Abstract
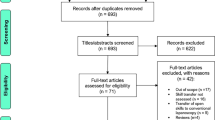
Robotic-Assisted Surgery (RAS) is experiencing rapid expansion, prompting the integration of robotic technical skills training into surgical education programs. As access to robotic training platforms remains limited, it is important to investigate the transferability of laparoscopic skills to RAS. This could potentially support the inclusion of early years laparoscopic training to mitigate the learning curve associated with robotic surgery. This study aims to assess the transferability of laparoscopic skills to robotic surgery. A systematic search was conducted using the PRISMA checklist to identify relevant articles. PubMed, MEDLINE, Embase, and Cochrane databases were searched, and inclusion and exclusion criteria were applied to collate eligible articles. Included were original articles comparing the performance of comparable tasks on both laparoscopic and robotic platforms written in English. Non-peer reviewed papers, conference abstracts, reviews, and case series were excluded. Seventeen articles met the inclusion criteria. Among these, 10 studies (59%) demonstrated skill transferability from laparoscopic surgery (LS) to robotic surgery (RS); while one study (5.8%) showed no significant transferability. Four studies highlighted the positive impact of prior laparoscopic training on robotic skill, whereas six papers suggested no significant difference between laparoscopic novices and experienced laparoscopists when utilizing a robotic simulator. Five studies evaluated advanced surgical skills such as intracorporeal knot tying and suturing, revealing superior robotic performance among experienced laparoscopists compared to novice learners. Laparoscopic skills appear to be transferrable to robotic surgery, particularly in complex surgical techniques. Robotic simulators demonstrate a significant reduction in the learning curve for surgical novices, albeit to a lesser extent for experienced laparoscopists.

Similar content being viewed by others
Data availability
All data supporting the findings of this study are available within the paper and its Supplementary Information. Data is, however, available from the authors upon reasonable request.
References
Lane T (2018) A short history of robotic surgery. Ann R Coll Surg Engl 100(6_sup):5–7. https://doi.org/10.1308/rcsann.supp1.5. (PMID: 29717892; PMCID: PMC5956578)
Kaul S, Shah NL, Menon M (2006) Learning curve using robotic surgery. Curr Urol Rep 7(2):125–129. https://doi.org/10.1007/s11934-006-0071-4
Future of Surgery. Royal College of Surgeons (RCS) (2018) The Future of Surgery. RCS Publications. p 30. https://futureofsurgery.rcseng.ac.uk/report/Future%20of%20Surgery%20Report.pdf. Accessed June 2023
Zendejas B, Ruparel RK, Cook DA (2016) Validity evidence for the fundamentals of laparoscopic surgery (FLS) program as an assessment tool: a systematic review. Surg Endosc 30(2):512–520. https://doi.org/10.1007/s00464-015-4233-7. (Epub 2015 Jun 20. PMID: 26091982)
Page MJ, Moher D, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD et al (2021) PRISMA 2020 explanation and elaboration: updated guidance and exemplars for reporting systematic reviews. BMJ 372:n160
Kilic GS, Walsh TM, Borahay M, Zeybek B, Wen M, Breitkopf D (2012) Effect of residents’ previous laparoscopic surgery experience on initial robotic suturing experience. ISRN Obstetr Gynecol 2012:569456
Finnerty BM, Afaneh C, Aronova A, Fahey TJ 3rd, Zarnegar R (2016) General surgery training and robotics: are residents improving their skills? Surg Endosc 30(2):567–573
Davila DG, Helm MC, Frelich MJ, Gould JC, Goldblatt MI (2018) Robotic skills can be aided by laparoscopic training. Surg Endosc 32(6):2683–2688
Tillou X, Collon S, Martin-Francois S, Doerfler A (2016) Robotic surgery simulator: elements to build a training program. J Surg Educ 73(5):870–878
Moncayo S, Compagnon R, Caire F, Grosos C, Bahans C, Ilhero P et al (2020) Transition effects from laparoscopic to robotic surgery skills in small cavities. J Robot Surg 14(3):525–530
Thomaier L, Orlando M, Abernethy M, Paka C, Chen CCG (2017) Laparoscopic and robotic skills are transferable in a simulation setting: a randomized controlled trial. Surg Endosc 31(8):3279–3285
Obek C, Hubka M, Porter M, Chang L, Porter JR (2005) Robotic versus conventional laparoscopic skill acquisition: implications for training. J Endourol 19(9):1098–1103
Hagen ME, Wagner OJ, Inan I, Morel P (2009) Impact of IQ, computer-gaming skills, general dexterity, and laparoscopic experience on performance with the da Vinci surgical system. Int J Med Robot 5(3):327–331
Angell J, Gomez MS, Baig MM, Abaza R (2013) Contribution of laparoscopic training to robotic proficiency. J Endourol 27(8):1027–1031
Zihni A, Ge T, Ray S, Wang R, Liang Z, Cavallo JA et al (2016) Transfer and priming of surgical skills across minimally invasive surgical platforms. J Surg Res 206(1):48–52
Mehta A, Patel S, Robison W, Senkowski T, Allen J, Shaw E et al (2018) Can teenage novel users perform as well as general surgery residents upon initial exposure to a robotic surgical system simulator? J Robot Surg 12(1):165–171
Kim HJ, Choi G-S, Park JS, Park SY (2014) Comparison of surgical skills in laparoscopic and robotic tasks between experienced surgeons and novices in laparoscopic surgery: an experimental study. Ann Coloproctol 30(2):71–76
Pimentel M, Cabral RD, Costa MM, Neto BS, Cavazzola LT (2018) Does previous laparoscopic experience influence basic robotic surgical skills? J Surg Educ 75(4):1075–1081
Yoo BE, Kim J, Cho JS, Shin JW, Lee DW, Kwak JM et al (2015) Impact of laparoscopic experience on virtual robotic simulator dexterity. J Min Access Surg 11(1):68–71
Kowalewski K-F, Schmidt MW, Proctor T, Pohl M, Wennberg E, Karadza E et al (2018) Skills in minimally invasive and open surgery show limited transferability to robotic surgery: results from a prospective study. Surg Endosc 32(4):1656–1667
Teishima J, Hattori M, Inoue S, Ikeda K, Hieda K, Miyamoto K et al (2012) Impact of laparoscopic experience on the proficiency gain of urologic surgeons in robot-assisted surgery. J Endourol 26(12):1635–1638
Carter FJ, Schijven MP, Aggarwal R, Grantcharov T, Francis NK, Hanna GB et al (2005) Consensus guidelines for validation of virtual reality surgical simulators. Surg Endosc 19(12):1523–1532
Panait L, Doarn CR, Merrell RC (2002) Applications of robotics in surgery. Chirurgia (Bucur) 97(6):549–555
Panait L, Shetty S, Shewokis PA, Sanchez JA (2014) Do laparoscopic skills transfer to robotic surgery? J Surg Res 187(1):53–58
Yohannes P, Rotariu P, Pinto P, Smith AD, Lee BR (2002) Comparison of robotic versus laparoscopic skills: is there a difference in the learning curve? Urology 60(1):39–45 (discussion)
Sanchez BR, Mohr CJ, Morton JM, Safadi BY, Alami RS, Curet MJ (2005) Comparison of totally robotic laparoscopic Roux-en-Y gastric bypass and traditional laparoscopic Roux-en-Y gastric bypass. Surg Obes Relat Dis 1(6):549–554
Ashley CW, Donaldson K, Evans KM, Nielsen B, Everett EN (2019) Surgical cross-training with surgery naive learners: implications for resident training. J Surg Educ 76(6):1469–1475
Melvin WS, Johnson JA, Ellison EC (1996) Laparoscopic skills enhancement. Am J Surg 172(4):377–379
Funding
None.
Author information
Authors and Affiliations
Contributions
JT,JA and JH proposed idea of paper and developed literature review criteria KB performed literature review and collation. JA + MM reviewed results, scrutinised included / excluded papers and contributed to collation. KB developed first draft of main text. LS, GM and MM further developed main text: LS revised introduction and methodology. GS revised results and created tables. JA and MM revised discussion and conclusion. MM and JA wrote final draft along with expertise and further review by MD. All authors reviewed figures, tables and appendix. MM developed abstract and did final formatting and cover letter. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Appendix
Appendix
Appendix 1 Summary of evidence levels [22]
Level of evidence | Criteria |
|---|---|
1a | Systematic reviews (meta-analysis) containing at least some trials of level 1b evidence, in which results of separate, independently conducted trials are consistent |
1b | Randomized controlled trial of good quality and of adequate sample size (power calculation) |
2a | Randomized trials of reasonable quality and/or of inadequate sample size |
2b | Nonrandomized trials, comparative research (parallel cohort) |
2c | Nonrandomized trial, comparative research (historical cohort, literature controls) |
3 | Nonrandomized, noncomparative trials, descriptive research |
4 | Expert opinions, including the opinion of Work Group members |
Appendix 2 Summary of recommendation levels [22]
Level of recommendation | Criteria |
|---|---|
1 | Based on one systematic review (1a) or at least two independently conducted research projects classified as 1b |
2 | Based on at least two independently conducted research projects classified as level 2a or 2b, within concordance |
3 | Based on one independently conducted research project level 2b, or at least two trials of level 3, within concordance |
4 | Based on one trial at level 3 or multiple expert opinions, including the opinion of Work Group members (e.g., level 4) |
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Behera, K., McKenna, M., Smith, L. et al. Transferring laparoscopic skills to robotic-assisted surgery: a systematic review. J Robotic Surg 18, 11 (2024). https://doi.org/10.1007/s11701-023-01757-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11701-023-01757-x