Abstract
Purpose
Loss of skeletal muscle mass, which depends on a balance between protein synthesis and degradation, is common in sarcopenia, cachexia, and some diseases. The purpose of this study was to investigate the alterations and interactions of protein synthesis and degradation signaling components induced by 8-week endurance exercise training with a normal diet.
Methods
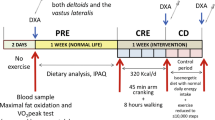
Two exercise (n = 8) and control (n = 7) groups of Wistar rats were kept under standard conditions. The exercise group performed 8-week endurance running at 65–70% VO2max, 30–60 min, on a treadmill with 0° slope, and the rats of the control group were maintained under identical conditions except exercise training. Forty-eight hours after the last exercise session, the dissected soleus muscles were stored at − 80 °C for gene and protein expression analyses.
Results
Although there was a non-significant increase in mTOR gene expression, Akt1 and S6K1 increased significantly compared with the control group, which was confirmed by Western blot analysis. In addition, given that the FoxO3a did not increase, 4E-BP1 and LC3a were suppressed significantly and were confirmed by Western blot analysis. Contrary to our hypothesis, the MuRF1 gene expression was significantly increased compared with the control group.
Conclusion
The results showed that the moderate-intensity endurance exercise training protocol with no calories restrictions, normal diet, not only does not lead to protein degradation but also sufficiently activates protein synthesis signaling. Further investigations including exercise training with different intensities and nutritional status are needed to reveal the cause of the unusual MuRF1 response.




Similar content being viewed by others
References
Kandarian SC, Jackman RW (2006) Intracellular signaling during skeletal muscle atrophy. Muscle Nerve 33(2):155–165. https://doi.org/10.1002/mus.20442
McCarthy JJ, Esser KA (2010) Anabolic and catabolic pathways regulating skeletal muscle mass. Curr Opin Clin Nutr Metab Care 13(3):230–235. https://doi.org/10.1097/MCO.0b013e32833781b5
Sandri M (2008) Signaling in muscle atrophy and hypertrophy. Physiology 23(3):160–170. https://doi.org/10.1152/physiol.00041.2007
Manning BD, Cantley LC (2007) AKT/PKB signaling: navigating downstream. Cell 129(7):1261–1274. https://doi.org/10.1016/j.cell.2007.06.009
Schiaffino S, Dyar KA, Ciciliot S, Blaauw B, Sandri M (2013) Mechanisms regulating skeletal muscle growth and atrophy. FEBS J 280(17):4294–4314. https://doi.org/10.1111/febs.12253
Wullschleger S, Loewith R, Hall MN (2006) TOR signaling in growth and metabolism. Cell 124(3):471–484. https://doi.org/10.1016/j.cell.2006.01.016
Hodson N, Philp A (2019) The importance of mTOR trafficking for human skeletal muscle translational control. Exerc Sport Sci Rev 47(1):46–53. https://doi.org/10.1249/JES.0000000000000173
Mamane Y, Petroulakis E, Rong L, Yoshida K, Ler LW, Sonenberg N (2004) eIF4E–from translation to transformation. Oncogene 23(18):3172–3179. https://doi.org/10.1038/sj.onc.1207549
Saxton RA, Sabatini DM (2017) mTOR signaling in growth, metabolism, and disease. Cell 168(6):960–976. https://doi.org/10.1016/j.cell.2017.02.004
Stitt TN, Drujan D, Clarke BA, Panaro F, Timofeyva Y, Kline WO, Gonzalez M, Yancopoulos GD, Glass DJ (2004) The IGF-1/PI3K/Akt pathway prevents expression of muscle atrophy-induced ubiquitin ligases by inhibiting FOXO transcription factors. Mol Cell 14(3):395–403. https://doi.org/10.1016/S1097-2765(04)00211-4
Wang L, Karpac J, Jasper H (2014) Promoting longevity by maintaining metabolic and proliferative homeostasis. J Exp Biol 217(1):109–118. https://doi.org/10.1242/jeb.089920
Benayoun BA, Caburet S, Veitia RA (2011) Forkhead transcription factors: key players in health and disease. Trends Genet 27(6):224–232. https://doi.org/10.1016/j.tig.2011.03.003
Bodine SC, Baehr LM (2014) Skeletal muscle atrophy and the E3 ubiquitin ligases MuRF1 and MAFbx/atrogin-1. Am J Physiol Endocrinol Metab 307(6):E469-484. https://doi.org/10.1152/ajpendo.00204.2014
Zhao L, Li H, Wang Y, Zheng A, Cao L, Liu J (2019) Autophagy deficiency leads to impaired antioxidant defense via p62-FOXO1/3 axis. Oxid Med Cell Longev. https://doi.org/10.1155/2019/2526314
Sandri M, Sandri C, Gilbert A, Skurk C, Calabria E, Picard A, Walsh K, Schiaffino S, Lecker SH, Goldberg AL (2004) Foxo transcription factors induce the atrophy-related ubiquitin ligase atrogin-1 and cause skeletal muscle atrophy. Cell 117(3):399–412. https://doi.org/10.1016/S0092-8674(04)00400-3
Waddell DS, Baehr LM, Van Den Brandt J, Johnsen SA, Reichardt HM, Furlow JD, Bodine SC (2008) The glucocorticoid receptor and FOXO1 synergistically activate the skeletal muscle atrophy-associated MuRF1 gene. Am J Physiol Endocrinol Metab 295(4):E785-797. https://doi.org/10.1152/ajpendo.00646.2007
Lee YK, Lee JA (2016) Role of the mammalian ATG8/LC3 family in autophagy: differential and compensatory roles in the spatiotemporal regulation of autophagy. BMB Rep 49(8):424–430. https://doi.org/10.5483/BMBRep.2016.49.8.081
Zhao J, Brault JJ, Schild A, Cao P, Sandri M, Schiaffino S, Lecker SH, Goldberg AL (2007) FoxO3 coordinately activates protein degradation by the autophagic/lysosomal and proteasomal pathways in atrophying muscle cells. Cell Metab 6(6):472–483. https://doi.org/10.1016/j.cmet.2007.11.004
Atherton PJ, Babraj J, Smith K, Singh J, Rennie MJ, Wackerhage H (2005) Selective activation of AMPK-PGC-1α or PKB-TSC2-mTOR signaling can explain specific adaptive responses to endurance or resistance training-like electrical muscle stimulation. FASEB J 19(7):786–788. https://doi.org/10.1096/fj.04-2179fje
Huet C, Boudaba N, Guigas B, Viollet B, Foretz M (2020) Glucose availability but not changes in pancreatic hormones sensitizes hepatic AMPK activity during nutritional transition in rodents. J Biol Chem 295(18):5836–5849. https://doi.org/10.1074/jbc.RA119.010244
Kazior Z, Willis SJ, Moberg M, Apro W, Calbet JA, Holmberg HC, Blomstrand E (2016) Endurance exercise enhances the effect of strength training on muscle fiber size and protein expression of Akt and mTOR. PLoS One 11(2):e0149082. https://doi.org/10.1371/journal.pone.0149082
Cui X, Zhang Y, Wang Z, Yu J, Kong Z, Ružić L (2019) High-intensity interval training changes the expression of muscle RING-finger protein-1 and muscle atrophy F-box proteins and proteins involved in the mechanistic target of rapamycin pathway and autophagy in rat skeletal muscle. Exp Physiol 104(10):1505–1517. https://doi.org/10.1113/EP087601
Høydal MA, Wisløff U, Kemi OJ, Ellingsen Ø (2007) Running speed and maximal oxygen uptake in rats and mice: practical implications for exercise training. Eur J Cardiovasc Prev Rehabil 14(6):753–760. https://doi.org/10.1097/HJR.0b013e3281eacef1
Wisløff U, Helgerud J, Kemi OJ, Ellingsen Ø (2001) Intensity-controlled treadmill running in rats: V̇o(2 max) and cardiac hypertrophy. Am J Physiol Heart Circ Physiol 280(3):H1301-1310. https://doi.org/10.1152/ajpheart.2001.280.3.H1301
Liao J, Li Y, Zeng F, Wu Y (2015) Regulation of mTOR pathway in exercise-induced cardiac hypertrophy. Int J Sports Med 36(5):343–350. https://doi.org/10.1055/s-0034-1395585
Sturgeon K, Muthukumaran G, Ding D, Bajulaiye A, Ferrari V, Libonati JR (2015) Moderate-intensity treadmill exercise training decreases murine cardiomyocyte cross-sectional area. Physiol Rep 3(5):e12406. https://doi.org/10.14814/phy2.12406
Sakakima H, Yoshida Y, Sakae K, Morimoto N (2004) Different frequency treadmill running in immobilization-induced muscle atrophy and ankle joint contracture of rats. Scand J Med Sci Sports 14(3):186–192. https://doi.org/10.1111/j.1600-0838.2004.382.x
McKenzie MJ, Goldfarb AH, Kump DS (2011) Gene response of the gastrocnemius and soleus muscles to an acute aerobic run in rats. J Sport Sci Med 10(2):385. https://doi.org/10.1249/01.mss.0000353510.09224.94
Glass DJ (2005) Skeletal muscle hypertrophy and atrophy signaling pathways. Int J Biochem Cell Biol 37(10):1974–1984. https://doi.org/10.1016/j.biocel.2005.04.018
Schiaffino S, Mammucari C (2011) Regulation of skeletal muscle growth by the IGF1-Akt/PKB pathway: insights from genetic models. Skelet Muscle 1(1):4. https://doi.org/10.1186/2044-5040-1-4
Kim E, Goraksha-Hicks P, Li L, Neufeld TP, Guan KL (2008) Regulation of TORC1 by Rag GTPases in nutrient response. Nat Cell Biol 10(8):935–945. https://doi.org/10.1038/ncb1753
Sancak Y, Bar-Peled L, Zoncu R, Markhard AL, Nada S, Sabatini DM (2010) Ragulator-Rag complex targets mTORC1 to the lysosomal surface and is necessary for its activation by amino acids. Cell 141(2):290–303. https://doi.org/10.1016/j.cell.2010.02.024
Aoyama T, Matsui T, Novikov M, Park J, Hemmings B, Rosenzweig A (2005) Serum and glucocorticoid-responsive kinase-1 regulates cardiomyocyte survival and hypertrophic response. Circulation 111(13):1652–1659. https://doi.org/10.1161/01.CIR.0000160352.58142.06
Avruch J, Belham C, Weng Q, Hara K, Yonezawa K (2001) The p70S6 kinase integrates nutrient and growth signals to control translational capacity. Prog Mol Subcell Biol 26:115–154. https://doi.org/10.1007/978-3-642-56688-2_5
Hay N, Sonenberg N (2004) Upstream and downstream of mTOR. Genes Dev 18(16):1926–1945. https://doi.org/10.1101/gad.1212704
Ma XM, Blenis J (2009) Molecular mechanisms of mTOR-mediated translational control. Nat Rev Mol Cell Biol 10(5):307–318. https://doi.org/10.1038/nrm2672
Qin X, Jiang B, Zhang Y (2016) 4E-BP1, a multifactor regulated multifunctional protein. Cell Cycle 15(6):781–786. https://doi.org/10.1080/15384101.2016.1151581
Milan G, Romanello V, Pescatore F, Armani A, Paik JH, Frasson L, Seydel A, Zhao J, Abraham R, Goldberg AL, Blaauw B, DePinho RA, Sandri M (2015) Regulation of autophagy and the ubiquitin–proteasome system by the FoxO transcriptional network during muscle atrophy. Nat Commun 6:6670. https://doi.org/10.1038/ncomms7670
Puig O, Marr MT, Ruhf ML, Tjian R (2003) Control of cell number by Drosophila FOXO: downstream and feedback regulation of the insulin receptor pathway. Genes Dev 17(16):2006–2020. https://doi.org/10.1101/gad.1098703
Tzivion G, Dobson M (1813) Ramakrishnan G (2011) FoxO transcription factors; regulation by AKT and 14–3-3 proteins. Biochim Biophys Acta 11:1938–1945. https://doi.org/10.1016/j.bbamcr.2011.06.002
Huang H, Tindall DJ (2007) Dynamic FoxO transcription factors. J Cell Sci 120(15):2479–2487. https://doi.org/10.1242/jcs.001222
Mizushima N, Yamamoto A, Matsui M, Yoshimori T, Ohsumi Y (2004) In vivo analysis of autophagy in response to nutrient starvation using transgenic mice expressing a fluorescent autophagosome marker. Mol Biol Cell 15(3):1101–1111. https://doi.org/10.1091/mbc.e03-09-0704
Ghosh R, Pattison JS (2018) Macroautophagy and chaperone-mediated autophagy in heart failure: the known and the unknown. Oxid Med Cell Longev. https://doi.org/10.1155/2018/8602041
Parzych KR, Klionsky DJ (2014) An overview of autophagy: morphology, mechanism, and regulation. Antioxid Redox Signal 20(3):460–473. https://doi.org/10.1089/ars.2013.5371
Clarke BA, Drujan D, Willis MS, Murphy LO, Corpina RA, Burova E, Rakhilin SV, Stitt TN, Patterson C, Latres E, Glass DJ (2007) The E3 Ligase MuRF1 degrades myosin heavy chain protein in dexamethasone-treated skeletal muscle. Cell Metab 6(5):376–385. https://doi.org/10.1016/j.cmet.2007.09.009
Popovic B, Popovic D, Macut D, Antic IB, Isailovic T, Ognjanovic S, Bogavac T, Kovacevic VE, Ilic D, Petrovic M, Damjanovic S (2019) Acute response to endurance exercise stress: focus on catabolic/anabolic interplay between cortisol, testosterone, and sex hormone binding globulin in professional athletes. J Med Biochem 38(1):6–12. https://doi.org/10.2478/jomb-2018-0016
Martin-Rincon M, Pérez-López A, Morales-Alamo D, Perez-Suarez I, de Pablos-Velasco P, Perez-Valera M, Perez-Regalado S, Martinez-Canton M, Gelabert-Rebato M, Juan-Habib JW, Holmberg HC (2019) Exercise mitigates the loss of muscle mass by attenuating the activation of autophagy during severe energy deficit. Nutrients 11(11):E2824. https://doi.org/10.3390/nu11112824
Sudhakar SR, Varghese J (2018) Insulin signalling activates multiple feedback loops to elicit hunger-induced feeding in Drosophila. Dev Biol. https://doi.org/10.1016/j.ydbio.2019.11.013
Hellyer NJ, Nokleby JJ, Thicke BM, Zhan WZ, Sieck GC, Mantilla CB (2012) Reduced ribosomal protein S6 phosphorylation following progressive resistance exercise in growing adolescent rats. J Strength Cond Res 26(6):1657–1666. https://doi.org/10.1519/JSC.0b013e318231abc9
Cartee GD, Hepple RT, Bamman MM, Zierath JR (2016) Exercise promotes healthy aging of skeletal muscle. Cell Metab 23(6):1034–1047. https://doi.org/10.1016/j.cmet.2016.05.007
Funding
No funding was supported for conducting this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All experiments and procedures used in this study were in accordance with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. In addition, approval was obtained from the ethics committee of the Sport Sciences Research Institute of Iran.
Informed consent
For this type of study formal consent is not required.
Human and animal rights
All procedures of this study were approved by the Payame Noor University Research Ethics Committee.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Gholipour, M., Seifabadi, M. & Asad, M.R. Endurance exercise training under normal diet conditions activates skeletal muscle protein synthesis and inhibits protein degradation signaling except MuRF1. Sport Sci Health 18, 1033–1041 (2022). https://doi.org/10.1007/s11332-021-00888-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11332-021-00888-8