Abstract
Purpose
Since hypoxia increases erythropoietin production and inflammation, the complete blood count (CBC) has been proposed as an inexpensive alternative for obstructive sleep apnea (OSA) screening. The objective of this study was to determine whether or not intermittent hypoxia and OSA severity, as measured by the mean oxygen saturation (SpO2) and apnea–hypopnea index (AHI), affect parameters measured by the CBC.
Methods
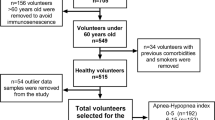
This retrospective study included a total of 941 surgical patients who had a pre-operative home sleep study. The pre-operative CBC was extracted from the electronic patient records. Patients were stratified according to their AHI scores, into mild (AHI ≥ 5 – < 15), moderate (AHI ≥ 15 – < 30), and severe (AHI ≥ 30) OSA groups.
Results
There were 244 patients without OSA, 294 with mild, 223 with moderate, and 180 with severe OSA. Our analysis showed that hemoglobin (P = 0.010), hematocrit (P = 0.027), and basophils (P = 0.006) showed significant changes among the different severities of OSA. For mean SpO2, there were negative associations with body mass index (r = − 0.287; P < 0.001), age (r = − 0.077; P = 0.021), hemoglobin (r = − 0.208; P < 0.001), hematocrit (r = − 0.220; P < 0.001), red blood cells (r = − 0.107; P = 0.001), mean corpuscular volume (MCV) (r = − 0.159; P < 0.001), mean corpuscular hemoglobin (r = − 0.142; P < 0.001), and basophils (r = − 0.091; P = 0.007). All analyzed parameters remained within normal clinical range. Multivariable regression identified hemoglobin, MCV, and basophils to be independent predictors of mean SpO2 and AHI.
Conclusion
Hemoglobin, MCV, and basophils were independently associated with intermittent hypoxia defined by mean SpO2 and AHI. Adding CBC parameters to other screening tools for OSA may have additional value due to its association with changes in mean SpO2.

Similar content being viewed by others
Abbreviations
- CBC:
-
Complete blood count
- AHI:
-
Apnea–hypopnea index
- OSA:
-
Obstructive sleep apnea
- SpO2 :
-
Oxygen saturation
References
Peppard PE, Young T, Barnet JH, Palta M, Hagen EW, Hla KM (2013) Increased prevalence of sleep-disordered breathing in adults. Am J Epidemiol 177(9):1006–1014. https://doi.org/10.1093/aje/kws342
Somers VK, White DP, Amin R, Abraham WT, Costa F, Culebras A, Daniels S, Floras JS, Hunt CE, Olson L, Pickering T, Russell T, Woo M, Young T (2008) Sleep apnea and cardiovascular disease. J Am Coll Cardiol 52(8):686–717. https://doi.org/10.1161/CIRCULATIONAHA.107.189420
Wang X, Bi Y, Zhang Q, Pan F (2013) Obstructive sleep apnoea and the risk of type 2 diabetes: a meta-analysis of prospective cohort studies. Respirology 18(1):140–146. https://doi.org/10.1111/j.1440-1843.2012.02267.x
Young T, Finn L, Peppard PE, Szklo-Coxe M, Austin D, Nieto FJ, Stubbs R, Hla K (2008) Sleep disordered breathing and mortality: eighteen-year follow-up of the Wisconsin sleep cohort. Sleep 31(8):1071–1078
Fan Z, Lu X, Long H, Li T, Zhang Y (2019) The association of hemocyte profile and obstructive sleep apnea. J Clin Lab Anal 33(2):e22680. https://doi.org/10.1002/jcla.22680
Ryan S, Taylor CT, McNicholas WT (2006) Predictors of elevated nuclear factor-kappaB-dependent genes in obstructive sleep apnea syndrome. Am J Respir Crit Care Med 174(7):824–830. https://doi.org/10.1164/rccm.200601-066OC
Bulbul Y, Aydin Ozgur E, Orem A (2016) Platelet indices in obstructive sleep apnea: the role of mean platelet volume, platelet distribution widht and plateletcrit. Tuberk Toraks 64(3):206–210. https://doi.org/10.5578/tt.29170
Freire AX, Kadaria D, Avecillas JF, Murillo LC, Yataco JC (2010) Obstructive sleep apnea and immunity: relationship of lymphocyte count and apnea hypopnea index. South Med J 103(8):771–774. https://doi.org/10.1097/SMJ.0b013e3181e6dabf
Korkmaz M, Korkmaz H, Kucuker F, Ayyildiz SN, Çankaya S (2015) Evaluation of the association of sleep apnea- related systemic inflammation with CRP, ESR, and neutrophil-to-lymphocyte ratio. Med Sci Monit 21:477–481. https://doi.org/10.12659/MSM.893175
Kurt OK, Yildiz N (2013) The importance of laboratory parameters in patients with obstructive sleep apnea syndrome. Blood Coagul Fibrinolysis 24(4):371–374. https://doi.org/10.1097/MBC.0b013e32835d53d4
Wu M, Zhou L, Zhu D, Lai T, Chen Z, Shen H (2018) Hematological indices as simple, inexpensive and practical severity markers of obstructive sleep apnea syndrome: a meta-analysis. J Thorac Dis 10(12):6509–6521. https://doi.org/10.21037/jtd.2018.10.105
Choi JB, Loredo JS, Norman D, Mills PJ, Ancoli-Israel S, Ziegler MG, Dimsdale JE (2006) Does obstructive sleep apnea increase hematocrit? Sleep Breath 10(3):155–160. https://doi.org/10.1007/s11325-006-0064-z
Nguyen CD, Holty J-EC (2017) Does untreated obstructive sleep apnea cause secondary erythrocytosis? Respir Med 130:27–34. https://doi.org/10.1016/j.rmed.2017.07.003
Li N, Li HP, Wang P, Yan YR, Li SQ, Li QY (2019) Nocturnal mean oxygen saturation is associated with secondary polycythemia in young adults with obstructive sleep apnea, especially in men. Nat Sci Sleep 11:377. https://doi.org/10.2147/NSS.S226143
Suen C, Ryan CM, Mubashir T, Ayas NT, Abrahamyan L, Wong J, Mokhlesi B, Chung F (2019) Sleep study and oximetry parameters for predicting postoperative complications in patients with OSA. Chest 155(5):855–867. https://doi.org/10.1016/j.chest.2018.09.030
Chung F, Liao P, Elsaid H, Shapiro CM, Kang W (2014) Factors associated with postoperative exacerbation of sleep-disordered breathing. Anesthesiology 120(2):299–311. https://doi.org/10.1097/aln.0000000000000041
Chan MTV, Wang CY, Seet E, Tam S, Lai HY, Chew EFF, Wu WKK, Cheng BCP, Lam CKM, Short TG, Hui DSC, Chung F (2019) Association of unrecognized obstructive sleep apnea with postoperative cardiovascular events in patients undergoing major noncardiac surgery. JAMA 321(18):1788. https://doi.org/10.1001/jama.2019.4783
Berry RB, Gamaldo CE, Harding SM, Brooks R, Lloyd RM, Vaughn BV, Marcus CL (2015) AASM scoring manual version 2.2 updates: new chapters for scoring infant sleep staging and home sleep apnea testing. J Clin Sleep Med 11(11):1253–1254. https://doi.org/10.5664/jcsm.5176
Windsor JS, Rodway GW (2007) Heights and haematology: the story of haemoglobin ataltitude. Postgrad Med J 83:148–51. https://doi.org/10.1136/pgmj.2006.049734
Jelkmann W (2011) Regulation of erythropoietin production. J Physiol 589(6):1251–1258. https://doi.org/10.1113/jphysiol.2010.195057
Zhang XB, Zeng YM, Zeng HQ, Zhang HP, Wang HL (2017) Erythropoietin levels in patients with sleep apnea: a meta-analysis. Eur Arch Otorhinolaryngol 274(6):2505–2512. https://doi.org/10.1007/s00405-017-4483-1
Zhang C, Zhang J, Lü X, Li B (2009) Effects of intermittent hypoxic exposure on the parameter of erythrocyte and serum hypoxia inducible factor-1 alpha and erythropoietin levels. Xi Bao Yu Fen Zi Mian Yi Xue Za Zhi 25(10):932–934
Kang J, Li Y, Hu K, Lu W, Zhou X, Yu S, Xu L (2016) Chronic intermittent hypoxia versus continuous hypoxia: same effects on hemorheology? Clin Hemorheol Microcirc 63(3):245–255. https://doi.org/10.3233/CH-151973
Cahan C, Decker MJ, Arnold JL, Goldwasser E, Strohl KP (1995) Erythropoietin levels with treatment of obstructive sleep apnea. J Appl Physiol 79(4):1278–1285. https://doi.org/10.1152/jappl.1995.79.4.1278
Doğan D, Öcal R (2019) Possible changes in hematological parameters of the patients with obstructive sleep apnea. Gulhane Med J 61(3). https://doi.org/10.26657/gulhane.00064
Andersen CJ, Vance TM (2019) Gender dictates the relationship between serum lipids and leukocyte counts in the national health and nutrition examination survey 1999–2004. J Clin Med 8(3):365. https://doi.org/10.3390/jcm8030365
Gündüz C, Basoglu OK, Hedner J, Zou D, Bonsignore MR, Hein H, Staats R, Pataka A, Barbe F, Sliwinski P, Kent BD, Pepin JL, Grote L, Collaborators ESAD (2018) Obstructive sleep apnoea independently predicts lipid levels: Data from the European Sleep Apnea Database. Respirology 23(12):1180–1189. https://doi.org/10.1111/resp.13372
Cao Y, Wu S, Zhang L, Yang Y, Cao S, Li Q (2018) Association of allergic rhinitis with obstructive sleep apnea: a meta-analysis. Medicine (Baltimore) 97(51). https://doi.org/10.1097/MD.0000000000013783
Miyake K, Karasuyama H (2017) Emerging roles of basophils in allergic inflammation. Allergol Int 66(3):382–391. https://doi.org/10.1016/j.alit.2017.04.007
Chung F, Abdullah HR, Liao P (2016) STOP-Bang questionnaire: a practical approach to screen for obstructive sleep apnea. Chest 149(3):631–638. https://doi.org/10.1378/chest.15-0903
Funding
This work was funded by University Health Network Foundation and the Department of Anesthesia and Pain Medicine, Toronto Western Hospital, University Health Network, University of Toronto.
Author information
Authors and Affiliations
Contributions
Emer Cummins – This author contributed to data collection and interpretation, and writing of the manuscript.
Rida Waseem – This author contributed to data analysis and writing of the manuscript.
Deween Piyasena – This author contributed to data collection and interpretation, and writing of the manuscript.
Chew Yin Wang – This author contributed to data collection and writing of the manuscript.
Colin Suen – This author contributed to writing of the manuscript.
Clodagh Ryan – This author contributed to writing of the manuscript.
Jean Wong – This author contributed to writing of the manuscript.
Meir Kryger – This author contributed to writing of the manuscript.
Frances Chung – This author contributed to study concept and design, data acquisition and interpretation, and writing of the manuscript.
All authors have seen and approved this manuscript.
Corresponding author
Ethics declarations
Conflict of interest
Frances Chung is supported by Up-to-Date royalties, STOP-Bang questionnaire (proprietary to University Health Network). The rest of the authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This work was performed at University Health Network, University of Toronto, Ontario, Canada and University of Malaya, Kuala Lumpur, Malaysia
Rights and permissions
About this article
Cite this article
Cummins, E., Waseem, R., Piyasena, D. et al. Can the complete blood count be used as a reliable screening tool for obstructive sleep apnea?. Sleep Breath 26, 613–620 (2022). https://doi.org/10.1007/s11325-021-02383-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-021-02383-3