Abstract
Summary
This systematic review analyzes the effects of bracing and taping after osteoporotic vertebral fractures. Spinal orthose may have positive effects on pain, but the evidence is of very low certainty. Clinical judgment is recommended when prescribing spinal orthoses.
Purpose
To examine the effects of bracing and taping interventions on pain, physical functioning, health-related quality of life, back extensor strength, kyphosis curvature, and adverse events in individuals with vertebral fragility fractures.
Methods
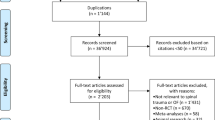
Four databases were searched from inception up to January 2022. We included randomized controlled trials testing the effect of bracing or taping interventions compared with a non-intervention control in adults ≥ 45 years with vertebral fragility fractures. Narrative syntheses were presented for all the outcomes. We assessed the risk of bias using the Cochrane Risk of Bias Assessment Tool and the certainty of evidence using the Grading of Recommendations Assessment, Development and Evaluation.
Results
Three studies were included. Soft bracing interventions exhibited inconsistent effects on pain. One study showed no difference between groups, and another study should a decrease in pain in the soft bracing group compared to the control group. Rigid bracing interventions did not have a significant change in pain between the control and intervention groups. One study demonstrated a decrease in pain at rest (VAS: − 10.8 ± 19.3) and during movement (VAS: − 20.9 ± 29.8) after a taping intervention. The other outcomes were not consistent across studies.
Conclusions
Spinal orthoses may improve pain in people with vertebral fractures; however, we cannot draw definitive conclusions on the efficacy or harms of bracing or taping due to the very low certainty evidence and the small number of studies. Effects on other outcomes are uncertain.



Similar content being viewed by others
Data Availability
Data sharing is not applicable to this article as no new data were created or analyzed in this study.
References
NIH. National Institutes of Health (NIH) (2001) Consensus development panel on osteoporosis prevention, diagnosis, and therapy. JAMA 285(6):785–795
What is osteoporosis? Osteoposis Canada. Published 2021. https://osteoporosis.ca/what-is-osteoporosis/. Accessed 14 Feb 2022
Burge R, Dawson-Hughes B, Solomon DH, Wong JB, King A, Tosteson A (2007) Incidence and economic burden of osteoporosis-related fractures in the United States, 2005–2025. J Bone Miner Res 22(3):465–475. https://doi.org/10.1359/jbmr.061113
Jansson KÅ, Blomqvist P, Svedmark P et al (2010) Thoracolumbar vertebral fractures in Sweden: an analysis of 13,496 patients admitted to hospital. Eur J Epidemiol 25(6):431–437. https://doi.org/10.1007/s10654-010-9461-5
Suzuki N, Ogikubo O, Hansson T (2008) The course of the acute vertebral body fragility fracture: its effect on pain, disability and quality of life during 12 months. Eur Spine J 17:1380–1390. https://doi.org/10.1007/s00586-008-0753-3
Ross PD (1997) Clinical consequences of vertebral fractures. Am J Med 103(2):S30–S43. https://doi.org/10.1016/S0002-9343(97)90025-5
Fink HA, Milavetz DL, Palermo L et al (2005) What proportion of incident radiographic vertebral deformities is clinically diagnosed and vice versa? J Bone Miner Res 20(7):1216–1222. https://doi.org/10.1359/JBMR.050314
Francis RM, Baillie SP, Chuck AJ et al (2004) Acute and long-term management of patients with vertebral fractures. QJM 97(2):63–74. https://doi.org/10.1093/qjmed/hch012
Gerdhem P (2013) Osteoporosis and fragility fractures: vertebral fractures. Best Pract Res Clin Rheumatol 27(6):743–755. https://doi.org/10.1016/j.berh.2014.01.002
Huang C, Ross PD, Wasnich RD (1996) Vertebral fracture and other predictors of physical impairment and health care utilization. Arch Intern Med 156(21):2469–2475. https://doi.org/10.1001/archinte.156.21.2469
Morin SN, Djekic-Ivankovic M, Funnell L et al (2020) Patient engagement in clinical guidelines development: input from > 1000 members of the Canadian Osteoporosis Patient Network. Osteoporos Int 31(5):867–874. https://doi.org/10.1007/s00198-019-05248-4
Jin YZ, Lee JH (2016) Effect of brace to osteoporotic vertebral fracture: a meta-analysis. J Korean Med Sci 31(10):1641–1649. https://doi.org/10.3346/jkms.2016.31.10.1641
Marchenkova LA, Makarova EV (2019) Exercise therapy and bracing in patients with osteoporotic compression vertebral fractures. Vopr Kurortol Fizioter Lech Fiz Kult 96(4):69–75. https://doi.org/10.17116/kurort20199604169
Murata K, Watanabe G, Kawaguchi S et al (2012) Union rates and prognostic variables of osteoporotic vertebral fractures treated with a rigid external support. J Neurosurg Spine 17(5):469–475. https://doi.org/10.3171/2012.7.SPINE122
Schmidt K, Hübscher M, Vogt L et al (2012) Einflüsse einer wirbelsäulenorthese auf gangparameter und alltagsfunktion bei postmenopausaler osteoporose. Orthopade 41(3):200–205. https://doi.org/10.1007/s00132-011-1867-6
Pfeifer M, Begerow B, Minne HW (2004) Effects of a new spinal orthosis on posture, trunk strength, and quality of life in women with postmenopausal osteoporosis: a randomized trial. Am J Phys Med Rehabil 83:177–186. https://doi.org/10.1097/01.PHM.0000113403.16617.93
Longo UG, Loppini M, Denaro L, Maffulli N, Denaro V (2012) Osteoporotic vertebral fractures: current concepts of conservative care. Br Med Bull 102(1):171–189. https://doi.org/10.1093/bmb/ldr048
Greig A, Bennell K, Briggs A, Hodges P (2008) Postural taping decreases thoracic kyphosis but does not influence trunk muscle electromyographic activity or balance in women with osteoporosis. Man Ther 13(3):249–257. https://doi.org/10.1016/j.math.2007.01.011
Palmer S, Barnett S, Cramp M, Berry A, Thomas A, Clark EM (2018) Effects of postural taping on pain, function and quality of life following osteoporotic vertebral fractures—a feasibility trial. Musculoskeletal Care 16:345–352. https://doi.org/10.1002/msc.1350
Ebeling PR, Akesson K, Bauer DC et al (2019) The efficacy and safety of vertebral augmentation: a second ASBMR task force report. J Bone Miner Res 34(1):3–21. https://doi.org/10.1002/jbmr.3653
Goodwin VA, Hall AJ, Rogers E, Bethel A (2016) Orthotics and taping in the management of vertebral fractures in people with osteoporosis: a systematic review. BMJ Open 6(5):e010657. https://doi.org/10.1136/bmjopen-2015-010657
Hofler RC, Jones GA (2020) Bracing for acute and subacute osteoporotic compression fractures: a systematic review of the literature. World Neurosurg 141:e453–e460. https://doi.org/10.1016/j.wneu.2020.05.199
Newman M, Minns Lowe C, Barker K (2016) Spinal orthoses for vertebral osteoporosis and osteoporotic vertebral fracture: a systematic review. Arch Phys Med Rehabil 97(6):1013–1025. https://doi.org/10.1016/j.apmr.2015.10.108
Ponzano M, Tibert N, Brien S, Funnell, L, Gibbs, JC, Keller, H, Laprade, J, Morin, SN, Papaioannou, A, Weston, Z, Wideman, TH, Giangregorio, LM. International consensus on the non-pharmacological management of osteoporotic vertebral fractures. Osteoporos Int., under review. Accessed 14 Feb 2022
Page MJ, Moher D, Bossuyt PM et al (2021) PRISMA 2020 explanation and elaboration: updated guidance and exemplars for reporting systematic reviews. BMJ 372:n160. https://doi.org/10.1136/bmj.n160
Kanis JA, Oden A, Johnell O, Jonsson B, De Laet C, Dawson A (2001) The burden of osteoporotic fractures: a method for setting intervention thresholds. Osteoporos Int 12(5):417–427. https://doi.org/10.1007/s001980170112
Health Canada. Overview of the reporting adverse reactions to marketed health products – guidance document for industry. Govenment of Canada. Published 2019. https://www.canada.ca/en/health-canada/services/drugs-health-products/reports-publications/medeffect-canada/reporting-adverse-reactions-marketed-health-products-guidance-industry.html. Accessed 14 Feb 2022
O’Neill J, Tabish H, Welch V et al (2014) Applying an equity lens to interventions: using PROGRESS ensures consideration of socially stratifying factors to illuminate inequities in health. J Clin Epidemiol 67(1):56–64. https://doi.org/10.1016/j.jclinepi.2013.08.005
Rodrigues IB, Ponzano M, Hosseini Z et al (2021) The effect of impact exercise (alone or multicomponent intervention) on health-related outcomes in individuals at risk of fractures: a systematic review and meta-analysis of randomized controlled trials. Sport Med 51(6):1273–1292. https://doi.org/10.1007/s40279-021-01432-x
Higgins JPT, Savović J, Page MJ, Elbers RG. Assessing risk of bias in a randomized trial. In: Higgins JPT, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, Welch VA (editors). Cochrane Handbook for Systematic Reviews of Interventions version 6.2. Published 2021. https://training.cochrane.org/handbook/. Accessed 1 March 2022
Schünemann HJ, Higgins JPT, Vist GE, et al. Chapter 14: Completing “Summary of Findings” tables and grading the certainty of evidence. In: Higgins JPT, Thomas J, Chandler J, et al. (editors). Cochrane Handbook for Systematic Reviews of Interventions version 6.1. Published 2020. https://training.cochrane.org/handbook/. Accessed 1 March 2022
Pfeifer M, Kohlwey L, Begerow B, Minne HW (2011) Effects of two newly developed spinal orthoses on trunk muscle strength, posture, and quality-of-life in women with postmenopausal osteoporosis: a randomized trial. Am J Phys Med Rehabil 90(10):805–815. https://doi.org/10.1097/PHM.0b013e31821f6df3
Giangregorio LM, Ponzano M. Letter to the editor on “Effects of two newly developed spinal orthoses on trunk muscle strength, posture, and quality-of-life in women with postmenopausal osteoporosis: a randomized trial.” Am J Phys Med Rehabil. Published online 2022.
Kim HJ, Yi JM, Cho HG et al (2014) Comparative study of the treatment outcomes of osteoporotic compression fractures without neurologic injury using a rigid brace, a soft brace, and no brace: a prospective randomized controlled non-inferiority trial. J Bone Jt Surg - Am 96(23):1959–1966. https://doi.org/10.2106/JBJS.N.00187
Begerow B, Pfeifer M, Pospeschill M et al (1999) Time since vertebral fracture: an important variable concerning quality of life in patients with postmenopausal osteoporosis. Osteoporos Int 10(1):26–33. https://doi.org/10.1007/s001980050190
Alcalá-Cerra G, Paternina-Caicedo ÁJ, Díaz-Becerra C, Moscote-Salazar LR, Fernandes-Joaquim A (2014) Orthosis for thoracolumbar burst fractures without neurologic deficit: a systematic review of prospective randomized controlled trials. J Craniovertebr Junction Spine 5(1):25–32. https://doi.org/10.4103/0974-8237.135213
Li M, Law SW, Cheng J, Kee HM, Wong MS (2015) A comparison study on the efficacy of SpinoMed and soft lumbar orthosis for osteoporotic vertebral fracture. Prosthet Orthot Int 39(4):270–276. https://doi.org/10.1177/0309364614528204
Bennell KL, Matthews B, Greig A et al (2010) Effects of an exercise and manual therapy program on physical impairments, function and quality-of-life in people with osteoporotic vertebral fracture: a randomised, single-blind controlled pilot trial. BMC Musculoskelet Disord 11:36. https://doi.org/10.1186/1471-2474-11-36
Dionyssiotis Y, Trovas G, Thoma S, Lyritis G, Papaioannou N (2015) Prospective study of spinal orthoses in women. Prosthet Orthot Int 39(6):487–495. https://doi.org/10.1177/0309364614545416
Eisinger DB, Kumar R, Woodrow R (1996) Effect of lumbar orthotics on trunk muscle strength. Am J Phys Med Rehabil 75(3):194–197. https://doi.org/10.1097/00002060-199605000-00008
Sinaki M, Wollan PC, Scott RW, Gelczer RK (1996) Can strong back extensors prevent vertebral fractures in women with osteoporosis? Mayo Clin Proc 71(10):951–956. https://doi.org/10.4065/71.10.951
Ponzano M, Tibert N, Bansal S, Katzman W, Giangregorio L (2021) Exercise for improving age-related hyperkyphosis: a systematic review and meta-analysis with GRADE assessment. Arch Osteoporos Published online. https://doi.org/10.1007/s11657-021-00998-3
Liaw M, Chen C, Chen J, Tang F, Wong A, Ho H (2009) Effects of Knight-Taylor brace on balance performance in osteoporotic patients with vertebral compression fracture. J Back Musculoskelet Rehabil 22(2):75–81. https://doi.org/10.3233/BMR-2009-0218
Ruckstuhl J (1972) Early results in the treatment of vertebral body fractures using a so-called 3-point corset. Monatsschr Unfallheilkd Versicher Versorg Verkehrsmed 75(12):560–567. https://www.scopus.com/inward/record.uri?eid=2-s2.0-0015440411&partnerID=40&md5=ade27bb8bcdb252b0c1c6408b0bb330a. Accessed 18 Nov 2020
von Gumppenberg S, Claudi B (1989) Conservative fracture treatment of the cervical spine with halo fixation. Aktuelle Traumatol 19(2):57–60
von Gumppenberg S, Vieweg J, Claudi B, Harms J (1991) Primary management of fresh injuries of the thoracic and lumbar vertebrae. Aktuelle Traumatol 21(6):265–273
Nagel-Albustin K, Preisinger E (2012) Proprioceptive orthoses and osteoporosis. J fur Miner 19(3):120–123. https://www.scopus.com/inward/record.uri?eid=2-s2.0-84866748082&partnerID=40&md5=eb4b5ed8d70a8230badf7ad4684365c1. Accessed 18 Nov 2020
Wendt O, Petracic B, Lang HD, Vogel K (1975) Treatment of thoracic and lumbar vertebral fractures using the 3-point support-brace. Hefte Unfallheilkd (126):342–344. https://www.scopus.com/inward/record.uri?eid=2-s2.0-14844334462&partnerID=40&md5=547471b3e25ace8eec0dd974a1352e7e. Accessed 18 Nov 2020
Shamji MF, Roffey DM, Young DK, Reindl R, Wai EK (2014) A pilot evaluation of the role of bracing in stable thoracolumbar burst fractures without neurological deficit. J Spinal Disord Tech 27(7):370–375. https://doi.org/10.1097/BSD.0b013e31826eacae
Bailey CS, Urquhart JC, Dvorak MF et al (2014) Orthosis versus no orthosis for the treatment of thoracolumbar burst fractures without neurologic injury: a multicenter prospective randomized equivalence trial. Spine J 14(11):2557–2564. https://doi.org/10.1016/j.spinee.2013.10.017
Urquhart JC, Alrehaili OA, Fisher CG et al (2017) Treatment of thoracolumbar burst fractures: extended follow-up of a randomized clinical trial comparing orthosis versus no orthosis. J Neurosurg Spine 27(1):42–47. https://doi.org/10.3171/2016.11.SPINE161031
Kato T, Inose H, Ichimura S et al (2019) Comparison of rigid and soft-brace treatments for acute osteoporotic vertebral compression fracture: a prospective, randomized, multicenter study. J Clin Med Published online. https://doi.org/10.3390/jcm8020198
Kaplan RS, Sinaki M, Hameister MD (1996) Effect of back supports on back strength in patients with osteoporosis: a pilot study. Mayo Clin Proc 71(3):235–241. https://doi.org/10.4065/71.3.235
Raeissadat S, Sedighipour L, Pournajaf S, VahabKashani R, Sadeghi S (2014) Effect of posture training with Weighted Kypho-Orthosis (WKO) on Improving balance in women with osteoporosis. J Aging Res 2014:427903. https://doi.org/10.1155/2014/427903
Sinaki M, Lynn SG (2002) Reducing the risk of falls through proprioceptive dynamic posture training in osteoporotic women with kyphotic posturing: a randomized pilot study. Am J Phys Med Rehabil 81(4):241–246. https://doi.org/10.1097/00002060-200204000-00001
Funding
We acknowledge the support of the Natural Sciences and Engineering Research Council of Canada (NSERC), CREATE 509950–2018 Training in Global Biomedical Technology Research and Innovation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
Not required.
Conflicts of interest
None.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Peckett, K.H., Ponzano, M., Steinke, A. et al. Bracing and taping interventions for individuals with vertebral fragility fractures: a systematic review of randomized controlled trials with GRADE assessment. Arch Osteoporos 18, 36 (2023). https://doi.org/10.1007/s11657-023-01224-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11657-023-01224-y