Abstract
Purpose
Successful in vitro transplantation of spermatogonial stem cells (SSCs) demands effective culture systems for SSCs proliferation and differentiation. Natural extracellular matrix (ECM) creates a microenvironment suitable for culture of stem cells. In the present study, we intended to assess the capability of the porous scaffold consisting of hyaluronic acid (HA), chitosan, and decellularized testicular matrix (DTM) as a proper niche for SSCs seeding.
Methods
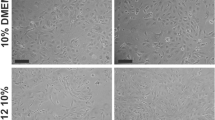
The testes of four NMRI mice were extracted for further detergent-based decellularization process. We isolated, cultured, and clarified neonate mouse SSC, and a three-dimensional scaffold was prepared for SSCs culture. The loaded SSCs and hydrogel-based scaffold were investigated by several studies including scanning electron microscopy (SEM), 4′,6-diamidino-2-phenylindole (DAPI), 3-[4, 5-dimethyl (thiazol-2yl)-3,5diphenyl] tetrazolium bromide (MTT), Acridine orange, and Immunohistochemistry (IHC) staining.
Results
The efficiency of decellularization process was confirmed by DAPI, hematoxylin and eosin (H&E), and Masson’s Trichrome staining. Acridine orange also depicted SSCs proliferation and viability. SEM approved the preservation of ECM components and also showed complex, coiled, and tubular seminiferous tubules, with intact and condensed collagenous form of the tunica albuginea. MTT test also revealed the scaffold’s non-toxicity. Expression of PLZF, TP1, and TEKT1 markers also verified the capacity of SSCs proliferation on a cogel scaffold.
Conclusion
In conclusion, cogel scaffold consisting of DTM, HA, and chitosan may provide the supporting layer for in vitro SSC differentiation and proliferation.








Similar content being viewed by others
References
Kargar-Abarghouei E, Vojdani Z, Hassanpour A, Alaee S, Talaei-Khozani T (2018) Characterization, recellularization, and transplantation of rat decellularized testis scaffold with bone marrow-derived mesenchymal stem cells. Stem Cell Res Ther 9(1):1–16
Del Vento F, Vermeulen M, De Michele F, Giudice MG, Poels J, Des Rieux A, Wyns C (2018) Tissue engineering to improve immature testicular tissue and cell transplantation outcomes: one step closer to fertility restoration for prepubertal boys exposed to gonadotoxic treatments. J Mol Sci 19(1):286
George B, Lal N, Damodaran JR, Suchithra TV (2020) Tissue engineering and regenerative medicines: an interdisciplinary understanding. In: Patra J, Shukla A, Das G (eds) Advances in pharmaceutical biotechnology. Springer, Singapore
Jahanbani Y, Davaran S, Ghahremani-Nasab M, Aghebati-Maleki L, Yousefi M (2020) Scaffold-based tissue engineering approaches in treating infertility. Life Sci 240:117066
Sabetkish S, Kajbafzadeh AM, Sabetkish N, Khorramirouz R, Akbarzadeh A, Seyedian SL, Pasalar P, Orangian S, Beigi RSH, Aryan Z (2015) Whole-organ tissue engineering: decellularization and recellularization of three-dimensional matrix liver scaffolds. J Biomed Mater Res A 103(4):1498–1508
Li H, Liu S, Wu S, Li L, Ge R, Cheng CY (2020) Bioactive fragments of laminin and collagen chains: lesson from the testis. Reproduct 159(3):111–123
Fayomi AP, Orwig KE (2018) Spermatogonial stem cells and spermatogenesis in mice, monkeys and men. Stem Cell Res 29:207–214
Yang Y, Lin Q, Zhou C, Li Q, Li Z, Cao Z, Liang J, Li H, Mei J, Zhang Q (2020) A testis-derived hydrogel as an efficient feeder-free culture platform to promote mouse spermatogonial stem cell proliferation and differentiation. Front Cell Dev Biol 8:250
Huang Y, Seitz D, König F, Müller PE, Jansson V, Klar RM (2019) Induction of articular chondrogenesis by chitosan/hyaluronic-acid-based biomimetic matrices using human adipose-derived stem cells. Int J Mol Sci 20(18):4487
Yoo HS, Lee EA, Yoon JJ, Park TG (2005) Hyaluronic acid modified biodegradable scaffolds for cartilage tissue engineering. Biomaterials 26(14):1925–1933
Wang M, Li W, Zhang Y, Tian W, Wang H (2017) Comparison of intra-arterial and subcutaneous testicular hyaluronidase injection treatments and the vascular complications of hyaluronic acid filler. Dermatol Surg 43(2):246–254
Drury JL, Mooney DJ (2003) Hydrogels for tissue engineering: scaffold design variables and applications. Biomaterials 24(24):4337–4351
Gharenaz NM, Movahedin M, Mazaheri Z (2020) Three-dimensional culture of mouse spermatogonial stem cells using a decellularised testicular scaffold. Cell J (Yakhteh) 21(4):410
Mirzapour T, Movahedin M, Tengku Ibrahim T, Koruji M, Haron A, Nowroozi M, Rafieian S (2012) Effects of basic fibroblast growth factor and leukaemia inhibitory factor on proliferation and short-term culture of human spermatogonial stem cells. Andrology 44:41–55
Mohaqiq M, Movahedin M, Mazaheri Z, Amirjannati N (2019) In vitro transplantation of spermatogonial stem cells isolated from human frozen–thawed testis tissue can induce spermatogenesis under 3-dimensional tissue culture conditions. Biol Res 52(1):16
Vermeulen M, Del Vento F, De Michele F, Poels J, Wyns C (2018) Development of a cytocompatible scaffold from pig immature testicular tissue allowing human sertoli cell attachment, proliferation and functionality. Int J Mol Sci 19(1):227
Baert Y, Stukenborg J-B, Landreh M, De Kock J, Jörnvall H, Söder O, Goossens E (2015) Derivation and characterization of a cytocompatible scaffold from human testis. Hum Reprod 30(2):256–267
Sabetkish S, Kajbafzadeh A-M, Sabetkish N (2020) Recellularization of testicular feminization testis in C57bl6 as a natural bioreactor for creation of cellularized seminiferous tubules: an experimental study. Cell Tissue Bank. https://doi.org/10.1007/s10561-020-09877-6
Reda A, Hou M, Landreh L, Kjartansdóttir KR, Svechnikov K, Soder O, Stukenborg J-B (2014) In vitro spermatogenesis—optimal culture conditions for testicular cell survival, germ cell differentiation, and steroidogenesis in rats. Front Endocrinol 5:21
Reuter K, Ehmcke J, Stukenborg J-B, Simoni M, Damm OS, Redmann K, Schlatt S, Wistuba J (2014) Reassembly of somatic cells and testicular organogenesis in vitro. Tissue Cell 46(1):86–96
Stukenborg J-B, Schlatt S, Simoni M, Yeung C-H, Elhija MA, Luetjens CM, Huleihel M, Wistuba J (2009) New horizons for in vitro spermatogenesis? An update on novel three-dimensional culture systems as tools for meiotic and post-meiotic differentiation of testicular germ cells. Mol Hum Reprod 15(9):521–529
Pandit AH, Mazumdar N, Ahmad S (2019) Periodate oxidized hyaluronic acid-based hydrogel scaffolds for tissue engineering applications. Int J Biol Macromol 137:853–869
Ashouri Movassagh S, Banitalebi Dehkordi M, Koruji M, Pourmand G, Farzaneh P, Ashouri Movassagh S, Jabari A, Samadian A, Khadivi F, Abbasi M (2019) In vitro spermatogenesis by three-dimensional culture of spermatogonial stem cells on decellularized testicular matrix. Galen Med J 8:1565
Ding K, Yang Z, Zhang YL, Xu JZ (2013) Injectable thermosensitive chitosan/β-glycerophosphate/collagen hydrogel maintains the plasticity of skeletal muscle satellite cells and supports their in vivo viability. Cell Biol Int 37(9):977–987
Gül M, Dong L, Wang D, Diri MA, Andersen CY (2020) Surrogate testes: allogeneic spermatogonial stem cell transplantation within an encapsulation device may restore male fertility. Med Hypotheses 139:109634
Huang D, Wang R, Yang S (2016) Cogels of hyaluronic acid and acellular matrix for cultivation of adipose-derived stem cells: potential application for vocal fold tissue engineering. BioMed Res Int 18:1–10
Nasiri B, Mashayekhan S (2017) Fabrication of porous scaffolds with decellularized cartilage matrix for tissue engineering application. Biology 48:39–46
Baert Y, De Kock J, Alves-Lopes JP, Söder O, Stukenborg J-B, Goossens E (2017) Primary human testicular cells self-organize into organoids with testicular properties. Stem Cell Rep 8(1):30–38
Baert Y, Rombaut C, Goossens E (2019) Scaffold-based and scaffold-free testicular organoids from primary human testicular cells. Methods Mol Biol 1576:283–290
Azizi H, Koruji M, Skutella T (2020) Comparison of PLZF gene expression between pluripotent stem cells and testicular germ cells. Cell J (Yakhteh) 22(1):60–65
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The author(s) declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Naeemi, S., Eidi, A., Khanbabaee, R. et al. Differentiation and proliferation of spermatogonial stem cells using a three-dimensional decellularized testicular scaffold: a new method to study the testicular microenvironment in vitro. Int Urol Nephrol 53, 1543–1550 (2021). https://doi.org/10.1007/s11255-021-02877-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-021-02877-9