Abstract
Background
The purpose of this study was to review our experience with laparoscopic colectomy and fistula resection, evaluate the frequency of conversion to open, and to compare the perioperative courses of the complete laparoscopic and conversion groups.
Methods
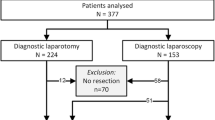
This study is a retrospective analysis of 111 consecutive adult patients with diverticular fistulae diagnosed clinically or radiographically over 11 years at a single institution. Five patients were excluded for preoperative comorbidities. The remaining 106 consecutive patients underwent minimally invasive sigmoid colectomy with primary anastomosis. Preoperative, intraoperative, and postoperative variables were collected from the colorectal surgery service database. A retrospective cohort analysis was performed between laparoscopic and converted groups.
Results
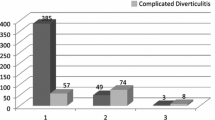
Within the group, 47% had colovesical fistulas, followed by colovaginal, coloenteric, colocutaneous, and colocolonic fistulas. The overall conversion rate to laparotomy was 34.7% (n = 37). The most common reason for conversion was dense fibrosis. Mean operative time was similar between groups. Combined postoperative complications occurred in 26.4% of patients (21.4% laparoscopic and 37.8% converted, p = 0.075). Length of stay was significantly shorter in the laparoscopic group (5.8 vs 8.1 days, p = 0.014). There were two anastomotic leaks, both in the open group. There were no 30-day mortalities.
Conclusions
Laparoscopic sigmoid colectomy for diverticular fistula is safe, with complication rates comparable to open sigmoid resection. We identify a conversion rate which allows the majority of patients to benefit from minimally invasive procedures.


Similar content being viewed by others
References
Stollman NH, Raskin JB (1999) Diagnosis and management of diverticular disease of the colon in adults. Ad Hoc Practice Parameters Committee of the American College of Gastroenterology. Am J Gastroenterol 94:3110–3121
Woods RJ, Lavery IC, Fazio VW, Jagelman DG, Weakley FL (1988) Internal fistulas in diverticular disease. Dis Colon Rectum 31:591–596
Feingold D, Steele SR, Lee S, Kaiser A, Boushey R, Buie WD, Rafferty JF (2014) Practice parameters for the treatment of sigmoid diverticulitis. Dis Colon Rectum 57:284–294
Badic B, Leroux G, Thereaux J, Joumond A, Gancel CH, Bail JP, Meurette G (2017) Colovesical Fistula Complicating Diverticular Disease: A 14-Year Experience. Surg Laparosc Endosc Percutan Tech 27:94–97
Bhakta A, Tafen M, Glotzer O, Canete J, Chismark AD, Valerian BT, Stain SC, Lee EC (2016) Laparoscopic sigmoid colectomy for complicated diverticulitis is safe: review of 576 consecutive colectomies. Surg Endosc 30:1629–1634
Laurent SR, Detroz B, Detry O, Degauque C, Honore P, Meurisse M (2005) Laparoscopic sigmoidectomy for fistulized diverticulitis. Dis Colon Rectum 48:148–152
Cirocchi R, Arezzo A, Renzi C, Cochetti G, D'Andrea V, Fingerhut A, Mearini E, Binda GA (2015) Is laparoscopic surgery the best treatment in fistulas complicating diverticular disease of the sigmoid colon? A systematic review Int J Surg 24:95–100
Cirocchi R, Cochetti G, Randolph J, Listorti C, Castellani E, Renzi C, Mearini E, Fingerhut A (2014) Laparoscopic treatment of colovesical fistulas due to complicated colonic diverticular disease: a systematic review. Tech Coloproctol 18:873–885
Engledow AH, Pakzad F, Ward NJ, Arulampalam T, Motson RW (2007) Laparoscopic resection of diverticular fistulae: a 10-year experience. Colorectal Dis 9:632–634
Maciel V, Lujan HJ, Plasencia G, Zeichen M, Mata W, Jorge I, Lee D, Viamonte M, 3rd, Hartmann RF (2014) Diverticular disease complicated with colovesical fistula: laparoscopic versus robotic management. Int Surg 99:203–210
Hinchey EJ, Schaal PG, Richards GK (1978) Treatment of perforated diverticular disease of the colon. Adv Surg 12:85–109
Klarenbeek BR, Veenhof AA, Bergamaschi R, van der Peet DL, van den Broek WT, de Lange ES, Bemelman WA, Heres P, Lacy AM, Engel AF, Cuesta MA (2009) Laparoscopic sigmoid resection for diverticulitis decreases major morbidity rates: a randomized control trial: short-term results of the Sigma Trial. Ann Surg 249:39–44
Lawrence DM, Pasquale MD, Wasser TE (2003) Laparoscopic versus open sigmoid colectomy for diverticulitis. Am Surg 69:499–503; discussion 503-494
Haas JM, Singh M, Vakil N (2016) Mortality and complications following surgery for diverticulitis: Systematic review and meta-analysis. United European Gastroenterol J 4:706–713
Papageorge CM, Kennedy GD, Carchman EH (2016) National Trends in Short-term Outcomes Following Non-emergent Surgery for Diverticular Disease. J Gastrointest Surg 20:1376–1387
Giovanni C, Emanuele C, Francesco B, Emanuele L, Andrea B, Solajd P, Ettore M (2013) Laparoscopic conservative treatment of colovesical fistula: a new surgical approach. Int Braz J Urol 39:752; discussion 753
Cirocchi R, Farinella E, Trastulli S, Sciannameo F, Audisio RA (2012) Elective sigmoid colectomy for diverticular disease. Laparoscopic vs open surgery: a systematic review. Colorectal Dis 14:671–683
Marcucci T, Giannessi S, Giudici F, Riccadonna S, Gori A, Tonelli F (2017) Management of colovesical and colovaginal diverticular fistulas Our experience and literature reviewed. Ann ITal Chir 88:55–61
He Y, Wang J, Bian H, Deng X, Wang Z (2017) BMI as a Predictor for Perioperative Outcome of Laparoscopic Colorectal Surgery: a Pooled Analysis of Comparative Studies. Dis Colon Rectum 60:433–445
Hotouras A, Ribas Y, Zakeri SA, Nunes QM, Murphy J, Bhan C, Wexner SD (2016) The influence of obesity and body mass index on the outcome of laparoscopic colorectal surgery: a systematic literature review. Colorectal dis 18:O337-o366
Rosa M. Jiménez Rodríguez, José M. Díaz Pavón, Fernando de La Portilla de Juan, Emilio Prendes Sillero, Jean Marie Hisnard Cadet Dussort, Javier Padillo, (2011) Estudio prospectivo, aleatorizado: cirugà a laparoscópica con asistencia robótica versus cirugà a laparoscópica convencional en la resección del cáncer colorrectal. Cirugà a Española 89 (7):432-438
Baik SH, Ko YT, Kang CM, Lee WJ, Kim NK, Sohn SK, Chi HS, Cho CH (2008) Robotic tumor-specific mesorectal excision of rectal cancer: short-term outcome of a pilot randomized trial. Surg Endosc 22:1601–1608
Author information
Authors and Affiliations
Contributions
Martinolich J contributed substantially to the conception, acquisition, analysis, drafting the work, and final approval and is accountable for the accuracy and integrity of the work.
Croasdale DR contributed substantially to the conception, acquisition, analysis, drafting the work, and final approval and is accountable for the accuracy and integrity of the work.
Bhakta A contributed substantially to the conception, acquisition, analysis, drafting the work, and final approval and is accountable for the accuracy and integrity of the work.
Ata A contributed substantially to the conception, acquisition, analysis and interpretation, drafting the work, and final approval and is accountable for the accuracy and integrity of the work.
Chismark AD contributed substantially to the conception, acquisition, analysis, drafting the work, and final approval and is accountable for the accuracy and integrity of the work.
Valerian BT contributed substantially to the conception, acquisition, analysis, drafting the work, and final approval and is accountable for the accuracy and integrity of the work.
Canete JJ contributed substantially to the conception, acquisition, analysis, drafting the work, and final approval and is accountable for the accuracy and integrity of the work.
Lee EC contributed substantially to the conception, acquisition, analysis, drafting the work, and final approval and is accountable for the accuracy and integrity of the work.
Corresponding author
Ethics declarations
Competing Interests
The authors declare that they have no conflicts of interest.
Additional information
Presented as Poster Presentation; ASCRS Annual Scientific and Tripartite Meeting June 2017 Seattle, Washington
Rights and permissions
About this article
Cite this article
Martinolich, J., Croasdale, D.R., Bhakta, A.S. et al. Laparoscopic Surgery for Diverticular Fistulas: Outcomes of 111 Consecutive Cases at a Single Institution. J Gastrointest Surg 23, 1015–1021 (2019). https://doi.org/10.1007/s11605-018-3950-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-018-3950-3