Abstract
Background
Docetaxel is commonly used in elderly patients, who are frequently diagnosed with prostate cancer. Although previous studies revealed no clinically relevant impact of older age on docetaxel pharmacokinetics (PK), this may be masked by indication. Metastatic castration-resistant prostate cancer (mCRPC) patients were reported to have approximately two-times lower systemic exposure compared to patients with other solid tumors. This study assessed the impact of older age on docetaxel PK, also considering the effect of indication on docetaxel PK.
Methods
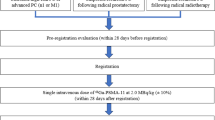
Prospectively collected docetaxel PK data from patients aged ≥70 was pooled with PK data from an earlier published multicenter study. A 3-compartment population PK model, including multiple covariates, was used to describe docetaxel plasma concentration-time data. We added the effect of prostate cancer (mCRPC and metastatic hormone-sensitive prostate cancer (mHSPC)) on clearance to this model. Hereafter, we evaluated the additional impact of older age on docetaxel clearance, using a significance threshold of p < 0.005.
Results
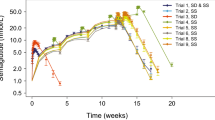
Docetaxel plasma concentration-time data from 157 patients were analyzed. Median age in the total cohort was 67 years (range 31-87), with 49% of the total cohort aged ≥70. The impact of age on docetaxel clearance was statistically significant (p < 0.005). For a typical patient, a 10-year and 20-year increase of age led to a reduction in clearance of 17% and 34%, respectively.
Conclusion
In this cohort study, age significantly and independently affected docetaxel clearance, showing lower docetaxel clearance in elderly patients. In our cohort, mCRPC and mHSPC patients both had higher clearance than patients with other solid tumors.




Similar content being viewed by others
References
DRUGDEX®. Truven health analytics. Docetaxel. 2015.
Food and Drug Administration. Official label - taxotere (docetaxel), NDA 020449. 2015.
Bruno R, Vivier N, Vergniol JC, De Phillips SL, Montay G, Sheiner LB. A population pharmacokinetic model for docetaxel (Taxotere): model building and validation. J Pharmacokinet Biopharm. 1996;24:153–72.
Bruno R, Vivier N, Veyrat-Follet C, Montay G, Rhodes GR. Population pharmacokinetics and pharmacokinetic-pharmacodynamic relationships for docetaxel. Investig New Drugs. 2001;19:163–9.
Bosch TM, Huitema ADR, Doodeman VD, Jansen R, Witteveen E, Smit WM, et al. Pharmacogenetic screening of CYP3A and ABCB1 in relation to population pharmacokinetics of docetaxel. Clin Cancer Res. 2006;12:5786–93.
Sehl M, Sawhney R, Naeim A. Physiologic aspects of aging: impact on cancer management and decision making, part II. Cancer J. 2005;11:461–73.
Crombag MRBS, Joerger M, Thürlimann B, Schellens JHM, Beijnen JH, Huitema ADR. Pharmacokinetics of selected anticancer drugs in elderly cancer patients: focus on breast cancer. Cancers (Basel). 2016;8.
de Vries Schultink A, Crombag M, van Werkhoven E, Otten H, Bergman A, Schellens J, et al. Neutropenia and docetaxel exposure in metastatic castration-resistant prostate cancer patients: a meta-analysis and evaluation of a clinical cohort. Cancer Med. 2019;8:1406–15.
Franke RM, Carducci MA, Rudek MA, Baker SD, Sparreboom A. Castration-dependent pharmacokinetics of docetaxel in patients with prostate cancer. J Clin Oncol. 2010;28:4562–7.
Belderbos BPS, Hussaarts KGAM, van Harten LJ, Oomen-de Hoop E, de Bruijn P, Hamberg P, et al. Effects of prednisone on docetaxel pharmacokinetics in men with metastatic prostate cancer: a randomized drug-drug interaction study. Br J Clin Pharmacol. 2019; 986–92.
Hendrikx JJMA, Hillebrand MJX, Thijssen B, Rosing H, Schinkel AH, Schellens JHM, et al. A sensitive combined assay for the quantification of paclitaxel, docetaxel and ritonavir in human plasma using liquid chromatography coupled with tandem mass spectrometry. J Chromatogr B Anal Technol Biomed Life Sci. 2011;879:2984–90.
The International Conference on Harmonisation of Technical Requirements for Registration of Pharmaceuticals for Human Use. (ICH). 2018. www.ich.org.
Cornford P, Bellmunt J, Bolla M, Briers E, De Santis M, Gross T, et al. EAU-ESTRO-SIOG guidelines on prostate cancer. Part II: treatment of relapsing, metastatic, and castration-resistant prostate cancer. Eur Urol. 2017;71:630–42.
Vale CL, Burdett S, Rydzewska LHM, Albiges L, Clarke NW, Fisher D, et al. Addition of docetaxel or bisphosphonates to standard of care in men with localised or metastatic, hormone-sensitive prostate cancer: a systematic review and meta-analyses of aggregate data. Lancet Oncol. 2016;17:243–56.
Dosne AG, Bergstrand M, Harling K, Karlsson MO. Improving the estimation of parameter uncertainty distributions in nonlinear mixed effects models using sampling importance resampling. J Pharmacokinet Pharmacodyn. 2016;43:583–96.
Hutson PR, Oettel K, Douglas J, Ritter M, Messing E, Staab MJ, et al. Effect of medical castration on CYP3A4 enzyme activity using the erythromycin breath test. Cancer Chemother Pharmacol. 2008;62:373–7.
Minami H, Ohe Y, Niho S, Goto K, Ohmatsu H, Kubota K, et al. Comparison of pharmacokinetics and pharmacodynamics of docetaxel and cisplatin in elderly and non-elderly patients: why is toxicity increased in elderly patients? J Clin Oncol. 2004;22:2901–8.
Slaviero KA, Clarke SJ, McLachlan AJ, Blair EYL, Rivory LP. Population pharmacokinetics of weekly docetaxel in patients with advanced cancer. Br J Clin Pharmacol. 2004;57:44–53.
ten Tije AJ, Verweij J, Carducci MA, Graveland W, Rogers T, Pronk T, et al. Prospective evaluation of the pharmacokinetics and toxicity profile of docetaxel in the elderly. J Clin Oncol. 2005;23:1070–7.
Hurria A, Fleming MT, Baker SD, Kelly WK, Cutchall K, Panageas K, et al. Pharmacokinetics and toxicity of weekly docetaxel in older patients. Clin Cancer Res. 2006;12:6100–5.
Yamamoto N, Tamura T, Kamiya Y, Sekine I, Kunitoh H, Saijo N. Correlation between docetaxel clearance and estimated cytochrome P450 activity by urinary metabolite of exogenous cortisol. J Clin Oncol. 2000;18:2301–8.
Michael M, Cullinane C, Hatzimihalis A, O’Kane C, Milner A, Booth R, et al. Docetaxel pharmacokinetics and its correlation with two in vivo probes for cytochrome P450 enzymes: the C 14-erythromycin breath test and the antipyrine clearance test. Cancer Chemother Pharmacol. 2012;69:125–35.
James ND, Sydes MR, Clarke NW, Mason MD, Dearnaley DP, Spears MR, et al. Addition of docetaxel, zoledronic acid, or both to first-line long-term hormone therapy in prostate cancer (STAMPEDE): survival results from an adaptive, multiarm, multistage, platform randomised controlled trial. Lancet. 2016;387:1163–77. https://doi.org/10.1016/S0140-6736(15)01037-5.
Gravis G, Audenet F, Irani J, Timsit MO, Barthelemy P, Beuzeboc P, et al. Chemotherapy in hormone-sensitive metastatic prostate cancer: evidences and uncertainties from the literature. Cancer Treat Rev. 2017;55:211–7.
Hooker A, ten Tije A, Carducci M, Weber J, Garrett-Mayer E, Gelderblom H, et al. Population pharmacokinetic model for docetaxel in patients with varying degrees of liver function: incorporating cytochrome P450 3A activity measurements. Clin Parmacol Ther. 2008;84:111–8.
Klotz U. Pharmacokinetics and drug metabolism in the elderly. Drug Metab Rev. 2009;41:67–76.
Fukae M, Shiraishi Y, Hirota T, Sasaki Y, Yamahashi M, Takayama K, et al. Population pharmacokinetic-pharmacodynamic modeling and model-based prediction of docetaxel-induced neutropenia in Japanese patients with non-small cell lung cancer. Cancer Chemother Pharmacol. 2016;78:1013–23.
Rosing H, Lustig V, Van Warmerdam LJC, Huizing MT, Ten Bokkel Huinink WW, Schellens JHM, et al. Pharmacokinetics and metabolism of docetaxel administered as a 1-h intravenous infusion. Cancer Chemother Pharmacol. 2000;45:213–8.
John V, Mashru S, Lichtman S. Pharmacological factors influencing anticancer drug selection in the elderly. Drugs Aging. 2003;20:737–59.
European Medicines Agency. Summary of product characteristics - taxotere (docetaxel). 2015.
Trump DL. Commentary on “Androgen-deprivation therapy alone or with docetaxel in non-castrate metastatic prostate cancer (GETUG-AFU 15): A randomised, open-label, phase 3 trial”. Urol Oncol. 2013;31:1845.
Droz JP, Albrand G, Gillessen S, Hughes S, Mottet N, Oudard S, et al. Management of prostate cancer in elderly patients: recommendations of a task force of the International Society of Geriatric Oncology. Eur Urol. 2017;72:521–31.
Choi JH, Choi J, Chung SM, Oh JY, Lee YS, Min KH, et al. The clinical efficacy and safety of four-weekly docetaxel as first-line therapy in elderly lung Cancer patients with squamous cell carcinoma. Tuberc Respir Dis (Seoul). 2018;81:1–6.
Maia MC, Pereira AAL, Lage LV, Fraile NM, Vaisberg V Van, Kudo G, et al. Efficacy and safety of docetaxel in elderly patients with metastatic castration-resistant prostate cancer. J Glob Oncol. 2017; 1–9.
Crombag MRBS, de Vries Schultink AHM, Van Doremalen JGC, Martin H, Andries O, Jan MB, et al. Age - associated hematological toxicity in patients with metastatic castration - resistant prostate cancer treated with docetaxel in clinical practice. Drugs Aging. 2019;36:379–85.
ACKNOWLEDGMENTS AND DISCLOSURES
No sources of funding were used in the preparation of this manuscript. Jos H. Beijnen is (part-time) employee and (indirect) shareholder of Modra Pharmaceuticals and (partly) holds a patent on oral taxane pharmaceutical formulations. The other authors declare no conflicts of interest in connection with this manuscript.
The authors wish to express their gratitude to all study participants and engaged medical workers (physicians and nurses) who made this work possible. The authors thank the Research High Performance Computing facility of the NKI for support in the use of computational resources. All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committees and was carried out in accordance with ICH Guidelines for Good Clinical Practice. Written informed consent was obtained from all individual participants.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Key Points
• Older age significantly influenced docetaxel clearance
• mCRPC and mHSPC patients both had higher clearance than patients with other solid tumors
• Regardless of the impact of prostate cancer, older age was a significant determinant for docetaxel clearance
Rights and permissions
About this article
Cite this article
Crombag, MR.B.S., Dorlo, T.P.C., van der Pan, E. et al. Exposure to Docetaxel in the Elderly Patient Population: a Population Pharmacokinetic Study. Pharm Res 36, 181 (2019). https://doi.org/10.1007/s11095-019-2706-4
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11095-019-2706-4