Abstract
Summary
Quantitative ultrasound (QUS) has been found to be a safe and reliable method for evaluating bone mineral density (BMD). Using calcaneal QUS techniques, the current study contributes to remedying this gap in the literature by establishing normative data among children and adolescents from Colombia.
Introduction
Minimal data on BMD changes are available from populations in developing countries. BMD reference values for children and adolescents have not been published for a Latin-American population. The aim of this study was to establish a normal reference range of calcaneal broadband ultrasound attenuation (BUA) in Colombian children and adolescents with ages ranging from 9 to 17.9 years.
Methods
A sample of 1001 healthy Colombian youth (boys n = 445 and girls n = 556), children, and adolescents (9–17.9 years old) participated in the study. A calcaneus QUS parameter (BUA) was obtained for boys and girls, stratified by age group. Furthermore, height, weight, fat mass percentage, and body mass index were measured. Centile smoothed curves for the third, tenth, 25th, 50th, 75th, 90th, and 97th percentiles were calculated using the LMS method (L [curve Box–Cox], M [curve median], and S [curve coefficient of variation]).
Results
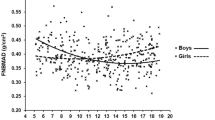
Mean (± SD) values for the participants’ anthropometric data were 12.9 ± 2.3 years of age, 45.2 ± 11.5 kg weight, 1.51 ± 0.1 m height, 19.5 ± 3.1 kg/m2 BMI, and 69.5 ± 17.1 dB/MHz BUA. Overall, all variables were significantly higher in boys except in BMI and body fat percentage. Girls generally had higher mean calcaneal BUA (dB/MHz) values than the boys, except in the age ranges 16 and 17.9, p > 0.05. In addition, the BUA (dB/MHz) increased with age throughout childhood and adolescence and reached a plateau by age 15–17.9 for girls.
Conclusions
For the first time, our results provide sex- and age-specific BUA reference values for Colombian children and adolescents aged 9–17.9 years. A more specific set of reference values is useful for clinicians and researchers and informs clinical practice to monitor bone mineral status.


Similar content being viewed by others
References
Baroncelli GI (2008) Quantitative ultrasound methods to assess bone mineral status in children: technical characteristics, performance, and clinical application. Pediatr Res 63(3):220–228
Henwood MJ, Binkovitz L (2009) Update on pediatric bone health. J Am Osteopath Assoc 109(1):5–12
Boyce AM, Gafni RI (2011) Approach to the child with fractures. J Clin Endocrinol Metab 96:1943–1952
Bonnick SL (2009) Bone densitometry in clinical practice: application and interpretation. Humana Press, Totowa
Njeh CF, Fuerst T, Hans D, Blake GM, Genant HK (1999) Radiation exposure in bone mineral density assessment. Appl Radiat Isot 50:215–236
Gluer CC (1997) Quantitative ultrasound techniques for the assessment of osteoporosis: expert agreement on current status. J Bone Miner Res 12:1280–1288
Genant HK, Engelke K, Fuerst T, Gluer C-C, Grampp S, Harris ST et al (1996) Noninvasive assessment of bone mineral and structure: state of the art. J Bone Miner Res 11:707–730
Goh SY, Aragon JM, Lee YS, Loke KY (2011) Normative data for quantitative calcaneal ultrasound in Asian children. Ann Acad Med Singap 40(2):74–79
Khaw KT, Reeve J, Luben R, Bingham S, Welch A, Wareham N et al (2004) Prediction of total and hip fracture risk in men and women by quantitative ultrasound of the calcaneus: Epic-Norfolk prospective population study. Lancet 363:197–202
Bauer DC, Glucer CC, Cauley JA, Vogt TM, Ensrud KE, Genant HK et al (1997) Broadband ultrasound attenuation predicts fractures strongly and independently of densitometry in older women: a prospective study. Study of Osteoporotic Fractures Research Group. Arch Intern Med 157:629–634
Mughal MZ, Langton CM, Utretch G, Morrison J, Specker BL (1996) Comparison between broad-band ultrasound attenuation of the calcaneum and total body bone mineral density in children. Acta Paediatr 85:663–665
Saraff V, Hoegler W (2015) Endocrinology and adolescence: osteoporosis in children: diagnosis and management. Eur J Endocrinol 173(6):R185–197
Bishop N, Arundel P, Clark E, Dimitri P, Farr J, Jones G, Makitie O, Munns CF, Shaw N (2014) Fracture prediction and the definition of osteoporosis in children and adolescents: the ISCD 2013 Pediatric Official Positions. J Clin Densitom 17:275–280
Foley S, Quinn S, Jones G (2009) Tracking of bone mass from childhood to adolescence and factors that predict deviation from tracking. Bone 44:752–757
Herrmann D, Intemann T, Lauria F, Mårild S, Molnár D, Moreno LA, Sioen I, Tornaritis M, Veidebaum T, Pigeot I, Ahrens W, IDEFICS consortium (2014) Reference values of bone stiffness index and C-terminal telopeptide in healthy European children. Int J Obes (Lond) 38(Suppl 2):S76–S85
Marcelli C (2007) Osteoporosis in children and adolescents. Presse Med 36(7–8):1078–1083
van den Bergh JP, Noordam C, Ozyilmaz A, Hermus AR, Smals AG (2000) Otten BJ Calcaneal ultrasound imaging in healthy children and adolescents: relation of the ultrasound parameters BUA and SOS to age, body weight, height, foot dimensions and pubertal stage. Osteoporos Int 11:967–976
Sawyer A, Moore S, Fielding KT, Nix DA, Kiratli J, Bachrach LK (2001) Calcaneus ultrasound measurements in a convenience sample of healthy youth. J Clin Densitom 4:111–120
Mughal MZ, Ward K, Qayyum N, Langton CM (1997) Assessment of bone status using the contact ultrasound bone analyser. Arch Dis Child 76:535–536
Wunsche K, Wunsche B, Fahnrich H, Mentzel HJ, Vogt S, Abendroth K, Kaiser WA (2000) Ultrasound bone densitometry of the os calcis in children and adolescents. Calcif Tissue Int 67:349–355
Zhu ZQ, Liu W, Xu CL, Han SM, Zu SY, Zhu GJ (2007) Ultrasound bone densitometry of the calcaneus in healthy Chinese children and adolescents. Osteoporos Int 18:533–541
Rauchenzauner M, Schmid A, Heinz-Erian P, Kapelari K, Falkensammer G, Griesmacher A et al (2007) Sex- and age-specific reference curves for serum markers of bone turnover in healthy children from 2 months to 18 years. J Clin Endocrinol Metab 92:443–449
Lin YC, Tu SH, Pan WH (2007) Bone mass status of school-aged children in Taiwan assessed by quantitative ultrasound: the Nutrition and Health Survey in Taiwan Elementary School Children (NAHSIT Children 2001–2002). Asia Pac J Clin Nutr 16:585–593
Tuzun S, Karacan I, Akarirmak U, Kasapcopur O, Arisoy N (2003) Evaluation of bone with quantitative ultrasound in healthy Turkish children. Turk J Pediatr 45:240–244
Zhu ZQ, Liu W, Xu CL, Han SM, Zu SY, Zhu GJ (2007) Ultrasound bone densitometry of the calcaneus in healthy Chinese children andadolescents. Osteoporos Int 18(4):533–541
Lavado-Garcia JM, Calderon-Garcia JF, Moran JM, Canal-Macias ML, Rodriguez-Dominguez T, Pedrera-Zamorano JD (2012) Bone mass of Spanish school children: impact of anthropometric, dietary and body composition factors. J Bone Miner Metab 30(2):193–201
Ramírez-Vélez R, Rodrigues-Bezerra D, Correa-Bautista JE, Izquierdo M, Lobelo F (2015) Reliability of health-related physical fitness tests among Colombian children and adolescents: the FUPRECOL study. PLoS One 10(10):e0140875
Marfell-Jones M, Olds T, Stewart A (2006) International standards for anthropometric assessment Potchefstroom. ISAK, South Africa
Jaworski M, Lebiedowski M, Lorenc RS, Trempe J (1995) Ultrasound bone measurement in pediatric subjects. Calcif Tissue Int 56(5):368–371
Vignolo M, Brignone A, Mascagni A, Ravera G, Biasotti B, Aicardi G (2003) Influence of age, sex, and growth variables on phalangeal quantitative ultrasound measures: a study in healthy children and adolescents. Calcif Tissue Int 72:681–688
Cole TJ, Green PJ (1992) Smoothing reference centile curves: the LMS method and penalized likelihood. Stat Med 11:1305–1319
Royston P, Wright EM (2000) Goodness-of-fit statistics for age-specific reference intervals. Stat Med 19:2943–2962
Bachrach LK (2001) Acquisition of optimal bone mass in childhood and adolescence. Trends Endocrinol Metab 12(1):22–28
Rivas-Ruiz R, Méndez-Sánchez L, Castelán-Martínez OD, Clark P, Tamayo J, Talavera JO et al (2015) Comparison of international reference values for bone speed of sound in pediatric populations: meta-analysis. J Clin Densitom. doi:10.1016/j.jocd.2015.04.005
Bonjour JP, Theintz G, Buchs B, Slosman D, Rizzoli R (1991) Critical years and stages of puberty for spinal and femoral bone mass accumulation during adolescence. J Clin Endocrinol Metab 73:555–563
Matkovic V, Jelic T, Wardlaw GM, Ilich JZ, Goel PK, Wright JK, Andon MB, Smith KT, Heaney RP (1994) Timing of peak bone mass in Caucasian females and its implication for the prevention of osteoporosis. J Clin Invest 93:799–808
Lloyd T, Petit MA, Lin HM, Beck TJ (2004) Lifestyle factors and the development of bone mass and bone strength in young women. J Pediatr 144(6):776–782
Chiu GR, Araujo AB, Travison TG, Hall SA, McKinlay JB (2009) Relative contributions of multiple determinants to bonemineral density in men. Osteoporos Int 20(12):2035–2047
Lim LS, Hoeksema LJ, Sherin K, ACPM Prevention Practice Committee (2009) Screening for osteoporosis in the adult U.S. population: ACPM position statement on preventive practice. Am J Prev Med 36(4):366–375
Parra DC, Iannotti L, Gomez LF, Pachón H, Haire-Joshu D, Sarmiento OL, Kuhlmann AS, Brownson RC (2015) The nutrition transition in Colombia over a decade: novel household classification system of anthropometricmeasures. Arch Public Health 73(1):12
Sarmiento OL, Parra DC, González SA, González-Casanova I, Forero AY, Garcia J (2014) The dual burden of malnutrition in Colombia. Am J Clin Nutr 100(6):1628S–1635S
Martínez-Torres J, Meneses-Echavéz JF, Ramírez-Vélez R (2014) Prevalence and demographic factors associated with vitamin A deficiency in Colombian children aged 12–59 months. Endocrinol Nutr 61(9):460–466
Martínez-Torres J, Ramírez-Vélez R (2014) Zinc deficiency and associated factors in colombian children; results from the 2010 national nutrition survey; a cross sectional study. Nutr Hosp 29(4):832–837
Ramírez-Vélez R, Matínez-Torres J, Meneses-Echavez JF (2014) Prevalence and demographic factors associated with ferritin deficiency in Colombian children, 2010. Rev Peru Med Exp Salud Publica 31(2):237–242
Villamor E, Mora-Plazas M, Forero Y, Lopez-Arana S, Baylin A (2008) Vitamin B-12 status is associated with socioeconomic level and adherence, to an animal food dietary pattern in Colombian school children. J Nutr 138:1391–1398
Sani FM, Sarji SA, Bilgen M (2011) Quantitative ultrasound measurement of the calcaneus in Southeast Asian children with thalassemia: comparison with dual-energy X-ray absorptiometry. J Ultrasound Med 30(7):883–894
Eliakim A, Nemet D, Wolach B (2001) Quantitative ultrasound measurements of bone strength in obese children and adolescents. J Pediatr Endocrinol Metab 14:159–164
Correa-Rodríguez M, Rueda-Medina B, González-Jiménez E, Navarro-Pérez CF, Schmidt-RioValle J (2014) The levels of bone mineralization are influenced by body composition in children and adolescents. Nutr Hosp 30(4):763–768
Liu W, Xu CL, Zhu ZQ, Wang W, Han SM, Zu SY, Zhu GJ (2006) Characteristics of calcaneus quantitative ultrasound normative data in Chinese mainland men and women. Osteoporos Int 17:1216–1224
Pollock NK, Bernard PJ, Gutin B, Davis CL, Zhu H, Dong YMD (2011) Adolescent obesity, bone mass, and cardiometabolic risk factors. J Pediatr 158:727–734
Acknowledgments
The FUPRECOL Study received funding from the Instituto Colombiano para el Desarrollo de la Ciencia y la Tecnología “Francisco José de Caldas” COLCIENCIAS [Contract N° 671-2014 Code 122265743978]. The authors are grateful to the Bogota District Education Secretary for the data used in this research. The authors would also like thank the Bogota District students, teachers, schools, and staff, who participated in this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None.
Rights and permissions
About this article
Cite this article
Ramírez-Vélez, R., Ojeda-Pardo, M.L., Correa-Bautista, J.E. et al. Normative data for calcaneal broadband ultrasound attenuation among children and adolescents from Colombia: the FUPRECOL Study. Arch Osteoporos 11, 2 (2016). https://doi.org/10.1007/s11657-015-0253-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11657-015-0253-0