Abstract
Introduction
Patients with obstructive sleep apnea (OSA) and comorbid diabetes mellitus (DM) are reported to have an increased risk of cardiovascular (CV) outcomes; however, data on CV mortality are scant.
Aim
This study aimed to evaluate if patients with comorbid OSA and DM have an increased risk of CV mortality that is higher than the two diseases in isolation.
Methods
In this prospective cohort study, we included patients referred for a sleep study with and without DM at baseline. We developed four study groups as follows: group 1 (reference group), OSA (−) DM (−); group 2, OSA (−) DM (+); group 3, OSA (+) DM (−); group 4, OSA (+) DM (+). Intergroup differences were evaluated using the t test and χ2 test, and multivariate analysis was performed using logistic regression. The incidence rates of CV mortality were calculated using the Kaplan–Meier (log-rank) model, and adjusted HRs were calculated using the Cox regression model.
Results
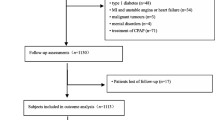
A total of 1447 patients were included in the analysis—group 1: 441 participants; group 2: 141 participants; group 3: 736 participants; group 4: 151 participants. The mean follow-up was 5 years. The association between OSA + DM showed an independent risk of incident CV mortality (HR 2.37, CI 1.16–4.82, p = 0.02) and an increased prevalence of coronary heart disease (OR 3.44, CI 1.73–5.59, p < 0.01). In addition, T90% was also associated with CV mortality.
Conclusion
The coexistence of OSA + DM was associated with an independent risk of CV mortality. In addition, T90% was also associated with CV mortality.


Similar content being viewed by others
References
Benjafield AV, Ayas NT, Eastwood PR, Heinzer R, Ip MSM, Morrell MJ, Nunez CM, Patel SR, Penzel T, Pépin JL, Peppard PE, Sinha S, Tufik S, Valentine K, Malhotra A (2019) Estimation of the global prevalence and burden of obstructive sleep apnoea: a literature-based analysis. Lancet Respir Med. 7(8):687–698
Phillipson EA (1993) Sleep apnea—a major public health problem. N Engl J Med. 328(17):1271–1273
Qaseem A, Dallas P, Owens DK, Starkey M, Holty JE, Shekelle P et al (2014) Diagnosis of obstructive sleep apnea in adults: a clinical practice guideline from the American College of Physicians. Ann Intern Med. 161(3):210–220
Kapur VK, Auckley DH, Chowdhuri S, Kuhlmann DC, Mehra R, Ramar K, Harrod CG (2017) Clinical practice guideline for diagnostic testing for adult obstructive sleep apnea: an American Academy of Sleep Medicine clinical practice guideline. J Clin Sleep Med. 13(3):479–504
Labarca G, Gower J, Lamperti L, Dreyse J, Jorquera J (2020) Chronic intermittent hypoxia in obstructive sleep apnea: a narrative review from pathophysiological pathways to a precision clinical approach. Sleep Breath 24(2):751–760. https://doi.org/10.1007/s11325-019-01967-4
Marin JM, Carrizo SJ, Vicente E, Agusti AG (2005) Long-term cardiovascular outcomes in men with obstructive sleep apnoea–hypopnoea with or without treatment with continuous positive airway pressure: an observational study. Lancet. 365(9464):1046–1053
Koo CY, Drager LF, Sethi R, Ho HH, Hein T, Jim MH, Tai BC, Zhang JJ, Lee CH (2018) Obstructive sleep apnea and diabetes independently add to cardiovascular risk after coronary revascularization. Diabetes Care. 41(2):e12–ee4
Mahmood K, Akhter N, Eldeirawi K, Onal E, Christman JW, Carley DW et al (2009) Prevalence of type 2 diabetes in patients with obstructive sleep apnea in a multi-ethnic sample. J Clin Sleep Med. 5(3):215–221
Li X, Sotres-Alvarez D, Gallo LC, Ramos AR, Aviles-Santa L, Perreira KM, Isasi CR, Zee PC, Savin KL, Schneiderman N, Wassertheil-Smoller S, Sofer T, Daviglus M, Redline S (2020) Associations of sleep disordered breathing and insomnia with incident hypertension and diabetes: The Hispanic Community Health Study/Study of Latinos. Am J Respir Crit Care Med.
Knutson KL, Wu D, Patel SR, Loredo JS, Redline S, Cai J, et al (2017) Association between sleep timing, obesity, diabetes: The Hispanic Community Health Study/Study of Latinos (HCHS/SOL) cohort study. Sleep 40(4)
von Elm E, Altman DG, Egger M, Pocock SJ, Gotzsche PC, Vandenbroucke JP et al (2007) The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. PLoS Med. 4(10):e296
Johns MW (1991) A new method for measuring daytime sleepiness: the Epworth sleepiness scale. Sleep. 14(6):540–545
Ye L, Pien GW, Ratcliffe SJ, Bjornsdottir E, Arnardottir ES, Pack AI et al (2014) The different clinical faces of obstructive sleep apnoea: a cluster analysis. Eur Respir J. 44(6):1600–1607
Pien GW, Ye L, Keenan BT, Maislin G, Bjornsdottir E, Arnardottir ES et al (2018) Changing faces of obstructive sleep apnea: treatment effects by cluster designation in the Icelandic sleep apnea cohort. Sleep 41(3)
Flemons WW (2002) Clinical practice. Obstructive sleep apnea. N Engl J Med. 347(7):498–504
Labarca G, Dreyse J, Salas C, Gaete MI, Jorquera J (2019) Performance of instruments aimed at detecting obstructive sleep apnea syndrome among individuals in Chile. J Bras Pneumol. 46(1):e20190015
Wang YP, Gorenstein C (2013) Psychometric properties of the Beck Depression Inventory-II: a comprehensive review. Braz J Psychiatry. 35(4):416–431
Lam JC, Mak JC, Ip MS (2012) Obesity, obstructive sleep apnoea and metabolic syndrome. Respirology. 17(2):223–236
Yilmaz Avci A, Avci S, Lakadamyali H, Can U (2017) Hypoxia and inflammation indicate significant differences in the severity of obstructive sleep apnea within similar apnea–hypopnea index groups. Sleep Breath. 21(3):703–711
Labarca G, Cruz NR, Descalzi F (2014) Multisystemic involvement in obstructive sleep apnea. Rev Med Chil. 142(6):748–757
Izci Balserak B, Pien GW, Prasad B, Mastrogiannis D, Park C, Quinn LT et al (2020) Obstructive sleep apnea is associated with newly-diagnosed gestational diabetes mellitus. Ann Am Thorac Soc
Labarca G, Reyes T, Jorquera J, Dreyse J, Drake L (2018) CPAP in patients with obstructive sleep apnea and type 2 diabetes mellitus: systematic review and meta-analysis. Clin Respir J. 12(8):2361–2368
Labarca G, Abud R (2020) Impact of continuous positive airway pressure on glucose metabolism. Sleep Med 65:149. https://doi.org/10.1016/j.sleep.2019.10.009
Javaheri S, Martinez-Garcia MA, Campos-Rodriguez F (2019) CPAP treatment and cardiovascular prevention: we need to change the design and implementation of our trials. Chest. 156(3):431–437
Mazzotti DR, Keenan BT, Lim DC, Gottlieb DJ, Kim J, Pack AI (2019) Symptom subtypes of obstructive sleep apnea predict incidence of cardiovascular outcomes. Am J Respir Crit Care Med
Azarbarzin A, Sands SA, Stone KL, Taranto-Montemurro L, Messineo L, Terrill PI, Ancoli-Israel S, Ensrud K, Purcell S, White DP, Redline S, Wellman A (2019) The hypoxic burden of sleep apnoea predicts cardiovascular disease-related mortality: the Osteoporotic Fractures in Men Study and the Sleep Heart Health Study. Eur Heart J. 40(14):1149–1157
Labarca G, Campos J, Thibaut K, Dreyse J, Jorquera J (2019) Do T90 and SaO2 nadir identify a different phenotype in obstructive sleep apnea? Sleep Breath 23(3):1007–1010. https://doi.org/10.1007/s11325-019-01860-0
Punjabi NM (2016) COUNTERPOINT: Is the apnea–hypopnea index the best way to quantify the severity of sleep-disordered breathing? No Chest 149(1):16–19
Labarca G, Dreyse J, Salas C, Letelier F, Schmidt A, Rivera F, Jorquera J (2020) Clinical utility of oximetric parameters to identify a high-risk phenotype of moderate-severe obstructive sleep apnea (OSA). Clin Respir J. 14:1166–1175
Martinez-Garcia MA, Campos-Rodriguez F, Catalan-Serra P, Soler-Cataluna JJ, Almeida-Gonzalez C, De la Cruz MI et al (2012) Cardiovascular mortality in obstructive sleep apnea in the elderly: role of long-term continuous positive airway pressure treatment: a prospective observational study. Am J Respir Crit Care Med. 186(9):909–916
Sillah A, Watson NF, Schwartz SM, Gozal D, Phipps AI (2018) Sleep apnea and subsequent cancer incidence. Cancer Causes Control. 29(10):987–994
Martinez-Garcia MA, Campos-Rodriguez F, Barbe F, Gozal D, Agusti A (2019) Precision medicine in obstructive sleep apnoea. Lancet Respir Med. 7(5):456–464
Salas C, Dreyse J, Contreras A, Nazar G, Astorquiza C, Cabezon R, Labarca G, Jorquera J (2019) Differences in patients derived from otolaryngology and other specialties with sleep apnea. J Otolaryngol Head Neck Surg. 48(1):53
Cespedes EM, Dudley KA, Sotres-Alvarez D, Zee PC, Daviglus ML, Shah NA, Talavera GA, Gallo LC, Mattei J, Qi Q, Ramos AR, Schneiderman N, Espinoza-Giacinto RA, Patel SR (2016) Joint associations of insomnia and sleep duration with prevalent diabetes: The Hispanic Community Health Study/Study of Latinos (HCHS/SOL). J Diabetes. 8(3):387–397
McEvoy RD, Antic NA, Heeley E, Luo Y, Ou Q, Zhang X et al (2016) CPAP for prevention of cardiovascular events in obstructive sleep apnea. N Engl J Med. 375(10):919–931
Sánchez-de-la-Torre M, Sánchez-de-la-Torre A, Bertran S, Abad J, Duran-Cantolla J, Cabriada V et al (2019) Effect of obstructive sleep apnea and its treatment with CPAP on the incidence of cardiovascular events in patients with acute coronary syndrome. Lancet Respir Med. [In Press]
Yu J, Zhou Z, McEvoy RD, Anderson CS, Rodgers A, Perkovic V et al (2017) Association of positive airway pressure with cardiovascular events and death in adults with sleep apnea: a systematic review and meta-analysis. JAMA. 318(2):156–166
Labarca G, Dreyse J, Drake L, Jorquera J, Barbe F (2020) Efficacy of continuous positive airway pressure (CPAP) in the prevention of cardiovascular events in patients with obstructive sleep apnea: systematic review and meta-analysis. Sleep Med Rev. 52:101312
Author information
Authors and Affiliations
Contributions
Study design and ISRCTN register: G.L., J.J. Data analysis: J.D., F.L., C.S., A.S., F.R. Interpretation of the results: G.L., J.D., A.S., F.R., J.J. Manuscript preparation: G.L., J.J., A.S., F.R., J.D. Manuscript revision, editing, and approval: G.L., J.D., F.L., C.S., J.J. All authors approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Study register
ISRCTN62293645
Ethical approval
All procedures performed in this study were in accordance with the ethical standards of the institutional and/or national research committee from Clinica Las Condes, IRB: 00008758, Santiago, Chile, and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the prospective cohort included in the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(DOCX 17 kb)
Rights and permissions
About this article
Cite this article
Labarca, G., Dreyse, J., Salas, C. et al. Risk of mortality among patients with moderate to severe obstructive sleep apnea and diabetes mellitus: results from the SantOSA cohort. Sleep Breath 25, 1467–1475 (2021). https://doi.org/10.1007/s11325-020-02283-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-020-02283-y