Abstract
Objective
The blood–brain barrier (BBB) plays a critical role in central nervous system homeostasis, and the integrity of BBB is disrupted in many neurodegenerative diseases. Matrix metalloproteinases (MMPs) degrade the tight junctions (TJs) of endothelial cells and basement membrane components essential to BBB integrity, which leads to increased BBB permeability and allows inflammatory cells and neurotoxic substances to enter the brain. Tissue inhibitors of metalloproteinases (TIMPs), endogenous inhibitors of MMPs, regulate MMP activity, thereby maintaining BBB integrity.
Methods
The disruptive impacts of MMP-3 and MMP-9 on BBB and protective effect of TIMP-1 were investigated in a simplified in vitro model of the BBB, which was generated using rat brain microvascular endothelial cells (RBMEC). The main features of BBB formation, including permeability and the trans-endothelial electrical resistance (TEER), were monitored over time after the addition of MMP-3 and MMP-9 and their complexes with TIMP-1 inhibitor.
Results
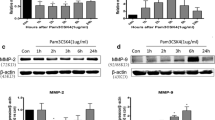
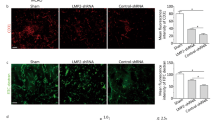
Our results indicated that MMP-3 and MMP-9 caused a dose-dependent disruption of the BBB, with 1.5 µM MMPs resulting in an over threefold increase in permeability, while TIMP-1 inhibition protected the integrity of the BBB model and recovered TEER and permeability of RBMECs. The disruption and recovery of tight junction proteins of RBMECs after MMP and TIMP treatment were also detected using fluorescent microscopy.
Conclusion
MMP-9 and MMP-3 disrupt the BBB by degrading tight junctions in endothelial cells, and TIMP-1 could inhibit the disruptive effect of MMP-3 and MMP-9 by showing potential as therapeutic protein against MMP-related diseases where BBB disruption plays a role.







Similar content being viewed by others
Data Availability
The authors declare that the data supporting the findings of this study are available within the paper and its Supplementary Information files. Should any raw data files be needed in another format they are available from the corresponding author upon reasonable request.
References
Yong VW, Power C, Forsyth P, Edwards DR. Metalloproteinases in biology and pathology of the nervous system. Nat Rev Neurosci. 2001;2(7):502–11. https://doi.org/10.1038/35081571.
Cunningham LA, Wetzel M, Rosenberg GA. Multiple roles for MMPs and TIMPs in cerebral ischemia. Glia. 2005;50(4):329–39. https://doi.org/10.1002/glia.20169.
Raeeszadeh-Sarmazdeh M, Do LD, Hritz BG. Metalloproteinases and Their Inhibitors: Potential for the Development of New Therapeutics. Cells. 2020;9(5). https://doi.org/10.3390/cells9051313.
Asahi M, Wang X, Mori T, Sumii T, Jung JC, Moskowitz MA, et al. Effects of matrix metalloproteinase-9 gene knock-out on the proteolysis of blood-brain barrier and white matter components after cerebral ischemia. J Neurosci. 2001;21(19):7724–32. https://doi.org/10.1523/JNEUROSCI.21-19-07724.2001.
Harkness KA, Adamson P, Sussman JD, Davies-Jones GA, Greenwood J, Woodroofe MN. Dexamethasone regulation of matrix metalloproteinase expression in CNS vascular endothelium. Brain. 2000;123(Pt 4):698–709. https://doi.org/10.1093/brain/123.4.698.
Fukuda S, Fini CA, Mabuchi T, Koziol JA, Eggleston LL, del Zoppo GJ. Focal cerebral ischemia induces active proteases that degrade microvascular matrix. Stroke. 2004;35(4):998–1004. https://doi.org/10.1161/01.STR.0000119383.76447.05.
Hamann GF, Okada Y, Fitridge R, del Zoppo GJ. Microvascular basal lamina antigens disappear during cerebral ischemia and reperfusion. Stroke. 1995;26(11):2120–6. https://doi.org/10.1161/01.str.26.11.2120.
Song LQ, Oseid DE, Wells EA, Coaston T, Robinson AS. Heparan Sulfate Proteoglycans (HSPGs) Serve as the Mediator Between Monomeric Tau and Its Subsequent Intracellular ERK1/2 Pathway Activation. J Mol Neurosci. 2022;72(4):772–91. https://doi.org/10.1007/s12031-021-01943-2.
Gurney KJ, Estrada EY, Rosenberg GA. Blood-brain barrier disruption by stromelysin-1 facilitates neutrophil infiltration in neuroinflammation. Neurobiol Dis. 2006;23(1):87–96. https://doi.org/10.1016/j.nbd.2006.02.006.
Banks WA. Characteristics of compounds that cross the blood-brain barrier. BMC Neurol. 2009;9 Suppl 1(Suppl 1):3. https://doi.org/10.1186/1471-2377-9-S1-S3.
Banks WA, Greig NH. Small molecules as central nervous system therapeutics: old challenges, new directions, and a philosophic divide. Future Med Chem. 2019;11(6):489–93. https://doi.org/10.4155/fmc-2018-0436.
Reese TS, Karnovsky MJ. Fine structural localization of a blood-brain barrier to exogenous peroxidase. J Cell Biol. 1967;34(1):207–17. https://doi.org/10.1083/jcb.34.1.207.
Iwatake A, Murakami A, Ebihara N. The expression of matrix metalloproteinases and their inhibitors in corneal fibroblasts by alarmins from necrotic corneal epithelial cells. Jpn J Ophthalmol. 2018;62(1):92–100. https://doi.org/10.1007/s10384-017-0541-x.
Van Hove I, Lemmens K, Van de Velde S, Verslegers M, Moons L. Matrix metalloproteinase-3 in the central nervous system: a look on the bright side. J Neurochem. 2012;123(2):203–16. https://doi.org/10.1111/j.1471-4159.2012.07900.x.
Rosenberg GA. Matrix metalloproteinases and their multiple roles in neurodegenerative diseases. Lancet Neurol. 2009;8(2):205–16. https://doi.org/10.1016/S1474-4422(09)70016-X.
Rosenberg GA, Yang Y. Vasogenic edema due to tight junction disruption by matrix metalloproteinases in cerebral ischemia. Neurosurg Focus. 2007;22(5):E4. https://doi.org/10.3171/foc.2007.22.5.5.
Wang X, Jung J, Asahi M, Chwang W, Russo L, Moskowitz MA, et al. Effects of matrix metalloproteinase-9 gene knock-out on morphological and motor outcomes after traumatic brain injury. J Neurosci. 2000;20(18):7037–42. https://doi.org/10.1523/JNEUROSCI.20-18-07037.2000.
Becker JW, Marcy AI, Rokosz LL, Axel MG, Burbaum JJ, Fitzgerald PM, et al. Stromelysin-1: three-dimensional structure of the inhibited catalytic domain and of the C-truncated proenzyme. Protein Sci. 1995;4(10):1966–76. https://doi.org/10.1002/pro.5560041002.
Nagase H, Woessner JF. Matrix metalloproteinases. J Biol Chem. 1999;274(31):21491–4. https://doi.org/10.1074/jbc.274.31.21491.
Baker AH, Edwards DR, Murphy G. Metalloproteinase inhibitors: biological actions and therapeutic opportunities. J Cell Sci. 2002;115(Pt 19):3719–27. https://doi.org/10.1242/jcs.00063.
Stetler-Stevenson WG. Matrix metalloproteinases in angiogenesis: a moving target for therapeutic intervention. J Clin Invest. 1999;103(9):1237–41. https://doi.org/10.1172/JCI6870.
Dreymueller D, Pruessmeyer J, Groth E, Ludwig A. The role of ADAM-mediated shedding in vascular biology. Eur J Cell Biol. 2012;91(6–7):472–85. https://doi.org/10.1016/j.ejcb.2011.09.003.
Dreymueller D, Martin C, Kogel T, Pruessmeyer J, Hess FM, Horiuchi K, et al. Lung endothelial ADAM17 regulates the acute inflammatory response to lipopolysaccharide. EMBO Mol Med. 2012;4(5):412–23. https://doi.org/10.1002/emmm.201200217.
Brew K, Nagase H. The tissue inhibitors of metalloproteinases (TIMPs): an ancient family with structural and functional diversity. Biochim Biophys Acta. 2010;1803(1):55–71. https://doi.org/10.1016/j.bbamcr.2010.01.003.
Masciantonio MG, Lee CKS, Arpino V, Mehta S, Gill SE. The Balance Between Metalloproteinases and TIMPs: Critical Regulator of Microvascular Endothelial Cell Function in Health and Disease. Prog Mol Biol Transl Sci. 2017;147:101–31. https://doi.org/10.1016/bs.pmbts.2017.01.001.
Murphy G. Tissue inhibitors of metalloproteinases. Genome Biol. 2011;12(11):233. https://doi.org/10.1186/gb-2011-12-11-233.
Yang Y, Estrada EY, Thompson JF, Liu W, Rosenberg GA. Matrix metalloproteinase-mediated disruption of tight junction proteins in cerebral vessels is reversed by synthetic matrix metalloproteinase inhibitor in focal ischemia in rat. J Cereb Blood Flow Metab. 2007;27(4):697–709. https://doi.org/10.1038/sj.jcbfm.9600375.
Fujimoto M, Takagi Y, Aoki T, Hayase M, Marumo T, Gomi M, et al. Tissue inhibitor of metalloproteinases protect blood-brain barrier disruption in focal cerebral ischemia. J Cereb Blood Flow Metab. 2008;28(10):1674–85. https://doi.org/10.1038/jcbfm.2008.59.
Deli MA, Abrahám CS, Kataoka Y, Niwa M. Permeability studies on in vitro blood-brain barrier models: physiology, pathology, and pharmacology. Cell Mol Neurobiol. 2005;25(1):59–127. https://doi.org/10.1007/s10571-004-1377-8.
Abbott NJ, Dolman DE, Drndarski S, Fredriksson SM. An improved in vitro blood-brain barrier model: rat brain endothelial cells co-cultured with astrocytes. Methods Mol Biol. 2012;814:415–30. https://doi.org/10.1007/978-1-61779-452-0_28.
Srinivasan B, Kolli AR, Esch MB, Abaci HE, Shuler ML, Hickman JJ. TEER measurement techniques for in vitro barrier model systems. J Lab Autom. 2015;20(2):107–26. https://doi.org/10.1177/2211068214561025.
Helms HC, Abbott NJ, Burek M, Cecchelli R, Couraud PO, Deli MA, et al. In vitro models of the blood-brain barrier: An overview of commonly used brain endothelial cell culture models and guidelines for their use. J Cereb Blood Flow Metab. 2016;36(5):862–90. https://doi.org/10.1177/0271678X16630991.
Geldenhuys WJ, Mohammad AS, Adkins CE, Lockman PR. Molecular determinants of blood-brain barrier permeation. Ther Deliv. 2015;6(8):961–71. https://doi.org/10.4155/tde.15.32.
Daneman R, Prat A. The blood-brain barrier. Cold Spring Harb Perspect Biol. 2015;7(1):a020412. https://doi.org/10.1101/cshperspect.a020412.
Raeeszadeh-Sarmazdeh M, Coban M, Mahajan S, Hockla A, Sankaran B, Downey GP, et al. Engineering of tissue inhibitor of metalloproteinases TIMP-1 for fine discrimination between closely related stromelysins MMP-3 and MMP-10. J Biol Chem. 2022;298(3):101654. https://doi.org/10.1016/j.jbc.2022.101654.
Bolt AJ, Do LD, Raeeszadeh-Sarmazdeh M. Bacterial Expression and Purification of Human Matrix Metalloproteinase-3 using Affinity Chromatography. J Vis Exp. 2022(181). https://doi.org/10.3791/63263
Raeeszadeh-Sarmazdeh M, Greene KA, Sankaran B, Downey GP, Radisky DC, Radisky ES. Directed evolution of the metalloproteinase inhibitor TIMP-1 reveals that its N- and C-terminal domains cooperate in matrix metalloproteinase recognition. J Biol Chem. 2019;294(24):9476–88. https://doi.org/10.1074/jbc.RA119.008321.
Toumaian MR, Raeeszadeh-Sarmazdeh M. Engineering Tissue Inhibitors of Metalloproteinases Using Yeast Surface Display. Methods Mol Biol. 2022;2491:361–85. https://doi.org/10.1007/978-1-0716-2285-8_19.
Liu J, Jin X, Liu KJ, Liu W. Matrix metalloproteinase-2-mediated occludin degradation and caveolin-1-mediated claudin-5 redistribution contribute to blood-brain barrier damage in early ischemic stroke stage. J Neurosci. 2012;32(9):3044–57. https://doi.org/10.1523/JNEUROSCI.6409-11.2012.
Jones AR, Shusta EV. Blood-brain barrier transport of therapeutics via receptor-mediation. Pharm Res. 2007;24(9):1759–71. https://doi.org/10.1007/s11095-007-9379-0.
Gumbleton M, Audus KL. Progress and limitations in the use of in vitro cell cultures to serve as a permeability screen for the blood-brain barrier. J Pharm Sci. 2001;90(11):1681–98. https://doi.org/10.1002/jps.1119.
Reichel A, Begley DJ, Abbott NJ. An overview of in vitro techniques for blood-brain barrier studies. Methods Mol Med. 2003;89:307–24. https://doi.org/10.1385/1-59259-419-0:307.
Gaillard PJ, de Boer AG. Relationship between permeability status of the blood-brain barrier and in vitro permeability coefficient of a drug. Eur J Pharm Sci. 2000;12(2):95–102. https://doi.org/10.1016/s0928-0987(00)00152-4.
Zhang Q, Zheng M, Betancourt CE, Liu L, Sitikov A, Sladojevic N, et al. Increase in Blood-Brain Barrier (BBB) Permeability Is Regulated by MMP3 via the ERK Signaling Pathway. Oxid Med Cell Longev. 2021;2021:6655122. https://doi.org/10.1155/2021/6655122.
Gomis-Ruth FX, Maskos K, Betz M, Bergner A, Huber R, Suzuki K, et al. Mechanism of inhibition of the human matrix metalloproteinase stromelysin-1 by TIMP-1. Nature. 1997;389(6646):77–81. https://doi.org/10.1038/37995.
Brilha S, Ong CWM, Weksler B, Romero N, Couraud PO, Friedland JS. Matrix metalloproteinase-9 activity and a downregulated Hedgehog pathway impair blood-brain barrier function in an in vitro model of CNS tuberculosis. Sci Rep. 2017;7(1):16031. https://doi.org/10.1038/s41598-017-16250-3.
Nguyen JH, Yamamoto S, Steers J, Sevlever D, Lin W, Shimojima N, et al. Matrix metalloproteinase-9 contributes to brain extravasation and edema in fulminant hepatic failure mice. J Hepatol. 2006;44(6):1105–14. https://doi.org/10.1016/j.jhep.2005.09.019.
Salah MM, Abdelmawla MA, Eid SR, Hasanin RM, Mostafa EA, Abdelhameed MW. Role of Matrix Metalloproteinase-9 in Neonatal Hypoxic-Ischemic Encephalopathy. Open Access Maced J Med Sci. 2019;7(13):2114–8. https://doi.org/10.3889/oamjms.2019.618.
Liu X, Su P, Meng S, Aschner M, Cao Y, Luo W, et al. Role of matrix metalloproteinase-2/9 (MMP2/9) in lead-induced changes in an. Int J Biol Sci. 2017;13(11):1351–60. https://doi.org/10.7150/ijbs.20670.
Tang J, Kang Y, Huang L, Wu L, Peng Y. TIMP1 preserves the blood-brain barrier through interacting with CD63/integrin. Acta Pharm Sin B. 2020;10(6):987–1003. https://doi.org/10.1016/j.apsb.2020.02.015.
Lakhan SE, Kirchgessner A, Tepper D, Leonard A. Matrix metalloproteinases and blood-brain barrier disruption in acute ischemic stroke. Front Neurol. 2013;4:32. https://doi.org/10.3389/fneur.2013.00032.
Hyatt AD, Eaton BT. Virological applications of the grid-cell-culture technique. Electron Microsc Rev. 1990;3(1):1–27. https://doi.org/10.1016/0892-0354(90)90011-g.
Huber JD, Egleton RD, Davis TP. Molecular physiology and pathophysiology of tight junctions in the blood-brain barrier. Trends Neurosci. 2001;24(12):719–25. https://doi.org/10.1016/s0166-2236(00)02004-x.
Prime SS, Nixon SV, Crane IJ, Stone A, Matthews JB, Maitland NJ, et al. The behaviour of human oral squamous cell carcinoma in cell culture. J Pathol. 1990;160(3):259–69. https://doi.org/10.1002/path.1711600313.
Shin K, Margolis B. ZOning out tight junctions. Cell. 2006;126(4):647–9. https://doi.org/10.1016/j.cell.2006.08.005.
Hawkins BT, Davis TP. The blood-brain barrier/neurovascular unit in health and disease. Pharmacol Rev. 2005;57(2):173–85. https://doi.org/10.1124/pr.57.2.4.
Obermeier B, Daneman R, Ransohoff RM. Development, maintenance and disruption of the blood-brain barrier. Nat Med. 2013;19(12):1584–96. https://doi.org/10.1038/nm.3407.
Nakagawa S, Deli MA, Kawaguchi H, Shimizudani T, Shimono T, Kittel A, et al. A new blood-brain barrier model using primary rat brain endothelial cells, pericytes and astrocytes. Neurochem Int. 2009;54(3–4):253–63. https://doi.org/10.1016/j.neuint.2008.12.002.
Calabria AR, Weidenfeller C, Jones AR, de Vries HE, Shusta EV. Puromycin-purified rat brain microvascular endothelial cell cultures exhibit improved barrier properties in response to glucocorticoid induction. J Neurochem. 2006;97(4):922–33. https://doi.org/10.1111/j.1471-4159.2006.03793.x.
Cardoso FL, Kittel A, Veszelka S, Palmela I, Tóth A, Brites D, et al. Exposure to lipopolysaccharide and/or unconjugated bilirubin impair the integrity and function of brain microvascular endothelial cells. PLoS One. 2012;7(5):e35919. https://doi.org/10.1371/journal.pone.0035919.
Veszelka S, Tóth A, Walter FR, Tóth AE, Gróf I, Mészáros M, et al. Comparison of a Rat Primary Cell-Based Blood-Brain Barrier Model With Epithelial and Brain Endothelial Cell Lines: Gene Expression and Drug Transport. Front Mol Neurosci. 2018;11:166. https://doi.org/10.3389/fnmol.2018.00166.
Aday S, Cecchelli R, Hallier-Vanuxeem D, Dehouck MP, Ferreira L. Stem Cell-Based Human Blood-Brain Barrier Models for Drug Discovery and Delivery. Trends Biotechnol. 2016;34(5):382–93. https://doi.org/10.1016/j.tibtech.2016.01.001.
Abbott NJ, Patabendige AA, Dolman DE, Yusof SR, Begley DJ. Structure and function of the blood-brain barrier. Neurobiol Dis. 2010;37(1):13–25. https://doi.org/10.1016/j.nbd.2009.07.030.
Zlokovic BV. The blood-brain barrier in health and chronic neurodegenerative disorders. Neuron. 2008;57(2):178–201. https://doi.org/10.1016/j.neuron.2008.01.003.
Molino Y, Jabès F, Lacassagne E, Gaudin N, Khrestchatisky M. Setting-up an in vitro model of rat blood-brain barrier (BBB): a focus on BBB impermeability and receptor-mediated transport. J Vis Exp. 2014;88:51278. https://doi.org/10.3791/51278.
Díaz-Coránguez M, Segovia J, López-Ornelas A, Puerta-Guardo H, Ludert J, Chávez B, et al. Transmigration of neural stem cells across the blood brain barrier induced by glioma cells. PLoS One. 2013;8(4):e60655. https://doi.org/10.1371/journal.pone.0060655.
Yan XB, Zhao YF, Yang YM, Wang N, He BZ, Qiu XT. Impact of astrocyte and lymphocyte interactions on the blood-brain barrier in multiple sclerosis. Rev Neurol (Paris). 2019;175(6):396–402. https://doi.org/10.1016/j.neurol.2018.12.006.
Safa N, Pettigrew JH, Gauthier TJ, Melvin AT. Direct measurement of deubiquitinating enzyme activity in intact cells using a protease-resistant, cell-permeable, peptide-based reporter. Biochem Eng J. 2019;151:ARTN 107320. https://doi.org/10.1016/j.bej.2019.107320.
Acknowledgements
The authors acknowledge the UNR genomic center. The authors would also like to thank Dr. Robert Rendon for his help with confocal fluorescence microscopy and Dr. Eric Shusta for his scientific consultation on fluorescence microscopy in vitro BBB model.
Funding
M. R.-S. had funding support from NIH R03AG070511 and NIH R21HD109743.
Author information
Authors and Affiliations
Contributions
M. R.-S., conception; H. A. and J. A. L., performing the experiments; H. A, J. A. L., M. R.-S., data analysis, writing and editing the manuscript drafts. M. R.-S. funding and supervision.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.

ESM 1
Supplemental Fig S1. Effect of MMP-3 and TIMP-1 alone or with each other’s and their buffer on permeability of RBMEC. MMP-3 disrupts the TJs of RBMEC leading to a nearly 25-fold increase over baseline permeability at 1.5 µM of MMP-3-cd. In the presence of 1.5 µM of both TIMP-1 and MMP-3cd, permeability is slightly over twice baseline. The 1.5 µM of MMP-3 and 1.5 µM of both TIMP-1 and MMP-3cd shown highest effect on RBMEC so we tried these amounts for rest of experiments. No significant effect of buffers or TIMP-1 alone on RBMEC permeability was observed. Experiment was performed in 24-well Transwells (Vc,t = 600 µl × Sb,t / Sa) (PNG 288 kb)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ahmadighadykolaei, H., Lambert, J.A. & Raeeszadeh-Sarmazdeh, M. TIMP-1 Protects Tight Junctions of Brain Endothelial Cells From MMP-Mediated Degradation. Pharm Res 40, 2121–2131 (2023). https://doi.org/10.1007/s11095-023-03593-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11095-023-03593-y