Abstract
Background
Laparoscopic sleeve gastrectomy (LSG) has gained popularity as a stand-alone bariatric procedure, but only a few reports provide data of long-term outcomes on high-risk patients.
Objective
To evaluate long-term efficacy of LSG as a definitive management on high-risk obese patients and to study factors that predict its success.
Setting
University hospital in Spain.
Methods
A retrospective analysis of prospectively collected data from 134 high-risk patients undergoing LSG from January 2007 through December 2016. Long-term weight loss, resolution of comorbidities, morbidity, and mortality were analyzed.
Results
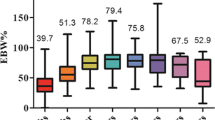
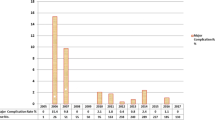
One hundred thirty-four high-risk patients underwent LSG. The mean overall follow-up time was 70.9 ± 4.5 months. The mean age was 47 ± 11.0 years. The mean preoperative body mass index (BMI) was 55.9 ± 6.7 kg/m2 (83.5% were super-obese and 24.6% had BMI ≥ 60). The incidence of postoperative complications was 15%. Mean percentage of total weight loss (%TWL) at 5, 6, 7, and 8 years was 30.7 ± 12.8%, 28.7 ± 14.0%, 29.7 ± 12.3%, and 27.9 ± 11.1%, respectively. Differences were found in age, preoperative BMI, time to reach nadir weight and percentage of excess weight loss (%EWL) at 1 year between patients considered a failure compared to those considered a success. Using multivariate regression analysis, only age (p = 0.009) and time to reach nadir weight after surgery (p = 0.008) correlated with %EWL at 4 years. Resolution of type 2 diabetes (T2DM) was achieved in 62.2% of patients.
Conclusion
This study supports effectiveness and durability of LSG as a definitive bariatric procedure in high-risk patients.



Similar content being viewed by others
References
Buchwald H, Oien DM. Metabolic/bariatric surgery worldwide 2011. Obes Surg. 2013;23(4):427–36.
Marceau P, Biron S, St Georges R, et al. Biliopancreatic diversion with gastrectomy as surgical treatment of morbid obesity. Obes Surg. 1991;1(4):381–7.
Regan JP, Inabnet WB, Gagner M, et al. Early experience with two-stage laparoscopic Roux-en-Y gastric bypass as an alternative in the super-super obese patient. Obes Surg. 2003;13(6):861–4.
Surgery CICotASfMaB. Updated position statement on sleeve gastrectomy as a bariatric procedure. Surg Obes Relat Dis. 2010;6(1):1–5.
Brethauer SA, Hammel JP, Schauer PR. Systematic review of sleeve gastrectomy as staging and primary bariatric procedure. Surg Obes Relat Dis. 2009;5(4):469–75.
Catheline JM, Fysekidis M, Bachner I, et al. Five-year results of sleeve gastrectomy. J Visc Surg. 2013;150(5):307–12.
Braghetto I, Csendes A, Lanzarini E, et al. Is laparoscopic sleeve gastrectomy an acceptable primary bariatric procedure in obese patients? Early and 5-year postoperative results. Surg Laparosc Endosc Percutan Tech. 2012;22(6):479–86.
Christou NV, Look D, Maclean LD. Weight gain after short- and long-limb gastric bypass in patients followed for longer than 10 years. Ann Surg. 2006;244(5):734–40.
Reinhold RB. Critical analysis of long term weight loss following gastric bypass. Surg Gynecol Obstet. 1982;155(3):385–94.
Eid GM, Brethauer S, Mattar SG, et al. Laparoscopic sleeve gastrectomy for super obese patients: forty-eight percent excess weight loss after 6 to 8 years with 93% follow-up. Ann Surg. 2012;256(2):262–5.
Sarela AI, Dexter SP, O'Kane M, et al. Long-term follow-up after laparoscopic sleeve gastrectomy: 8-9-year results. Surg Obes Relat Dis. 2012;8(6):679–84.
Association. WM. World Medical Association Declaration of Helsinki. Ethical principles for medical research involving human subjects. Bull World Health Organ. 2001;79(4):373–4.
Ley Orgánica 15/1999, de 13 de Diciembre, de Protección de datos de Carácter Personal (1999) Boletín Oficial Del Estado: Agencia Estatal Boletín Oficial Del Estado, pp 43088–99.
Gastrointestinal surgery for severe obesity. NIH consensus development conference, March 25-7, 1991. Nutrition. 1996;12(6):397–404.
Hamoui N, Anthone GJ, Kaufman HS, et al. Sleeve gastrectomy in the high-risk patient. Obes Surg. 2006;16(11):1445–9.
Abd Ellatif ME, Abdallah E, Askar W, et al. Long term predictors of success after laparoscopic sleeve gastrectomy. Int J Surg. 2014;12(5):504–8.
Casella G, Soricelli E, Giannotti D, et al. Long-term results after laparoscopic sleeve gastrectomy in a large monocentric series. Surg Obes Relat Dis. 2016;12(4):757–62.
Gadiot RP, Biter LU, van Mil S, et al. Long-term results of laparoscopic sleeve gastrectomy for morbid obesity: 5 to 8-year results. Obes Surg. 2017;27(1):59–63.
Garg H, Aggarwal S, Misra MC, et al. Mid to long term outcomes of laparoscopic sleeve gastrectomy in Indian population: 3-7 year results—a retrospective cohort study. Int J Surg. 2017;48:201–9.
Hirth DA, Jones EL, Rothchild KB, et al. Laparoscopic sleeve gastrectomy: long-term weight loss outcomes. Surg Obes Relat Dis. 2015;11(5):1004–7.
Alexandrou A, Athanasiou A, Michalinos A, et al. Laparoscopic sleeve gastrectomy for morbid obesity: 5-year results. Am J Surg. 2015;209(2):230–4.
Felsenreich DM, Langer FB, Kefurt R, et al. Weight loss, weight regain, and conversions to Roux-en-Y gastric bypass: 10-year results of laparoscopic sleeve gastrectomy. Surg Obes Relat Dis. 2016;12(9):1655–62.
Arman GA, Himpens J, Dhaenens J, et al. Long-term (11+years) outcomes in weight, patient satisfaction, comorbidities, and gastroesophageal reflux treatment after laparoscopic sleeve gastrectomy. Surg Obes Relat Dis. 2016;12(10):1778–86.
Ece I, Yilmaz H, Alptekin H, et al. Comparative effectiveness of laparoscopic sleeve gastrectomy on morbidly obese, super-obese, and super-super obese patients for the treatment of morbid obesity. Obes Surg. 2018;28(6):1484–91.
Chang DM, Lee WJ, Chen JC, et al. Thirteen-year experience of laparoscopic sleeve gastrectomy: surgical risk, weight loss, and revision procedures. Obes Surg. 2018;28:2991–7.
Csendes A, Burgos AM, Martinez G, et al. Loss and regain of weight after laparoscopic sleeve gastrectomy according to preoperative BMI: late results of a prospective study (78-138 months) with 93% of follow-up. Obes Surg. 2018;28:3424–30.
Golomb I, Ben David M, Glass A, et al. Long-term metabolic effects of laparoscopic sleeve gastrectomy. JAMA Surg. 2015;150(11):1051–7.
Li J, Lai D, Wu D. Laparoscopic Roux-en-Y gastric bypass versus laparoscopic sleeve gastrectomy to treat morbid obesity-related comorbidities: a systematic review and meta-analysis. Obes Surg. 2016;26(2):429–42.
Shoar S, Saber AA. Long-term and midterm outcomes of laparoscopic sleeve gastrectomy versus Roux-en-Y gastric bypass: a systematic review and meta-analysis of comparative studies. Surg Obes Relat Dis. 2017;13(2):170–80.
Lemanu DP, Singh PP, Rahman H, et al. Five-year results after laparoscopic sleeve gastrectomy: a prospective study. Surg Obes Relat Dis. 2015;11(3):518–24.
Boza C, Daroch D, Barros D, et al. Long-term outcomes of laparoscopic sleeve gastrectomy as a primary bariatric procedure. Surg Obes Relat Dis. 2014;10(6):1129–33.
Bohdjalian A, Langer FB, Shakeri-Leidenmühler S, et al. Sleeve gastrectomy as sole and definitive bariatric procedure: 5-year results for weight loss and ghrelin. Obes Surg. 2010;20(5):535–40.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The study was approved by the Hospital Ethics Committee. All participants gave informed consent prior to participation in the study. The study complies with the Code of Ethics of the World Medical Association (Declaration of Helsinki) for experiments on human beings [12], and the data were computerized in accordance with the guidelines established by Organic Law 15/1999 on Data Protection [13]. All protocols used were approved by the hospital’s Clinical Research Ethics Committee.
Conflict of Interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Gil–Rendo, A., Muñoz-Rodríguez, J.R., Domper Bardají, F. et al. Laparoscopic Sleeve Gastrectomy for High-Risk Patients in a Monocentric Series: Long-Term Outcomes and Predictors of Success. OBES SURG 29, 3629–3637 (2019). https://doi.org/10.1007/s11695-019-04044-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-019-04044-7