Abstract
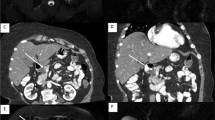
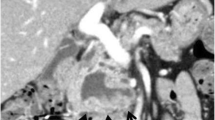
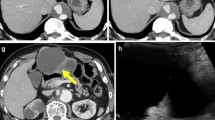
Intraductal papillary mucinous neoplasms (IPMNs) are rare, mucin-producing, predominantly noninvasive tumors arising from epithelial cells. Most IPMNs arise from the pancreas. There exists a subset of IPMN of the biliary tract (BT-IPMN). IPMNs regardless of origin produce large amounts of mucin relative to scant amounts of epithelial cells, leading to mass effect disturbances in bile flow. Affected bile ducts exhibit marked dilatation. The majority of IPMN patients present with a non-malignant neoplasm. Because of potential for transformation, surgery is the treatment of choice. Bronchobiliary fistulas can present as congenital defects, following thoracoabodominal trauma, or as rare complications of diseases of the biliary tract such as BT-IPMN. There are no reported cases in the literature of bronchobiliary fistula associated with BT-IPMN, but there is a clear theoretical risk.


Similar content being viewed by others
References
Minagawa N, Sato N, Mori Y, Tamura T, Higure A, Yamaguchi K. A comparison between intraductal papillary neoplasms of the biliary tract (BT-IPMNs) and intraductal papillary mucinous neoplasms of the pancreas (P-IPMNs) reveals distinct clinical manifestations and outcomes. Eur. J. Surg. Oncol. 2013;39(6):554–8. Available at: http://www.ncbi.nlm.nih.gov/pubmed/23506840. Accessed January 4, 2014.
Barton JG, Barrett DA, Maricevich MA, et al. Intraductal papillary mucinous neoplasm of the biliary tract: a real disease? HPB (Oxford). 2009;11(8):684–91. Available at: http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=2799622&tool=pmcentrez&rendertype=abstract. Accessed December 19, 2013.
Terada T. Non-invasive intraductal papillary neoplasms of the common bile duct: a clinicopathologic study of six cases. Int. J. Clin. Exp. Pathol. 2012;5(7):690–7. Available at: http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=3438766&tool=pmcentrez&rendertype=abstract. Accessed January 4, 2014.
Terada T, Mitsui T, Nakanuma Y, Miura S, Toya D. Intrahepatic biliary papillomatosis arising in nonobstructive intrahepatic biliary dilatations confined to the hepatic left lobe. Am. J. Gastroenterol. 1991;86(10):1523–6. Available at: http://www.ncbi.nlm.nih.gov/pubmed/1928050. Accessed January 4, 2014.
Lim JH, Jang K-T, Choi D. Biliary intraductal papillary-mucinous neoplasm manifesting only as dilatation of the hepatic lobar or segmental bile ducts: imaging features in six patients. AJR. Am. J. Roentgenol. 2008;191(3):778–82. Available at: http://www.ajronline.org/doi/full/10.2214/AJR.07.2091. Accessed December 19, 2013.
Jung G, Park K-M, Lee SS, Yu E, Hong S-M, Kim J. Long-term clinical outcome of the surgically resected intraductal papillary neoplasm of the bile duct. J. Hepatol. 2012;57(4):787–93. Available at: http://www.ncbi.nlm.nih.gov/pubmed/22634127. Accessed January 4, 2014.
Gugenheim J, Ciardullo M, Traynor O, Bismuth H. Bronchobiliary fistulas in adults. Ann. Surg. 1988;207(1):90–4. Available at: http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=1493242&tool=pmcentrez&rendertype=abstract. Accessed January 7, 2014.
Eryigit H, Oztas S, Urek S, Olgac G, Kurutepe M, Kutlu CA. Management of acquired bronchobiliary fistula: 3 case reports and a literature review. J. Cardiothorac. Surg. 2007;2(1):52. Available at: http://www.cardiothoracicsurgery.org/content/2/1/52. Accessed January 7, 2014.
IRB Approval
Done
Conflict of Interest
None
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Mo, A., Brat, G., Spolverato, G. et al. Intraductal Papillary Mucinous Neoplasm of the Liver: GI Image. J Gastrointest Surg 19, 792–794 (2015). https://doi.org/10.1007/s11605-015-2750-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-015-2750-2