Abstract
Purpose
Osteosarcopenic obesity syndrome (OSO) is a recently recognized disorder encompassing osteopenia/osteoporosis, sarcopenia, and obesity. However, evidence in pooling knowledge regarding the prevalence of OSO worldwide is scarce. Hence, this review aimed to determine the pooled prevalence of OSO in middle-aged and older adults.
Methods
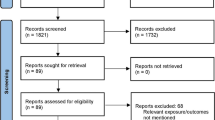
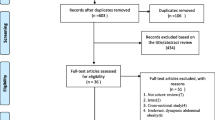
We conducted systematic searches in Scopus, Embase, PubMed Central, MEDLINE, ScienceDirect, and Google Scholar from inception until October 2022. We evaluated the quality of the included studies using the Newcastle–Ottawa scale. The meta-analysis results using a random-effects model included the pooled prevalence and 95% confidence intervals (CIs).
Results
We included 20 studies with a total of 23,909 participants. Most of the studies were of good quality. The final pooled prevalence of OSO in middle-aged and older adults worldwide was 8% (95% CI: 6%-11%; n = 20). Females (pooled prevalence = 9%; 95% CI:7%-12%; n = 17) had a higher burden of OSO than males (pooled prevalence = 5%; 95% CI:3%-8%; n = 11). We also found that the burden was higher among studies reporting OSO prevalence only in the elderly population (pooled prevalence = 13%; 95% CI: 9%-17%). The asymmetric nature of the funnel plot indicates the presence of publication bias. Additional sensitivity analysis did not reveal any significant variation in the pooled effect size estimation.
Conclusion
Approximately one in ten middle-aged and older adults suffer from OSO. The burden was highest among females and older adults. Diagnostic and intervention packages targeting such patients should be developed and implemented in high-risk settings.






Similar content being viewed by others
Data Availability
Data will be made available upon reasonable request from investigators.
References:
Ilich JZ, Kelly OJ, Inglis JE, Panton LB, Duque G, Ormsbee MJ (2014) Interrelationship among muscle, fat, and bone: Connecting the dots on cellular, hormonal, and whole body levels. Ageing Res Rev 15:51–60
JafariNasabian P, Inglis JE, Kelly OJ, Ilich JZ (2017) Osteosarcopenic obesity in women: Impact, prevalence, and management challenges. Int J Women Health 9:33–42
Ilich JZ, Kelly OJ, Inglis JE (2016) Osteosarcopenic obesity syndrome: What is it and how can it be identified and diagnosed? Curr Gerontol Geriatr Res 2016:7325973
Kaji H (2013) Linkage between muscle and bone: Common catabolic signals resulting in osteoporosis and sarcopenia. Curr Opin Clin Nutr Metab Care 16:272–277
Reginster JY, Beaudart C, Buckinx F, Bruyere O (2016) Osteoporosis and sarcopenia: Two diseases or one? Curr Opin Clin Nutr Metab Care 19:31–36
Stenholm S, Harris TB, Rantanen T, Visser M, Kritchevsky SB, Ferrucci L (2008) Sarcopenic obesity: Definition, cause and consequences. Curr Opin Clin Nutr Metab Care 11:693–700
Zamboni M, Mazzali G, Fantin F, Rossi A, Di Francesco V (2008) Sarcopenic obesity: A new category of obesity in the elderly. Nutr Metab Cardiovasc Dis 18:388–395
Vaidya R (2014) Obesity, sarcopenia and postmenopausal osteoporosis: An interlinked triad. J Midlife Health 5:1–2
School of Biosciences, Faculty of Science and Engineering, University of Nottingham Malaysia, Mitra SR, Abidin NZ, School of Biosciences, Faculty of Science and Engineering, University of Nottingham Malaysia, Lifestyle Science Cluster, Advanced Medical and Dental Institute, Universiti Sains Malaysia, Malaysia. Comparison of anthropometric profile, bone-related parameters, biochemical parameters, functional capacity, and vitamin D status – A study on postmenopausal Malaysian women. Mal J Nutr [Internet]. 2021 Jul 28 [cited 2022 Nov 21];27(2). Available from: https://www.nutriweb.org.my/mjn/publication/27-2/Vol%2027(2)%205.%20mjn.2020.0080%20Soma%20Mitra%20(online%20first)%20final.pdf
Pang BWJ, Wee SL, Chen KK, Lau LK, Jabbar KA, Seah WT et al (2021) Coexistence of osteoporosis, sarcopenia and obesity in community-dwelling adults – The Yishun Study. Osteoporos Sarcopenia 7(1):17–23
Chung JH, Hwang HJ, Shin HY, Han CH (2016) Association between Sarcopenic Obesity and Bone Mineral Density in Middle-Aged and Elderly Korean. Ann Nutr Metab 68(2):77–84
Chen X, Kong C, Yu H, Gong J, Lan L, Zhou L et al (2019) Association between osteosarcopenic obesity and hypertension among four minority populations in China: a cross-sectional study. BMJ Open 9(7):e026818
Abidin NZ, Mitra SR (2021) Determination of Cutoff Values for the Screening of Osteosarcopenia in Obese Postmenopausal Women. Kuo YF, editor. Curr Gerontol Geriatr Res 2021:1–15
Moher D, Liberati A, Tetzlaff J, Altman DG (2010) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Int J Surg 8:336–341
Peterson J, Welch V, Losos M, Tugwell P (2011) The Newcastle-Ottawa scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses. Ottawa Hospital Research Institute, Ottawa
Nyaga VN, Arbyn M, Aerts M (2014) Metaprop: a Stata command to perform meta-analysis of binomial data. Arch Public Health 72:39
Higgins JP, Green S, editors. (2011) Cochrane handbook for systematic reviews of interventions. John Wiley & Sons
Egger M, Davey Smith G, Schneider M et al (1997) Bias in meta-analysis detected by a simple, graphical test. BMJ 315:629–634
Su YH, Chang YM, Kung CY, Sung CK, Foo WS, Wu MH et al (2021) A study of correlations between metabolic syndrome factors and osteosarcopenic adiposity. BMC Endocr Disord 21(1):216
Kashiwagi K, Takayama M, Ichikawa H, Takaishi H, Iwao Y, Kanai T (2021) A significant association of non-obese non-alcoholic fatty liver disease with osteosarcopenic obesity in females 50 years and older. Clin Nutr ESPEN 42:166–172
Bae YJ (2020) Fruit intake and osteosarcopenic obesity in Korean postmenopausal women aged 50–64 years. Maturitas 134:41–46
Nie YZ, Yan ZQ, Yin H, Shan LH, Wang JH, Wu QH (2022) Osteosarcopenic obesity and its components—osteoporosis, sarcopenia, and obesity—are associated with blood cell count-derived inflammation indices in older Chinese people. BMC Geriatr 22(1):532
Mo D, Hsieh P, Yu H, Zhou L, Gong J, Xu L et al (2018) Osteosarcopenic obesity and its relationship with dyslipidemia in women from different ethnic groups of China. Arch Osteoporos 13(1):65
Saltzman BS, Kenney KC (2019) Osteosarcopenic obesity and vitamin d in u.s. Adults ages 50 and older: a cross-sectional study. Innov Aging 3(Suppl 1):S481. https://doi.org/10.1093/geroni/igz038.1789.
Ma Y, Zhang W, Han P, Kohzuki M, Guo Q (2020) Osteosarcopenic Obesity Associated with Poor Physical Performance in the Elderly Chinese Community. CIA 15:1343–1352
Ilich JZ, Inglis JE, Kelly OJ, McGee DL (2015) Osteosarcopenic obesity is associated with reduced handgrip strength, walking abilities, and balance in postmenopausal women. Osteoporos Int 26(11):2587–2595
Keramidaki K, Tsagari A, Hiona M, Risvas G (2019) Osteosarcopenic obesity, the coexistence of osteoporosis, sarcopenia and obesity and consequences in the quality of life in older adults ≥365 years-old in Greece. JFSF 1:91–101
Szlejf C, Parra-Rodríguez L, Rosas-Carrasco O (2017) Osteosarcopenic Obesity: Prevalence and Relation With Frailty and Physical Performance in Middle-Aged and Older Women. J Am Med Dir Assoc 18(8):733.e1-733.e5
Perna S, Spadaccini D, Nichetti M, Avanzato I, Faliva MA, Rondanelli M (2018) Osteosarcopenic Visceral Obesity and Osteosarcopenic Subcutaneous Obesity, Two New Phenotypes of Sarcopenia: Prevalence, Metabolic Profile, and Risk Factors. J Aging Res 2018:1–8
de Jaeger C, Voronska E, Lamberti C, Saskia K, Cherin P (2021) Prevalence of Osteo-Sarcopenia and Osteosarcopenic Obesity in Healthy Ambulatory Subjects older than 45 years in France 2:7
Sasaki K-I, Kakuma T, Sasaki M, Ishizaki Y, Fukami A, Enomoto M et al (2020) The prevalence of sarcopenia and subtypes in cardiovascular diseases, and a new diagnostic approach. J Cardiol 76(3):266–272
OkyarBaş A, GünerOytun M, Deniz O, Öztürk Y, Kahyaoğlu Z, Ceylan S et al (2022) Ultrasonografically assessed osteosarcopenic obesity is associated with frailty in community-dwelling older adults. Nutrition 103–104:111827
Kolbaşı EN, Demirdağ F (2020) Prevalence of osteosarcopenic obesity in community-dwelling older adults: a cross-sectional retrospective study. Arch Osteoporos 15(1):1–9
Bauer JM, Cruz-Jentoft AJ, Fielding RA, Kanis JA, Reginster JY, Bruyère O et al (2019) Is there enough evidence for osteosarcopenic obesity as a distinct entity? A critical literature review. Calcif Tissue Int 105(2):109–124
Cruz-Jentoft AJ, Bahat G, Bauer J, Boirie Y, Bruyere O, Cederholm T et al (2018) Sarcopenia: revised European consensus on definition and diagnosis. Age Ageing. https://doi.org/10.1093/ageing/afy169
World Health Organization. Obesity. [cited 21 Nov 2022] [Internet]. Available from: https://www.who.int/health-topics/obesity#tab=tab_1
Kanis JA, Melton LJ 3rd, Christiansen C, Johnston CC, Khaltaev N (1994) The diagnosis of osteoporosis. J Bone Miner Res 9(8):1137–1141. https://doi.org/10.1002/jbmr.5650090802
Scott D, Daly RM, Sanders KM, Ebeling PR (2015) Fall and fracture risk in sarcopenia and dynapenia with and without obesity: the role of lifestyle interventions. Curr Osteoporos Rep 13(4):235–244
Funding
National Key Research and Development Program of China, Grant/Award Number: 2018YFC2002100 and 2018YFC2002103.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Patient consent
Not required.
Conflict of interest
Ying Liu, Yi Song, Qinjian Hao, Jinhui Wu declare that they have no conflict of interest.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Liu, Y., Song, Y., Hao, Q. et al. Global prevalence of osteosarcopenic obesity amongst middle aged and older adults: a systematic review and meta-analysis. Arch Osteoporos 18, 60 (2023). https://doi.org/10.1007/s11657-023-01247-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11657-023-01247-5