Abstract
Purpose
Obese patients have neurodegeneration of the optic nerve demonstrated by decreased peripapillary nerve fiber layer. Whether bariatric surgery reverses this neurodegenerative process has not been explored. We aimed to evaluate the impact of bariatric surgery in the structure of the retina and optic nerve.
Methods
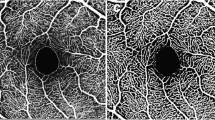
Multicentric observational study. Obese patients scheduled for bariatric surgery were consecutively recruited and included in the study and evaluated before and 6–12 months after the intervention. The retinal structure was evaluated as retinal thickness in the different retinal layers in the foveal, perifoveal, and parafoveal regions using optical coherence tomography. Choroidal thickness and optic nerve retinal nerve fiber layer thickness were also evaluated.
Results
Eighty eyes from 40 participants were included. Globally, we found a significant thickening of the retina after bariatric surgery (foveal: 273.5 (21.5) μm vs 280.0 (28.8) μm, p < 0.001; parafoveal 332.4 ± 17.8 μm vs 336.6 ± 15.9 μm, p = 0.003; perifoveal: 293.4 ± 13.8 μm vs 295.7 ± 14.9 μm; p = 0.001), whereas no significant differences were found for the ganglion cell layer, choroid, or peripapillary nerve fiber layer thickness. The retinal thickening was confined to inner retinal layers and was independent of the diabetic status of the patients. After multivariate adjustment, HbA1c variation, preoperative C-peptide, preoperative hypertension, preoperative OSA, and preoperative LDL and TG levels seem to be clinical predictors of retinal thickening.
Conclusions
We found a significant thickening of the retina after bariatric surgery that was independent of the diabetic status. The thickening was confined to inner retinal layers and may represent and improve perfusion. The peripapillary nerve fiber layer remained unchanged after the surgery.

Similar content being viewed by others
References
WHO. Obesity and overweight - key facts. 2020. Available from: https://www.who.int/news-room/fact-sheets/detail/obesity-and-overweight
Ayer J, Charakida M, Deanfield JE, et al. Lifetime risk: childhood obesity and cardiovascular risk. Eur Heart J. 2015;36:1371–6.
Afshin A, Forouzanfar MH, Reitsma MB, et al. Health effects of overweight and obesity in 195 countries over 25 years. N Engl J Med. 2017;377:13–27.
Bray GA, Frühbeck G, Ryan DH, et al. Management of obesity. Lancet. 2016;387:1947–56.
Fried M, Ribaric G, Buchwald JN, et al. Metabolic surgery for the treatment of type 2 diabetes in patients with BMI. Obes Surg. 2010;20:776–90. Available from: http://link.springer.com/10.1007/s11695-010-0113-3
Wolfe BM, Kvach E, Eckel RH. Treatment of obesity: weight loss and bariatric surgery. Circ Res. 2016;118:1844–55. Available from: http://www.ncbi.nlm.nih.gov/pubmed/27230645http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=PMC4888907
Sheng B, Truong K, Spitler H, et al. The long-term effects of bariatric surgery on type 2 diabetes remission, microvascular and macrovascular complications, and mortality: a systematic review and meta-analysis. Obes Surg. 2017;27:2724–32.
Feldman-Billard S, Larger É, Massin P. Early worsening of diabetic retinopathy after rapid improvement of blood glucose control in patients with diabetes. Diabetes Metab Elsevier Masson SAS. 2017;44:1–11. https://doi.org/10.1016/j.diabet.2017.10.014.
Dahl-Jørgensen K, Brinchmann-Hansen O, Hanssen KF, et al. Rapid tightening of blood glucose control leads to transient deterioration of retinopathy in insulin dependent diabetes mellitus: the Oslo study. Br Med J (Clin Res Ed). 1985;290:811–5.
Ballegooie EV, Hooymans JMM, Timmerman Z, et al. Rapid deterioration of diabetic retinopathy during treatment with continuous subcutaneous insulin infusion. Diabetes Care. 1984;7:236–42. Available from: http://www.bmj.com/cgi/doi/10.1136/bmj.290.6471.811
Lauritzen T, Larsen H-W, Frost-Larsen K, et al. Effect of 1 year of near-normal blood glucose levels on retinopathy in insulin-dependent diabetics. Lancet. 1983;321:200–4. Available from: https://linkinghub.elsevier.com/retrieve/pii/S0140673683925850
Brynskov T, Laugesen CS, Svenningsen AL, Floyd AK, Sørensen TL. Monitoring of diabetic retinopathy in relation to bariatric surgery: a prospective observational study. Obes Surg [Internet]. Obes Surg; 2016;26:1279–1286. https://doi.org/10.1007/s11695-015-1936-8
Miras AD, Chuah LL, Khalil N, et al. Type 2 diabetes mellitus and microvascular complications 1 year after Roux-en-Y gastric bypass: a case–control study. Diabetologia. 2015;58:1443–7.
Sjöström L, Peltonen M, Jacobson P, et al. Association of bariatric surgery with long-term remission of type 2 diabetes and with microvascular and macrovascular complications. JAMA - J Am Med Assoc. 2014;311:2297–304.
Viljanen A, Soinio M, Cheung CY lui, Hannukainen JC, Karlsson HK, Wong TY, et al. Effects of bariatric surgery on retinal microvascular architecture in obese patients. Int J Obes. Springer US; 2018; Available from: https://doi.org/10.1038/s41366-018-0242-7
Abbatini F, Capoccia D, Casella G, et al. Long-term remission of type 2 diabetes in morbidly obese patients after sleeve gastrectomy. Surg Obes Relat Dis. 2013;9:498–502.
Demir S, Özer S, Alim S, Güneş A, Ortak H, Yılmaz R. Retinal nerve fiber layer and ganglion cell-inner plexiform layer thickness in children with obesity. Int J Ophthalmol. 2016 [cited 2018 Aug 4];9:434–8. Available from: http://www.ncbi.nlm.nih.gov/pubmed/27158616
Laiginhas R, Guimarães M, Cardoso P, et al. Retinal nerve fiber layer thickness decrease in obesity as a marker of neurodegeneration. Obes Surg. 2019;
Raman M, Middleton RJ, Kalra PA, et al. Estimating renal function in old people: an in-depth review. Int Urol Nephrol Springer Netherlands. 2017;49:1979–88.
Miras AD, Chuah LL, Lascaratos G, et al. Bariatric surgery does not exacerbate and may be beneficial for the microvascular complications of type 2 diabetes. Diabetes Care. 2012;35:2012.
Morén A, Sundbom M, Ottosson J, et al. Gastric bypass surgery does not increase the risk for sight-threatening diabetic retinopathy. Acta Ophthalmol. 2017:2015–8.
Coleman KJ, Haneuse S, Johnson E, et al. Long-term microvascular disease outcomes in patients with type 2 diabetes after bariatric surgery: evidence for the legacy effect of surgery. Diabetes Care. 2016;39:1400–7.
Dogan B, Dogan U, Erol MK, Habibi M, Bulbuller N. Optical coherence tomography parameters in morbidly obese patients who underwent laparoscopic sleeve gastrectomy. J Ophthalmol. Hindawi Limited; 2016 [cited 2018 May 20];2016:5302368. Available from: http://www.ncbi.nlm.nih.gov/pubmed/27413543
Posarelli C, Salvetti G, Piaggi P, et al. Ophthalmologic evaluation of severely obese patients undergoing bariatric surgery: a pilot, monocentric, prospective, open-label study. PLoS One. 2019;14:1–11.
Brynskov T, Laugesen CS, Floyd AK, et al. Thickening of inner retinal layers in the parafovea after bariatric surgery in patients with type 2 diabetes. Acta Ophthalmol. 2016;94:668–74.
Daruich A, Matet A, Moulin A, Kowalczuk L, Nicolas M, Sellam A, et al. Mechanisms of macular edema: beyond the surface. Prog. Retin. Eye Res. Elsevier Ltd; 2018. Available from: https://doi.org/10.1016/j.preteyeres.2017.10.006
Grizelj I, Cavka A, Bian JT, et al. Reduced flow-and acetylcholine-induced dilations in visceral compared to subcutaneous adipose arterioles in human morbid obesity. Microcirculation. 2015;22:44–53.
Tarzia P, Lanza GA, Sestito A, et al. Long-term effects of bariatric surgery on peripheral endothelial function and coronary microvascular function. Obes Res Clin Pract. 2017;11:114–7.
Tucker WJ, Thomas BP, Puzziferri N, et al. Impact of bariatric surgery on cerebral vascular reactivity and cognitive function: a non-randomized pilot study. Pilot Feasibility Stud. 2020;6:1–13.
Kadłubowska J, Malaguarnera L, Wąż P, et al. Neurodegeneration and neuroinflammation in diabetic retinopathy: potential approaches to delay neuronal loss. Curr Neuropharmacol. 2016;14:831–9.
Dimitriadis GK, Randeva HS, Miras AD. Microvascular complications after metabolic surgery. Lancet Diabetes Endocrinol . Elsevier Ltd; 2017;5:240–1. Available from: https://doi.org/10.1016/S2213-8587(17)30042-6
Carlsson LM, Sjöholm K, Karlsson C, et al. Long-term incidence of microvascular disease after bariatric surgery or usual care in patients with obesity stratified by baseline glucose status. Lancet Diabetes Endocrinol. 2017;5:271–9.
Pierro L, Giatsidis SM, Mantovani E, Gagliardi M. Macular thickness interoperator and intraoperator reproducibility in healthy eyes using 7 optical coherence tomography instruments. Am J Ophthalmol. Elsevier Inc.; 2010;150:199–204.e1. Available from: https://doi.org/10.1016/j.ajo.2010.03.015
Vajzovic L, Hendrickson AE, O’Connell RV, et al. Maturation of the human fovea: correlation of spectral-domain optical coherence tomography findings with histology. Am J Ophthalmol. 2012;154:779–789.e2. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3624763/pdf/nihms412728.pdf
Nieves-Moreno M, Martínez-de-la-Casa JM, Morales-Fernández L, et al. Impacts of age and sex on retinal layer thicknesses measured by spectral domain optical coherence tomography with Spectralis. PLoS One. 2018;13:1–9.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sector.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This manuscript is not submitted or published elsewhere.
Electronic Supplementary Material
ESM 1
(DOCX 23 kb)
Rights and permissions
About this article
Cite this article
Laiginhas, R., Guimarães, M., Cardoso, P. et al. Bariatric Surgery Induces Retinal Thickening Without Affecting the Retinal Nerve Fiber Layer Independent of Diabetic Status. OBES SURG 30, 4877–4884 (2020). https://doi.org/10.1007/s11695-020-04904-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-020-04904-7