Abstract
Objective
To evaluate the value of the contrast enhancing pattern on pre-treatment MRI for predicting the response to anti-angiogenic treatment in patients with IDH-wild type recurrent glioblastoma.
Methods
This retrospective study enrolled 65 patients with IDH wild-type recurrent glioblastoma who received standard therapy and then received either bevacizumab (46 patients) or temozolomide (19 patients) as a secondary treatment. The contrast enhancing pattern on pre-treatment MRI was visually analyzed and dichotomized into contrast enhancing lesion (CEL) dominant and non-enhancing lesion (NEL) dominant types. Quantitative volumetric analysis was used to support the dichotomization. The Kaplan–Meier method and Cox proportional hazards regression analysis were used to stratify progression free survival (PFS) according to the treatment in the entire patients, CEL dominant group, and NEL dominant group.
Results
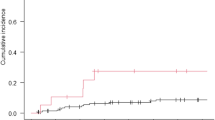
In all patients, the PFS of those treated with bevacizumab was not significantly different from those treated with temozolomide (log-rank test, P = 0.96). When the contrast enhancing pattern was considered, bevacizumab was associated with longer PFS in the CEL dominant group (P = 0.031), whereas temozolomide showed longer PFS in the NEL dominant group (P = 0.022). Quantitative analysis revealed mean values for the proportion of solid-enhancing tumor of 13.7% for the CEL dominant group and 4.3% for the NEL dominant group.
Conclusion
Patients with the CEL dominant type showed a better treatment response to bevacizumab, whereas NEL dominant types showed a better response to temozolomide. The contrast enhancing pattern on pre-treatment MRI can be used to stratify patients with IDH wild-type recurrent glioblastoma according to the effect of anti-angiogenic treatment.



Similar content being viewed by others

References
Kreisl TN, Kim L, Moore K, Duic P, Royce C, Stroud I, Garren N, Mackey M, Butman JA, Camphausen K (2009) Phase II trial of single-agent bevacizumab followed by bevacizumab plus irinotecan at tumor progression in recurrent glioblastoma. J Clin Oncol 27:740
Norden AD, Drappatz J, Muzikansky A, David K, Gerard M, McNamara MB, Phan P, Ross A, Kesari S, Wen PY (2009) An exploratory survival analysis of anti-angiogenic therapy for recurrent malignant glioma. J Neurooncol 92:149–155
Ballman KV (2015) Biomarker: predictive or prognostic? J Clin Oncol 33:3968–3971. https://doi.org/10.1200/jco.2015.63.3651
Oldenhuis CN, Oosting SF, Gietema JA, de Vries EG (2008) Prognostic versus predictive value of biomarkers in oncology. Eur J Cancer (Oxford, England: 1990) 44:946–953. https://doi.org/10.1016/j.ejca.2008.03.006
Bennett IE, Field KM, Hovens CM, Moffat BA, Rosenthal MA, Drummond K, Kaye AH, Morokoff AP (2017) Early perfusion MRI predicts survival outcome in patients with recurrent glioblastoma treated with bevacizumab and carboplatin. J Neurooncol 131:321–329. https://doi.org/10.1007/s11060-016-2300-0
Kickingereder P, Wiestler B, Burth S, Wick A, Nowosielski M, Heiland S, Schlemmer H-P, Wick W, Bendszus M, Radbruch A (2015) Relative cerebral blood volume is a potential predictive imaging biomarker of bevacizumab efficacy in recurrent glioblastoma. Neuro Oncol 17:1139–1147. https://doi.org/10.1093/neuonc/nov028
Kong Z, Yan C, Zhu R, Wang J, Wang Y, Wang Y, Wang R, Feng F, Ma W (2018) Imaging biomarkers guided anti-angiogenic therapy for malignant gliomas. NeuroImage: Clin 20:51–60
Pope WB, Lai A, Mehta R, Kim H, Qiao J, Young JR, Xue X, Goldin J, Brown M, Nghiemphu P (2011) Apparent diffusion coefficient histogram analysis stratifies progression-free survival in newly diagnosed bevacizumab-treated glioblastoma. Am J Neuroradiol 32:882–889
Schmainda KM, Zhang Z, Prah M, Snyder BS, Gilbert MR, Sorensen AG, Barboriak DP, Boxerman JL (2015) Dynamic susceptibility contrast MRI measures of relative cerebral blood volume as a prognostic marker for overall survival in recurrent glioblastoma: results from the ACRIN 6677/RTOG 0625 multicenter trial. Neuro Oncol 17:1148–1156
Zhang J, Liu H, Tong H, Wang S, Yang Y, Liu G, Zhang W (2017) Clinical applications of contrast-enhanced perfusion MRI techniques in gliomas: recent advances and current challenges. Contrast Media Mol imaging. https://doi.org/10.1155/2017/7064120
Nowosielski M, Wiestler B, Goebel G, Hutterer M, Schlemmer HP, Stockhammer G, Wick W, Bendszus M, Radbruch A (2014) Progression types after antiangiogenic therapy are related to outcome in recurrent glioblastoma. Neurology 82:1684–1692
Cachia D, Elshafeey NA, Kamiya-Matsuoka C, Hatami M, Alfaro-Munoz KD, Mandel JJ, Colen R, DeGroot JF (2017) Radiographic patterns of progression with associated outcomes after bevacizumab therapy in glioblastoma patients. J Neurooncol 135:75–81. https://doi.org/10.1007/s11060-017-2550-5
Nowosielski M, Ellingson BM, Chinot OL, Garcia J, Revil C, Radbruch A, Nishikawa R, Mason WP, Henriksson R, Saran F (2018) Radiologic progression of glioblastoma under therapy—an exploratory analysis of AVAglio. Neuro Oncol 20:557–566
Cho SJ, Kim HS, Suh CH, Park JE (2020) Radiological recurrence patterns after bevacizumab treatment of recurrent high-grade glioma: a systematic review and meta-analysis. Korean J Radiol 21:908–918. https://doi.org/10.3348/kjr.2019.0898
Azok J, Guccione S, Lim M, Harsh G, Atlas S, Li K, Bednarski M (2004) The use of magnetic resonance imaging to guide the analysis of serum proteomic patterns in glioblastoma multiforme. Proc Intl Soc Mag Reson Med 11:220
Hobbs SK, Shi G, Homer R, Harsh G, Atlas SW, Bednarski MD (2003) Magnetic resonance image–guided proteomics of human glioblastoma multiforme. J Magn Reson Imaging 18:530–536
Pope WB, Chen JH, Dong J, Carlson MR, Perlina A, Cloughesy TF, Liau LM, Mischel PS, Nghiemphu P, Lai A (2008) Relationship between gene expression and enhancement in glioblastoma multiforme: exploratory DNA microarray analysis. Radiology 249:268–277
Stupp R, Mason WP, van den Bent MJ, Weller M, Fisher B, Taphoorn MJ, Belanger K, Brandes AA, Marosi C, Bogdahn U, Curschmann J, Janzer RC, Ludwin SK, Gorlia T, Allgeier A, Lacombe D, Cairncross JG, Eisenhauer E, Mirimanoff RO, European Organisation for R, Treatment of Cancer Brain T, Radiotherapy G, National Cancer Institute of Canada Clinical Trials G (2005) Radiotherapy plus concomitant and adjuvant temozolomide for glioblastoma. N Engl J Med 352:987–996. https://doi.org/10.1056/NEJMoa043330
Wen PY, Macdonald DR, Reardon DA, Cloughesy TF, Sorensen AG, Galanis E, DeGroot J, Wick W, Gilbert MR, Lassman AB (2010) Updated response assessment criteria for high-grade gliomas: response assessment in neuro-oncology working group. J Clin Oncol 28:1963–1972
Huang RY, Rahman R, Ballman KV, Felten SJ, Anderson SK, Ellingson BM, Nayak L, Lee EQ, Abrey LE, Galanis E, Reardon DA, Pope WB, Cloughesy TF, Wen PY (2016) The impact of T2/FLAIR evaluation per RANO criteria on response assessment of recurrent glioblastoma patients treated with bevacizumab. Clin Cancer Res 22:575–581. https://doi.org/10.1158/1078-0432.Ccr-14-3040
Pope W, Xia Q, Paton V, Das A, Hambleton J, Kim H, Huo J, Brown M, Goldin J, Cloughesy T (2011) Patterns of progression in patients with recurrent glioblastoma treated with bevacizumab. Neurology 76:432–437
Isensee F, Schell M, Pflueger I, Brugnara G, Bonekamp D, Neuberger U, Wick A, Schlemmer HP, Heiland S, Wick W, Bendszus M, Maier-Hein KH, Kickingereder P (2019) Automated brain extraction of multisequence MRI using artificial neural networks. J Time Ser Anal 40:4952–4964. https://doi.org/10.1002/hbm.24750
Verhoeff JJC, van Tellingen O, Claes A, Stalpers LJA, van Linde ME, Richel DJ, Leenders WPJ, van Furth WR (2009) Concerns about anti-angiogenic treatment in patients with glioblastoma multiforme. BMC Cancer 9:444. https://doi.org/10.1186/1471-2407-9-444
Jain RK (2003) Molecular regulation of vessel maturation. Nat Med 9:685–693. https://doi.org/10.1038/nm0603-685
Hardee ME, Zagzag D (2012) Mechanisms of glioma-associated neovascularization. Am J Pathol 181:1126–1141
Pope WB, Lai A, Nghiemphu P, Mischel P, Cloughesy T (2006) MRI in patients with high-grade gliomas treated with bevacizumab and chemotherapy. Neurology 66:1258–1260
Liu TT, Achrol AS, Mitchell LA, Rodriguez SA, Feroze A, Iv M, Kim C, Chaudhary N, Gevaert O, Stuart JM (2017) Magnetic resonance perfusion image features uncover an angiogenic subgroup of glioblastoma patients with poor survival and better response to antiangiogenic treatment. Neuro Oncol 19:997–1007
Zhang W, Kreisl T, Solomon J, Reynolds R, Glen D, Cox R, Fine H, Butman J. Acute effects of bevacizumab on glioblastoma vascularity assessed with DCE-MRI and relation to patient survival. Proceedings ISMRM, p 282
Lamszus K, Kunkel P, Westphal M (2003) Invasion as limitation to anti-angiogenic glioma therapy. Acta Neurochir Suppl 88:169–177. https://doi.org/10.1007/978-3-7091-6090-9_23
van Kempen LC, Leenders WP (2006) Tumours can adapt to anti-angiogenic therapy depending on the stromal context: lessons from endothelial cell biology. Eur J Cell Biol 85:61–68. https://doi.org/10.1016/j.ejcb.2005.10.003
Mathieu V, De Nève N, Le Mercier M, Dewelle J, Gaussin J-F, Dehoux M, Kiss R, Lefranc F (2008) Combining bevacizumab with temozolomide increases the antitumor efficacy of temozolomide in a human glioblastoma orthotopic xenograft model. Neoplasia 10:1383–1392
Leten C, Struys T, Dresselaers T, Himmelreich U (2014) In vivo and ex vivo assessment of the blood brain barrier integrity in different glioblastoma animal models. J Neurooncol 119:297–306
Pries AR, Höpfner M, Le Noble F, Dewhirst MW, Secomb TW (2010) The shunt problem: control of functional shunting in normal and tumour vasculature. Nat Rev Cancer 10:587–593
Bonekamp D, Mouridsen K, Radbruch A, Kurz FT, Eidel O, Wick A, Schlemmer H-P, Wick W, Bendszus M, Østergaard L (2017) Assessment of tumor oxygenation and its impact on treatment response in bevacizumab-treated recurrent glioblastoma. J Cereb Blood Flow Metab 37:485–494
Lasocki A, Gaillard F, Tacey M, Drummond K, Stuckey S (2016) Incidence and prognostic significance of non-enhancing cortical signal abnormality in glioblastoma. J Med Imaging Radiat Oncol 60:66–73
Kotrotsou A, Elakkad A, Sun J, Thomas GA, Yang D, Abrol S, Wei W, Weinberg JS, Bakhtiari AS, Kircher MF (2018) Multi-center study finds postoperative residual non-enhancing component of glioblastoma as a new determinant of patient outcome. J Neurooncol 139:125–133
Park JE, Kim HS, Park SY, Jung SC, Kim JH, Heo H-Y (2020) Identification of early response to anti-angiogenic therapy in recurrent glioblastoma: amide proton transfer–weighted and perfusion-weighted MRI compared with diffusion-weighted MRI. Radiology 295:397–406
Friedman HS, Prados MD, Wen PY, Mikkelsen T, Schiff D, Abrey LE, Yung WA, Paleologos N, Nicholas MK, Jensen R (2009) Bevacizumab alone and in combination with irinotecan in recurrent glioblastoma. J Clin Oncol 27:4733–4740
Gilbert MR, Dignam JJ, Armstrong TS, Wefel JS, Blumenthal DT, Vogelbaum MA, Colman H, Chakravarti A, Pugh S, Won M (2014) A randomized trial of bevacizumab for newly diagnosed glioblastoma. N Engl J Med 370:699–708
Taal W, Oosterkamp HM, Walenkamp AM, Dubbink HJ, Beerepoot LV, Hanse MC, Buter J, Honkoop AH, Boerman D, de Vos FY (2014) Single-agent bevacizumab or lomustine versus a combination of bevacizumab plus lomustine in patients with recurrent glioblastoma (BELOB trial): a randomised controlled phase 2 trial. Lancet Oncol 15:943–953
de Groot JF, Fuller G, Kumar AJ, Piao Y, Eterovic K, Ji Y, Conrad CA (2010) Tumor invasion after treatment of glioblastoma with bevacizumab: radiographic and pathologic correlation in humans and mice. Neuro Oncol 12:233–242. https://doi.org/10.1093/neuonc/nop027
Norden AD, Young GS, Setayesh K, Muzikansky A, Klufas R, Ross GL, Ciampa AS, Ebbeling LG, Levy B, Drappatz J, Kesari S, Wen PY (2008) Bevacizumab for recurrent malignant gliomas. Neurology 70:779. https://doi.org/10.1212/01.wnl.0000304121.57857.38
Stecco A, Pisani C, Quarta R, Brambilla M, Masini L, Beldi D, Zizzari S, Fossaceca R, Krengli M, Carriero A (2011) DTI and PWI analysis of peri-enhancing tumoral brain tissue in patients treated for glioblastoma. J Neurooncol 102:261–271. https://doi.org/10.1007/s11060-010-0310-x
Funding
The authors have not disclosed any funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors state that they have no conflicts of interest to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Moon, H.H., Park, J.E., Kim, YH. et al. Contrast enhancing pattern on pre-treatment MRI predicts response to anti-angiogenic treatment in recurrent glioblastoma: comparison of bevacizumab and temozolomide treatment. J Neurooncol 157, 405–415 (2022). https://doi.org/10.1007/s11060-022-03980-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-022-03980-2