Abstract
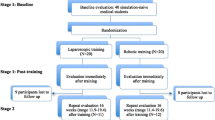
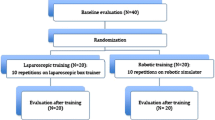
New techniques in minimally invasive and robotic surgical platforms require staged curricula to insure proficiency. Scant literature exists as to how much simulation should play a role in training those who have skills in advanced surgical technology. The abilities of novel users may help discriminate if surgically experienced users should start at a higher simulation level or if the tasks are too rudimentary. The study’s purpose is to explore the ability of General Surgery residents to gain proficiency on the dVSS as compared to novel users. The hypothesis is that Surgery residents will have increased proficiency in skills acquisition as compared to naive users. Six General Surgery residents at a single institution were compared with six teenagers using metrics measured by the dVSS. Participants were given two 1-h sessions to achieve an MScoreTM in the 90th percentile on each of the five simulations. MScoreTM software compiles a variety of metrics including total time, number of attempts, and high score. Statistical analysis was run using Student’s t test. Significance was set at p value <0.05. Total time, attempts, and high score were compared between the two groups. The General Surgery residents took significantly less Total Time to complete Pegboard 1 (PB1) (p = 0.043). No significant difference was evident between the two groups in the other four simulations across the same MScoreTM metrics. A focused look at the energy dissection task revealed that overall score might not be discriminant enough. Our findings indicate that prior medical knowledge or surgical experience does not significantly impact one’s ability to acquire new skills on the dVSS. It is recommended that residency-training programs begin to include exposure to robotic technology.



Similar content being viewed by others
Abbreviations
- dVSS:
-
da Vinci Surgical Simulator
- SAGES:
-
Society of American Gastrointestinal and Endoscopic Surgeons
- MIRA:
-
Minimally Invasive Robotic Association
References
Binder J, Kramer W (2001) Robotically-assisted laparoscopic radical prostatectomy. BJU Int 87:408–410
Loulmet D, Carpentier A, d’Attellis N et al (1999) Endoscopic coronary artery bypass grafting with the aid of robotic assisted instruments. J Thorac Cardiovasc Surg 118:4–10
Zorn KC, Gofrit ON, Steinberg GD et al (2007) Evolution of robotic surgery in the treatment of localized prostate cancer. Curr Treat Options Oncol 8:197–210
Herron DM, Marohn M (2008) A consensus document on robotic surgery. Surg Endosc 22:313–325
Rogula T, Acquafresca PA, Bazan M (2014) Training and credentialing in robotic surgery. In: Essentials of robotic surgery. Springer, Switzerland
Sood A, Menon M, Aggarwal S, Jeong W, Ahlawat R, Campbell L, Bhandari M (2015) Robotic surgical skill acquisition: what one needs to know? J Min Access Surg 11:10–15
Zorn KC, Gautam G, Shalhav AL, Clayman RV, Ahlering TE, Albala DM, Lee DI, Sundaram CP, Matin SF, Castle EP, Winfield HN, Gettman MT, Lee BR, Thomas R, Patel VR, Leveillee RJ, Wong C, Badlani GH, Rha KH, Eggener SE, Wiklund P, Mottrie A, Atug F, Kural AR, Joseph JV (2009) Training, credentialing, proctoring and medicolegal risks of robotic urological surgery: recommendations of the society of urologic robotic surgeons. J Urol 182(3):1126–1132
Lee JY, Mucksavage P, Sundaram CP, Mcdougall EM (2011) Best practices for robotic surgery training and credentialing. J Urol 185(4):1191–1197
Kelly DC, Margules AC, Kundavaram CR, Narins H, Gomella LG, Trabulsi EJ, Lallas CD (2012) Face, content, and construct validation of the da vinci skills simulator. Urology 79(5):1068–1072
Hung AJ, Zehnder P, Patil MB, Cai J, Ng CK, Aron M, Gill IS, Desai MM (2011) Face, content and construct validity of a novel robotic surgery simulator. J Urol 186:1019–1026
Finnegan KT, Meraney AM, Staff I, Shichman SJ (2012) Da vinci skills simulator construct validation study: correlation of prior robotic experience with overall score and time score simulator performance. Urology 80(2):330–336
Farivar BS, Flannagan M, Leitman IM (2015) General surgery residents’ perception of robotic-assisted procedures during surgical training. J Surg Educ 72(2):235–242
Panait L, Shetty S, Shewokis PA (2014) Sanchez JA (2014) Do laparoscopic skills transfer to robotic surgery? J Surg Res 184:53–58
Jenison EL, Gil KM, Lendvay TS, Guy MS (2012) Robotic surgical skills: acquisition, maintenance, and degradation. J Soc Laparosc Surg 16:218–228
Guseila LM, Saranathan A, Jenison EL, Gil KM, Elias JJ (2014) Training to maintain surgical skills during periods of robotic surgery inactivity. Int J Med Robot Comput Assist Surg 10:237–243
Simmonds C (2016) Mimic Technologies Blog. Web log post. Mimic simulation. Mimic Technologies Inc., 1 Feb. 2016. Web. 08 Sept. 2016
Bric J, Connolly M, Kastenmeier A, Goldblatt M, Gould JC (2014) Proficiency training on a virtual reality robotic surgical skills. Surg Endosc 28:3343–3348
Orlando MS, Thomaier L, Abernethy MG, Chen CC (2017) Retention of laparoscopic and robotic skills among medical students: a randomized controlled trial. Surg Endosc 10:1007–1013
Angell J, Gomez MS, Baig MM, Abaza R (2013) Contribution of laproscopic training to robotic proficiency. J Endourol 13(8):1027–1031
Finnerty BM, Afaneh C, Aronova A, Fahey TJ III, Zarnegar R (2016) General surgery training and robotics: are residents improving their skills? Surg Endosc 30:567–573
Öge T, Borahay MA, Achjian T, Kihç SG (2015) Impact of current video game playing on robotic simulation skills among medical students. Journal of Turk-Ger Gynecol Assoc 16:1–4
Kang SG, Ryu BJ, Yang KS, Ko YH, Cho S, Kang SH, Patel VR, Cheon J (2015) An effective repetitive training schedule to achieve skill proficiency using a novel robotic virtual reality simulator. J Surg Educ 72:369–376
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Conflict of interest
Author Mehta A declares that he has no conflict of interest. Author Patel S declares she has no conflict of interest. Author Robison W declares he has no conflict of interest. Author Senkowski T declares he has no conflict of interest. Author Allen J declares he has no conflict of interest. Author Shaw E declares he has no conflict of interest. Author Senkowski C declare he have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Mehta, A., Patel, S., Robison, W. et al. Can teenage novel users perform as well as General Surgery residents upon initial exposure to a robotic surgical system simulator?. J Robotic Surg 12, 165–171 (2018). https://doi.org/10.1007/s11701-017-0715-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11701-017-0715-z