Abstract
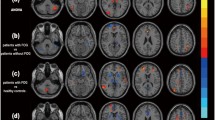
Freezing of gait (FOG), a disabling symptom of Parkinson’s disease (PD), severely affects PD patients’ life quality. Previous studies found neuropathologies in functional connectivity related to FOG, but few studies detected abnormal regional activities related to FOG in PD patients. In the present study, we analyzed the amplitude of low-frequency fluctuations (ALFF) to detect brain regions showing abnormal activity in PD patients with FOG (PD-with-FOG) and without FOG (PD-without-FOG). As different frequencies of neural oscillations in brain may reflect distinct brain functional and physiological properties, we conducted this study in three frequency bands, slow-5 (0.01–0.027 Hz), slow-4 (0.027–0.073 Hz), and classical frequency band (0.01–0.08 Hz). We acquired rs-fMRI data from 18 PD-with-FOG patients, 18 PD-without-FOG patients, and 17 healthy controls, then calculated voxel-wise ALFF across the whole brain and compared ALFF among the three groups in each frequency band. We found: (1) in slow-5, both PD-with-FOG and PD-without-FOG patients showed lower ALFF in the bilateral putamen compared to healthy controls, (2) in slow-4, PD-with-FOG patients showed higher ALFF in left inferior temporal gyrus (ITG) and lower ALFF in right middle frontal gyrus (MFG) compared to either PD-without-FOG patients or healthy controls, (3) in classical frequency band, PD-with-FOG patients also showed higher ALFF in ITG compared to either PD-without-FOG patients or healthy controls. Furthermore, we found that ALFF in MFG and ITG in slow-4 provided the highest classification accuracy (96.7%) in distinguishing PD-with-FOG from PD-without-FOG patients by using a stepwise multivariate pattern analysis. Our findings indicated frequency-specific regional spontaneous neural activity related to FOG, which may help to elucidate the pathogenesis of FOG.



Similar content being viewed by others
References
Aarsland, D., Creese, B., Politis, M., Chaudhuri, K. R., Ffytche, D. H., Weintraub, D., & Ballard, C. (2017). Cognitive decline in Parkinson disease. Nature Reviews. Neurology, 13(4), 217–231. https://doi.org/10.1038/nrneurol.2017.27.
Anand, A., Li, Y., Wang, Y., Wu, J., Gao, S., Bukhari, L., Mathews, V. P., Kalnin, A., & Lowe, M. J. (2005). Activity and connectivity of brain mood regulating circuit in depression: A functional magnetic resonance study. Biological Psychiatry, 57(10), 1079–1088. https://doi.org/10.1016/j.biopsych.2005.02.021.
Birn, R. M., Murphy, K., & Bandettini, P. A. (2008). The effect of respiration variations on independent component analysis results of resting state functional connectivity. Human Brain Mapping, 29(7), 740–750. https://doi.org/10.1002/hbm.20577.
Biswal, B., Yetkin, F. Z., Haughton, V. M., & Hyde, J. S. (1995). Functional connectivity in the motor cortex of resting human brain using echo-planar MRI. Magnetic Resonance in Medicine, 34(4), 537–541. https://doi.org/10.1002/mrm.1910340409.
Brodersen, K. H., Schofield, T. M., Leff, A. P., Ong, C. S., Lomakina, E. I., Buhmann, J. M., & Stephan, K. E. (2011). Generative embedding for model-based classification of fMRI data. PLoS Computational Biology, 7(6), e1002079. https://doi.org/10.1371/journal.pcbi.1002079.
Buzsaki, G., & Draguhn, A. (2004). Neuronal oscillations in cortical networks. Science, 304(5679), 1926–1929. https://doi.org/10.1126/science.1099745.
Cai, S., Tao, C., Peng, Y., Shen, W., Li, J., Deneen, K. M. V., & Huang, L. (2016). Altered functional brain networks in amnestic mild cognitive impairment: A resting-state fMRI study. Brain Imaging and Behavior, 11(3), 619–631. https://doi.org/10.1007/s11682-016-9539-0.
Caminiti, S. P., Presotto, L., Baroncini, D., Garibotto, V., Moresco, R. M., Gianolli, L., Volonté, M. A., Antonini, A., & Perani, D. (2017). Axonal damage and loss of connectivity in nigrostriatal and mesolimbic dopamine pathways in early Parkinson's disease. Neuroimage Clin, 14(C), 734–740. https://doi.org/10.1016/j.nicl.2017.03.011.
Canu, E., Agosta, F., Sarasso, E., Volonte, M. A., Basaia, S., Stojkovic, T., Stefanova, E., Comi, G., Falini, A., Kostic, V. S., Gatti, R., & Filippi, M. (2015). Brain structural and functional connectivity in Parkinson's disease with freezing of gait. Human Brain Mapping, 36(12), 5064–5078. https://doi.org/10.1002/hbm.22994.
Cerasa, A., Pugliese, P., Messina, D., Morelli, M., Gioia, M. C., Salsone, M., Novellino, F., Nicoletti, G., Arabia, G., & Quattrone, A. (2012). Prefrontal alterations in Parkinson's disease with levodopa-induced dyskinesia during fMRI motor task. Movement Disorders, 27(3), 364–371. https://doi.org/10.1002/mds.24017.
Chen, H. M., Wang, Z. J., Fang, J. P., Gao, L. Y., Ma, L. Y., Wu, T., Hou, Y. N., Zhang, J. R., & Feng, T. (2015). Different patterns of spontaneous brain activity between tremor-dominant and postural instability/gait difficulty subtypes of Parkinson's disease: A resting-state fMRI study. CNS Neuroscience & Therapeutics, 21(10), 855–866. https://doi.org/10.1111/cns.12464.
Choe, I. H., Yeo, S., Chung, K. C., Kim, S. H., & Lim, S. (2013). Decreased and increased cerebral regional homogeneity in early Parkinson's disease. Brain Research, 1527, 230–237. https://doi.org/10.1016/j.brainres.2013.06.027.
Curtis, C. E. (2006). Prefrontal and parietal contributions to spatial working memory. Neuroscience, 139(1), 173–180. https://doi.org/10.1016/j.neuroscience.2005.04.070.
Dai, Z., Yan, C., Wang, Z., Wang, J., Xia, M., Li, K., & He, Y. (2012). Discriminative analysis of early Alzheimer's disease using multi-modal imaging and multi-level characterization with multi-classifier (M3). Neuroimage, 59(3), 2187–2195. https://doi.org/10.1016/j.neuroimage.2011.10.003.
Di Martino, A., Ghaffari, M., Curchack, J., Reiss, P., Hyde, C., Vannucci, M., Petkova, E., Klein, D. F., & Castellanos, F. X. (2008). Decomposing intra-subject variability in children with attention-deficit/hyperactivity disorder. Biological Psychiatry, 64(7), 607–614. https://doi.org/10.1016/j.biopsych.2008.03.008.
Diener, C., Kuehner, C., Brusniak, W., Ubl, B., Wessa, M., & Flor, H. (2012). A meta-analysis of neurofunctional imaging studies of emotion and cognition in major depression. Neuroimage, 61(3), 677–685. https://doi.org/10.1016/j.neuroimage.2012.04.005.
Esposito, F., Tessitore, A., Giordano, A., De Micco, R., Paccone, A., Conforti, R., Pignataro, G., Annunziato, L., & Tedeschi, G. (2013). Rhythm-specific modulation of the sensorimotor network in drug-naive patients with Parkinson's disease by levodopa. Brain, 136(Pt 3), 710–725. https://doi.org/10.1093/brain/awt007.
Ffytche, D. H., Creese, B., Politis, M., Chaudhuri, K. R., Weintraub, D., Ballard, C., & Aarsland, D. (2017). The psychosis spectrum in Parkinson disease. Nature Reviews. Neurology, 13(2), 81–95. https://doi.org/10.1038/nrneurol.2016.200.
Folstein, M. F., Folstein, S. E., & McHugh, P. R. (1975). Mini-mental state. A practical method for grading the cognitive state of patients for the clinician. Journal of Psychiatric Research, 12(3), 189–198. https://doi.org/10.1016/0022-3956(75)90026-6.
Fransson, P. (2005). Spontaneous low-frequency BOLD signal fluctuations: An fMRI investigation of the resting-state default mode of brain function hypothesis. Human Brain Mapping, 26(1), 15–29. https://doi.org/10.1002/hbm.20113.
Giladi, N., & Nieuwboer, A. (2008). Understanding and treating freezing of gait in parkinsonism, proposed working definition, and setting the stage. Movement Disorders, 23(Suppl 2), S423–S425. https://doi.org/10.1002/mds.21927.
Giladi, N., Shabtai, H., Simon, E. S., Biran, S., Tal, J., & Korczyn, A. D. (2000). Construction of freezing of gait questionnaire for patients with parkinsonism. Parkinsonism & Related Disorders, 6(3), 165–170. https://doi.org/10.1016/S1353-8020(99)00062-0.
Goetz, C. G. (2003). The unified Parkinson's disease rating scale (UPDRS): Status and recommendations. Movement Disorders, 18(7), 738–750. https://doi.org/10.1002/mds.10473.
Goldstein, D. S., Sullivan, P., Holmes, C., Mash, D. C., Kopin, I. J., & Sharabi, Y. (2017). Determinants of denervation-independent depletion of putamen dopamine in Parkinson's disease and multiple system atrophy. Parkinsonism & Related Disorders, 35, 88–91. https://doi.org/10.1016/j.parkreldis.2016.12.011.
Gratwicke, J., Jahanshahi, M., & Foltynie, T. (2015). Parkinson’s disease dementia: A neural networks perspective. Brain, 138(6), 1454–1476. https://doi.org/10.1093/brain/awv104.
Hoehn, M. M., & Yahr, M. D. (1998). Parkinsonism: onset, progression, and mortality. Neurology, 50(2), 11–26. https://doi.org/10.1212/WNL.17.5.427.
Hou, Y., Wu, X., Hallett, M., Chan, P., & Wu, T. (2014). Frequency-dependent neural activity in Parkinson's disease. Human Brain Mapping, 35(12), 5815–5833. https://doi.org/10.1002/hbm.22587.
Hughes, A. J., Daniel, S. E., Kilford, L., & Lees, A. J. (1992). Accuracy of clinical diagnosis of idiopathic Parkinson's disease: A clinico-pathological study of 100 cases. Journal of Neurology, Neurosurgery, and Psychiatry, 55(3), 181–184. https://doi.org/10.1136/jnnp.55.3.181.
Jackson, R. L., Bajada, C. J., Rice, G. E., Cloutman, L. L., & Lambon Ralph, M. A. (2018). An emergent functional parcellation of the temporal cortex. Neuroimage, 170, 385–399. https://doi.org/10.1016/j.neuroimage.2017.04.024.
Jenkinson, M., Bannister, P., Brady, M., & Smith, S. (2002). Improved optimization for the robust and accurate linear registration and motion correction of brain images. Neuroimage, 17(2), 825–841. https://doi.org/10.1006/nimg.2002.1132.
Kalia, L. V., & Lang, A. E. (2015). Parkinson's disease. Lancet, 386(9996), 896–912. https://doi.org/10.1016/s0140-6736(14)61393-3.
Kamei, S. (2013). Executive dysfunction in Parkinson’s disease: A review. Journal of Neuropsychology, 7(2), 193–224. https://doi.org/10.1111/jnp.12028.
Kish, S. J., Boileau, I., Callaghan, R. C., & Tong, J. (2017). Brain dopamine neurone 'damage': Methamphetamine users vs. Parkinson's disease - a critical assessment of the evidence. The European Journal of Neuroscience, 45(1), 58–66. https://doi.org/10.1111/ejn.13363.
Kiviniemi, V., Kantola, J. H., Jauhiainen, J., Hyvarinen, A., & Tervonen, O. (2003). Independent component analysis of nondeterministic fMRI signal sources. Neuroimage, 19(2 Pt 1), 253–260. https://doi.org/10.1016/S1053-8119(03)00097-1.
Kwak, Y., Peltier, S. J., Bohnen, N. I., Muller, M. L., Dayalu, P., & Seidler, R. D. (2012). L-DOPA changes spontaneous low-frequency BOLD signal oscillations in Parkinson's disease: A resting state fMRI study. Frontiers in Systems Neuroscience, 6(6), 52. https://doi.org/10.3389/fnsys.2012.00052.
Lee, S. Y., Kim, M. S., Chang, W. H., Cho, J. W., Youn, J. Y., & Kim, Y. H. (2014). Effects of repetitive transcranial magnetic stimulation on freezing of gait in patients with parkinsonism. Restorative Neurology and Neuroscience, 32(6), 743–753. https://doi.org/10.3233/rnn-140397.
Lefaucheur, J. P., Andre-Obadia, N., Antal, A., Ayache, S. S., Baeken, C., Benninger, D. H., Cantello, R. M., Cincotta, M., de Carvalho, M., De Ridder, D., Devanne, H., Di Lazzaro, V., Filipovic, S. R., Hummel, F. C., Jaaskelainen, S. K., Kimiskidis, V. K., Koch, G., Langguth, B., Nyffeler, T., Oliviero, A., Padberg, F., Poulet, E., Rossi, S., Rossini, P. M., Rothwell, J. C., Schonfeldt-Lecuona, C., Siebner, H. R., Slotema, C. W., Stagg, C. J., Valls-Sole, J., Ziemann, U., Paulus, W., & Garcia-Larrea, L. (2014). Evidence-based guidelines on the therapeutic use of repetitive transcranial magnetic stimulation (rTMS). Clinical Neurophysiology, 125(11), 2150–2206. https://doi.org/10.1016/j.clinph.2014.05.021.
Lenka, A., Naduthota, R. M., Jha, M., Panda, R., Prajapati, A., Jhunjhunwala, K., Saini, J., Yadav, R., Bharath, R. D., & Pal, P. K. (2016). Freezing of gait in Parkinson's disease is associated with altered functional brain connectivity. Parkinsonism & Related Disorders, 24, 100–106. https://doi.org/10.1016/j.parkreldis.2015.12.016.
Lewis, S. J., & Shine, J. M. (2016). The next step: A common neural mechanism for freezing of gait. Neuroscientist, 22(1), 72–82. https://doi.org/10.1177/1073858414559101.
Li, C., Huang, B., Zhang, R., Ma, Q., Yang, W., Wang, L., Wang, L., Xu, Q., Feng, J., Liu, L., Zhang, Y., & Huang, R. (2017a). Impaired topological architecture of brain structural networks in idiopathic Parkinson's disease: A DTI study. Brain Imaging and Behavior, 11(1), 113–128. https://doi.org/10.1007/s11682-015-9501-6.
Li, D., Huang, P., Zang, Y., Lou, Y., Cen, Z., Gu, Q., Xuan, M., Xie, F., Ouyang, Z., Wang, B., Zhang, M., & Luo, W. (2017b). Abnormal baseline brain activity in Parkinson's disease with and without REM sleep behavior disorder: A resting-state functional MRI study. Journal of Magnetic Resonance Imaging, 46(3), 697–703. https://doi.org/10.1002/jmri.25571.
Man, A., Tsoi, T. H., Mok, V., Cheung, C. M., Lee, C. N., Li, R., & Yeung, E. (2012). Ten year survival and outcomes in a prospective cohort of new onset Chinese Parkinson's disease patients. Journal of Neurology, Neurosurgery, and Psychiatry, 83(6), 607–611. https://doi.org/10.1136/jnnp-2011-301590.
Mi, T. M., Mei, S. S., Liang, P. P., Gao, L. L., Li, K. C., Wu, T., & Chan, P. (2017). Altered resting-state brain activity in Parkinson's disease patients with freezing of gait. Scientific Reports, 7(1), 16711. https://doi.org/10.1038/s41598-017-16922-0.
Michely, J., Volz, L. J., Barbe, M. T., Hoffstaedter, F., Viswanathan, S., Timmermann, L., Eickhoff, S. B., Fink, G. R., & Grefkes, C. (2015). Dopaminergic modulation of motor network dynamics in Parkinson's disease. Brain, 138(Pt 3), 664–678. https://doi.org/10.1093/brain/awu381.
Moore, S. T., Yungher, D. A., Morris, T. R., Dilda, V., MacDougall, H. G., Shine, J. M., Naismith, S. L., & Lewis, S. J. (2013). Autonomous identification of freezing of gait in Parkinson's disease from lower-body segmental accelerometry. Journal of Neuroengineering and Rehabilitation, 10, 19. https://doi.org/10.1186/1743-0003-10-19.
Naismith, S. L., Shine, J. M., & Lewis, S. J. (2010). The specific contributions of set-shifting to freezing of gait in Parkinson's disease. Movement Disorders, 25(8), 1000–1004. https://doi.org/10.1002/mds.23005.
Nitschke, K., Kostering, L., Finkel, L., Weiller, C., & Kaller, C. P. (2017). A meta-analysis on the neural basis of planning: Activation likelihood estimation of functional brain imaging results in the tower of London task. Human Brain Mapping, 38(1), 396–413. https://doi.org/10.1002/hbm.23368.
Nonnekes, J., Snijders, A. H., Nutt, J. G., Deuschl, G., Giladi, N., & Bloem, B. R. (2015). Freezing of gait: A practical approach to management. Lancet Neurology, 14(7), 768–778. https://doi.org/10.1016/S1474-4422(15)00041-1.
Nutt, J. G., Bloem, B. R., Giladi, N., Hallett, M., Horak, F. B., & Nieuwboer, A. (2011). Freezing of gait: Moving forward on a mysterious clinical phenomenon. Lancet Neurology, 10(8), 734–744. https://doi.org/10.1016/s1474-4422(11)70143-0.
Ogawa, S., & Lee, T. M. (1990). Magnetic resonance imaging of blood vessels at high fields: In vivo and in vitro measurements and image simulation. Magnetic Resonance in Medicine, 16(1), 9–18. https://doi.org/10.1002/mrm.1910160103.
Pan, P., Zhang, Y., Liu, Y., Zhang, H., Guan, D., & Xu, Y. (2017). Abnormalities of regional brain function in Parkinson's disease: A meta-analysis of resting state functional magnetic resonance imaging studies. Scientific Reports, 7, 40469. https://doi.org/10.1038/srep40469.
Pereira, F., Mitchell, T., & Botvinick, M. (2009). Machine learning classifiers and fMRI: A tutorial overview. Neuroimage, 45(1), S199–S209. https://doi.org/10.1016/j.neuroimage.2008.11.007.
Prodoehl, J., Spraker, M., Corcos, D., Comella, C., & Vaillancourt, D. (2010). Blood oxygenation level dependent activation in basal ganglia nuclei relates to specific symptoms in De novo Parkinson's disease. Movement Disorders, 25(13), 2035–2043. https://doi.org/10.1002/mds.23360.
Ricciardi, L., Bloem, B. R., Snijders, A. H., Daniele, A., Quaranta, D., Bentivoglio, A. R., & Fasano, A. (2014). Freezing of gait in Parkinson's disease: The paradoxical interplay between gait and cognition. Parkinsonism & Related Disorders, 20(8), 824–829. https://doi.org/10.1016/j.parkreldis.2014.04.009.
Rodriguez-Oroz, M. C., Jahanshahi, M., Krack, P., Litvan, I., Macias, R., Bezard, E., & Obeso, J. A. (2009). Initial clinical manifestations of Parkinson's disease: Features and pathophysiological mechanisms. Lancet Neurology, 8(12), 1128–1139. https://doi.org/10.1016/s1474-4422(09)70293-5.
Salvador, R., Martinez, A., Pomarol-Clotet, E., Gomar, J., Vila, F., Sarro, S., Capdevila, A., & Bullmore, E. (2008). A simple view of the brain through a frequency-specific functional connectivity measure. Neuroimage, 39(1), 279–289. https://doi.org/10.1016/j.neuroimage.2007.08.018.
Shine, J. M., Matar, E., Ward, P. B., Frank, M. J., Moustafa, A. A., Pearson, M., Naismith, S. L., & Lewis, S. J. (2013). Freezing of gait in Parkinson's disease is associated with functional decoupling between the cognitive control network and the basal ganglia. Brain, 136(Pt 12), 3671–3681. https://doi.org/10.1093/brain/awt272.
Skidmore, F. M., Yang, M., Baxter, L., von Deneen, K. M., Collingwood, J., He, G., White, K., Korenkevych, D., Savenkov, A., Heilman, K. M., Gold, M., & Liu, Y. (2013). Reliability analysis of the resting state can sensitively and specifically identify the presence of Parkinson disease. Neuroimage, 75, 249–261. https://doi.org/10.1016/j.neuroimage.2011.06.056.
Snijders, A. H., Takakusaki, K., Debu, B., Lozano, A. M., Krishna, V., Fasano, A., Aziz, T. Z., Papa, S. M., Factor, S. A., & Hallett, M. (2016). Physiology of freezing of gait. Annals of Neurology, 80(5), 644–659. https://doi.org/10.1002/ana.24778.
Tahmasian, M., Eickhoff, S.B., Giehl, K., Schwartz, F., Herz, D.M., Drzezga, A., van Eimeren, T., Laird, A.R., Fox, P.T., Khazaie, H., Zarei, M., Eggers, C., Eickhoff, C.R. Resting-state functional reorganization in Parkinson's disease: An activation likelihood estimation meta-analysis. Cortex 2017; 92: 119–138. https://doi.org/10.1016/j.cortex.2017.03.016.
Tessitore, A., Amboni, M., Esposito, F., Russo, A., Picillo, M., Marcuccio, L., Pellecchia, M. T., Vitale, C., Cirillo, M., Tedeschi, G., & Barone, P. (2012). Resting-state brain connectivity in patients with Parkinson's disease and freezing of gait. Parkinsonism & Related Disorders, 18(6), 781–787. https://doi.org/10.1016/j.parkreldis.2012.03.018.
van Buuren, M., Gladwin, T. E., Zandbelt, B. B., van den Heuvel, M., Ramsey, N. F., Kahn, R. S., & Vink, M. (2009). Cardiorespiratory effects on default-mode network activity as measured with fMRI. Human Brain Mapping, 30(9), 3031–3042. https://doi.org/10.1002/hbm.20729.
Vandenbossche, J., Deroost, N., Soetens, E., Spildooren, J., Vercruysse, S., Nieuwboer, A., & Kerckhofs, E. (2011). Freezing of gait in Parkinson disease is associated with impaired conflict resolution. Neurorehabilitation and Neural Repair, 25(8), 765–773. https://doi.org/10.1177/1545968311403493.
Vercruysse, S., Spildooren, J., Heremans, E., Wenderoth, N., Swinnen, S. P., Vandenberghe, W., & Nieuwboer, A. (2014). The neural correlates of upper limb motor blocks in Parkinson's disease and their relation to freezing of gait. Cerebral Cortex, 24(12), 3154–3166. https://doi.org/10.1093/cercor/bht170.
Vervoort, G., Heremans, E., Bengevoord, A., Strouwen, C., Nackaerts, E., Vandenberghe, W., & Nieuwboer, A. (2016). Dual-task-related neural connectivity changes in patients with Parkinson' disease. Neuroscience, 317, 36–46. https://doi.org/10.1016/j.neuroscience.2015.12.056.
Visser, M., Jefferies, E., Embleton, K. V., & Lambon Ralph, M. A. (2012). Both the middle temporal gyrus and the ventral anterior temporal area are crucial for multimodal semantic processing: Distortion-corrected fMRI evidence for a double gradient of information convergence in the temporal lobes. Journal of Cognitive Neuroscience, 24(8), 1766–1778. https://doi.org/10.1162/jocn_a_00244.
Wu, T., & Hallett, M. (2013). The cerebellum in Parkinson's disease. Brain, 136(Pt 3), 696–709. https://doi.org/10.1093/brain/aws360.
Xue, S., Wang, X., Wang, W., Liu, J., & Qiu, J. (2016). Frequency-dependent alterations in regional homogeneity in major depression. Behavioural Brain Research, 306, 13–19. https://doi.org/10.1016/j.bbr.2016.03.012.
Yang, H., Long, X. Y., Yang, Y., Yan, H., Zhu, C. Z., Zhou, X. P., Zang, Y. F., & Gong, Q. Y. (2007). Amplitude of low frequency fluctuation within visual areas revealed by resting-state functional MRI. Neuroimage, 36(1), 144–152. https://doi.org/10.1016/j.neuroimage.2007.01.054.
Zach, H., Janssen, A. M., Snijders, A. H., Delval, A., Ferraye, M. U., Auff, E., Weerdesteyn, V., Bloem, B. R., & Nonnekes, J. (2015). Identifying freezing of gait in Parkinson's disease during freezing provoking tasks using waist-mounted accelerometry. Parkinsonism & Related Disorders, 21(11), 1362–1366. https://doi.org/10.1016/j.parkreldis.2015.09.051.
Zang, Y. F., He, Y., Zhu, C. Z., Cao, Q. J., Sui, M. Q., Liang, M., Tian, L. X., Jiang, T. Z., & Wang, Y. F. (2007). Altered baseline brain activity in children with ADHD revealed by resting-state functional MRI. Brain & Development, 29(2), 83–91. https://doi.org/10.1016/j.braindev.2006.07.002.
Zhong, M., Yang, W., Huang, B., Jiang, W., Zhang, X., Liu, X., Wang, L., Wang, J., Zhao, L., Zhang, Y., Liu, Y., Lin, J., & Huang, R. (2018). Effects of levodopa therapy on voxel-based degree centrality in Parkinson's disease. Brain Imaging and Behavior. https://doi.org/10.1007/s11682-018-9936-7.
Zhu, W., Fu, X., Cui, F., Yang, F., Ren, Y., Zhang, X., Zhang, X., Chen, Z., Ling, L., & Huang, X. (2015). ALFF value in right Parahippocampal gyrus acts as a potential marker monitoring amyotrophic lateral sclerosis progression: A neuropsychological, voxel-based morphometry, and resting-state functional MRI study. Journal of Molecular Neuroscience, 57(1), 106–113. https://doi.org/10.1007/s12031-015-0583-9.
Zuo, X. N., Di Martino, A., Kelly, C., Shehzad, Z. E., Gee, D. G., Klein, D. F., Castellanos, F. X., Biswal, B. B., & Milham, M. P. (2010). The oscillating brain: Complex and reliable. Neuroimage, 49(2), 1432–1445. https://doi.org/10.1016/j.neuroimage.2009.09.037.
Acknowledgments
The study was supported by grants from the National Natural Science Foundation of China [Grant numbers: 81871338, 81471654, 81428013, 81671275, and 81371535]; Planned Science and Technology Project of Guangdong Province, China [Grant numbers: 2014B020212022, 1563000653, 20160402007]; Innovation Project of Graduate School of South China Normal University. The funding organizations played no further role in study design, data collection, analysis and interpretation, and paper writing. The authors appreciate the editing assistance of Drs.Rhoda E. and Edmund F. Perozzi.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Informed consent
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2000. Informed consent was obtained from all participants for being included in the study.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hu, H., Chen, J., Huang, H. et al. Common and specific altered amplitude of low-frequency fluctuations in Parkinson’s disease patients with and without freezing of gait in different frequency bands. Brain Imaging and Behavior 14, 857–868 (2020). https://doi.org/10.1007/s11682-018-0031-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11682-018-0031-x