Abstract
Background
Understanding the acute effects of inspiratory muscle training (IMT) at different intensities on the autonomic nervous system, arterial stiffness, and blood pressure in healthy young people will be important in the constitution of appropriate IMT prescriptions.
Aims
To investigate the acute effects of IMT at different intensities on autonomic function, arterial stiffness, and blood pressure in healthy young people
Methods
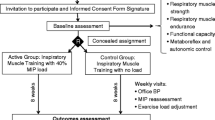
Thirty-six healthy participants were enrolled in this crossover study. All participants randomly performed IMT sessions, which consisted of diaphragmatic breathing exercise (DBE), 10%, 30%, and 60% of maximal inspiratory pressure (MIP) on consecutive days. Autonomic function and arterial stiffness were assessed by measuring heart rate variability (HRV) and aortic pulse wave velocity (AoPWV), respectively. HRV, AoPWV, and blood pressure were recorded before and immediately after each IMT session.
Results
There was no significant difference in the baseline measurements between IMT sessions (p > 0.05). Heart rate (HR) significantly decreased after DBE and IMT at 10% of MIP (p < 0.05). All time domain parameters of HRV significantly improved after DBE compared with the baseline (p < 0.05). There was no difference in the frequency domain of HRV after the IMT sessions (p > 0.05). AoPWV significantly increased after IMT at 60% of MIP (p < 0.05). Mean arterial pressure significantly changed after DBE and IMT at 60% of MIP (p < 0.05).
Conclusions
A single session of DBE positively affects autonomic function and blood pressure, while IMT at 60% of MIP increases arterial stiffness. The different intensities of IMT have various impacts on autonomic function, arterial stiffness, and blood pressure.
Trial registration
NCT03788356
Similar content being viewed by others
Change history
09 September 2020
A Correction to this paper has been published: https://doi.org/10.1007/s11845-020-02363-8
References
Mendis S, Lindholm LH, Mancia G et al (2007) World Health Organization (WHO) and International Society of Hypertension (ISH) risk prediction charts: assessment of cardiovascular risk for prevention and control of cardiovascular disease in low and middle-income countries. J Hypertens 25:1578–1582. https://doi.org/10.1097/HJH.0b013e3282861fd3
Thayer JF, Yamamoto SS, Brosschot JF (2010) The relationship of autonomic imbalance, heart rate variability and cardiovascular disease risk factors. Int J Cardiol 141:122–131. https://doi.org/10.1016/j.ijcard.2009.09.543
Vlachopoulos C, Aznaouridis K, Stefanadis C (2010) Prediction of cardiovascular events and all-cause mortality with arterial stiffness: a systematic review and meta-analysis. J Am Coll Cardiol 55:1318–1327. https://doi.org/10.1016/j.jacc.2009.10.061
Eriksson JG, Forsen T, Tuomilehto J et al (2001) Early growth and coronary heart disease in later life: longitudinal study. Bmj 322:949–953. https://doi.org/10.1136/bmj.322.7292.949
Guo S, Huang C, Maynard L et al (2000) Body mass index during childhood, adolescence and young adulthood in relation to adult overweight and adiposity: the Fels Longitudinal Study. Int J Obes 24:1628. https://doi.org/10.1038/sj.ijo.0801461
Gkaliagkousi E, Gavriilaki E, Douma S (2014) Effects of acute and chronic exercise in patients with essential hypertension: benefits and risks. Am J Hypertens 28:429–439. https://doi.org/10.1093/ajh/hpu203
Sardeli AV, Gaspari AF, Chacon-Mikahil MP (2018) Acute, short-, and long-term effects of different types of exercise in central arterial stiffness: a systematic review and meta-analysis. J Sports Med Phys Fitness 58:923–932. https://doi.org/10.23736/S0022-4707.17.07486-2
Caruso F, Arena R, Phillips S et al. (2015) Resistance exercise training improves heart rate variability and muscle performance: a randomized controlled trial in coronary artery disease patients. Eur J Phys Rehabil Med 51:281–289
Killingback C, Tsofliou F, Clark C (2017) Older people’s adherence to community-based group exercise programmes: a multiple-case study. BMC Public Health 17:115. https://doi.org/10.1186/s12889-017-4049-6
McConnell A (2013) Respiratory muscle training e-book: theory and practice: Elsevier Health Sciences
Enright SJ, Unnithan VB, Heward C et al (2006) Effect of high-intensity inspiratory muscle training on lung volumes, diaphragm thickness, and exercise capacity in subjects who are healthy. Phys Ther 86:345–354
DeLucia CM, De Asis RM, Bailey EF (2018) Daily inspiratory muscle training lowers blood pressure and vascular resistance in healthy men and women. Exp Physiol 103:201–211. https://doi.org/10.1113/EP086641
de Abreu RM, Rehder-Santos P, Minatel V et al (2017) Effects of inspiratory muscle training on cardiovascular autonomic control: a systematic review. Auton Neurosci 208:29–35. https://doi.org/10.1016/j.autneu.2017.09.002
Archiza B, Simões RP, Mendes RG et al (2013) Acute effects of different inspiratory resistive loading on heart rate variability in healthy elderly patients. Braz J Phys Ther 17:401–408. https://doi.org/10.1590/S1413-35552013005000100
Janić M, Lunder M, Šabovič M (2014) Arterial stiffness and cardiovascular therapy. Biomed Res Int 2014:621437. https://doi.org/10.1155/2014/621437
Bisconti AV, Devoto M, Venturelli M et al (2018) Respiratory muscle training positively affects vasomotor response in young healthy women. PLoS One 13(9):e0203347. https://doi.org/10.1371/journal.pone.0203347
Geddes EL, O’Brien K, Reis WD et al (2008) Inspiratory muscle training in adults with chronic obstructive pulmonary disease: an update of a systematic review. Respir Med 102:1715–1729. https://doi.org/10.1016/j.rmed.2008.07.005
Cahalin LP, Braga M, Matsuo Y et al (2002) Efficacy of diaphragmatic breathing in persons with chronic obstructive pulmonary disease: a review of the literature. J Cardpulm Rehabil 22:7–21. https://doi.org/10.1097/00008483-200201000-00002
Vitacca M, Clini E, Bianchi L et al (1998) Acute effects of deep diaphragmatic breathing in COPD patients with chronic respiratory insufficiency. Eur Respir J 11:408–415. https://doi.org/10.1183/09031936.98.11020408
Miller MR, Hankinson J, Brusasco V et al (2005) Standardisation of spirometry. Eur Respir J 26:319–338. https://doi.org/10.1183/09031936.05.00034805
European RS, Society AT (2002) ATS/ERS statement on respiratory muscle testing. Am J Respir Crit Care Med 166:518. https://doi.org/10.1164/rccm.166.4.518
Wilson S, Cooke N, Edwards R et al (1984) Predicted normal values for maximal respiratory pressures in Caucasian adults and children. Thorax 39:535–538. https://doi.org/10.1136/thx.39.7.535
Saglam M, Arikan H, Savci S et al (2010) International physical activity questionnaire: reliability and validity of the Turkish version. Percept Mot Skills 111:278–284. https://doi.org/10.2466/06.08.PMS.111.4.278-284
Lee PH, Macfarlane DJ, Lam T et al (2011) Validity of the International Physical Activity Questionnaire Short Form (IPAQ-SF): a systematic review. Int J Behav Nutr Phys Act 8:115. https://doi.org/10.1186/1479-5868-8-115
Ferreira M Jr, Zanesco A (2016) Heart rate variability as important approach for assessment autonomic modulation. Motriz: Motriz: rev educ fis 22:3–8. https://doi.org/10.1590/S1980-65742016000200001
Hwang M, Yoo J, Kim H et al Validity and reliability of aortic pulse wave velocity and augmentation index determined by the new cuff-based SphygmoCor Xcel. J Hum Hypertens 28:475. https://doi.org/10.1038/jhh.2013.144
Nakagomi A, Shoji T, Okada S et al (2018) Validity of the augmentation index and pulse pressure amplification as determined by the SphygmoCor XCEL device: a comparison with invasive measurements. Hypertens Res 41:27. https://doi.org/10.1038/hr.2017.81
Wilson RC, Jones P (1991) Long-term reproducibility of Borg scale estimates of breathlessness during exercise. Clin Sci 80:309–312. https://doi.org/10.1042/cs0800309
Gift AG. (1989) Visual analogue scales: measurement of subjective phenomena. Nurs res, Visual Analogue Scales
Tornberg J, Ikäheimo TM, Kiviniemi A et al (2019) Physical activity is associated with cardiac autonomic function in adolescent men. PLoS One 14:e0222121. https://doi.org/10.1371/journal.pone.0222121
Germano-Soares AH, Andrade-Lima A, Menêses AL et al (2018) Association of time spent in physical activities and sedentary behaviors with carotid-femoral pulse wave velocity: a systematic review and meta-analysis. Atherosclerosis 269:211–218. https://doi.org/10.1016/j.atherosclerosis.2018.01.009
Hirsch JA, Bishop B (1981) Respiratory sinus arrhythmia in humans: how breathing pattern modulates heart rate. Am J Physiol Heart Circ Physiol 241:H620–H6H9. https://doi.org/10.1152/ajpheart.1981.241.4.H620
Calabrese P, Perrault H, Dinh TP et al (2000) Cardiorespiratory interactions during resistive load breathing. Am J Phys Regul Integr Comp Phys 279:R2208–R2R13. https://doi.org/10.1152/ajpregu.2000.279.6.R2208
McConnell AK, Griffiths LA (2010) Acute cardiorespiratory responses to inspiratory pressure threshold loading. Med Sci Sports Exerc 42:1696–1703. https://doi.org/10.1249/MSS.0b013e3181d435cf
Routledge FS, Campbell TS, McFetridge-Durdle JA et al (2010) Improvements in heart rate variability with exercise therapy. Can J Cardiol 26:303–312. https://doi.org/10.1016/s0828-282X(10)70395-0
Pal G, Velkumary S (2004) Effect of short-term practice of breathing exercises on autonomic functions in normal human volunteers. Indian J Med Res 120:115
Damon DH (2005) Sympathetic innervation promotes vascular smooth muscle differentiation. Am J Physiol Heart Circ Physiol. https://doi.org/10.1152/ajpheart.00354.2004
Nakao M, Nomura K, Karita K et al (2004) Relationship between brachial-ankle pulse wave velocity and heart rate variability in young Japanese men. Hypertens Res 27:925–931. https://doi.org/10.1291/hypres.27.925
Siasos G, Athanasiou D, Terzis G et al (2016) Acute effects of different types of aerobic exercise on endothelial function and arterial stiffness. Eur J Prev Cardiol 23:1565–1572. https://doi.org/10.1177/2047487316647185
Lanfranchi PA, Somers VK (2002) Arterial baroreflex function and cardiovascular variability: interactions and implications. Am J Phys Regul Integr Comp Phys 283:R815–RR26. https://doi.org/10.1152/ajpregu.00051.2002
Bernardi L, Porta C, Spicuzza L et al (2002) Slow breathing increases arterial baroreflex sensitivity in patients with chronic heart failure. Circulation 105:143–145. https://doi.org/10.1161/hc0202.103311
Joseph CN, Porta C, Casucci G et al (2005) Slow breathing improves arterial baroreflex sensitivity and decreases blood pressure in essential hypertension. Hypertension 46:714–718. https://doi.org/10.1161/01.HYP.0000179581.68566.7d
Callegaro CC, Ribeiro JP, Tan CO et al (2011) Attenuated inspiratory muscle metaboreflex in endurance-trained individuals. Respir Physiol Neurobiol 177:24–29. https://doi.org/10.1016/j.resp.2011.03.001
Monahan KD, Tanaka H, Dinenno FA et al (2001) Central arterial compliance is associated with age-and habitual exercise–related differences in cardiovagal baroreflex sensitivity. Circulation 104:1627–1632. https://doi.org/10.1161/hc3901.096670
Sheel AW, Derchak PA, Morgan BJ et al (2001) Fatiguing inspiratory muscle work causes reflex reduction in resting leg blood flow in humans. J Physiol 537:277–289. https://doi.org/10.1111/j.1469-7793.2001.0277k.x
Gosselink R, Wagenaar RC, Rijswijk H et al (1995) Diaphragmatic breathing reduces efficiency of breathing in patients with chronic obstructive pulmonary disease. Am J Respir Crit Care Med 151:1136–1142. https://doi.org/10.1164/ajrccm.151.4.7697243
Acknowledgments
The authors thank Turhan Kahraman for statistical analysis support.
Author information
Authors and Affiliations
Contributions
Conception and design: Aylin Tanriverdi, Buse Ozcan Kahraman, Ismail Ozsoy, Ebru Ozpelit, Sema Savci; data collection: Aylin Tanriverdi, Buse Ozcan Kahraman, Ebru Ozpelit; statistical analyses: Aylin Tanriverdi, Buse Ozcan Kahraman, Ismail Ozsoy; writing of the manuscript: Aylin Tanriverdi, Sema Savci; revising the article for important intellectual content and final approval: all authors
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethics approval
This study conformed in accordance with the 2013 Declaration of Helsinki (study was not registered in a database). The study protocol was approved by the Ethics Committee of Dokuz Eylül University (reference number 2018/14-16).
Consent to participate
Written informed consent was obtained from all individual participants included in the study.
Consent for publication
Additional informed consent was obtained from all individual participants for whom identifying information is included in this article.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original version of this article was revised: This article was published online with an error. In Table 3, the name of the variable in the last row is missing. It just says 'mmHg'. The name to be written is ‘MAP (mmHg)’.
Rights and permissions
About this article
Cite this article
Tanriverdi, A., Kahraman, B.O., Ozsoy, I. et al. Acute effects of inspiratory muscle training at different intensities in healthy young people. Ir J Med Sci 190, 577–585 (2021). https://doi.org/10.1007/s11845-020-02353-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11845-020-02353-w