Abstract
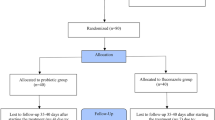
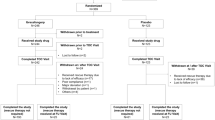
Recurrent vulvovaginal candidiasis (RVVC) is a common condition that can physically and psychologically impact patients. We compared the efficacy and safety of vaginal nystatin suppositories for 14 days each month versus standard oral fluconazole regimens for the treatment for RVVC. Patients (n = 293) were enrolled in the study from April 2010 to September 2013. After the initial therapy, the mycological cure rates were 78.3 % (119/152) and 73.8 % (104/141) in the nystatin group and fluconazole group, respectively (95 % CI, 0.749–2.197, p > 0.05). The mycological cure rates at the end of maintenance therapy were 80.7 % (96/119) and 72.7 % (72/99) in the two groups, respectively (95 % CI, 0.954–3.293, p > 0.05).The mycological cure rates at the end without treatment for 6 months were 81.25 % (78/96) and 82.19 % (60/73) in the two groups, respectively (95 % CI, 0.427–2.066, p > 0.05). The mycological cure rates of RVVC caused by C. albicans were 84.0 % (89/106) and 81.8 % (99/121) in the two groups, respectively. The mycological cure rates of RVVC caused by C. glabrata were 64.3 % (27/42) and 12.5 % (2/16) in the two groups, respectively. The initial and 6-month maintenance therapy were successful in five of the nine patients in the nystatin group with RVVC caused by fluconazole-resistant Candida, whereas in the fluconazole group, initial therapy failed in all patients with RVVC caused by fluconazole-resistant Candida (n = 7). We conclude that both fluconazole and nystatin therapies are effective in treating RVVC. Nystatin may also be effective for the treatment for RVVC caused by C. glabrata or fluconazole-resistant Candida.

Similar content being viewed by others
References
Foxman B, Muraglia R, Dietz JP, Sobel JD, Wagner J. Prevalence of recurrent vulvovaginal candidiasis in 5 European countries and the United States: results from an internet panel survey. J Low Genit Tract Dis. 2013;17(3):340–5.
Sobel JD. Genital candidiasis. Medicine. 2010;38:286–90.
Aballéa S, Guelfucci F, Wagner J, Khemiri A, Dietz JP, Sobel J, Toumi M. Subjective health status and health-related quality of life among women with recurrent vulvovaginal candidosis (RVVC) in Europe and the USA. Health Qual Life Outcomes. 2013;11:169.
Workowski KA, Berman S. Centers for disease control and prevention (CDC). Sexually transmitted diseases treatment guidelines, 2010. MMWR Recomm Rep. 2010;59:1–110.
Mendling W, Brasch J. Guideline vulvovaginal candidosis (2010) of the German Society for Gynecology and Obstetrics, the Working Group for Infections and Infectimmunology in Gynecology and Obstetrics, the German Society of Dermatology, the Board of German Dermatologists and the German Speaking Mycological Society. Mycoses. 2012;55(Suppl 3):1–13.
Colombo AL, Guimarães T, Camargo LF, Richtmann R, de Queiroz-Telles F, Salles MJ, Cunha CA, Yasuda MA, Moretti ML, Nucci M. Brazilian guidelines for the management of candidiasis: a joint meeting report of three medical societies: Sociedadebrasileira de Infectologia, Sociedade Paulista de Infectologia and SociedadeBrasileira de Medicina Tropical. Braz J Infect Dis. 2013;17:283–312.
Sobel JD, Wiesenfeld HC, Martens M, Danna P, Hooton TM, Rompalo A, Sperling M, Livengood C 3rd, Horowitz B, Von Thron J, Edwards L, Panzer H, Chu TC. Maintenance fluconazole therapy for recurrent vulvovaginal candidiasis. N Engl J Med. 2004;351:876–83.
Donders G, Bellen G, Byttebier G. Individualised decreasing-dose maintenance fluconazole regimen for recurrent vulvovaginal candidiasis (ReCiDiF trial). Am J Obstet Gynecol. 2008;199:613.e1–9.
Rosa MI, Silva BR, Pires PS, Silva FR, Silva NC, Silva FR, Souza SL, Madeira K, Panatto AP, Medeiros LR. Weekly fluconazole therapy for recurrent vulvovaginal candidiasis: a systematic review and meta-analysis. Eur J Obstet Gynecol Reprod Biol. 2013;167:132–6.
Watson C, Calabretto H. Comprehensive review of conventional and non-conventional methods of management of recurrent vulvovaginal candidiasis. Aust N Z J Obstet Gynaecol. 2007;47(4):262–72.
Rosco Diagnostica A/S. User’s guide for neo-sensitabs susceptibility testing. 19th ed. Taastrup, Denmark: Rosco Diagnostica A/S; 2007/2008.
Achkar JM, Fries BC. Candida infections of the genitourinary tract. Clin Microbiol Rev. 2010;23:253–73.
Liu XP, Fan SR, Peng YT, Zhang HP. Species distribution and susceptibility of Candida isolates from patient with vulvovaginal candidiasis in southern China from 2003 to 2012. J Mycol Med. 2014;24(2):106–11.
Richter SS, Galask RP, Messer SA, Hollis RJ, Diekema DJ, Pfaller MA. Antifungal susceptibilities of Candida species causing vulvovaginitis and epidemiology of recurrent cases. J Clin Microbiol. 2005;43:2155–62.
Shahid Z, Sobel JD. Reduced fluconazole susceptibility of Candida albicans isolates in women with recurrent vulvovaginal candidiasis: effects of long-term fluconazole therapy. Diagn Microbiol Infect Dis. 2009;64:354–6.
Marchaim D, Lemanek L, Bheemreddy S, Kaye KS, Sobel JD. Fluconazole-resistant Candida albicans vulvovaginitis. Obstet Gynecol. 2012;120(6):1407–14.
Fan SR, Liu XP. In vitro fluconazole and nystatin susceptibility and clinical outcome in complicated vulvovaginal candidosis. Mycoses. 2011;54:501–5.
Fan SR, Liu XP, Li JW. Clinical characteristics of vulvovaginal candidiasis and antifungal susceptibilities of Candida species isolates among patients in southern China from 2003 to 2006. J Obstet Gynaecol Res. 2008;34:561–6.
Witt A, Kaufmann U, Bitschnau M, Tempfer C, Ozbal A, Haytouglu E, Gregor H, Kiss H. Monthly itraconazole versus classic homeopathy for the treatment of recurrent vulvovaginal candidiasis: a randomised trial. BJOG. 2009;116:1499–505.
Sobel JD, Chaim W, Nagappan V, Leaman D. Treatment of vaginitis caused by Candida glabrata: use of topical boric acid and flucytosine. Am J Obstet Gynecol. 2003;189:1297–300.
Hale EK, Pomeranz MK. Dermatologic agents during pregnancy and lactation: an update and clinical review. Int J Dermatol. 2002;41:197–203.
Acknowledgments
This research was supported by a Shenzhen Science and Technology Grant 201201001.
Conflict of interest
The authors have no conflict of interests to declare.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Fan, S., Liu, X., Wu, C. et al. Vaginal Nystatin Versus Oral Fluconazole for the Treatment for Recurrent Vulvovaginal Candidiasis. Mycopathologia 179, 95–101 (2015). https://doi.org/10.1007/s11046-014-9827-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11046-014-9827-4