Abstract
It is important to examine normative age-related change in substance use risk factors across the lifespan, with research focusing on middle adulthood particularly needed. The current study examined time-varying associations between depressive symptoms and alcohol, cigarette, and marijuana use from modal ages 35 to 55 in a national sample of US adults, overall and by sex. Data were obtained from 11,147 individuals in the longitudinal Monitoring the Future study. Participants were in 12th grade (modal age 18) in 1976–1982 and (for the data reported in this study) were surveyed again at modal ages 35 (in 1993–1999), 40, 45, 50, and 55 (in 2013–2019). Weighted time-varying effect modeling was used to examine age-related change in associations among depressive symptoms, any and heavy use of cigarettes, alcohol, and marijuana. Across midlife, greater depressive symptoms were associated with decreased odds of any alcohol use during the 40 s and 50 s, but with increased odds of binge drinking from ages 35–40, and—at most ages—any and pack + cigarette use and any and frequent marijuana use. The association between depressive symptoms and substance use was generally similar for men and women. Results highlight the increased risk for binge drinking, smoking, and marijuana with higher levels of depressive symptoms and underscore the importance of screening and interventions for depressive symptoms and substance use in midlife.
Similar content being viewed by others
Introduction
Substance use can convey serious health, social, and legal consequences across the lifespan, making it a key target for prevention and intervention efforts (Patrick et al., 2021; Schulte & Hser, 2013). Substance use prevention research often has focused on younger age groups, while less work has focused on midlife (defined here as mid-thirties to mid-fifties). Midlife is characterized by unique patterns of both substance use and mental health factors (Deeken et al., 2020; Hoertel et al., 2015; Sutin et al., 2013).
Substance use and use disorders are among the greatest threats for adult morbidity and mortality (GBD, 2020; Zucker et al., 2016). The most prevalent substances used during midlife in the United States (U.S.) are alcohol, cigarettes, and marijuana (Patrick et al., 2022a). Heavy use of these substances is of particular concern, as it leads to increased risk of adverse consequences including major health conditions (e.g., cancer, heart disease, etc.), accidents, injury, violence, and incarceration (NIAAA, 2015; NIDA, 2020; SAMHSA, 2020; Volkow et al., 2014). Among U.S. adults aged 55 in 2021, prevalence estimates were 21.5% for binge drinking, 9.5% for daily cigarette use, and 4% for daily marijuana use (Patrick et al., 2022a). There are significant age-related changes in substance use across midlife (Britton et al., 2015; Patrick et al., 2021, 2022a), but existing studies have not examined alcohol, cigarette, and marijuana use among the same individuals over time. National estimates of age-related change in alcohol, cigarette, and marijuana use—including heavy use—across midlife for the same sample of individuals would hold constant possible differences resulting from either cohort or period effects.
Midlife is also characterized by high rates of depressive symptoms and life dissatisfaction (Blanchflower & Graham, 2020; Gondek et al., 2022; Reeves et al., 2011); depressive symptoms vary across this period with some individuals showing increased symptoms (Villarroel & Terlizzi, 2020). Substance use rates are consistently higher among adults with versus without mental illness (SAMHSA, 2022), and reciprocal connections have been observed between substance use and depression (Garey et al., 2020; Han & Palamar, 2018; Hasin & Kilcoyne, 2012; Hunt et al., 2020; Kessler, 2004) including during midlife (Blonigen et al., 2013). However, little is understood about normative age-related changes in associations between depressive symptoms and substance use across midlife, including the degree to which age-related changes may vary by substance. Research using national samples to examine plasticity in associations between depressive symptoms and substance use across midlife might help inform development of age-appropriate substance use interventions (Schulte & Hser, 2013).
There may be important sex differences in how links between depressive symptoms and substance use change during midlife. Women are more likely to experience depressive symptoms than men (Villarroel & Terlizzi, 2020). Men have historically had higher substance use prevalence rates than women (although such sex differences have decreased; Patrick et al., 2022a). Research indicates women may drink as a result of depressive symptoms, while men may experience depressive symptoms due to increased drinking (Brennan et al., 1993; Erol & Karpyak, 2015). Further, women may be more likely than men to smoke in order to regulate mood and in response to stress (NIDA, 2020). While evidence is mixed on the extent to which there may be sex-specific differences in associations between depressive symptoms and marijuana, sex differences in physiological responses to marijuana indicate women may experience more depressive-like symptoms in response to use than men (Calakos et al., 2017).
The current study examined time-varying associations between depressive symptoms and substance use (any and heavy use of alcohol, cigarettes, and marijuana) from modal ages 35 to 55 in a national sample of U.S. adults via three research aims: (1) describe age-related changes in depressive symptom and substance use prevalence; (2) examine age-related changes in associations between depressive symptoms and substance use; and (3) identify potential sex differences in changes in age-related associations.
Methods
Participants and Procedure
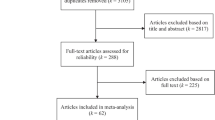
Data were obtained from the longitudinal component of the Monitoring the Future (MTF) study (for detailed methods, see Patrick et al., 2022a). MTF surveys new nationally representative samples of U.S. 12th grade students (modal age 18) each year (Miech et al., 2022). From each yearly sample, approximately 2450 individuals are selected for longitudinal follow-up which is randomized to begin one or two years after high school (i.e., ages 19 or 20; Patrick et al., 2022a). Six biennial follow-up surveys are collected between the ages of 19 and 30; thereafter, surveys are collected every five years (at ages modal 35, 40, 45, 50, 55).Footnote 1 The current study used data from the surveys at modal ages 35 to 55 (with an actual age range of 33 to 57). Participants were surveyed at age 18 in 1976–1982; age 35 data were collected in 1993–1999 and age 55 data in 2013–2019 using mailed questionnaires. Of the 16,783 respondents purposively selected from the noted 12th grade cohorts, 5369 (32.0%) did not respond at any of the relevant surveys (see the Statistical Analysis section below for attrition adjustments). An additional 15 respondents provided no valid depressive symptom data; 9 respondents provided no valid substance use data, and 243 respondents had missing covariate measure data, leaving 11,147 respondents (66.4% of 16,783) for analysis (see Supplement Fig. 1 for sample diagram and Supplement Appendix for sensitivity analysis).
Measures
Outcome Variables
Substance use measures were asked at each follow-up. For cigarette use, respondents were asked, “How frequently have you smoked cigarettes during the past 30 days?” with response options of not at all, < 1 cigarette/day, 1–5 cigarettes/day, about ½ pack/day, about 1 pack/day, about 1 ½ packs/day, and 2 or more packs/day. For alcohol use, respondents were asked, “On how many occasions (if any) have you had any alcoholic beverage to drink—more than just a few sips—during the last 30 days?” For marijuana use, respondents were asked, “On how many occasions (if any) have you used marijuana (weed, pot) or hashish (hash, hash oil) during the last 30 days?” Alcohol and marijuana items used the same response scale of 0 occasions, 1–2, 3–5, 6–9, 10–19, 20–39, and 40 + occasions. From these items, three measures were coded to indicate past 30-day prevalence of any use of cigarettes, alcohol, and marijuana. Heavy cigarette and marijuana use measures were also coded from the 30-day use measures: pack + cigarette use (1 + packs per day vs. not at all or < 1 cigarette/day); and frequent marijuana use (20 + occasions vs. 0–19 occasions). For heavy alcohol use, a separate measure assessed binge drinking. Respondents were asked, “Think back over the last two weeks. How many times have you had five or more drinks in a row?” with response options of none, once, twice, 3–5 times, 6–9 times, and 10 + times. A binge drinking indicator (any vs. none in the past two weeks) was coded. The use of a universal 5 + drink threshold for both men and women stems from the fact that data for this study were collected over a significant period of time, including years predating the now more commonly used biological sex-specific thresholds of 4 + /5 + drinks for women and men (Patrick & Terry-McElrath, 2021).
Independent Variable
Depressive symptoms were measured at each follow-up using four individual items (α = 0.82) derived from the Bentler Medical and Psychological Functioning Inventory’s Depression scale (Newcomb et al., 1981, 1986): “Life often seems meaningless,” “I enjoy life as much as anyone,” “The future often seems hopeless,” and “It feels good to be alive” with response options of 1 = disagree, 2 = mostly disagree, 3 = neither, 4 = mostly agree, 5 = agree. The items “I enjoy life as much as anyone” and “it feels good to be alive” were reverse-coded so that higher values indicated higher depressive symptoms. After reverse coding, the mean of the four items was calculated (reliability of 0.72 as reported by Newcomb et al., 1986). In the current study, missing data on up to 3 items were allowed; however, out of all wave-specific responses included in analyses, 99.9% of respondents provided valid data for all items. The resulting measure is an indication of depressive symptoms, not a clinical diagnosis of depression. However, it has been used by the MTF study to enable consistent measurement of depressive symptoms across age (Kreski et al., 2021; Maslowsky et al., 2013, 2014).
Covariates
Covariates were selected based on factors associated with important differences in substance use and depressive symptoms during midlife (Davison et al., 2019; Dunlop et al., 2003; Villarroel & Terlizzi, 2020). At age 18, respondents provided data on sex (male, female) and racial/ethnic identity (coded as Black, Hispanic, White, or Other [combined due to sample size limitations]). Based on responses provided at ages 19–30, respondents were coded as ever having graduated from a 4-year college versus not. Cohort (year of 12th grade survey) was coded as a 3-level categorical measure (1976–1977, 1978–1979, and 1980–1982). Age in years was coded based on age reported during the 12th grade survey. For example, if a respondent reported being 17 years 2 months of age at the 12th grade survey, at the age 35 survey (occurring 17 years after the 12th grade survey), they were coded as age 34 and 2 months. The resulting measure ranged from 30 years 10 months to 58 years 2 months (see Supplement Fig. 2). Integer ages with fewer than 10 observations (30, 31, 32, and 58) were excluded from analyses, leaving 43,059 observations from 11,147 respondents with an age range of 33 to 57 (mean waves per respondent = 3.86; range 1–5).
Statistical Analysis
Analyses used SAS version 9.4 (SAS Institute Inc., Cary, NC). Descriptive estimates were obtained using SURVEYFREQ and SURVEYMEANS procedures, clustering by respondent. Time-varying effect modeling (TVEM) was used to model continuous change across age in years. TVEM examines associations over continuous time without parametric assumptions (e.g., linear, quadratic, etc.); the only assumption is that change over time happens in a smooth manner (Lanza et al., 2014; Tan et al., 2012). Models used the logistic option in the %WeightedTVEM macro (Dziak et al., 2017) and included attrition weights calculated for age 55 participation based on extensive information available from 12th grade measures. Coefficient functions were estimated as a series of splines, incorporating data from neighboring time points. Analyses used the default of 100 time points (here, continuous age in years) for plotting estimated coefficients and confidence bands (Li et al., 2017). Because of the large number of estimates across age, results are presented in figures showing point estimates and confidence intervals by age. Model fit was based on pseudo likelihood information criteria (pseudo-Akaike information criterion, pseudo-Bayesian information criterion).
For research aim (RA) 1 (modeling descriptive age-related change in depressive symptom and substance use prevalence), descriptive estimates of mean depressive symptoms and substance use prevalence were modeled and reported in figures with 95% point-wise confidence intervals (CI) across age in years. For RA 2 (modeling age-related change in associations between depressive symptoms and substance use outcomes), results are presented as odds ratios (ORs) or adjusted odds ratios (AORs) with 95% point-wise confidence intervals. Simple unadjusted models included only mean depressive symptoms and one substance use outcome. Adjusted regression models also included sex, race/ethnicity, college status, cohort, and other substance use. For example, in the adjusted depressive symptoms and alcohol prevalence model, covariates included cigarette and marijuana prevalence. In the adjusted depressive symptoms and binge drinking model, covariates included pack + cigarette and frequent marijuana use. By including the other two substance use measures in the models as covariates, obtained adjusted estimates are better able to parse out the specific association between depressive symptoms and the specific substance use outcome, versus associations between depressive symptoms and substance use in general. For RA 3 (examining differences in age-related association change by sex), a sex \(\times\) depressive symptoms interaction term was included in each adjusted model.
Results
At the respondent level, the weighted analytic sample was 49.7% male; racial/ethnic distribution was 14.2% Black, 3.4% Hispanic, 77.7% White, and 4.7% other racial/ethnic identity. Graduating from a 4-year college between ages 19–30 was reported by 35.2% of respondents. Across data collection waves, overall mean depressive symptoms was 1.64 (SE 0.01). Past 30-day prevalence levels were 20.4% for cigarettes, 65.4% for alcohol, and 8.8% for marijuana. Heavy use prevalence levels were 10.1% for pack + cigarette use, 21.4% for binge drinking, and 2.6% for frequent marijuana use.
RA 1: Age-Related Change in Depressive Symptoms and Substance Use
Depressive Symptoms
Mean depressive symptoms evidenced very little change across age, ranging from 1.68 at age 33 to 1.58 at age 57 (figure not shown).
Cigarette Use
Figure 1 presents substance use outcome prevalence by age. Cigarette prevalence showed generally steady declines across age, decreasing from a high of 26.8% at age 33 to a low of 12.8% at age 57. Pack + cigarette use similarly decreased from a high of 13.2% at ages 34 and 35 to a low of 5.5% at age 57.
Alcohol Use
The highest prevalence levels for alcohol use (between 67.0 and 67.6%) were observed at ages 33 and 50, 51; prevalence was lowest at age 57 (61.2%). Binge drinking evidenced generally steady but minor declines across age; prevalence was highest at age 33 (22.9%) and lowest at age 57 (18.9%).
Marijuana Use
Marijuana prevalence was highest at ages 35 and 56, 57 (10.4% or higher) and lowest at ages 46–48 (7.2%). Frequent use prevalence showed relatively little change but was highest at ages 56 and 57, peaking at 3.9%.
RA 2: Age-Related Change in Associations Between Depressive Symptoms and Substance Use
Figure 2 presents simple unadjusted depressive symptom and substance use associations; adjusted associations are presented in Fig. 3.
Cigarette Use
In simple unadjusted models, higher depressive symptoms were associated with higher odds of any cigarette use through age 56 and higher odds of pack + cigarette use across midlife. After controlling for covariates, associations remained significant and positive through age 56 for any use, and across all ages for pack + use, reaching AOR 1.39 [1.26, 1.53] at ages 51 and 52 for any cigarette use, and AOR 1.47 [1.30, 1.65] for pack + use at ages 53–54.
Alcohol Use
In unadjusted models, depressive symptoms were not associated with the odds of any alcohol use from ages 33–46; from ages 47–56, higher depressive symptoms were associated with lower use (ORs ranging from 0.93 [95% CI 0.87, 0.99] to 0.83 [0.70, 0.99]). In the adjusted model, negative associations between depressive symptoms and any alcohol use were observed from ages 41–57 (AORs ranging from 0.93 [0.87, 0.99] to 0.71 [0.56, 0.89]).
Regarding depressive symptoms and binge drinking, the unadjusted association peaked at age 37 (OR 1.32 [1.22, 1.43]) and then lessened through age 54 when it became non-significant. After controlling for covariates, depressive symptoms remained associated with higher adjusted odds of binge drinking only from ages 34–41, reaching AOR 1.19 [1.11, 1.28] at age 35.
Marijuana Use
In unadjusted models, higher depressive symptoms were associated with higher odds of any and frequent marijuana use across ages 33–57. After controlling for covariates, higher depressive symptoms were associated with higher odds of any marijuana use at ages 33–36 (peaking at AOR 1.33 [1.06, 1.67]) and 41–57 (peaking at AOR 1.50 [1.08, 2.09]). Adjusted associations with frequent marijuana use were observed at ages 33–35, 42–48, and 53–57, peaking at age 57 (AOR 1.93 [1.21, 3.09]).
RA 3: Interindividual Differences by Sex
No significant interactions between sex and depressive symptoms were observed for any or pack + cigarette use, any alcohol use, or any or frequent marijuana use. For binge drinking, the sex \(\times\) depressive symptoms interaction term was significant at ages 35–36 and 40–42 (AORs 0.85 [0.72, 0.99] to 0.85 [0.74, 0.98]), indicating depressive symptoms and binge drinking associations at the noted ages were stronger among women than men. When the binge drinking interaction model was re-run using 99% confidence intervals, no significant interaction was observed.
Discussion
In this national sample examining age-related change during midlife, we found that mean depressive symptoms were largely stable. However, there were important normative age-related changes in substance use prevalence and in depressive symptom/substance use associations. As has been found previously (Patrick et al., 2021, 2022a), age-related changes in use varied by substance. Any and pack + cigarette use declined across midlife. Any alcohol use oscillated between roughly 70% and 60%, but binge drinking declined steadily after age 35. Marijuana use decreased through the 40 s but rebounded somewhat by the mid-50 s.
The current study observed important differences between substances in the degree to which associations with depressive symptoms shifted across midlife. Depressive symptoms were consistently associated with greater odds of any and pack + cigarette use throughout midlife. This is consistent with existing research about the strong and persistent ties between depressive symptoms and smoking observed across age (Anda et al., 1990; Mendelsohn, 2012; Paperwalla et al., 2004).
Greater depressive symptoms were associated with increased odds of binge drinking during the mid-30 s but lower odds of any alcohol use during the mid-40 s and 50 s. Binge drinking is more prevalent during the mid-30 s than later midlife (Patrick et al., 2022a) and is a recognized risk factor for alcohol use disorder (AUD) (Esser et al., 2014). There are clear links between AUD and depressive symptoms (Boden & Fergusson, 2011). However, we also found evidence of associations between greater depressive symptoms and decreased alcohol use during the mid-40 s and 50 s. There are strong connections between alcohol use and social interaction in young adulthood (Orehek et al., 2020; Sayette et al., 2012), and qualitative research indicates that during midlife, both men and women who drink see alcohol as very important for relating with others and maintaining friendships (Kersey et al., 2022; Parke et al., 2018). In midlife, adults who do not drink may have fewer socializing opportunities; conversely, depressive symptoms may lead to less socializing and thus indirectly decrease the likelihood of alcohol use among moderate social drinkers. The fact that associations between depressive symptoms and alcohol use were more pronounced during later midlife may be based on drinking reasons. Among young adults, drinking reasons related to coping motives gained importance across age in differentiating alcohol risk (Patrick et al., 2017); by later midlife, social drinking and depressive symptoms may be more strongly associated. Additional research on age-related changes in drinking motives and reasons is relevant for understanding the connections between depressive symptoms and alcohol use.
For marijuana, greater depressive symptoms were generally associated with increased odds of any use and, to a lesser extent, frequent use across midlife. Inconsistent evidence for links between depressive symptoms and marijuana use have been found (Dierker et al., 2018; Harder et al., 2006); associations may depend on use motivations (Green & Ritter, 2000). Coping-related marijuana use reasons have been increasing among young adults (Patrick et al., 2019), and it will be important to examine if such findings also apply during midlife.
Overall, associations did not differ by sex. While prior research has found that women are more likely than men to experience depressive symptoms (Villarroel & Terlizzi, 2020), and sex-specific differences exist in the associations between depressive symptoms and alcohol, tobacco and marijuana use (Brennan et al., 1993; Calakos et al., 2017; Erol & Karpyak, 2015; NIDA, 2020), the current study found few sex differences. For both women and men, higher depressive symptoms were correlated with higher use, and associations appeared to vary across midlife in similar ways. There was some evidence that sex moderated age-related change in depressive symptom/binge drinking associations, with stronger associations among women at ages 35 and 40. Due to using the universal 5 + binge drinking definition (vs. biological sex-specific thresholds), the intoxication level associated with the binge drinking measure generally may have been higher for women than men, possibly exacerbating associations with depressive symptoms. Future research using sex-specific thresholds may be useful. Results underscore accumulating evidence about the closing alcohol use gender gap among U.S. drinkers (Keyes et al., 2008; White et al., 2015). Women are at elevated risk for several alcohol-related problems (Slade et al., 2016; White, 2020), including slower reductions in binge drinking (Hasin et al., 2019) and AUD prevalence across midlife (Jager et al., 2021). Given substance use effects on fertility, pregnancy, and breastfeeding—common issues among women in early midlife—understanding substance use among women in this age group is an important area for additional research (Zilberman, 2009).
Future research should examine the ongoing effects of the COVID-19 pandemic. The pandemic’s emergence in 2020 has been associated with significant change in both mental health and substance use (Imtiaz et al., 2021; Niedzwiedz et al., 2021). There are indications that among those in midlife, the pandemic was associated with historical increases in daily alcohol use (Patrick et al., 2022b). Several studies have noted pandemic-related increased substance use coping motives and use due to boredom and stress (Clare et al., 2021; Graupensperger et al., 2021; Jackson et al., 2021; McPhee et al., 2020; Patrick et al., 2022b); some studies have found indications of changes in drinking contexts (e.g., more drinking alone and at home; Patrick et al., 2022b). Individuals with mental health symptoms have reported more pandemic-related change in substance use (Eastman et al., 2021). The extent to which the global COVID-19 pandemic may have shifted levels of depressive symptoms, substance use, and their short- and long-term associations during midlife should be an active area for future research.
Implications for Prevention
Our results suggest depressive symptoms and substance use are not uncommon across midlife, thus it is important to continue universal efforts to prevent substance misuse and worsening mental health. Workplace health initiatives and employee assistance programs may be one avenue to provide public health messaging about these problems to individuals in middle age. Substance use and use disorders in adults are becoming increasingly common compared to previous generations and are expected to continue increasing (SAMHSA, 2020). Unfortunately, these disorders often go unrecognized or untreated due to stigma and age-related biases (Kuerbris et al., 2014). When adults seek care, they are more likely to do so from primary care and emergency department providers (Kuerbris et al., 2014). Universal screening in these settings paired with indicated referral and follow-up for both depressive symptoms and substance use in midlife are recommended given our findings. Furthermore, providers treating patients for depression should screen for substance use, and vice versa. These findings also highlight the importance of providing mental health and substance use treatment resources for the population, along with improved treatments for co-morbid substance use and depressive symptoms. Some transdiagnostic treatments exist (e.g., Unified Protocol [Barlow et al., 2017], Transdiagnostic Behavior Therapy [Gros, 2014]), and some disorder-specific treatments target co-morbid dysfunction (e.g., Cognitive Behavioral Therapy for Substance Use Disorders [DeMarce et al., 2014]). However, few treatment organizations have the capacity to serve dually diagnosed patients (McGovern et al., 2014). Given shifts in the population, the retirement and health care system—along with other services—may face increased strain as a growing number of older adults require comprehensive, integrated substance use disorder and mental health screening, assessment, and treatment if effective prevention mechanisms are not implemented.
Limitations
The current study’s findings are subject to limitations. The study was based on longitudinal follow-up of 12th grade students; those who dropped out prior to 12th grade were not able to participate. School drop-out is associated with higher depressive symptoms (Askeland et al., 2022) and substance use (Davis et al., 2022; Tice et al., 2017). Thus, the depressive symptom and substance use levels reported during midlife in the current study may underestimate total population levels. As noted previously, the measure of depressive symptoms used in the current study is not a clinical diagnosis, and we examined associations between depressive symptoms and only three substances (cigarettes, alcohol, and marijuana). Future research examining time-varying associations across midlife between clinical depression (possibly controlling for other mental health issues) and a wider range of substances (e.g., nicotine vaping, opioids, stimulants) is needed.
Conclusion
Across midlife, depressive symptoms were largely stable, while substance use levels exhibited meaningful age-related change. Associations between depressive symptoms and substance use varied by substance and age, but highlighted the increased risk for heavier alcohol use, cigarette use, and marijuana use that accompanied higher levels of depressive symptoms. Clinicians and those seeking to promote health among adults in midlife should be aware of the importance of monitoring depressive symptoms and substance use among both men and women.
Data Availability
Monitoring the Future Restricted-Use Panel Data are available through the National Addiction & HIV Data Archive program at https://www.icpsr.umich.edu/web/pages/NAHDAP/index.html.
Notes
A modest incentive is provided with the invitation for each survey; see Patrick et al. (2022a).
References
Anda, R. F., Williamson, D. F., Escobedo, L. G., Mast, E. E., Giovino, G. A., & Remington, P. L. (1990). Depression and the dynamics of smoking: A national perspective. JAMA, 264(12), 1541–1545. https://doi.org/10.1001/jama.1990.03450120053028
Askeland, K. G., Bøe, T., Sivertsen, B., Linton, S. J., Heradstveit, O., Nilsen, S. A., & Hysing, M. (2022). Association of depressive symptoms in late adolescence and school dropout. School Mental Health. Advance online publication. https://doi.org/10.1007/s12310-022-09522-5
Barlow, D. H., Farchione, T. J., Sauer-Zavala, S., Latin, H. M., Ellard, K. K., Bullis, J. R., Bentley, K. H., Boettcher, H. T., & Cassiello-Robbins, C. (2017). Unified protocol for transdiagnostic treatment of emotional disorders: Therapist guide (2nd ed.). Oxford University Press. https://doi.org/10.1093/med-psych/9780190685973.001.0001
Blanchflower, D. G., & Graham, C. L. (2020). The mid-life dip in well-being: Economists (who find it) versus psychologists (who don’t)! NBER Working Paper 26888. https://doi.org/10.3386/w26888
Blonigen, D. M., Burroughs, T., Haber, J. R., & Jacob, T. (2013). Psychiatric morbidity is linked to problem drinking in midlife among alcohol-dependent men: A co-twin control study. Journal of Studies on Alcohol and Drugs, 74(1), 136–140. https://doi.org/10.15288/jsad.2013.74.136
Boden, J. M., & Fergusson, D. M. (2011). Alcohol and depression. Addiction, 106(5), 906–914. https://doi.org/10.1111/j.1360-0443.2010.03351.x
Brennan, P. L., Moos, R. H., & Kim, J. Y. (1993). Gender differences in the individual characteristics and life contexts of late-middle-aged and older problem drinkers. Addiction, 88(6), 781–790. https://doi.org/10.1111/j.1360-0443.1993.tb02092.x.27
Britton, A., Ben-Shlomo, Y., Benzeval, M., Kuh, D., & Bell, S. (2015). Life course trajectories of alcohol consumption in the United Kingdom using longitudinal data from nine cohort studies. BMC Medicine, 13, 47. https://doi.org/10.1186/s12916-015-0273-z
Calakos, K. C., Bhatt, S., Foster, D. W., & Cosgrove, K. P. (2017). Mechanisms underlying sex differences in cannabis use. Current Addiction Reports, 4(4), 439–453. https://doi.org/10.1007/s40429-017-0174-7
Clare, P. J., Aiken, A., Yuen, W. S., Upton, E., Kypri, K., Degenhardt, L., Bruno, R., McCambridge, J., McBride, N., Hutchinson, D., Slade, T., Mattick, R., & Peacock, A. (2021). Alcohol use among young Australian adults in May-June 2020 during the COVID-19 pandemic: A prospective cohort study. Addiction, 116(12), 3398–3407. https://doi.org/10.1111/add.15599
Davis, C. N., Gizer, I. R., Lynskey, M. T., Statham, D. J., Health, A. C., Martin, N. G., & Slutske, W. S. (2022). Adolescent substance use and high school noncompletion: Exploring the nature of the relationship using a discordant twin design. Addiction. Advance online publication. https://doi.org/10.1111/add.15996
Davison, K. M., Lung, Y., Lin, S., Tong, H., Kobayashi, K. M., & Fuller-Thomson, E. (2019). Depression in middle and older adulthood: The role of immigration, nutrition, and other determinants of health in the Canadian longitudinal study on aging. BMC Psychiatry, 19(1), 329. https://doi.org/10.1186/s12888-019-2309-y
Deeken, F., Banaschewski, T., Kluge, U., & Rapp, M. A. (2020). Risk and protective factors for alcohol use disorders across the lifespan. Current Addiction Reports, 7, 245–251. https://doi.org/10.1007/s40429-020-00313-z
DeMarce, J. M., Gnys, M., Raffa, S. D., & Karlin, B. E. (2014). Cognitive behavioral therapy for substance use disorders among veterans: Therapist manual. U.S. Department of Veterans Affairs.
Dierker, L., Selya, A., Lanza, S., Li, R., & Rose, J. (2018). Depression and marijuana use disorder symptoms among current marijuana users. Addictive Behaviors, 76, 161–168. https://doi.org/10.1016/j.addbeh.2017.08.013
Dunlop, D. D., Song, J., Lyons, J. S., Manheim, L. M., & Chang, R. W. (2003). Racial/ethnic differences in rates of depression among preretirement adults. American Journal of Public Health, 93(11), 1945–1952. https://doi.org/10.2105/ajph.93.11.1945
Dziak, J. J., Li, R., & Wagner, A. T. (2017). Weighted TVEM SAS macro users’ guide (Version 2.6). The Methodology Center, Penn State. Retrieved January 13, 2023, from https://aimlab.psu.edu/wp-content/uploads/2020/02/WeightedTVEMUsersGuidev2.6-v5ung3.pdf
Eastman, M. R., Finlay, J. M., & Kobayashi, L. C. (2021). Alcohol use and mental health among older American adults during the early months of the COVID-19 pandemic. International Journal of Environmental Research and Public Health, 18(8), 4222. https://doi.org/10.3390/ijerph18084222
Erol, A., & Karpyak, V. M. (2015). Sex and gender-related differences in alcohol use and its consequences: Contemporary knowledge and future research considerations. Drug and Alcohol Dependence, 156, 1–13. https://doi.org/10.1016/j.drugalcdep.2015.08.023
Esser, M. B., Hedden, S. L., Kanny, D., Brewer, R. D., Gfroerer, J. C., & Naimi, T. S. (2014). Prevalence of alcohol dependence among US adult drinkers, 2009–2011. Prevention of Chronic Diseases, 11, 140329. https://doi.org/10.5888/pcd11.140329
Garey, L., Olofsson, H., Garza, T., Rogers, A. H., Kauffman, B. Y., & Zvolensky, M. J. (2020). Directional effects of anxiety and depressive disorders with substance use: A review of recent prospective research. Current Addiction Reports, 7, 344–355. https://doi.org/10.1007/s40429-020-00321-z
GBD 2019 Diseases and Injuries Collaborators. (2020). Global burden of 369 diseases and injuries in 204 countries and territories, 1990–2019: A systematic analysis for the Global Burden of Disease Study 2019. The Lancet, 396(10258), 1204–1222. https://doi.org/10.1016/S0140-6736(20)30925-9
Gondek, D., Bann, D., Patalay, P., Goodman, A., McElroy, E., Richards, M., & Ploubidis, G. B. (2022). Psychological distress from early adulthood to early old age: Evidence from the 1946, 1958 and 1970 British birth cohorts. Psychological Medicine, 52(8), 1471–1480. https://doi.org/10.1017/S003329172000327X
Graupensperger, S., Fleming, C. B., Jaffe, A. E., Rhew, I. C., Patrick, M. E., & Lee, C. M. (2021). Changes in young adults’ alcohol and marijuana use, norms, and motives from before to during the COVID-19 pandemic. Journal of Adolescent Health, 68(4), 658–665. https://doi.org/10.1016/j.jadohealth.2021.01.008
Green, B. E., & Ritter, C. (2000). Marijuana use and depression. Journal of Health and Social Behavior, 41(1), 40–49. https://doi.org/10.2307/2676359
Gros, D. F. (2014). Development and initial evaluation of Transdiagnostic Behavior Therapy (TBT) for veterans with affective disorders. Psychiatry Research, 220(1–2), 275–282. https://doi.org/10.1016/j.psychres.2014.08.018
Han, B. H., & Palamar, J. J. (2018). Marijuana use by middle-aged and older adults in the United States, 2015–2016. Drug and Alcohol Dependence, 191, 374–381. https://doi.org/10.1016/j.drugalcdep.2018.07.006
Hasin, D. S., & Kilcoyne, B. (2012). Comorbidity of psychiatric and substance use disorders in the United States: Current issues and findings from the NESARC. Current Opinion in Psychiatry, 25(3), 165–171. https://doi.org/10.1097/YCO.0b013e3283523dcc
Hasin, D. S., Shmulewitz, D., & Keyes, K. M. (2019). Alcohol use and binge drinking among U.S. men, pregnant and non-pregnant women ages 18–44: 2002–2017. Drug and Alcohol Dependence, 205, 107590. https://doi.org/10.1016/j.drugalcdep.2019.107590
Harder, V. S., Morral, A. R., & Arkes, J. (2006). Marijuana use and depression among adults: Testing for causal associations. Addiction, 101(10), 1463–1472. https://doi.org/10.1111/j.1360-0443.2006.01545.x
Hoertel, N., McMahon, K., Olfson, M., Wall, M. M., Rodríguez-Fernández, J. M., Lemogne, C., Limosin, F., & Blanco, C. (2015). A dimensional liability model of age differences in mental disorder prevalence: Evidence from a national sample. Journal of Psychiatric Research, 64, 107–113. https://doi.org/10.1016/j.jpsychires.2015.03.017
Hunt, G. E., Malhi, G. S., Lai, H. M. X., & Cleary, M. (2020). Prevalence of comorbid substance use in major depressive disorder in community and clinical settings, 1990–2019: Systematic review and meta-analysis. Journal of Affective Disorders, 266, 288–304. https://doi.org/10.1016/j.jad.2020.01.141
Imtiaz, S., Wells, S., Rehm, J., Hamilton, H. A., Nigatu, Y. T., Wickens, C. M., Jankowicz, D., & Elton-Marshall, T. (2021). Cannabis use during the COVID-19 pandemic in Canada: A repeated cross-sectional study. Journal of Addiction Medicine, 15(6), 484–490. https://doi.org/10.1097/ADM.0000000000000798
Jackson, K. M., Merrill, J. E., Stevens, A. K., Hayes, K. L., & White, H. R. (2021). Changes in alcohol use and drinking context due to the COVID-19 pandemic: A multimethod study of college student drinkers. Alcoholism: Clinical and Experimental Research, 45(4), 752–764. https://doi.org/10.1111/acer.14574
Jager, J., Keyes, K. M., Son, D., Kloska, D., Patrick, M. E., & Schulenberg, J. E. (2021). Cohort and age trends in age 35–45 prevalence of alcohol use disorder symptomology, by severity, sex, race, and education. Drug and Alcohol Dependence, 226, 108820. https://doi.org/10.1016/j.drugalcdep.2021.108820
Kersey, K., Lyons, A. C., & Hutton, F. (2022). Alcohol and drinking within the lives of midlife women: A meta-study systematic review. International Journal of Drug Policy, 99, 103453. https://doi.org/10.1016/j.drugpo.2021.103453
Kessler, R. C. (2004). The epidemiology of dual diagnosis. Biological Psychiatry, 56, 730–737. https://doi.org/10.1016/j.biopsych.2004.06.034
Keyes, K. M., Grant, B. F., & Hasin, D. S. (2008). Evidence for a closing gender gap in alcohol use, abuse, and dependence in the United States population. Drug and Alcohol Dependence, 93(1–2), 21–29. https://doi.org/10.1016/j.drugalcdep.2007.08.017
Kreski, N., Platt, J., Rutherford, C., Olfson, M., Odgers, C., Schulenberg, J. E., & Keyes, K. M. (2021). Social media use and depressive symptoms among United States adolescents. Journal of Adolescent Health, 68(3), 572–579. https://doi.org/10.1016/j.jadohealth.2020.07.006
Kuerbris, A., Sacco, P., Blazer, D. G., & Moore, A. A. (2014). Substance abuse among older adults. Clinical and Geriatric Medicine, 30(3), 629–654. https://doi.org/10.1016/j.cger.2014.04.008
Lanza, S. T., Vasilenko, S. A., Liu, X., Li, R., & Piper, M. E. (2014). Advancing the understanding of craving during smoking cessation attempts: A demonstration of the time-varying effect model. Nicotine & Tobacco Research, 16(Sup 2), S127–S134. https://doi.org/10.1093/ntr/ntt128
Li, R., Dziak, J. J., Tan, X., Huang, L., Wagner, A. T., & Yang, J. (2017). TVEM (time-varying effect modeling) SAS macro users’ guide version 3.1.1. Retrieved October 22, 2022, from https://www.methodology.psu.edu/files/2019/03/TVEM_3.1.1-1fxcco8.pdf
Maslowsky, J., Schulenberg, J. E., O’Malley, P. M., & Kloska, D. D. (2013). Depressive symptoms, conduct problems, and risk for polysubstance use among adolescents: Results from US national surveys. Mental Health and Substance Use, 7(2), 157–169. https://doi.org/10.1080/17523281.2013.786750
Maslowsky, J., Schulenberg, J. E., & Zucker, R. A. (2014). Influence of conduct problems and depressive symptomatology on adolescent substance use: Developmentally proximal versus distal effects. Developmental Psychology, 50(4), 1179–1189. https://doi.org/10.1037/a0035085
McGovern, M. P., Lambert-Harris, C., Gotham, H. J., Claus, R. E., & Xie, H. (2014). Dual diagnosis capability in mental health and addiction treatment services: An assessment of programs across multiple state systems. Administration and Policy in Mental Health and Mental Health Services Research, 41(2), 205–214. https://doi.org/10.1007/s10488-012-0449-1
McPhee, M. D., Keough, M. T., Rundle, S., Heath, L. M., Wardell, J. D., & Hendershot, C. S. (2020). Depression, environmental reward, coping motives and alcohol consumption during the COVID-19 Pandemic. Frontiers in Psychiatry, 11, 574676. https://doi.org/10.3389/fpsyt.2020.574676
Mendelsohn, C. (2012). Smoking and depression: A review. Australian Family Physician, 41(5), 304–307. https://doi.org/10.3316/informit.264503269215159
Miech R. A., Johnston, L. D., O'Malley, P. M., Bachman, J. G., Schulenberg J. E., & Patrick M. E. (2022). Monitoring the Future national survey results on drug use, 1975–2021: Volume I, Secondary school students. Ann Arbor: Institute for Social Research, The University of Michigan.
Newcomb, M. D., Huba, G. J., & Bentler, P. M. (1981). A multidimensional assessment of stressful life events among adolescents: Derivation and correlates. Journal of Health and Social Behavior, 22(4), 400–415. https://doi.org/10.2307/2136681
Newcomb, M. D., Huba, G. J., & Bentler, P. M. (1986). Life change events among adolescents: An empirical consideration of some methodological issues. Journal of Nervous and Mental Disease, 174(5), 280–289. https://doi.org/10.1097/00005053-198605000-00004
NIAAA (National Institute on Alcohol Abuse and Alcoholism). (2015). Alcohol overdose: The dangers of drinking too much. Retrieved October 22, 2022, from https://pubs.niaaa.nih.gov/publications/alcoholoverdosefactsheet/overdosefact.htm
Niedzwiedz, C. L., Green, M. J., Benzeval, M., Campbell, D., Craig, P., Demou, E., Leyland, A., Pearce, A., Thomson, R., Whitley, E., & Katikireddi, S. V. (2021). Mental health and health behaviours before and during the initial phase of the COVID-19 lockdown: Longitudinal analyses of the UK Household Longitudinal Study. Journal of Epidemiology and Community Health, 75(3), 224–231. https://doi.org/10.1136/jech-2020-215060
NIDA (National Institute on Drug Abuse). (2020). Tobacco, nicotine, and e-cigarettes research report. Retrieved October 22, 2022, from https://www.drugabuse.gov/download/1344/tobacco-nicotine-e-cigarettes-research-report.pdf?v=4b566e8f4994f24caa650ee93b59ec41
Orehek, E., Human, L. J., Sayette, M. A., Dimoff, J. D., Winograd, R. P., & Sher, K. J. (2020). Self-expression while drinking alcohol: Alcohol influences personality expression during first impressions. Personality and Social Psychology Bulletin, 46(1), 109–123. https://doi.org/10.1177/0146167219843933
Paperwalla, K. N., Levin, T. T., Weiner, J., & Saravay, S. M. (2004). Smoking and depression. Medical Clinics of North America, 88(6), 1483–1494. https://doi.org/10.1016/j.mcna.2004.06.007
Parke, H., Michalska, M., Russell, A., Moss, A. C., Holdsworth, C., Ling, J., & Larsen, J. (2018). Understanding drinking among midlife men in the United Kingdom: A systematic review of qualitative studies. Addictive Behaviors Reports, 8, 85–94. https://doi.org/10.1016/j.abrep.2018.08.001
Patrick, M. E., Kloska, D. D., Mehus, C. J., Terry-McElrath, Y. M., O’Malley, P. M., & Schulenberg, J. E. (2021). Key subgroup differences in age-related change from 18 to 55 in alcohol and marijuana use: U.S. national data. Journal of Studies on Alcohol and Drugs, 82(1), 93–102. https://doi.org/10.15288/jsad.2021.82.93
Patrick, M. E., Evans-Polce, R. J., Kloska, D. D., & Maggs, J. L. (2019). Reasons high school students use marijuana: Prevalence and correlations with use across four decades. Journal of Studies on Alcohol and Drugs, 80(1), 15–25. https://doi.org/10.15288/jsad.2019.80.15
Patrick, M. E., Evans-Polce, R., Kloska, D. D., Maggs, J. L., & Lanza, S. T. (2017). Age-related changes in associations between reasons for alcohol use and high-intensity drinking across young adulthood. Journal of Studies on Alcohol and Drugs, 78(4), 558–570. https://doi.org/10.15288/jsad.2017.78.558
Patrick, M. E., Schulenberg, J. E., Miech, R. A., Johnston, L. D., O’Malley, P. M., & Bachman, J. G. (2022a). Monitoring the Future Panel Study annual report: National data on substance use among adults ages 19 to 60, 1976–2021. University of Michigan Institute for Social Research. https://doi.org/10.7826/ISR-UM.06.585140.002.07.0001.2022
Patrick, M. E., Terry-McElrath, Y. M., Miech, R. A., Keyes, K. M., Jager, J., & Schulenberg, J. E. (2022b). Alcohol use and the COVID-19 pandemic: Historical trends in drinking, contexts, and reasons for use among U.S. adults. Social Science and Medicine, 301, 114887. https://doi.org/10.1016/j.socscimed.2022.114887
Patrick, M. E., & Terry-McElrath, Y. M. (2021). Consideration of an upper-bound continuous maximum drinks measure for adolescent binge and high-intensity drinking prevalence. Alcoholism: Clinical and Experimental Research, 45, 1821–1828.
Reeves, W. C., Pratt, L. A., Thompson, W., Ahluwalia, I. B., Dhingra, S. S., McKnight-Eily, L. R., Harrison, L., et al. (2011). Mental illness surveillance among adults in the United States. Morbidity and Mortality Weekly Report, 60(3), 1–32.
SAMHSA (Substance Abuse and Mental Health Services Administration). (2020). Key substance use and mental health indicators in the United States: Results from the 2019 National Survey on Drug Use and Health (HHS Publication No. PEP20–07–01–001, NSDUH Series H-55). Center for Behavioral Health Statistics and Quality, Substance Abuse and Mental Health Services Administration.
SAMHSA (Substance Abuse and Mental Health Services Administration). (2022). 2020 National Survey on Drug Use and Health: National OAS slides. Center for Behavioral Health Statistics and Quality, Substance Abuse and Mental Health Services Administration. Retrieved October 22, 2022, from https://www.samhsa.gov/data/
Sayette, M. A., Creswell, K. G., Dimoff, J. D., Fairbairn, C. E., Cohn, J. F., Heckman, B. W., Kirchner, T. R., Levine, J. M., & Moreland, R. L. (2012). Alcohol and group formation: A multimodal investigation of the effects of alcohol on emotion and social bonding. Psychological Science, 23(8), 869–878. https://doi.org/10.1177/0956797611435134
Schulte M. T., & Hser Y. I. (2013). Substance use and associated health conditions throughout the lifespan. Public Health Reviews, 35(2). https://doi.org/10.1007/BF03391702
Slade, T., Chapman, C., Swift, W., Keyes, K., Tonks, Z., & Teesson, M. (2016). Birth cohort trends in the global epidemiology of alcohol use and alcohol-related harms in men and women: Systematic review and metaregression. BMJ Open, 6(10), e011827. https://doi.org/10.1136/bmjopen-2016-011827
Sutin, A. R., Terracciano, A., Milaneschi, Y., An, Y., Ferrucci, L., & Zonderman, A. B. (2013). The trajectory of depressive symptoms across the adult life span. JAMA Psychiatry, 70(8), 803–811. https://doi.org/10.1001/jamapsychiatry.2013.193
Tan, X., Shiyko, M. P., Li, R., Li, Y., & Dierker, L. (2012). A time-varying effect model for intensive longitudinal data. Psychological Methods, 17, 61–77. https://doi.org/10.1037/a0025814
Tice, P., Lipari, R. N., & Van Horn, S. L. (2017). Substance use among 12th grade aged youths, by dropout status. The CBHSQ Report: August 15, 2017. Center for Behavioral Health Statistics and Quality, Substance Abuse and Mental Health Services Administration.
Villarroel, M. A., & Terlizzi, E. P. (2020). Symptoms of depression among adults: United States, 2019. NCHS Data Brief No. 379. Retrieved September from https://www.cdc.gov/nchs/data/databriefs/db379-H.pdf
Volkow, N. D., Baler, R. D., Compton, W. M., & Weiss, S. R. B. (2014). Adverse health effects of marijuana use. New England Journal of Medicine, 370(23), 2219–2227. https://doi.org/10.1056/NEJMra1402309
White, A. M. (2020). Gender differences in the epidemiology of alcohol use and related harms in the United States. Alcohol Research, 40(2), 1–13. https://doi.org/10.35946/arcr.v40.2.01
White, A., Castle, I. J., Chen, C. M., Shirley, M., Roach, D., & Hingson, R. (2015). Converging patterns of alcohol use and related outcomes among females and males in the United States, 2002 to 2012. Alcoholism: Clinical and Experimental Research, 39(9), 1712–1726. https://doi.org/10.1111/acer.12815
Zilberman, M. (2009). Substance abuse across the lifespan in women. In K. T. Brady, S. E. Back, & S. F. Greenfield (Eds.), Women and addiction: A comprehensive handbook (pp. 3–13). Guilford Press.
Zucker, R. A., Hicks, B. M., & Heitzeg, M. M. (2016). Alcohol use and the alcohol use disorders over the life course: A cross-level developmental review. In D. Cicchetti (Ed.), Developmental psychopathology: Maladaptation and psychopathology (pp. 793–832). Wiley. https://doi.org/10.1002/9781119125556.devpsy318
Funding
This study was supported by the National Institute on Drug Abuse (R01DA001411 and R01DA016575) and the National Institute on Alcohol Abuse and Alcoholism (R01AA026687 and R01 AA026861). The study sponsor had no role in (a) study design; (b) the collection, analysis, and interpretation of data; (c) the writing of the report; or (4) the decision to submit the manuscript for publication. The views expressed in this article are those of the authors and do not necessarily reflect the views of the sponsor.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics Approval
The study procedures were approved by the University of Michigan’s Health Sciences and Behavioral Sciences Institutional Review Board, and were performed in accordance with the ethical standards as laid down in the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards.
Consent to Participate
Active or passive consent (per school policy) was obtained from respondents when first participating in the Monitoring the Future study at 12th grade.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Patrick, M.E., Terry-McElrath, Y.M., Peterson, S.J. et al. Age- and Sex-Varying Associations Between Depressive Symptoms and Substance Use from Modal Ages 35 to 55 in a National Sample of U.S. Adults. Prev Sci 24, 852–862 (2023). https://doi.org/10.1007/s11121-023-01491-8
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11121-023-01491-8