Abstract
Introduction/objectives
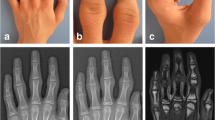
Pachydermodactyly is a rare, benign fibromatosis located around the proximal interphalangeal joints. It is often misdiagnosed as juvenile idiopathic arthritis and may cause unnecessary treatments and anxiety in patients. The goal of this paper is to describe this condition through all the existing information in the scientific literature.
Method
A systematic review and a descriptive study have been conducted. A systematic research was performed in PubMed, Embase, Cochrane Library and WOS.
Results
Pachydermodactyly was four times more frequent in male subjects and usually started in adolescence. Bilateral presentation was more frequent. History of microtrauma in both hands due to digital manipulation was found in almost half of the patients, many of them showed some neuropsychiatric disorder. In women, the onset happened later, unilateral involvement and family history were more frequent. Swelling of soft tissue without joint implication was found in imaging tests. The progression was usually positive and the treatment included stopping the microtrauma, administrating intralesional corticoids and/or surgery.
Conclusions
Diagnosis can be established in asymptomatic young patients through a congruent physical exam, regular analytic results and imaging tests that simply show swelling of soft tissue—a biopsy is generally not required for diagnosis. As pachydermodactyly’s course is asymptomatic and benign, knowledge about this condition is limited, which increases the likelihood of its underdiagnosis—it is important that clinicians know of pachydermodactyly in order to avoid misdiagnosis.





Similar content being viewed by others
References
Zuber Z, Dyduch G, Jaworek A et al (2016) Pachydermodactyly - a report of two cases. Reumatologia 54(3):136–140. https://doi.org/10.5114/reum.2016.61215
Verbov J (1975) Letter: Pachydermodactyly: a variant of the true knuckle pad. Arch Dermatol 111(4):524
Reichert CM, Costa J, Barsky SH, Claysmith AP, Liotta LA, Enzinger FM et al (1985) Pachydermodactyly. Clin Orthop Relat Res (194):252–7
Bardazzi F, Neri I, Raone B, Patrizi A (1998) Pachydermodactyly: seven new cases. Ann Dermatol Venereol 125(4):247–250
Tompkins SD, McNutt NS, Shea CR (1998) Distal pachydermodactyly. J Am Acad Dermatol 38(2 Pt 2):359–362
Chen CK, Shyur SD, Chu SH et al (2015) Pachydermodactyly: Three new cases in Taiwan. J Microbiol Immunol Infect 48(3):340–344. https://doi.org/10.1016/j.jmii.2012.09.002
Latheef F, Fairhurst D (2014) Pachydermodactyly: an unusual case of swollen fingers managed successfully with surgery. Br J Dermatol 171:126–126
Kavecan I, Pajic M, Vuckovic N et al (2018) Pachydermodactyly: A rare type of macrodactyly as a dermatological sign of compulsive behavior and repetitive minor trauma; a case report and review of the literature. Iran Red Crescent Med J 20(9). https://doi.org/10.5812/ircmj.79992
Beltraminelli H, Itin P (2009) Pachydermodactyly - Just a sign of emotional distress. Eur J Dermatol 19(1):5–13. https://doi.org/10.1684/ejd.2008.0543
Kopera D, Soyer HP, Kerl H (1995) An update on pachydermodactyly and a report of three additional cases. Br J Dermatol 133(3):433–437
Al Hammadi A, Hakim M (2007) Pachydermodactyly: case report and review of the literature. J Cutan Med Surg 11(5):185–187. https://doi.org/10.2310/7750.2007.00024
Dallos T, Oppl B, Kovacs L, Zwerina J (2014) Pachydermodactyly: a review. Curr Rheumatol Rep 16(9):442. https://doi.org/10.1007/s11926-014-0442-7
Itin PH, Lautenschlager S (1995) Pachydermodactyly: a psychocutaneous disorder. Dermatology 190(1):1–3. https://doi.org/10.1159/000246624
Agudo-Mena JL, Buedo-Rubio MI, Garcia-Atienza EM, Escario-Travesedo E (2017) Pachydermodactyly: The great mimicker (Paquidermodactilia: la gran simuladora.). Reumatol Clin. https://doi.org/10.1016/j.reuma.2017.07.015
Mesa-Del-Castillo Bermejo M, Menchon TM, de la Peña Moral J, Del Carmen Díaz F (2016) Classic pachydermodactyly. A simulator of juvenile idiopathic arthritis. An Pediatr 85(5):275–276. https://doi.org/10.1016/j.anpedi.2016.01.018
Blanes M, Bedlloch I, Pastor N, Banuls J (2005) Classic pachydermodactyly: Study of 5 cases in young boys. J Am Acad Dermatol 52(3):P153–P153
Cabanillas M, Monteagudo B, de las Heras C, Leon-Muinos E (2009) Pachydermodactyly in a young girl: cutaneous manifestation of a psychiatric disorder? J Am Acad Dermatol 60(3):AB53
Carrascosa R, Godoy A, Gordillo C, de Argila D (2014) Pachydermodactyly in a patient with generalized anxiety disorder and tics. Actas Dermosifiliogr 105(6):625–626. https://doi.org/10.1016/j.ad.2013.09.006
Castellanos González M, Sanz Motilva V (2011) Paquidermodactilia: Presentación de un caso. Arch Argent Pediatr 109(5):97–99
Garcia-Miguel J, Blanch-Rubio J, Calvo N, Iglesias M (2005) Young male with pachydermodactyly: imaging findings (Varon joven con paquidermodactilia: hallazgos radiologicos.). Reumatol Clin 1(2):131–133. https://doi.org/10.1016/s1699-258x(05)72727-3
Majlis PZ, Hermosa JMH (2009) Tumefaction of interphalangeal articulations in a 13-year-old boy. [Spanish]. Tumefaccion de articulaciones interfalangicas en un nino de 13 anos. Piel 24(10):552–553
Morales Callaghan AM, Horndler Argarate C, Garcia Latasa de Aranibar FJ, Zubiri Ara ML (2010) Pachydermodactyly: a rare form of acquired digital fibromatosis. Actas Dermosifiliogr 101(7):652–654
Perez B, Gomez MI, Sanchez E et al (1995) Pachydermodactyly: a case report. J Dermatol 22(1):43–45
Perez-Lopez I, Martinez-Lopez A, Retamero JA, Gallo F, Arias-Santiago S (2017) Paquidermodactilia, engrosamiento digital proximal. Pachydermodactyly, digital proximal thickening. Dermatol Online J 23(10)
Plana Pla A, Bassas Vila J, Toro Montecinos MA, Ferrandiz Foraster C (2014) Pachydermodactyly successfully treated with triamcinolone injections. Actas Dermosifiliogr 105(3):319–321. https://doi.org/10.1016/j.adengl.2013.04.024
Prieto D, Gallego E, Lopez-Navarro N et al (2011) Pachydermodactyly: an uncommon acquired digital fibromatosis. J Clin Rheumatol 17(1):53–54. https://doi.org/10.1097/RHU.0b013e3182056966
Russo F, Rodriguez-Pichardo A, Camacho F (1994) Familial pachydermodactyly. Acta Derm Venereol 74(5):386–387
Sola A, Vazquez-Doval J, Sola J, Quintanilla E (1992) Pachydermodactyly transgrediens. Int J Dermatol 31(11):796–797
Yanguas I, Goday JJ, Soloeta R (1994) Pachydermodactyly: report of two cases. Acta Derm Venereol 74(3):217–218
Acar A, Dirican F, Yaman B et al (2018) Swollen digits due to pachydermodactyly resembling inflammatory arthritis. Eur J Rheumatol. https://doi.org/10.5152/eurjrheum.2018.18079
Akikusa JD, Weinstein M, Laxer RM (2005) Clinical images: Pachydermodactyly. Arthritis Rheum 52(3):990. https://doi.org/10.1002/art.20848
Anandacoomarasamy A, Bak HS, Peduto A, Manolios N (2005) Magnetic resonance imaging in pachydermodactyly. J Rheumatol 32(11):2239–2241
Barnes LA, Bae GH, Lewis MA, Rieger KE (2018) Pachydermodactyly: case report including clinical and histopathologic diagnostic pitfalls. J Cutan Pathol 45(12):949–953. https://doi.org/10.1111/cup.13359
Brousse C, Rybojad M, Piette AM et al (1994) Pachydermodactyly - an observation. Rev Med Interne 15(6):412–414. https://doi.org/10.1016/s0248-8663(05)81458-4
Callot V, Wechsler J, Hovnanian A, Revuz J (1995) Pachydermodactyly and atrophia maculosa varioliformis cutis. Dermatology 190(1):56–58. https://doi.org/10.1159/000246636
Carpentier KG, Sevenants L, Wouters CH, Morren MA (2005) Pachydermodactyly may mimic juvenile idiopathic arthritis. Clin Exp Rheumatol 23(5):725
Cartier H, Guillet MH, Schollhammer M, Guillet G (1996) Pachydermodactyly in adolescents: a sign of discomfort? Arch Pediatr 3(11):1091–1094
Castori M, Paradisi A (2011) Pachydermodactyly with mild features of heritable connective tissue disorder and no sign of emotional distress. Clin Exp Dermatol 36(6):690–692. https://doi.org/10.1111/j.1365-2230.2010.04003.x
Chamberlain AJ, Venning VA, Wojnarowska F (2003) Pachydermodactyly: a forme fruste of knuckle pads? Australas J Dermatol 44(2):140–143
Chu H, Song J, Kim do Y (2016) Pachydermodactyly: a benign cutaneous condition that may be misdiagnosed as a joint disorder. J Rheumatol 43(8):1615–1616. https://doi.org/10.3899/jrheum.160242
Costa MM, Romeu JC, da Costa T (1995) Pachydermodactyly a rare cause of finger joint swelling. J Rheumatol 22(12):2374–2375
Curley RK, Hudson PM, Marsden RA (1991) Pachydermodactyly: a rare form of digital fibromatosis--report of four cases. Clin Exp Dermatol 16(2):121–123
d’Aunay V, Moutonguet I, Fraitag S (2017) Pachydermodactyly in an adolescent. Ann Dermatol Venereol 144(2):131–133. https://doi.org/10.1016/j.annder.2016.09.046
Dias JM, Costa MM, Romeu JC et al (2012) Pachydermodactyly in a 16-year-old adolescent boy. J Clin Rheumatol 18(5):246–248. https://doi.org/10.1097/RHU.0b013e3182614d08
Do Vale LRG, Coeli FR, Michalany N et al (2009) Transgrediens pachydermodactyly: report of a case. An Bras Dermatol 84(2):190–193. https://doi.org/10.1590/s0365-05962009000200014
Dupin N, Gautier MS, Rabary G et al (1994) Pachydermodactyly. Ann Dermatol Venereol 121(9):632–634
El-hallak M, Lovell D (2013) Clinical images: pachydermodactyly mimicking juvenile idiopathic arthritis. Arthritis Rheum 65(10):2736–2736. https://doi.org/10.1002/art.38045
Fathalla BM, Goldsmith DP (2009) Pachydermatodactyly mimics polyarticular juvenile idiopathic arthritis. J Pediatr 155(6):931–933. https://doi.org/10.1016/j.jpeds.2009.04.035
Fleeter TB, Myrie C, Adams JP (1984) Pachydermodactyly: a case report and discussion of the pathologic entity. J Hand Surg [Am] 9(5):764–766
Gjevre RT, El Maadawy S, Naik L, Nair B (2007) A case of deforming pachydermodactyly? J Rheumatol 34(7):1611–1611
Glicenstein J, Costa R (2004) Pachydermodactyly: a report of two cases. Chir Main 23(4):205–207
Hunt R, Mandal R, Walters R, Schaffer JV (2010) Pachydermodactyly. Dermatol Online J 16(11):5
Iraci S, Bianchi L, Innocenzi D et al (1993) Pachydermodactyly: a case of an unusual type of reactive digital fibromatosis. Arch Dermatol 129(2):247–248
Kang BD, Hong SH, Kim IH et al (1997) Two cases of pachydermodactyly. Int J Dermatol 36(10):768–772
Kato N, Niitsu M, Kawabe T et al (2015) Surgical management of unilateral soft tissue swelling around the proximal interphalangeal joint in an adolescent: a case report of pachydermodactyly. Case Rep Orthop 2015:242078–242078. https://doi.org/10.1155/2015/242078
Kim TH, Cho YH, Park HB (1996) Two cases of pachydermodactyly. J Dermatol 23(6):419–424
Lautenschlager S, Itin PH, Rufli T (1994) Pachydermodactyly: reflecting obsessive-compulsive behavior? Arch Dermatol 130(3):387
Lo WL, Wong CK (1993) Localized pachydermodactyly in tuberous sclerosis. Clin Exp Dermatol 18(2):146–147
Martin JC, Rennie JA, Kerr KM (1992) Pachydermodactyly: confused with JCA. Ann Rheum Dis 51(9):1101–1102
Mazzolai M, Naviglio S, Ventura A (2018) Pachydermodactyly. [Italian]. La pachidermodattilia. Medico e Bambino 37(2):105–107
Meunier L, Pailler C, Barneon G, Meynadier J (1994) Pachydermodactyly or acquired digital fibromatosis. Br J Dermatol 131(5):744–746
Mititelu R, Finch S, Dancey P, Landells I (2018) Two cases of pachydermodactyly presenting as polyarthritis. Case Rep Dermatology 2018:9835279–9835279. https://doi.org/10.1155/2018/9835279
Nicolay JP, Faulhaber J, Kutzner H, Schneider SW (2015) A new subtype of pachydermodactyly: unilateral pachydermodactyly transgrediens. Clin Exp Dermatol 40(6):633–635. https://doi.org/10.1111/ced.12617
Okuyama R, Kagatani S, Tagami H, Aiba S (2006) Pachydermodactyly in an elderly Japanese patient showing distal involvement of the fingers. Dermatology 213(2):177–178. https://doi.org/10.1159/000093865
Pereira JM, Pereira FCN, Pereira VCN (2004) Coxins interfalangeanos sobre paquidermodactilia. An Bras Dermatol 79(3):313–321. https://doi.org/10.1590/s0365-05962004000300007
Poddighe D, Romano M, Gattinara M, Gerloni V (2018) Pachydermodactyly. J Clin Rheumatol 24(1):37–37. https://doi.org/10.1097/rhu.0000000000000547
Preston PW, Brundler MA, Southwood TR, Moss C (2007) CPD - Clinicopathological case - Swollen fingers in an adolescent boy - pachydermodactyly. Clin Exp Dermatol 32(1):117–118. https://doi.org/10.1111/j.1365-2230.2006.02241.x
Rai A, Zaphiropoulos GC (1994) An unusual case of peri-articular soft tissue finger swelling in an adolescent male: pachydermodactyly or pachydermoperiostosis? Br J Rheumatol 33(7):677–679
Rancy SK, Granstein RD, Bansal M et al (2016) Pachydermodactyly: A case report including histopathology. J Hand Surg [Am] 41(8):e243–e246. https://doi.org/10.1016/j.jhsa.2016.04.013
Rasi A, Behrangi E, Attar B, Azizian Z (2017) pachydermodactyly with broder hand span and long fingers: a case report. Iran J Public Health 46(2):258–260
Requena CB, Miot HA, Marques ME, Miot LD (2014) Case for diagnosis. Pachydermodactyly. An Bras Dermatol 89(2):359–360
Sagransky MJ, Pichardo-Geisinger RO, Munoz-Ali D et al (2012) Pachydermodactyly from repetitive motion in poultry processing workers: a report of 2 cases. Arch Dermatol 148(8):925–928. https://doi.org/10.1001/archdermatol.2012.983
Sandobal C, Kuznietz A, Varizat A et al (2007) Pachydermodactyly: four additional cases. Clin Rheumatol 26(6):962–964. https://doi.org/10.1007/s10067-006-0210-9
Saricam MH, Salman A, Yucelten AD (2015) Symmetrical fusiform swellings around the proximal interphalangeal joints. Dermatol Pract Concept 5(3):53–54. https://doi.org/10.5826/dpc.0503a12
Schneider SL, Patel D, Shwayder TA (2017) Teenage boy with thickened dorsal hands and feet. Pediatr Dermatol 34(6):719–720. https://doi.org/10.1111/pde.13298
Schuetz C, Morbach H, Weiss T, Pfeiffer C (2011) Atypical pachydermodactyly. Clin Exp Rheumatol 29(2):388–388
Seo S-H, Sung H-W (2011) A case of pachydermodactyly. Ann Dermatol 23(2):258–261. https://doi.org/10.5021/ad.2011.23.2.258
Small S, Murthy V, Sridhar AV (2011) A 12-year-old boy presenting with unilateral proximal interphalangeal joint swelling. BMJ Case Rep 2011. https://doi.org/10.1136/bcr.01.2011.3719
Solovastru LG, Vata D, Statescu L, Andrese E (2014) Pachydermodactyly--role of local corticotherapy. Rev Med Chir Soc Med Nat Iasi 118(3):643–648
Tolis K, Stavropoulos N, Mavrogenis A, Spyridonos S (2016) Pachydermodactyly: an unknown entity. J Hand Surg [Am] 41(8):e239–e241. https://doi.org/10.1016/j.jhsa.2016.05.013
Tollefson MM, Wright TI, Davis DM (2008) Soft-tissue swelling around the proximal interphalangeal joints bilaterally: pachydermodactyly. Arch Dermatol 144(12):1651. https://doi.org/10.1001/archderm.144.12.1651-a
Ulusoy H, Tas NP, Akgol G et al (2012) Unusual unilateral presentation of pachydermodactyly: a case report. Rheumatol Int 32(6):1747–1750. https://doi.org/10.1007/s00296-011-1895-x
Woodrow SL, Burrows NP (2003) Pachydermodactyly in association with Asperger syndrome. Clin Exp Dermatol 28(6):674–675
Yang ME, Ozols I, Perdue NJ, Warren S (2012) Pachydermodactyly in a patient with Tourette syndrome. J Am Acad Dermatol 66(4):AB59–AB59
Ye S, Chen SL, Dong YQ et al (2005) Pachydermodactyly: six new cases from China. J Clin Rheumatol 11(2):72–75
Yeh Y-L, Lin H-S, Hsiao Y-P et al (2008) Pachydermodactyly - a case report. Dermatol Sin 26(4):248–250
Zabotti A, Errichetti E, Cereser L et al (2017) Pachydermodactyly: the role of ultrasonography and dermoscopy for diagnosis. Rheumatology (Oxford) 56(5):703. https://doi.org/10.1093/rheumatology/kew378
Zamanian A, Ansar A (2011) Pachydermodactyly, a new case from Iran. Dermatol Online J 17(12):8
Zhu J, Liu F, Hu Z (2015) An unusual presentation of joint inflammation in pachydermodactyly. J Rheumatol 42(5):899–900. https://doi.org/10.3899/jrheum.141284
Bardazzi F, Fanti PA, de Padova MP, Varotti C (1994) Localized pachydermodactyly in a woman. Acta Derm Venereol 74(2):152–153
Bardazzi F, Neri I, Fanti PA, Patrizi A (1996) Pachydermodactyly in two young girls. Pediatr Dermatol 13(4):288–291
Draluck JC, Kopf AW, Hodak E (1992) Pachydermodactyly: first report in a woman. J Am Acad Dermatol 27(2 Pt 2):303–305
Erre GL, Piras M, Conti M, Passiu G (2016) Pachydermodactyly. Joint Bone Spine 83(1):95. https://doi.org/10.1016/j.jbspin.2015.03.008
Higuchi C, Tomita T, Yoshikawa H (2014) Pachydermodactyly treated with tranilast in a young girl. Case Rep Orthop 2014:132854–132854. https://doi.org/10.1155/2014/132854
Saka B, Mezdegi A, Ozturk A et al (2005) Two siblings with distal pachydermodactyly. Clin Exp Dermatol 30(6):707–709. https://doi.org/10.1111/j.1365-2230.2005.01856.x
Veraldi S, Rizzitelli G, Brusasco A, Gianotti R (1996) Pachydermodactyly of a single finger. Eur J Dermatol 6(8):576–578
Marcilly MC, Balme B, Luaute JP et al (2003) Pachydermatodactyly associated with plantar pachydermy. Ann Dermatol Venereol 130(8-9 Pt 1):777–780
Sinha NK, Ling SP, Nema SK, Pai DR (2013) Pachydermodactyly does not need rheumatologic work-up. J Postgrad Med 59(4):335–336. https://doi.org/10.4103/0022-3859.123182
Thakkar V, Singh-Grewal D (2010) Swollen digits. Diagnosis: Pachydermodactyly. J Paediatr Child Health 46(6):356–368. https://doi.org/10.1111/j.1440-1754.2010.01813-1.x
Denaro V, Ruzzini L, Longo UG et al (2010) Effect of dihydrotestosterone on cultured human tenocytes from intact supraspinatus tendon. Knee Surg Sports Traumatol Arthrosc 18:971–976
Shu MG, Yi CG, Han Y et al (2008) The effect of mechanical stress on the expression of growth factor in human skin fibroblasts. Chinese Journal of Aesthetic Medicine 17:689–691
Author information
Authors and Affiliations
Contributions
RVF and JRMF: Study design, literature search and selection of papers for inclusion, data collection, interpretation of data and drafting the article. ECCP: literature search and selection of papers for inclusion AMV: Conception and study design, interpretation of data, drafting the article and revising it critically for important intellectual content. All authors gave final approval of the version published.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Ethical approval and ethical standards
Not applicable. In compliance with ethics guidelines.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 131 kb).
Rights and permissions
About this article
Cite this article
Vázquez Fernández, R., Maneiro Fernández, J.R., Cervantes Pérez, E.C. et al. Pachydermodactyly: a systematic review. Ir J Med Sci 190, 1005–1014 (2021). https://doi.org/10.1007/s11845-020-02378-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11845-020-02378-1