Abstract
Purpose
Meningiomas are the most common primary intracranial tumor in older adults (Ostrom et al. in Neuro Oncol 21(Suppl 5):v1–v100, 2019). Treatment is largely driven by, in addition to patient characteristics and extent of resection/Simpson grade, the World Health Organization (WHO) grading of meningiomas. The current grading scheme, based predominantly on histologic features and only limited molecular characterization of these tumors (WHO Classification of Tumours Editorial Board, in: Central nervous system tumours, International Agency for Research on Cancer, Lyon, 2021), (Mirian et al. in J Neurol Neurosurg Psychiatry 91(4):379–387, 2020), does not consistently reflect the biologic behavior of meningiomas. This leads to both under-treatment and over-treatment of patients, and hence, suboptimal outcomes (Rogers et al. in Neuro Oncol 18(4):565–574). The goal of this review is to synthesize studies to date investigating molecular features of meningiomas as they relate to patient outcomes, in order to clarify best practices in assessing and, therefore, treating meningiomas.
Methods
The available literature of genomic landscape and molecular features of in meningioma was screened using PubMed.
Results
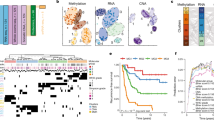
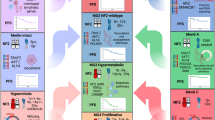
Greater understanding of meningiomas is reached by integrating histopathology, mutational analysis, DNA copy number changes, DNA methylation profiles, and potentially additional modalities to fully capture the clinical and biologic heterogeneity of these tumors.
Conclusion
Diagnosis and classification of meningioma is best accomplished using a combination of histopathology with genomic and epigenomic factors. Future classification schemes may benefit from such an integrated approach.


Similar content being viewed by others
References
WHO Classification of Tumours Editorial Board (2021) Central nervous system tumours. International Agency for Research on Cancer, Lyon
Sahm F et al (2016) TERT promoter mutations and risk of recurrence in meningioma. J Natl Cancer Inst 108(5):djv377
Mirian C et al (2020) Poor prognosis associated with TERT gene alterations in meningioma is independent of the WHO classification: an individual patient data meta-analysis. J Neurol Neurosurg Psychiatry 91(4):378–387
Rogers CL et al (2016) Pathology concordance levels for meningioma classification and grading in NRG Oncology RTOG Trial 0539. Neuro Oncol 18(4):565–574
Suppiah S et al (2019) Molecular and translational advances in meningiomas. Neuro Oncol 21(Suppl 1):i4–i17
Galani V et al (2017) Genetic and epigenetic alterations in meningiomas. Clin Neurol Neurosurg 158:119–125
Katz LM et al (2018) Loss of histone H3K27me3 identifies a subset of meningiomas with increased risk of recurrence. Acta Neuropathol 135(6):955–963
Aizer AA et al (2016) A prognostic cytogenetic scoring system to guide the adjuvant management of patients with atypical meningioma. Neuro Oncol 18(2):269–274
McNulty SN et al (2018) Analysis of point mutations and copy number variation in Grade II and III meningioma. Exp Mol Pathol 105(3):328–333
Driver J et al (2022) A molecularly integrated grade for meningioma. Neuro Oncol 24(5):796–808
Choudhury A et al (2022) Meningioma DNA methylation groups identify biological drivers and therapeutic vulnerabilities. Nat Genet 54(5):649–659
Maas SLN et al (2021) Integrated molecular-morphologic meningioma classification: a multicenter retrospective analysis, retrospectively and prospectively validated. J Clin Oncol 39(34):3839–3852
Nassiri F et al (2021) A clinically applicable integrative molecular classification of meningiomas. Nature 597(7874):119–125
Nassiri F et al (2019) DNA methylation profiling to predict recurrence risk in meningioma: development and validation of a nomogram to optimize clinical management. Neuro Oncol 21(7):901–910
Gao F et al (2013) DNA methylation in the malignant transformation of meningiomas. PLoS ONE 8(1):e54114
Kishida Y et al (2012) Epigenetic subclassification of meningiomas based on genome-wide DNA methylation analyses. Carcinogenesis 33(2):436–441
Olar A et al (2017) Global epigenetic profiling identifies methylation subgroups associated with recurrence-free survival in meningioma. Acta Neuropathol 133(3):431–444
Vengoechea J et al (2013) Methylation markers of malignant potential in meningiomas. J Neurosurg 119(4):899–906
Millesi M et al (2022) DNA methylation associates with clinical courses of atypical Meningiomas: a matched case-control study. Front Oncol 12:811729
Sahm F et al (2017) DNA methylation-based classification and grading system for meningioma: a multicentre, retrospective analysis. Lancet Oncol 18(5):682–694
Bayley JCt et al (2022) Multiple approaches converge on three biological subtypes of meningioma and extract new insights from published studies. Sci Adv 8(5):eabm6247
Yuzawa S, Nishihara H, Tanaka S (2016) Genetic landscape of meningioma. Brain Tumor Pathol 33(4):237–247
Birzu C, Peyre M, Sahm F (2020) Molecular alterations in meningioma: prognostic and therapeutic perspectives. Curr Opin Oncol 32(6):613–622
Abedalthagafi M et al (2016) Oncogenic PI3K mutations are as common as AKT1 and SMO mutations in meningioma. Neuro Oncol 18(5):649–655
Bujko M et al (2014) EGFR, PIK3CA, KRAS and BRAF mutations in meningiomas. Oncol Lett 7(6):2019–2022
Pang JC et al (2006) Rare mutation of PIK3CA in meningiomas. Acta Neuropathol 111(3):284–285
Clark VE et al (2016) Recurrent somatic mutations in POLR2A define a distinct subset of meningiomas. Nat Genet 48(10):1253–1259
Lynes J et al (2022) Molecular determinants of outcomes in meningiomas. Front Oncol 12:962702
Sievers P et al (2021) Clear cell meningiomas are defined by a highly distinct DNA methylation profile and mutations in SMARCE1. Acta Neuropathol 141(2):281–290
Smith MJ et al (2017) SMARCE1 mutation screening in classification of clear cell meningiomas. Histopathology 70(5):814–820
Tauziede-Espariat A et al (2018) Loss of SMARCE1 expression is a specific diagnostic marker of clear cell meningioma: a comprehensive immunophenotypical and molecular analysis. Brain Pathol 28(4):466–474
Kepes JJ et al (1998) Rhabdoid transformation of tumor cells in meningiomas: a histologic indication of increased proliferative activity: report of four cases. Am J Surg Pathol 22(2):231–238
Perry A et al (1998) “Rhabdoid” meningioma: an aggressive variant. Am J Surg Pathol 22(12):1482–1490
Louis D, Scheithaur B, Budka H (2000) Meningiomas. WHO classification of tumour: pathology and genetics of tumoursof the nervous system. IARC Press, Lyon
Vaubel RA et al (2016) Meningiomas with rhabdoid features lacking other histologic features of malignancy: a study of 44 cases and review of the literature. J Neuropathol Exp Neurol 75(1):44–52
Shankar GM et al (2017) Germline and somatic BAP1 mutations in high-grade rhabdoid meningiomas. Neuro Oncol 19(4):535–545
Williams EA et al (2020) Frequent inactivating mutations of the PBAF complex gene PBRM1 in meningioma with papillary features. Acta Neuropathol 140(1):89–93
Patel AJ et al (2019) Molecular profiling predicts meningioma recurrence and reveals loss of DREAM complex repression in aggressive tumors. Proc Natl Acad Sci U S A 116(43):21715–21726
Harmanci AS et al (2017) Integrated genomic analyses of de novo pathways underlying atypical meningiomas. Nat Commun 8:14433
Liu F, Qian J, Ma C (2021) MPscore: a novel predictive and prognostic scoring for progressive meningioma. Cancers (Basel) 13(5):1113
Schmidt M et al (2016) Transcriptomic analysis of aggressive meningiomas identifies PTTG1 and LEPR as prognostic biomarkers independent of WHO grade. Oncotarget 7(12):14551–14568
Chen WC et al (2020) A prognostic gene-expression signature and risk score for meningioma recurrence after resection. Neurosurgery 88(1):202–210
Olar A et al (2018) A gene expression signature predicts recurrence-free survival in meningioma. Oncotarget 9(22):16087–16098
Lee JY et al (2004) Loss of heterozygosity analysis of benign, atypical, and anaplastic meningiomas. Neurosurgery 55(5):1163–1173
Shoshan Y et al (2000) Radiation-induced meningioma: a distinct molecular genetic pattern? J Neuropathol Exp Neurol 59(7):614–620
Joachim T et al (2001) Comparative analysis of the NF2, TP53, PTEN, KRAS, NRAS and HRAS genes in sporadic and radiation-induced human meningiomas. Int J Cancer 94(2):218–221
Brastianos PK et al (2013) Genomic sequencing of meningiomas identifies oncogenic SMO and AKT1 mutations. Nat Genet 45(3):285–289
Sahm F et al (2017) Meningiomas induced by low-dose radiation carry structural variants of NF2 and a distinct mutational signature. Acta Neuropathol 134(1):155–158
Agnihotri S et al (2017) Therapeutic radiation for childhood cancer drives structural aberrations of NF2 in meningiomas. Nat Commun 8(1):186
Ostrom QT et al (2016) American brain tumor association adolescent and young adult primary brain and central nervous system tumors diagnosed in the United States in 2008–2012. Neuro Oncol 18(Suppl 1):i1–i50
Perry A, Dehner LP (2003) Meningeal tumors of childhood and infancy. An update and literature review. Brain Pathol 13(3):386–408
Rushing EJ et al (2005) Central nervous system meningiomas in the first two decades of life: a clinicopathological analysis of 87 patients. J Neurosurg 103(6 Suppl):489–495
Caroli E, Russillo M, Ferrante L (2006) Intracranial meningiomas in children: report of 27 new cases and critical analysis of 440 cases reported in the literature. J Child Neurol 21(1):31–36
Perry A et al (2001) Aggressive phenotypic and genotypic features in pediatric and NF2-associated meningiomas: a clinicopathologic study of 53 cases. J Neuropathol Exp Neurol 60(10):994–1003
Kirches E et al (2021) Molecular profiling of pediatric meningiomas shows tumor characteristics distinct from adult meningiomas. Acta Neuropathol 142(5):873–886
Erdincler P et al (1998) Intracranial meningiomas in children: review of 29 cases. Surg Neurol 49(2):136–40 (discussion 140-1)
Battu S et al (2018) Clinicopathological and molecular characteristics of pediatric meningiomas. Neuropathology 38(1):22–33
Toland A et al (2020) Pediatric meningioma: a clinicopathologic and molecular study with potential grading implications. Brain Pathol 30(6):1134–1143
Sievers P et al (2020) YAP1-fusions in pediatric NF2-wildtype meningioma. Acta Neuropathol 139(1):215–218
Schieffer KM et al (2021) YAP1-FAM118B fusion defines a rare subset of childhood and young adulthood meningiomas. Am J Surg Pathol 45(3):329–340
Esposito S et al (2022) Interhemispheric pediatric meningioma, YAP1 fusion-positive. Diagnostics (Basel) 12(10):2367
Hua L et al (2022) Two predominant molecular subtypes of spinal meningioma: thoracic NF2-mutant tumors strongly associated with female sex, and cervical AKT1-mutant tumors originating ventral to the spinal cord. Acta Neuropathol. https://doi.org/10.1007/s00401-022-02474-9
Sahm F et al (2013) AKT1E17K mutations cluster with meningothelial and transitional meningiomas and can be detected by SFRP1 immunohistochemistry. Acta Neuropathol 126(5):757–762
Clark VE et al (2013) Genomic analysis of non-NF2 meningiomas reveals mutations in TRAF7, KLF4, AKT1, and SMO. Science 339(6123):1077–80
Ricklefs FL et al (2022) Genetic and epigenetic profiling identifies two distinct classes of spinal meningiomas. Acta Neuropathol. https://doi.org/10.1007/s00401-022-02504-6
Smith MJ et al (2014) Germline SMARCE1 mutations predispose to both spinal and cranial clear cell meningiomas. J Pathol 234(4):436–440
Okano A et al (2022) Advances in Molecular biological and translational studies in World Health Organization grades 2 and 3 meningiomas: a literature review. Neurol Med Chir (Tokyo) 62(8):347–360
Funding
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
MPN and KDA: wrote the main manuscript text, and prepared the figures and table.
Corresponding author
Ethics declarations
Conflict of interest
MPN and KDA each have no relevant financial or non-financial interests to disclose.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Nasrallah, M.P., Aldape, K.D. Molecular classification and grading of meningioma. J Neurooncol 161, 373–381 (2023). https://doi.org/10.1007/s11060-022-04228-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-022-04228-9