Abstract
Background
The incidence and several risk factors of biliary complication (BC) following pediatric liver transplantation (LT) are widely known, but data on long-term outcomes and management is limited. This retrospective study aimed to investigate the incidence, associated risk factors, management, and outcomes of early and late BC in pediatric LT.
Methods
This study enrolled 134 pediatric patients (< 18 years old) who underwent LT at a tertiary care center in Taiwan between January 2001 and December 2015. Diagnosis of BC was based on clinical, biochemical, and radiologic examinations. Clinical data and chart records were reviewed and compared between the groups.
Results
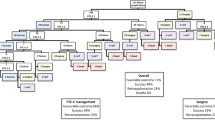
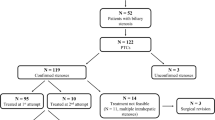
Among the 134 children, 21 children (15.7%) had BC after LT. Nine children had early complications, including leakage plus stricture (n = 2), stricture only (n = 2), and leakage only (n = 5). Twelve children had late BC; all of whom had anastomotic stricture. Of the 21 patients with BC, 11 patients (52.4%) were treated without surgery. The median time of first treatment for BC was 6.5 months (range, 11 days to 6.2 years). Five of the 9 patients with early complications and two of the 12 patients with late complications died of biliary tract infection. The major risk factors of BC in pediatric LT were (1) recipient age > 2 years, (2) Kasai portoenterostomy revision, and (3) hepatic artery thrombosis.
Conclusions
Several risk factors of BC in pediatric LT were identified. Children with early BC appeared to have relatively unfavorable outcomes. However, late BC treated by either radiological or surgical methods appeared to have a relatively good long-term prognosis.


Similar content being viewed by others
References
Muiesan P, Vergani D, Mieli-Vergani G. Liver transplantation in children. J Hepatol. 2007;46(2):340–8.
Colledan M, D'Antiga L. Biliary complications after pediatric liver transplantation: the endless heel. Pediatr Transplant. 2014;18(8):786–7.
Laurence JM, Sapisochin G, DeAngelis M, Seal JB, Miserachs MM, Marquez M, et al. Biliary complications in pediatric liver transplantation: Incidence and management over a decade. Liver Transpl. 2015;21(8):1082–90.
Chok KS, Chan SC, Chan KL, Sharr WW, Tam PK, Fan ST, et al. Bile duct anastomotic stricture after pediatric living donor liver transplantation. J Pediatr Surg. 2012;47(7):1399–403.
Tanaka K, Yol S. Incidence and management of biliary strictures in living-related donor graft. Pediatr Transplant. 2002;6(6):452–5.
Tanaka H, Fukuda A, Shigeta T, Kuroda T, Kimura T, Sakamoto S, et al. Biliary reconstruction in pediatric live donor liver transplantation: duct-to-duct or Roux-en-Y hepaticojejunostomy. J Pediatr Surg. 2010;45(8):1668–75.
Luthold SC, Kaseje N, Jannot AS, Mentha G, Majno P, Toso C, et al. Risk factors for early and late biliary complications in pediatric liver transplantation. Pediatr Transplant. 2014;18(8):822–30.
Darius T, Rivera J, Fusaro F, Lai Q, de Magnee C, Bourdeaux C, et al. Risk factors and surgical management of anastomotic biliary complications after pediatric liver transplantation. Liver Transpl. 2014;20(8):893–903.
Imamine R, Shibata T, Yabuta M, Shinozuka K, Kataoka M, Isoda H, et al. Long-Term Outcome of Percutaneous Biliary Interventions for Biliary Anastomotic Stricture in Pediatric Patients after Living Donor Liver Transplantation with Roux-en-Y Hepaticojejunostomy. J Vasc Interv Radiol. 2015;26(12):1852–9.
Holguin AJ, Rodriguez-Takeuchi S, Ospina L, Acosta D, Botero V, Thomas L, et al. Biliary strictures complicating liver transplantation in pediatric patients: Experience in a South American transplant center. Clin Transplant. 2017;31(2).
Lu CH, Tsang LL, Huang TL, Chen TY, Ou HY, Yu CY, et al. Biliary complications and management in pediatric living donor liver transplantation for underlying biliary atresia. Transplant Proc. 2012;44(2):476–7.
Uller W, Wohlgemuth WA, Hammer S, Knoppke B, Goessmann H, Loss M, et al. Percutaneous treatment of biliary complications in pediatric patients after liver transplantation. Rofo. 2014;186(12):1127–33.
Kitajima T, Sakamoto S, Sasaki K, Uchida H, Narumoto S, Fukuda A, et al. Living donor liver transplantation for post-Kasai biliary atresia: Analysis of pretransplant predictors of outcomes in infants. Liver Transpl. 2017.
Sundaram SS, Mack CL, Feldman AG, Sokol RJ. Biliary atresia: Indications and timing of liver transplantation and optimization of pretransplant care. Liver Transpl. 2017;23(1):96–109.
Sandler AD, Azarow KS, Superina RA. The impact of a previous Kasai procedure on liver transplantation for biliary atresia. J Pediatr Surg. 1997;32(3):416–9.
Urahashi T, Ihara Y, Sanada Y, Wakiya T, Yamada N, Okada N, et al. Effect of repeat Kasai hepatic portoenterostomy on pediatric live-donor liver graft for biliary atresia. Exp Clin Transplant. 2013;11(3):259–63.
Chung PH, Wong KK, Chan SC, Tam PK. Liver transplant for biliary atresia is associated with a worse outcome - Myth or fact?. J Pediatr Surg. 2015;50(12):2134–6.
Safwan M, Ramachandran P, Reddy MS, Shanmugam N, Rela M. Living donor liver transplantation for biliary atresia - An Indian experience. Pediatr Transplant. 2016;20(8):1045–50.
Meister RK, Esquivel CO, Cox KL, Concepcion W, Berquist W, Nakazato P, et al. The influence of portoenterostomy with stoma on morbidity in pediatric patients with biliary atresia undergoing orthotopic liver transplantation. J Pediatr Surg. 1993;28(3):387–90.
Alexopoulos SP, Merrill M, Kin C, Matsuoka L, Dorey F, Concepcion W, et al. The impact of hepatic portoenterostomy on liver transplantation for the treatment of biliary atresia: early failure adversely affects outcome. Pediatr Transplant. 2012;16(4):373–8.
Visser BC, Suh I, Hirose S, Rosenthal P, Lee H, Roberts JP, et al. The influence of portoenterostomy on transplantation for biliary atresia. Liver Transpl. 2004;10(10):1279–86.
Millis JM, Brems JJ, Hiatt JR, Klein AS, Ashizawa T, Ramming KP, et al. Orthotopic liver transplantation for biliary atresia. Evolution of management. Arch Surg. 1988;123(10):1237–9.
Neto JS, Feier FH, Bierrenbach AL, Toscano CM, Fonseca EA, Pugliese R, et al. Impact of Kasai portoenterostomy on liver transplantation outcomes: A retrospective cohort study of 347 children with biliary atresia. Liver Transpl. 2015;21(7):922–7.
Shirota C, Uchida H, Ono Y, Murase N, Tainaka T, Yokota K, et al. Long-term outcomes after revision of Kasai portoenterostomy for biliary atresia. J Hepatobiliary Pancreat Sci. 2016;23(11):715–20.
Pareja E, Cortes M, Navarro R, Sanjuan F, Lopez R, Mir J. Vascular complications after orthotopic liver transplantation: hepatic artery thrombosis. Transplant Proc. 2010;42(8):2970–2.
Wu L, Zhang J, Guo Z, Tai Q, He X, Ju W, et al. Hepatic artery thrombosis after orthotopic liver transplant: a review of the same institute 5 years later. Exp Clin Transplant. 2011;9(3):191–6.
Bekker J, Ploem S, de Jong KP. Early hepatic artery thrombosis after liver transplantation: a systematic review of the incidence, outcome and risk factors. Am J Transplant. 2009;9(4):746–57.
Howell JA, Gow PJ, Angus PW, Jones RM, Wang BZ, Bailey M, et al. Early-onset versus late-onset nonanastomotic biliary strictures post liver transplantation: risk factors reflect different pathogenesis. Transpl Int. 2012;25(7):765–75.
Rayhill SC, Wu YM, Katz DA, Voigt MD, Labrecque DR, Kirby PA, et al. Older donor livers show early severe histological activity, fibrosis, and graft failure after liver transplantation for hepatitis C. Transplantation. 2007;84(3):331–9.
Karakayali F, Kirnap M, Akdur A, Tutar N, Boyvat F, Moray G, et al. Biliary complications after pediatric liver transplantation. Transplant Proc. 2013;45(10):3524–7.
Racadio JM, Kukreja K. Pediatric biliary interventions. Tech Vasc Interv Radiol. 2010;13(4):244–9.
Krokidis M, Orgera G, Rossi M, Matteoli M, Hatzidakis A. Interventional radiology in the management of benign biliary stenoses, biliary leaks and fistulas: a pictorial review. Insights Imaging. 2013;4(1):77–84.
Author information
Authors and Affiliations
Contributions
Hsiao CY and Ho MC contributed to data collection, interpretation of data, and drafted the manuscript; Ho MC and Hu RH contributed to study concept and design; Hsiao CY, Ho CM, Wu YM, Ho MC, Hu RH, and Lee PH contributed to critical revision of the manuscript.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hsiao, CY., Ho, CM., Wu, YM. et al. Biliary Complication in Pediatric Liver Transplantation: a Single-Center 15-Year Experience. J Gastrointest Surg 23, 751–759 (2019). https://doi.org/10.1007/s11605-018-04076-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-018-04076-x