predisposition of liver cells is affected by liver zonation and hepatic regeneration. The TD propensity of liver cells is related to permissive epigenome which could be extended to TD-resistant cells by specific soluble factors. An obligatory role for active Wnt signaling in continuously maintaining a “permissive” epigenome is suggested. Moreover, the restoration of the pancreatic niche and vasculature promotes the maturation of TD cells along the β cell function.
Summary
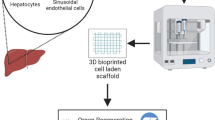
Future studies on liver to pancreas TD should include the maturation of TD cells by 3D culture, the restoration of vasculature and the pancreatic niche, and the extension of TD propensity to TD-resistant cells by epigenetic modifications. Liver to pancreas TD is expected to result in the generation of custom-made “self” surrogate β cells for curing diabetes.
Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Ferber S, Halkin A, Cohen H, Ber I, Einav Y, Goldberg I, et al. Pancreatic and duodenal homeobox gene 1 induces expression of insulin genes in liver and ameliorates streptozotocin-induced hyperglycemia. Nat Med. 2000;6(5):568–72.
Wagers AJ, Weissman IL. Plasticity of adult stem cells. Cell. 2004;116(5):639–48.
Filip S, English D, Mokry J. Issues in stem cell plasticity. J Cell Mol Med. 2004;8(4):572–7.
Takahashi K, Yamanaka S. Induction of pluripotent stem cells from mouse embryonic and adult fibroblast cultures by defined factors. Cell. 2006;126(4):663–76.
Ber I, Shternhall K, Perl S, Ohanuna Z, Goldberg I, Barshack I, et al. Functional, persistent, and extended liver to pancreas transdifferentiation. J Biol Chem. 2003;278(34):31950–7. https://doi.org/10.1074/jbc.M303127200.
Meivar-Levy I, Sapir T, Gefen-Halevi S, Aviv V, Barshack I, Onaca N, et al. Pancreatic and duodenal homeobox gene 1 induces hepatic dedifferentiation by suppressing the expression of CCAAT/enhancer-binding protein beta. Hepatology (Baltimore, Md). 2007;46(3):898–905.
Shen CN, Slack JM, Tosh D. Molecular basis of transdifferentiation of pancreas to liver. Nat Cell Biol. 2000;2:879–88.
Xie H, Ye M, Feng R, Graf T. Stepwise reprogramming of B cells into macrophages. Cell. 2004;117(5):663–76.
Zhou Q, Brown J, Kanarek A, Rajagopal J, Melton DA. In vivo reprogramming of adult pancreatic exocrine cells to beta-cells. Nature. 2008;455(7213):627–32.
Vierbuchen T, Ostermeier A, Pang ZP, Kokubu Y, Sudhof TC, Wernig M. Direct conversion of fibroblasts to functional neurons by defined factors. Nature. 2010;463(7284):1035–41.
Ieda M, Fu JD, Delgado-Olguin P, Vedatham V, Hayashi Y, Bruneau BG, et al. Direct reprogramming of fibroblasts into functional cardiomyocytes by defined factors. Cell. 2010;142(3):375–86.
Huang P, Zhang L, Gao Y, He Z, Yao D, Wu Z, et al. Direct reprogramming of human fibroblasts to functional and expandable hepatocytes. Cell Stem Cell. 2014;14(3):370–84. https://doi.org/10.1016/j.stem.2014.01.003.
van Oevelen C, Kallin EM, Graf T. Transcription factor-induced enhancer modulations during cell fate conversions. Curr Opin Genet Dev. 2013;23(5):562–7. https://doi.org/10.1016/j.gde.2013.07.003.
Meivar-Levy I, Ferber S. New organs from our own tissues: liver-to-pancreas transdifferentiation. Trends Endocrinol Metab. 2003;14(10):460–6.
Meivar-Levy I, Ferber S. Regenerative medicine: using liver to generate pancreas for treating diabetes. Isr Med Assoc J. 2006;8(6):430–4.
Meivar-Levy I, Ferber S. Reprogramming of liver cells into insulin-producing cells. Best Pract Res Clin Endocrinol Metab. 2015;29(6):873–82. https://doi.org/10.1016/j.beem.2015.10.006.
• Firas J, Polo JM. Towards understanding transcriptional networks in cellular reprogramming. Curr Opin Genet Dev. 2017;46:1–8. https://doi.org/10.1016/j.gde.2017.06.001. Suggests the need to develop computational tools to reconstruct the transcriptional networks of starting and target cells, based on published data and single cells approaches to help tailoring accurate and specific developmental processes (Cell Mogrify).
•• Ellis C, Ramzy A, Kieffer TJ. Regenerative medicine and cell-based approaches to restore pancreatic function. Nature reviews Gastroenterology & hepatology. 2017;14(10):612–28. https://doi.org/10.1038/nrgastro.2017.93. Comprehensive review that describes progress and challenges in cell-based methods to restore pancreatic function, with a focus on optimizing the site for cell delivery and decreasing requirements for immunosuppression through encapsulation. Strategies to generate insulin-producing β cell surrogates in situ are discussed; obstacles to clinical application are highlighted.
•• Latres E, Finan DA, Greenstein JL, Kowalski A, Kieffer TJ. Navigating Two Roads to Glucose Normalization in Diabetes: Automated Insulin Delivery Devices and Cell Therapy. Cell metabolism. 2019;29(3):545–63. https://doi.org/10.1016/j.cmet.2019.02.007. This recent review summarizes the significant progress that has been made in automated insulin delivery devices and cell therapy for diabetes. It addresses the barriers to widespread implementation of cell replacement approaches, compared with those achieved for artificial pancreas systems. It describes the road ahead, including the challenges and opportunities, as a cure for diabetes via both approaches.
Desmet VJ. Organization principles. In: Arias IM, Boyer JL, Chisari FV, Fausto N, Schachter D, Shafritz DA, editors. The liver; biology and pathobiology. 4th ed. Philadelphia, PA: Lippincott Williams and Wilkins; 2001. p. 3–15.
• Gilgenkrantz H, Collin de L’Hortet A. Understanding Liver Regeneration: From Mechanisms to Regenerative Medicine. The American journal of pathology. 2018;188(6):1316–27. https://doi.org/10.1016/j.ajpath.2018.03.008. The review summarizes data published in the past 5 years in the liver regeneration field, discusses the mechanisms leading to regeneration disruption in chronic liver disorders, and addresses the potential use of novel approaches for regenerative medicine. A better understanding of the role of distinct liver cell populations in liver regeneration is potentially relevant for identifying cells that are predisposed to undergo TD to pancreas.
Wang B, Zhao L, Fish M, Logan CY, Nusse R. Self-renewing diploid Axin2(+) cells fuel homeostatic renewal of the liver. Nature. 2015;524(7564):180–5. https://doi.org/10.1038/nature14863.
Fukuda K, Kikuchi Y. Endoderm development in vertebrates: fate mapping, induction and regional specification. Develop Growth Differ. 2005;47(6):343–55. https://doi.org/10.1111/j.1440-169X.2005.00815.x.
Ober EA, Field HA, Stainier DY. From endoderm formation to liver and pancreas development in zebrafish. Mech Dev. 2003;120(1):5–18.
Yang H, Morrison CM, Conlon JM, Laybolt K, Wright JR Jr. Immunocytochemical characterization of the pancreatic islet cells of the Nile tilapia (Oreochromis niloticus). Gen Comp Endocrinol. 1999;114(1):47–56.
Kito H, Ose Y, Mizuhira V, Sato T, Ishikawa T, Tazawa T. Separation and purification of (cd, cu, Zn)-metallothionein in carp hepato-pancreas. Comp Biochem Physiol C. 1982;73(1):121–7.
Deutsch G, Jung J, Zheng M, Lora J, Zaret KS. A bipotential precursor population for pancreas and liver within the embryonic endoderm. Development (Cambridge, England). 2001;128:871–81.
Otsuka M, Hoshida Y, Kato N, Moriyama M, Taniguchi H, Arai M, et al. Liver chip and gene shaving. J Gastroenterol. 2003;38(Suppl 15):89–92.
• Cerda-Esteban N, Naumann H, Ruzittu S, Mah N, Pongrac IM, Cozzitorto C, et al. Stepwise reprogramming of liver cells to a pancreas progenitor state by the transcriptional regulator Tgif2. Nature communications. 2017;8:14127. https://doi.org/10.1038/ncomms14127. This study uncovers the reprogramming activity of TGIF2 and suggests a stepwise reprogramming paradigm, whereby a “lineage-restricted” dedifferentiation step precedes the identity switch.
Varda-Bloom N, Shaish A, Gonen A, Levanon K, Greenbereger S, Ferber S, et al. Tissue-specific gene therapy directed to tumor angiogenesis. Gene Ther. 2001;8(11):819–27.
Sapir T, Shternhall K, Meivar-Levy I, Blumenfeld T, Cohen H, Skutelsky E, et al. From the cover: cell-replacement therapy for diabetes: generating functional insulin-producing tissue from adult human liver cells. Proc Natl Acad Sci U S A. 2005;102(22):7964–9.
Aviv V, Meivar-Levy I, Rachmut IH, Rubinek T, Mor E, Ferber S. Exendin-4 promotes liver cell proliferation and enhances PDX1-induced liver to pancreas transdifferentiation. J Biol Chem. 2009;284(48):33509–20.
Berneman-Zeitouni D, Molakandov K, Elgart M, Mor E, Fornoni A, Dominguez MR, et al. The temporal and hierarchical control of transcription factors-induced liver to pancreas transdifferentiation. PLoS One. 2014;9(2):e87812. https://doi.org/10.1371/journal.pone.0087812.
Gefen-Halevi S, Rachmut IH, Molakandov K, Berneman D, Mor E, Meivar-Levy I, et al. NKX6.1 promotes PDX1-induced liver to pancreatic beta-cells reprogramming. Cell Reprogram. 2010;12(6):655–64. https://doi.org/10.1089/cell.2010.0030.
• Chaimov D, Baruch L, Krishtul S, Meivar-Levy I, Ferber S, Machluf M. Innovative encapsulation platform based on pancreatic extracellular matrix achieve substantial insulin delivery. Journal of controlled release : official journal of the Controlled Release Society. 2017;257:91–101. https://doi.org/10.1016/j.jconrel.2016.07.045. The paper unravels a novel encapsulation platform for the treatment of diabetes that is based on solubilized whole porcine pancreatic extracellular matrix (ECM). The ECM-microcapsule platform provides a natural fibrous 3D niche, supporting cell viability and differentiation, while significantly improving insulin delivery. In vivo, ECM-encapsulated cells were shown to be non-immunogenic and to significantly improve the glycemic control in diabetic mouse preclinical model.
•• Cohen H, Barash H, Meivar-Levy I, Molakandov K, Ben-Shimon M, Gurevich M, et al. The Wnt/beta-catenin pathway determines the predisposition and efficiency of liver-to-pancreas reprogramming. Hepatology (Baltimore, Md). 2018. https://doi.org/10.1002/hep.29827. The study suggests that liver to pancreas TD inefficiency is due to the fact that only 5–15% of the cells in culture are a priori predisposed to undergo the pTFs induced process. A TD-prone subpopulation of liver cells from > 15 human donors is identified and separated, using lineage tracing system based on the hepatic pericentral-specific enhancer of glutamine synthetase (GLUL). The individually propagated cells exhibit substantially increased TD efficiency and insulin production occurs in > 60% of the cells upon ectopic pTF expression. The paper suggests also that TD propensity could be extended to most of the liver cells by artificially inducing epigenetic modifications. A role for active Wnt signaling in promoting liver to pancreas TD is discussed.
•• Meivar-Levy I, Zoabi F, Nardini G, Manevitz-Mendelson E, Leichner GS, Zadok O, et al. The role of the vasculature niche on insulin-producing cells generated by transdifferentiation of adult human liver cells. Stem cell research & therapy. 2019;10(1):–53. https://doi.org/10.1186/s13287-019-1157-5. The study discloses the paracrine role of vasculature (ECFC and MSC co-culture as well as conditioned media) in promoting TD-liver cells maturation both in vitro and in increasing insulin-producing cells survival upon implantation in vivo. The reconstitution of the vascular niche is expected to be an important player in regenerative medicine approaches in general.
Meivar-Levy I, Sapir T, Berneman D, Weissbach T, Polak-Charcon S, Ravassard P, et al. Human liver cells expressing albumin and mesenchymal characteristics give rise to insulin-producing cells. J Transp Secur. 2011.
Banga A, Akinci E, Greder LV, Dutton JR, Slack JM. In vivo reprogramming of Sox9+ cells in the liver to insulin-secreting ducts. Proc Natl Acad Sci U S A. 2012;109(38):15336–41. https://doi.org/10.1073/pnas.1201701109.
Banga A, Greder LV, Dutton JR, Slack JM. Stable insulin-secreting ducts formed by reprogramming of cells in the liver using a three-gene cocktail and a PPAR agonist. Gene Ther. 2014;21(1):19–27. https://doi.org/10.1038/gt.2013.50.
Wang AY, Ehrhardt A, Xu H, Kay MA. Adenovirus transduction is required for the correction of diabetes using PDX1 or Neurogenin-3 in the liver. Mol Ther. 2007;15(2):255–63.
Yechoor V, Liu V, Paul A, Lee J, Buras E, Ozer K, et al. Gene therapy with neurogenin 3 and betacellulin reverses major metabolic problems in insulin-deficient diabetic mice. Endocrinology. 2009;150(11):4863–73. https://doi.org/10.1210/en.2009-0527.
Yang Y, Akinci E, Dutton JR, Banga A, Slack JM. Stage specific reprogramming of mouse embryo liver cells to a beta cell-like phenotype. Mech Dev. 2013;130(11-12):602–12. https://doi.org/10.1016/j.mod.2013.08.002.
Luo H, Chen R, Yang R, Liu Y, Chen Y, Shu Y, et al. Reprogramming of mice primary hepatocytes into insulin-producing cells by transfection with multicistronic vectors. J Diabetes Res. 2014;2014:716163. https://doi.org/10.1155/2014/716163.
Koizumi M, Doi R, Toyoda E, Tulachan SS, Kami K, Mori T, et al. Hepatic regeneration and enforced PDX1 expression accelerate transdifferentiation in liver. Surgery. 2004;136(2):449–57.
Burke ZD, Reed KR, Phesse TJ, Sansom OJ, Clarke AR, Tosh D. Liver zonation occurs through a beta-catenin-dependent, c-Myc-independent mechanism. Gastroenterology. 2009;136(7):2316–24.e1-3.
Torre C, Perret C, Colnot S. Molecular determinants of liver zonation. Prog Mol Biol Transl Sci. 2010;97:127–50.
Gebhardt R, Matz-Soja M. Liver zonation: novel aspects of its regulation and its impact on homeostasis. World J Gastroenterol. 2014;20(26):8491–504. https://doi.org/10.3748/wjg.v20.i26.8491.
Gebhardt R, Baldysiak-Figiel A, Krugel V, Ueberham E, Gaunitz F. Hepatocellular expression of glutamine synthetase: an indicator of morphogen actions as master regulators of zonation in adult liver. Prog Histochem Cytochem. 2007;41(4):201–66.
Jungermann K, Kietzmann T. Oxygen: modulator of metabolic zonation and disease of the liver. Hepatology (Baltimore, Md). 2000;31(2):255–60.
Kietzmann T, Jungermann K. Modulation by oxygen of zonal gene expression in liver studied in primary rat hepatocyte cultures. Cell Biol Toxicol. 1997;13(4-5):243–55.
Benhamouche S, Decaens T, Godard C, Chambrey R, Rickman DS, Moinard C, et al. Apc tumor suppressor gene is the “zonation-keeper” of mouse liver. Dev Cell. 2006;10(6):759–70.
• Halpern KB, Shenhav R, Matcovitch-Natan O, Toth B, Lemze D, Golan M, et al. Single-cell spatial reconstruction reveals global division of labour in the mammalian liver. Nature. 2017;542(7641):–352, 6. https://doi.org/10.1038/nature21065. A detailed genome-wide reconstruction of the spatial hepatic zonation. The entire transcriptome of thousands of mouse liver cells and their lobule coordinates on the basis of a panel of zonated landmark genes is being characterized with single-molecule fluorescence in situ hybridization. Using this approach, the zonation profiles of all liver genes with high spatial resolution has been achieved. Information herein can be used for identifying membrane markers of hepatic predisposed cells.
• Tsuchiya A, Lu WY. Liver stem cells: plasticity of the liver epithelium. World journal of gastroenterology. 2019;25(9):1037–49. https://doi.org/10.3748/wjg.v25.i9.1037. The article highlights recent findings about plasticity in the liver epithelium and the cellular source of regeneration during liver injury. Cellular sources of liver regeneration could be relevant for identifying liver cell populations that are predisposed to undergo pTF-induced liver to pancreas TD.
Abu Rmilah A, Zhou W, Nelson E, Lin L, Amiot B, Nyberg SL. Understanding the marvels behind liver regeneration. Wiley interdisciplinary reviews Developmental biology. 2019;8(3):e340. https://doi.org/10.1002/wdev.340.
Kojima H, Fujimiya M, Matsumura K, Younan P, Imaeda H, Maeda M, et al. NeuroD-betacellulin gene therapy induces islet neogenesis in the liver and reverses diabetes in mice. Nat Med. 2003;9(5):596–603.
Yechoor V, Liu V, Espiritu C, Paul A, Oka K, Kojima H, et al. Neurogenin3 is sufficient for transdetermination of hepatic progenitor cells into neo-islets in vivo but not transdifferentiation of hepatocytes. Dev Cell. 2009;16(3):358–73.
Katz LS, Geras-Raaka E, Gershengorn MC. Reprogramming adult human dermal fibroblasts to islet-like cells by epigenetic modification coupled to transcription factor modulation. Stem Cells Dev. 2013;22(18):2551–60. https://doi.org/10.1089/scd.2013.0134.
Akinci E, Banga A, Tungatt K, Segal J, Eberhard D, Dutton JR, et al. Reprogramming of various cell types to a beta-like state by Pdx1, Ngn3 and MafA. PLoS One. 2013;8(11):e82424. https://doi.org/10.1371/journal.pone.0082424.
Cho YD, Yoon WJ, Kim WJ, Woo KM, Baek JH, Lee G, et al. Epigenetic modifications and canonical wingless/int-1 class (WNT) signaling enable trans-differentiation of nonosteogenic cells into osteoblasts. J Biol Chem. 2014;289(29):20120–8. https://doi.org/10.1074/jbc.M114.558064.
Narayanan S, Loganathan G, Dhanasekaran M, Tucker W, Patel A, Subhashree V, et al. Intra-islet endothelial cell and beta-cell crosstalk: implication for islet cell transplantation. World J Transplant. 2017;7(2):117–28. https://doi.org/10.5500/wjt.v7.i2.117.
Cleaver O, Dor Y. Vascular instruction of pancreas development. Development (Cambridge, England). 2012;139(16):2833–43. https://doi.org/10.1242/dev.065953.
Aamodt KI, Powers AC. Signals in the pancreatic islet microenvironment influence beta-cell proliferation. Diabetes Obes Metab. 2017;19(Suppl 1):124–36. https://doi.org/10.1111/dom.13031.
Peiris H, Bonder CS, Coates PT, Keating DJ, Jessup CF. The beta-cell/EC axis: how do islet cells talk to each other? Diabetes. 2014;63(1):3–11. https://doi.org/10.2337/db13-0617.
Cao Z, Wang X. The endocrine role between beta cells and intra-islet endothelial cells. Endocr J. 2014;61(7):647–54.
Brissova M, Aamodt K, Brahmachary P, Prasad N, Hong JY, Dai C, et al. Islet microenvironment, modulated by vascular endothelial growth factor-a signaling, promotes beta cell regeneration. Cell Metab. 2014;19(3):498–511. https://doi.org/10.1016/j.cmet.2014.02.001.
Nair GG, Liu JS, Russ HA, Tran S, Saxton MS, Chen R, et al. Recapitulating endocrine cell clustering in culture promotes maturation of human stem-cell-derived beta cells. Nat Cell Biol. 2019;21(2):263–74. https://doi.org/10.1038/s41556-018-0271-4.
Acknowledgments
We thank the present and former students and post-doctorate fellows for their enormous contribution during the years.
Funding
Funding supporting part of the presented studies include JDRF, ISF, D-Cure, BioDisc and EFSD, “Autologous cell replacement therapy for diabetic patients by liver cells transdifferentiation” (Dia-cure), P_37_794, POC-A. 1- A.1.1.4-E-2015 (2016 - 2020)/ SMIS 106897, Orgenesis Ltd.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Irit Meivar-Levy is a Senior Scientist at Orgenesis LTD. In addition, Dr. Meivar-Levy has a patent which is licensed to Orgenesis.
Sarah Ferber is the CSO of Orgenesis Inc. In addition, Dr. Ferber has several patents on Transdifferentiation, which are licensed to Orgenesis.
Human and Animal Rights and Informed Consent
Ethical approval: All procedures performed in studies involving human participants were in accordance with the ethical standards of Sheba Medical Center Committee on Clinical Investigations (the institutional review board; 0395-13-SMC) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. All procedures performed in studies involving animals were in accordance with the ethical standards of the institution at which the studies were conducted and ethical approval was obtained from the Institutional Animal Care and Use Committee of Sheba Medical Center (1023/16, 732/12).
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Immunology, Transplantation, and Regenerative Medicine
Rights and permissions
About this article
Cite this article
Meivar-Levy, I., Ferber, S. Liver to Pancreas Transdifferentiation. Curr Diab Rep 19, 76 (2019). https://doi.org/10.1007/s11892-019-1198-2
Published:
DOI: https://doi.org/10.1007/s11892-019-1198-2