Abstract
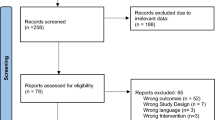
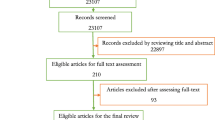
Emergency Department (ED) crowding is defined as a situation wherein the demands of emergency services overcome the ability of a department to provide high-quality care within an appropriate time frame. There is a need for solutions, as the harms of crowding impact patients, staff, and healthcare spending. An overview of ED crowding was previously published by our group, which outlines these global issues. The problem of overcrowding in emergency departments has emerged as a global public health concern, and several healthcare agencies have addressed the issue and proposed possible solutions at each level of emergency care. There is no current literature summarizing the extensive research on interventions and solutions, thus there is a need for data synthesis to inform policymakers in this field. The aim of this overview was to summarize the interventions at each level of emergency care: input, throughput, and output. The methodology was supported by the current PRIOR statement for an overview of reviews. The study summarized twenty-seven full-text systematic reviews, which encompassed three hundred and eight primary studies. The results of the summary displayed a requirement for increasing studies in input and output interventions, as these showed the best outcomes with regard to ED crowding metrics. Moreover, the results displayed heterogeneous results at each level of ED care; these reflected that generally solutions have not been matched to specific problems facing regional centres. Thus, individual factors need to be considered when implementing solutions in Emergency Departments.

Similar content being viewed by others
Data availability
Not applicable.
References
Affleck A et al (2013) Emergency department overcrowding and access block. Cjem 15(6):359–84
Javidan AP et al (2021) The International Federation for Emergency Medicine report on emergency department crowding and access block: A brief summary. CJEM 23(1):26–28
Cooksley T (2022) Editorial - The NHS urgent and emergency care crisis: how much worse could it get? Acute Med 21(4):166–167
Pearce S et al (2023) Emergency department crowding: an overview of reviews describing measures causes, and harms. Intern Emerg Med 46:1–22
Xu N, Bai J, Yan R (2022) Identifying the vulnerable regions of emergency medical services based on the three-stage of accessibility: a case study in Xi’an, China. Int J Equity Health 21(1):54
Jones PG, Mountain D, Forero R (2021) Review article: Emergency department crowding measures associations with quality of care: A systematic review. Emerg Med Australas 33(4):592–600
Asplin BR et al (2003) A conceptual model of emergency department crowding. Ann Emerg Med 42(2):173–80
Kocher KE, Asplin BR (2012) Emergency department crowding 2.0: coping with a dysfunctional system. Ann Emerg Med 60(6):687–91
Moroço DM, Pazin-Filho A (2022) Decreasing boarders in the emergency department by reducing clerical work in the discharge process of in-hospital patients in Brazil - an interrupted time-series analysis. BMC Emerg Med 22(1):99
Eiset AH, Kirkegaard H, Erlandsen M (2019) Crowding in the emergency department in the absence of boarding - a transition regression model to predict departures and waiting time. BMC Med Res Methodol 19(1):68
Gates M et al (2022) Reporting guideline for overviews of reviews of healthcare interventions: development of the PRIOR statement. BMJ 378:e070849
Crawford J et al (2017) The impact of walk-in centres and GP co-operatives on emergency department presentations: A systematic review of the literature. Int Emerg Nurs 34:36–42
Morley C et al (2018) Emergency department crowding: A systematic review of causes, consequences and solutions. PLoS One 13(8):e0203316
Yarmohammadian MH et al (2017) Overcrowding in emergency departments: A review of strategies to decrease future challenges. J Res Med Sci 22:23
Hong M et al (2020) The impact of improved access to after-hours primary care on emergency department and primary care utilization: A systematic review. Health Policy 124(8):812–818
Rasouli HR, Aliakbar Esfahani A, Abbasi Farajzadeh M (2019) Challenges, consequences, and lessons for way–outs to emergencies at hospitals: a systematic review study. BMC Emerg Med. 19(1):62
Gonçalves-Bradley D et al (2018) Primary care professionals providing non-urgent care in hospital emergency departments. Cochrane Database Syst Rev. 2(2):Cd002097
Morgan SR et al., (2013) Non-emergency department interventions to reduce ED utilization a systematic review. Acad Emerg Med 20(10):969–985
Moe J et al (2017) Effectiveness of Interventions to Decrease Emergency Department Visits by Adult Frequent Users: A Systematic Review. Acad Emerg Med 24(1):40–52
Hesselink G, Sir Ö, Schoon Y (2019) Effectiveness of interventions to alleviate emergency department crowding by older adults: a systematic review. BMC Emerg Med 19(1):69
Leduc S et al (2021) The Safety and Effectiveness of On-Site Paramedic and Allied Health Treatment Interventions Targeting the Reduction of Emergency Department Visits by Long-Term Care Patients: Systematic Review. Prehosp Emerg Care 25(4):556–565
Bucci S et al (2016) Emergency Department crowding and hospital bed shortage: is Lean a smart answer? A systematic review. Eur Rev Med Pharmacol Sci 20(20):4209–4219
Chan SS et al (2015) Strategies and solutions to alleviate access block and overcrowding in emergency departments. Hong Kong Med J 21(4):345–52
Grant KL et al (2020) Throughput interventions to reduce emergency department crowding: A systematic review. Cjem 22(6):864–874
Ortíz-Barrios MA, Alfaro-Saíz JJ (2020) Methodological Approaches to Support Process Improvement in Emergency Departments: A Systematic Review. Int J Environ Res Public Health 17(8):2664
Ming T, Lai A, Lau PM (2016) Can Team Triage Improve Patient Flow in the Emergency Department? A Systematic Review and Meta-Analysis. Adv Emerg Nurs J 38(3):233–50
Oredsson S et al (2011) A systematic review of triage-related interventions to improve patient flow in emergency departments. Scand J Trauma Resusc Emerg Med 19:43
Anderson JS et al (2020) The Effect of a Rapid Assessment Zone on Emergency Department Operations and Throughput. Ann Emerg Med 75(2):236–245
Pollaris G, Sabbe M (2016) Reverse triage: more than just another method. Eur J Emerg Med 23(4):240–247
Bullard MJ et al (2012) The role of a rapid assessment zone/pod on reducing overcrowding in emergency departments: a systematic review. Emerg Med J 29(5):372–8
Elder E, Johnston ANB, Crilly J (2015) Review article: Systematic review of three key strategies designed to improve patient flow through the emergency department. Emerg Med Australas 27(5):394–404
Rowe BH, McRae A, Rosychuk RJ (2020) Temporal trends in emergency department volumes and crowding metrics in a western Canadian province: a population-based, administrative data study. BMC Health Serv Res 20(1):356
Rowe BH et al (2011) The role of triage liaison physicians on mitigating overcrowding in emergency departments: a systematic review. Acad Emerg Med 18(2):111–20
Rowe BH et al (2011) The role of triage nurse ordering on mitigating overcrowding in emergency departments: a systematic review. Acad Emerg Med 18(12):1349–57
Sharma S, Rafferty AM, Boiko O (2020) The role and contribution of nurses to patient flow management in acute hospitals: A systematic review of mixed methods studies. Int J Nurs Stud 110:103709
Rasouli HR et al (2019) Outcomes of Crowding in Emergency Departments; a Systematic Review. Arch Acad Emerg Med 7(1):e52
Villa-Roel C et al (2012) The role of full capacity protocols on mitigating overcrowding in EDs. Am J Emerg Med 30(3):412–20
McRae AD et al (2022) A comparative evaluation of the strengths of association between different emergency department crowding metrics and repeat visits within 72 hours. Cjem 24(1):27–34
Galipeau J et al (2015) Effectiveness and safety of short-stay units in the emergency department: a systematic review. Acad Emerg Med 22(8):893–907
Voaklander B et al (2022) Interventions to improve consultations in the emergency department: A systematic review. Acad Emerg Med 29(12):1475–1495
Beckerleg W, Wooller K, Hasimjia D (2020) Interventions to reduce emergency department consultation time: A systematic review of the literature. Cjem 22(1):56–64
Plunkett PK et al (2011) Increasing wait times predict increasing mortality for emergency medical admissions. Eur J Emerg Med 18(4):192–6
Lee JH et al (2022) Effect of a Boarding Restriction Protocol on Emergency Department Crowding. Yonsei Med J 63(5):470–479
McKenna P et al (2019) Emergency department and hospital crowding: causes, consequences, and cures. Clin Exp Emerg Med 6(3):189–195
Chang AM et al (2018) Hospital Strategies for Reducing Emergency Department Crowding: A Mixed-Methods Study. Annals of emergency medicine 71(4):497-505.e4
Sartini M et al (2022) Overcrowding in Emergency Department: Causes, Consequences, and Solutions-A Narrative Review. Healthcare (Basel, Switzerland) 10(9):1625
Javidan AP et al (2021) The International Federation for Emergency Medicine report on emergency department crowding and access block: A brief summary. Emerg Med J : EMJ 38(3):245–246
Savioli G et al (2022) Emergency Department Overcrowding: Understanding the Factors to Find Corresponding Solutions. J Personal Med 12(2):279
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Pearce, S., Marr, E., Shannon, T. et al. Overcrowding in emergency departments: an overview of reviews describing global solutions and their outcomes. Intern Emerg Med 19, 483–491 (2024). https://doi.org/10.1007/s11739-023-03477-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11739-023-03477-4