Abstract
Introduction
Hutchinson-Gilford Progeria Syndrome (HGPS) is an extremely rare genetic disorder. HGPS children present a high incidence of cardiovascular complications along with altered metabolic processes and an accelerated aging process. No metabolic biomarker is known and the mechanisms underlying premature aging are not fully understood.
Objectives
The present work aims to evaluate the metabolic alterations in HGPS using high resolution mass spectrometry.
Methods
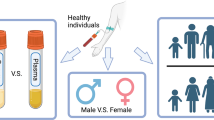
The present study analyzed plasma from six HGPS patients of both sexes (7.7 ± 1.4 years old; mean ± SD) and eight controls (8.6 ± 2.3 years old) by LC–MS/MS in high-resolution non-targeted metabolomics (Q-Exactive Plus). Targeted metabolomics was used to validate some of the metabolites identified by the non-targeted method in a triple quadrupole (TSQ-Quantiva).
Results
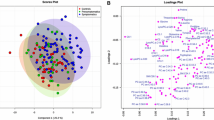
We found several endogenous metabolites with statistical differences between control and HGPS children. Multivariate statistical analysis showed a clear separation between groups. Potential novel metabolic biomarkers were identified using the multivariate area under ROC curve (AUROC) based analysis, showing an AUC value higher than 0.80 using only two metabolites, and tending to 1.00 when increasing the number of metabolites in the AUROC model. Taken together, changed metabolic pathways involve sphingolipids, amino acids, and oxidation of fatty acids, among others.
Conclusion
Our data show significant alterations in cellular energy use and availability, in signal transduction, and lipid metabolites, adding new insights on metabolic alterations associated with premature aging and suggesting novel putative biomarkers.






Similar content being viewed by others
References
Adam, B. W., Lim, T. H., Hall, E. M., & Hannon, W. H. (2009). Preliminary proficiency testing results for succinylacetone in dried blood spots for newborn screening for tyrosinemia type I. Clinical Chemistry, 55(12), 2207–2213. https://doi.org/10.1373/clinchem.2009.133819.
Adams, S. H. (2011). Emerging perspectives on essential amino acid metabolism in obesity and the insulin-resistant state. Advances in nutrition, 2(6), 445–456. https://doi.org/10.3945/an.111.000737.
Bahado-Singh, R. O., Ertl, R., Mandal, R., Bjorndahl, T. C., Syngelaki, A., Han, B., et al. (2014). Metabolomic prediction of fetal congenital heart defect in the first trimester. American Journal of Obstetrics and Gynecology, 211(3), 240.e1–240.e14. https://doi.org/10.1016/j.ajog.2014.03.056.
Bonomini, F., Rodella, L. F., & Rezzani, R. (2015). Metabolic syndrome, aging and involvement of oxidative stress. Aging and Disease, 6(2), 109–120. https://doi.org/10.14336/AD.2014.0305.
Bouchard, C. (2015). Exercise genomics—a paradigm shift is needed: a commentary. British Journal of Sports Medicine, 49(23), 1492–1496. https://doi.org/10.1136/bjsports-2015-095294.
Carneiro, G., Radcenco, A. L., Evaristo, J., & Monnerat, G. (2019). Novel strategies for clinical investigation and biomarker discovery: a guide to applied metabolomics. Hormone molecular biology and clinical investigation. https://doi.org/10.1515/hmbci-2018-0045.
Cheng, S., Larson, M. G., McCabe, E. L., Murabito, J. M., Rhee, E. P., Ho, J. E., et al. (2015). Distinct metabolomic signatures are associated with longevity in humans. Nat Commun, 6, 6791. https://doi.org/10.1038/ncomms7791.
Crawford, S. O., Hoogeveen, R. C., Brancati, F. L., Astor, B. C., Ballantyne, C. M., Schmidt, M. I., et al. (2010). Association of blood lactate with type 2 diabetes: the Atherosclerosis Risk in Communities Carotid MRI Study. International Journal of Epidemiology, 39(6), 1647–1655. https://doi.org/10.1093/ije/dyq126.
Cyr, D., Giguère, R., Villain, G., Lemieux, B., & Drouin, R. (2006). A GC/MS validated method for the nanomolar range determination of succinylacetone in amniotic fluid and plasma: an analytical tool for tyrosinemia type I. Journal Chromatography B Analytical Technologies Biomedical Life Sciences, 832(1), 24–29. https://doi.org/10.1016/j.jchromb.2005.12.007.
Dahse, R., Fiedler, W., & Ernst, G. (1997). Telomeres and telomerase: biological and clinical importance. Clinical Chemistry, 43(5), 708–714.
Dietzen, D. J., Bennett, M. J., Lo, S. F., Grey, V. L., & Jones, P. M. (2016). Dried Blood Spot Reference Intervals for Steroids and Amino Acids in a Neonatal Cohort of the National Children’s Study. Clinical Chemistry, 62(12), 1658–1667. https://doi.org/10.1373/clinchem.2016.263434.
Eriksson, M., Brown, W. T., Gordon, L. B., Glynn, M. W., Singer, J., Scott, L., et al. (2003). Recurrent de novo point mutations in lamin A cause Hutchinson-Gilford progeria syndrome. Nature, 423(6937), 293–298. https://doi.org/10.1038/nature01629.
Gordon, L. B., Kleinman, M. E., Miller, D. T., Neuberg, D. S., Giobbie-Hurder, A., Gerhard-Herman, M., et al. (2012). Clinical trial of a farnesyltransferase inhibitor in children with Hutchinson–Gilford progeria syndrome. Proceedings of the National Academy of Sciences, 109(41), 16666–16671. https://doi.org/10.1073/pnas.1202529109.
Gordon, L. B., Shappell, H., Massaro, J., D’Agostino, R. B., Brazier, J., Campbell, S. E., et al. (2018). Association of lonafarnib treatment vs no treatment with mortality rate in patients with hutchinson-gilford progeria syndrome. JAMA, 319(16), 1687–1695. https://doi.org/10.1001/jama.2018.3264.
Hennekam, R. C. (2006). Hutchinson-Gilford progeria syndrome: review of the phenotype. American journal of medical genetics Part A, 140(23), 2603–2624. https://doi.org/10.1002/ajmg.a.31346.
Houten, S. M., & Wanders, R. J. (2010). A general introduction to the biochemistry of mitochondrial fatty acid β-oxidation. Journal of Inherited Metabolic Disease, 33(5), 469–477. https://doi.org/10.1007/s10545-010-9061-2.
Houtkooper, R. H., Argmann, C., Houten, S. M., Cantó, C., Jeninga, E. H., Andreux, P. A., et al. (2011). The metabolic footprint of aging in mice. Scientific Reports, 1, 134. https://doi.org/10.1038/srep00134.
Katz, D. H., & Gerszten, R. E. (2018). A role for branched-chain amino acids in the pathophysiology of diabetes: using data to guide discovery. Clinical Chemistry, 64(8), 1250–1251. https://doi.org/10.1373/clinchem.2017.273516.
Kenyon, C. J. (2010). The genetics of ageing. Nature, 464(7288), 504–512. https://doi.org/10.1038/nature08980.
McClintock, D., Ratner, D., Lokuge, M., Owens, D. M., Gordon, L. B., Collins, F. S., et al. (2007). The mutant form of lamin A that causes Hutchinson–Gilford progeria is a biomarker of cellular aging in human skin. PLoS ONE, 2(12), e1269. https://doi.org/10.1371/journal.pone.0001269.
Merideth, M. A., Gordon, L. B., Clauss, S., Sachdev, V., Smith, A. C., Perry, M. B., et al. (2008). Phenotype and course of Hutchinson-Gilford progeria syndrome. New England Journal of Medicine, 358(6), 592–604. https://doi.org/10.1056/NEJMoa0706898.
Mihalik, S. J., Goodpaster, B. H., Kelley, D. E., Chace, D. H., Vockley, J., Toledo, F. G., et al. (2010). Increased levels of plasma acylcarnitines in obesity and type 2 diabetes and identification of a marker of glucolipotoxicity. Obesity (Silver Spring), 18(9), 1695–1700. https://doi.org/10.1038/oby.2009.510.
Monnerat, G., Seara, F. A. C., Evaristo, J. A. M., Carneiro, G., Evaristo, G. P. C., Domont, G., et al. (2018). Aging-related compensated hypogonadism: Role of metabolomic analysis in physiopathological and therapeutic evaluation. The Journal of Steroid Biochemistry and Molecular Biology. https://doi.org/10.1016/j.jsbmb.2018.05.005.
Nguyen, D., Samson, S. L., Reddy, V. T., Gonzalez, E. V., & Sekhar, R. V. (2013). Impaired mitochondrial fatty acid oxidation and insulin resistance in aging: novel protective role of glutathione. Aging Cell, 12(3), 415–425. https://doi.org/10.1111/acel.12073.
Noland, R. C., Koves, T. R., Seiler, S. E., Lum, H., Lust, R. M., Ilkayeva, O., et al. (2009). Carnitine insufficiency caused by aging and overnutrition compromises mitochondrial performance and metabolic control. Journal of Biological Chemistry, 284(34), 22840–22852. https://doi.org/10.1074/jbc.M109.032888.
North, B. J., & Sinclair, D. A. (2012). The intersection between aging and cardiovascular disease. Circulation Research, 110(8), 1097–1108. https://doi.org/10.1161/CIRCRESAHA.111.246876.
Park, S. K., & Shin, O. S. (2017). Metformin alleviates ageing cellular phenotypes in Hutchinson-Gilford progeria syndrome dermal fibroblasts. Experimental Dermatology, 26(10), 889–895. https://doi.org/10.1111/exd.13323.
Pluskal, T., Castillo, S., Villar-Briones, A., & Oresic, M. (2010). MZmine 2: modular framework for processing, visualizing, and analyzing mass spectrometry-based molecular profile data. BMC Bioinformatics, 11, 395. https://doi.org/10.1186/1471-2105-11-395.
Prakash, A., Gordon, L. B., Kleinman, M. E., Gurary, E. B., Massaro, J., D’Agostino, R., et al. (2018). Cardiac abnormalities in patients with Hutchinson–Gilford progeria syndrome. JAMA Cardiology, 3(4), 326–334. https://doi.org/10.1001/jamacardio.2017.5235.
Rajalahti, T., Lin, C., Mjøs, S. A., & Kvalheim, O. M. (2016). Changes in serum fatty acid and lipoprotein subclass concentrations from prepuberty to adulthood and during aging. Metabolomics, 12, 51. https://doi.org/10.1007/s11306-016-0968-y.
Rosenbloom, A. L., Kappy, M. S., DeBusk, F. L., Francis, G. L., Philpot, T. J., & Maclaren, N. K. (1983). Progeria: insulin resistance and hyperglycemia. Journal of Pediatrics, 102(3), 400–402.
Thompson Legault, J., L. Strittmatter, J. Tardif, R. Sharma, V. Tremblay-Vaillancourt, C. Aubut, G. Boucher, C. B. Clish, D. Cyr, C. Daneault, P. J. Waters, L. Vachon, C. Morin, C. Laprise, J. D. Rioux, V. K. Mootha, C. Des Rosiers, and LSFC Consortium. (2015). A metabolic signature of mitochondrial dysfunction revealed through a monogenic form of Leigh syndrome. Cell Reports, 13(5), 981–989. https://doi.org/10.1016/j.celrep.2015.09.054.
Wang, T. J., Larson, M. G., Vasan, R. S., Cheng, S., Rhee, E. P., McCabe, E., et al. (2011). Metabolite profiles and the risk of developing diabetes. Nature Medicine, 17(4), 448–453. https://doi.org/10.1038/nm.2307.
Wishart, D. S., Jewison, T., Guo, A. C., Wilson, M., Knox, C., Liu, Y., et al. (2013). HMDB 3.0–The Human Metabolome Database in 2013. Nucleic Acids Res, 41, D801–D807. https://doi.org/10.1093/nar/gks1065.
Xia, J., & Wishart, D. S. (2016). Using MetaboAnalyst 3.0 for Comprehensive Metabolomics Data Analysis. Current Protocols in Bioinformatics, 55, 14.10.1–14.10.91. https://doi.org/10.1002/cpbi.11.
Xu, J., Jiao, K., Liu, X., Sun, Q., Wang, K., Xu, H., et al. (2018). Omi/HtrA2 participates in age-related autophagic deficiency in rat liver. Aging Disease, 9(6), 1031–1042. https://doi.org/10.14336/AD.2018.0221.
Yu, M., Sun, S., Yu, J., Du, F., Zhang, S., Yang, W., et al. (2018). Discovery and validation of potential serum biomarkers for pediatric patients with congenital heart diseases by metabolomics. Journal of Proteome Research . https://doi.org/10.1021/acs.jproteome.8b00466.
Yu, Z., Zhai, G., Singmann, P., He, Y., Xu, T., Prehn, C., et al. (2012). Human serum metabolic profiles are age dependent. Aging Cell, 11(6), 960–967. https://doi.org/10.1111/j.1474-9726.2012.00865.x.
Acknowledgements
We are grateful to The Progeria Research Foundation for the availability of plasma samples, to Edna Aleixo from the Federal University of Rio de Janeiro for assistance with the importation process and to the Laboratório de Apoio ao Desenvolvimento Tecnológico (LADETEC) of the Chemistry Institute of the Federal University of Rio de Janeiro for providing high quality infrastructure for the LC–MS analysis.
Funding
This work was funded by the Ministry of Health (DECIT), the Brazilian National Research Council (CNPq), the Carlos Chagas Filho Rio de Janeiro State Research Foundation (FAPERJ) and National Institute of Science and Technology for Regenerative Medicine.
Author information
Authors and Affiliations
Contributions
GM and ACCC conceptualized the study and wrote the manuscript; GM, CGMS, JAME, GPCE, FCSN, GC, GBD, LM, ACCC acquired and analyzed the data; VOC, GBD, FCSN, ACCC critically revised the study and the manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Monnerat, G., Evaristo, G.P.C., Evaristo, J.A.M. et al. Metabolomic profiling suggests systemic signatures of premature aging induced by Hutchinson–Gilford progeria syndrome. Metabolomics 15, 100 (2019). https://doi.org/10.1007/s11306-019-1558-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11306-019-1558-6