Abstract
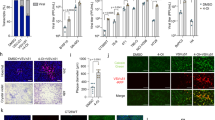
Glucocorticoid (GC) resistance is associated with poor response to the following chemotherapy in lymphoid malignancies, such as lymphoma and leukemia. However, it remains unclear whether GCs interfere with the cytotoxic effects of anti-cancer drugs on GC-resistant cells. In this study, we examined whether GCs affected the sensitivities to vincristine (VCR)/doxorubicin (DOX) and the expression of drug transporters in GC-resistant cells. The dexamethasone (DEX)/prednisolone (PSL)-resistant lymphoid and non-lymphoid cell lines Raji and HL60 were cultured with DEX for 7 days and then treated with VCR or DOX for 3 days. Seven days of DEX treatment increased the IC50s of both VCR and DOX in Raji cells but not in HL60 cells. The mRNA and protein expression levels of organic cation/carnitine transporter (OCTN) 2, one of the drug uptake transporters expressed in both cell lines, were decreased only in Raji cells. When Raji cells were cultured with PSL, the IC50 of DOX but not VCR increased as the expression of OCTN2 decreased. No significant increases in efflux transporter expression were induced by DEX or PSL. When siRNA against OCTN2 was introduced into Raji cells, the IC50 of DOX but not VCR increased significantly. These data suggested that both DEX and PSL decreased the sensitivity of the DEX/PSL-resistant Raji cells to DOX, a change that was at least partially due to reductions in OCTN2. Thus, the continuous usage of GCs may interfere with the effects of chemotherapy on GC-resistant lymphoid cells.






Similar content being viewed by others
References
Inaba H, Pui CH (2010) Glucocorticoid use in acute lymphoblastic leukaemia. Lancet Oncol 11:1096–1106. https://doi.org/10.1016/s1470-2045(10)70114-5
Renner K, Ausserlechner MJ, Kofler R (2003) A conceptual view on glucocorticoid-induced apoptosis, cell cycle arrest and glucocorticoid resistance in lymphoblastic leukemia. Curr Mol Med 3:707–717
Kato M, Koh K, Manabe A, Saito T, Hasegawa D, Isoyama K, Kinoshita A, Maeda M, Okimoto Y, Kajiwara M, Kaneko T, Sugita K, Kikuchi A, Tsuchida M, Ohara A (2014) No impact of high-dose cytarabine and asparaginase as early intensification with intermediate-risk paediatric acute lymphoblastic leukaemia: results of randomized trial TCCSG study L99-15. Br J Haematol 164:376–383. https://doi.org/10.1111/bjh.12632
Kato M, Manabe A, Koh K, Inukai T, Kiyokawa N, Fukushima T, Goto H, Hasegawa D, Ogawa C, Koike K, Ota S, Noguchi Y, Kikuchi A, Tsuchida M, Ohara A (2014) Treatment outcomes of adolescent acute lymphoblastic leukemia treated on Tokyo Children’s Cancer Study Group (TCCSG) clinical trials. Int J Hematol 100:180–187. https://doi.org/10.1007/s12185-014-1622-y
Conter V, Arico M, Valsecchi MG, Basso G, Biondi A, Madon E, Mandelli F, Paolucci G, Pession A, Rizzari C, Rondelli R, Zanesco L, Masera G (2000) Long-term results of the Italian Association of Pediatric Hematology and Oncology (AIEOP) acute lymphoblastic leukemia studies, 1982–1995. Leukemia 14:2196–2204
Felice MS, Zubizarreta PA, Alfaro EM, Sackmann-Muriel F (2001) Childhood acute lymphoblastic leukemia: prognostic value of initial peripheral blast count in good responders to prednisone. J Pediatr Hematol Oncol 23:411–415
Schrappe M, Reiter A, Zimmermann M, Harbott J, Ludwig WD, Henze G, Gadner H, Odenwald E, Riehm H (2000) Long-term results of four consecutive trials in childhood ALL performed by the ALL-BFM study group from 1981 to 1995. Leukemia 14:2205–2222
Patte C, Auperin A, Gerrard M, Michon J, Pinkerton R, Sposto R, Weston C, Raphael M, Perkins SL, McCarthy K, Cairo MS (2007) Results of the randomized international FAB/LMB96 trial for intermediate risk B-cell non-Hodgkin lymphoma in children and adolescents: it is possible to reduce treatment for the early responding patients. Blood 109:2773–2780. https://doi.org/10.1182/blood-2006-07-036673
Patte C, Auperin A, Michon J, Behrendt H, Leverger G, Frappaz D, Lutz P, Coze C, Perel Y, Raphael M, Terrier-Lacombe MJ (2001) The Societe Francaise d’Oncologie Pediatrique LMB89 protocol: highly effective multi agent chemotherapy tailored to the tumor burden and initial response in 561 unselected children with B-cell lymphomas and L3 leukemia. Blood 97:3370–3379
Arico M, Basso G, Mandelli F, Rizzari C, Colella R, Barisone E, Zanesco L, Rondelli R, Pession A, Masera G (1995) Good steroid response in vivo predicts a favorable outcome in children with T-cell acute lymphoblastic leukemia. The Associazione Italiana Ematologia Oncologia Pediatrica (AIEOP). Cancer 75:1684–1693
Dordelmann M, Reiter A, Borkhardt A, Ludwig WD, Gotz N, Viehmann S, Gadner H, Riehm H, Schrappe M (1999) Prednisone response is the strongest predictor of treatment outcome in infant acute lymphoblastic leukemia. Blood 94:1209–1217
Griffin TC, Shuster JJ, Buchanan GR, Murphy SB, Camitta BM, Amylon MD (2000) Slow disappearance of peripheral blood blasts is an adverse prognostic factor in childhood T cell acute lymphoblastic leukemia: a Pediatric Oncology Group study. Leukemia 14:792–795
Schrappe M, Arico M, Harbott J, Biondi A, Zimmermann M, Conter V, Reiter A, Valsecchi MG, Gadner H, Basso G, Bartram CR, Lampert F, Riehm H, Masera G (1998) Philadelphia chromosome-positive (Ph +) childhood acute lymphoblastic leukemia: good initial steroid response allows early prediction of a favorable treatment outcome. Blood 92:2730–2741
Schultz KR, Pullen DJ, Sather HN, Shuster JJ, Devidas M, Borowitz MJ, Carroll AJ, Heerema NA, Rubnitz JE, Loh ML, Raetz EA, Winick NJ, Hunger SP, Carroll WL, Gaynon PS, Camitta BM (2007) Risk- and response-based classification of childhood B-precursor acute lymphoblastic leukemia: a combined analysis of prognostic markers from the Pediatric Oncology Group (POG) and Children’s Cancer Group (CCG). Blood 109:926–935. https://doi.org/10.1182/blood-2006-01-024729
Tsuchida M, Ikuta K, Hanada R, Saito T, Isoyama K, Sugita K, Toyoda Y, Manabe A, Koike K, Kinoshita A, Maeda M, Ishimoto K, Sato T, Okimoto Y, Kaneko T, Kajiwara M, Sotomatsu M, Hayashi Y, Yabe H, Hosoya R, Hoshi Y, Ohira M, Bessho F, Tsunematsu Y, Tsukimoto I, Nakazawa S (2000) Long-term follow-up of childhood acute lymphoblastic leukemia in Tokyo Children’s Cancer Study Group 1981–1995. Leukemia 14:2295–2306
Bailey LC, Lange BJ, Rheingold SR, Bunin NJ (2008) Bone-marrow relapse in paediatric acute lymphoblastic leukaemia. Lancet Oncol 9:873–883. https://doi.org/10.1016/s1470-2045(08)70229-8
Riehm H, Reiter A, Schrappe M, Berthold F, Dopfer R, Gerein V, Ludwig R, Ritter J, Stollmann B, Henze G (1987) Corticosteroid-dependent reduction of leukocyte count in blood as a prognostic factor in acute lymphoblastic leukemia in childhood (therapy study ALL-BFM 83). Klin Padiatr 199:151–160. https://doi.org/10.1055/s-2008-1026781
Shnitsar V, Eckardt R, Gupta S, Grottker J, Muller GA, Koepsell H, Burckhardt G, Hagos Y (2009) Expression of human organic cation transporter 3 in kidney carcinoma cell lines increases chemosensitivity to melphalan, irinotecan, and vincristine. Cancer Res 69:1494–1501. https://doi.org/10.1158/0008-5472.can-08-2483
Okabe M, Szakacs G, Reimers MA, Suzuki T, Hall MD, Abe T, Weinstein JN, Gottesman MM (2008) Profiling SLCO and SLC22 genes in the NCI-60 cancer cell lines to identify drug uptake transporters. Mol Cancer Ther 7:3081–3091. https://doi.org/10.1158/1535-7163.mct-08-0539
Okabe M, Unno M, Harigae H, Kaku M, Okitsu Y, Sasaki T, Mizoi T, Shiiba K, Takanaga H, Terasaki T, Matsuno S, Sasaki I, Ito S, Abe T (2005) Characterization of the organic cation transporter SLC22A16: a doxorubicin importer. Biochem Biophys Res Commun 333:754–762. https://doi.org/10.1016/j.bbrc.2005.05.174
Januchowski R, Wojtowicz K, Andrzejewska M, Zabel M (2014) Expression of MDR1 and MDR3 gene products in paclitaxel-, doxorubicin- and vincristine-resistant cell lines. Biomed Pharmacother 68:111–117. https://doi.org/10.1016/j.biopha.2013.09.004
Xia CQ, Smith PG (2012) Drug efflux transporters and multidrug resistance in acute leukemia: therapeutic impact and novel approaches to mediation. Mol Pharmacol 82:1008–1021. https://doi.org/10.1124/mol.112.079129
Maeda T, Yotsumoto T, Oyabu M, Tamai I (2008) Effect of glucocorticoid receptor ligand dexamethasone on the expression of organic cation transporter in rat liver. Drug Metab Pharmacokinet 23:67–72
Gasser PJ, Lowry CA, Orchinik M (2006) Corticosterone-sensitive monoamine transport in the rat dorsomedial hypothalamus: potential role for organic cation transporter 3 in stress-induced modulation of monoaminergic neurotransmission. J Neurosci 26:8758–8766. https://doi.org/10.1523/jneurosci.0570-06.2006
Manceau S, Giraud C, Decleves X, Batteux F, Chereau C, Chouzenoux S, Scherrmann JM, Weill B, Perrot JY, Treluyer JM (2012) Expression and induction by dexamethasone of ABC transporters and nuclear receptors in a human T-lymphocyte cell line. J Chemother 24:48–55. https://doi.org/10.1179/1120009x12z.00000000010
Shikama Y, Hu H, Ohno M, Matsuoka I, Shichishima T, Kimura J (2010) Transcripts expressed using a bicistronic vector pIREShyg2 are sensitized to nonsense-mediated mRNA decay. BMC Mol Biol 11:42. https://doi.org/10.1186/1471-2199-11-42
Bachmann PS, Gorman R, Mackenzie KL, Lutze-Mann L, Lock RB (2005) Dexamethasone resistance in B-cell precursor childhood acute lymphoblastic leukemia occurs downstream of ligand-induced nuclear translocation of the glucocorticoid receptor. Blood 105:2519–2526. https://doi.org/10.1182/blood-2004-05-2023
Bachmann PS, Gorman R, Papa RA, Bardell JE, Ford J, Kees UR, Marshall GM, Lock RB (2007) Divergent mechanisms of glucocorticoid resistance in experimental models of pediatric acute lymphoblastic leukemia. Cancer Res 67:4482–4490. https://doi.org/10.1158/0008-5472.can-06-4244
Kaspers GJ, Pieters R, Van Zantwijk CH, Van Wering ER, Der Does-Van Van, Den Berg A, Veerman AJ (1998) Prednisolone resistance in childhood acute lymphoblastic leukemia: vitro-vivo correlations and cross-resistance to other drugs. Blood 92:259–266
Wei G, Twomey D, Lamb J, Schlis K, Agarwal J, Stam RW, Opferman JT, Sallan SE, den Boer ML, Pieters R, Golub TR, Armstrong SA (2006) Gene expression-based chemical genomics identifies rapamycin as a modulator of MCL1 and glucocorticoid resistance. Cancer Cell 10:331–342. https://doi.org/10.1016/j.ccr.2006.09.006
Hirai H, Murakami T, Urabe A, Takaku F (1985) Increased glucocorticoid receptor concentration in macrophage differentiation of myeloid leukemia cells with 12-O-tetradecanoylphorbol-13-acetate. Cancer Res 45:2456–2461
Piotrowska H, Jagodzinski PP (2007) Trichostatin A, sodium butyrate, and 5-aza-2′-deoxycytidine alter the expression of glucocorticoid receptor alpha and beta isoforms in Hut-78 T- and Raji B-lymphoma cell lines. Biomed Pharmacother 61:451–454. https://doi.org/10.1016/j.biopha.2007.03.007
Gu L, Xie L, Zuo C, Ma Z, Zhang Y, Zhu Y, Gao J (2015) Targeting mTOR/p70S6K/glycolysis signaling pathway restores glucocorticoid sensitivity to 4E-BP1 null Burkitt Lymphoma. BMC Cancer 15:529. https://doi.org/10.1186/s12885-015-1535-z
Molina ML, Guerrero J, Cidlowski JA, Gatica H, Goecke A (2017) LPS regulates the expression of glucocorticoid receptor alpha and beta isoforms and induces a selective glucocorticoid resistance in vitro. J Inflamm 14:22. https://doi.org/10.1186/s12950-017-0169-0
Koeffler HP, Golde DW, Lippman ME (1980) Glucocorticoid sensitivity and receptors in cells of human myelogenous leukemia lines. Cancer Res 40:563–566
Ito C, Evans WE, McNinch L, Coustan-Smith E, Mahmoud H, Pui CH, Campana D (1996) Comparative cytotoxicity of dexamethasone and prednisolone in childhood acute lymphoblastic leukemia. J Clin Oncol 14:2370–2376. https://doi.org/10.1200/jco.1996.14.8.2370
Kolbus A, Blazquez-Domingo M, Carotta S, Bakker W, Luedemann S, von Lindern M, Steinlein P, Beug H (2003) Cooperative signaling between cytokine receptors and the glucocorticoid receptor in the expansion of erythroid progenitors: molecular analysis by expression profiling. Blood 102:3136–3146. https://doi.org/10.1182/blood-2003-03-0923
Koyama Y, Ukita A, Abe K, Iwamae K, Tokuyama S, Tanaka K, Kotake Y (2017) Dexamethasone downregulates endothelin receptors and reduces endothelin-induced production of matrix metalloproteinases in cultured rat astrocytes. Mol Pharmacol 92:57–66. https://doi.org/10.1124/mol.116.107300
Zadi Heydarabad M, Nikasa M, Vatanmakanian M, Azimi A, Farshdousti Hagh M (2018) Regulatory effect of resveratrol and prednisolone on MDR1 gene expression in acute lymphoblastic leukemia cell line (CCRF-CEM): an epigenetic perspective. J Cell Biochem 119:4890–4896. https://doi.org/10.1002/jcb.26709
Silverman JA, Deitcher SR (2013) Marqibo(R) (vincristine sulfate liposome injection) improves the pharmacokinetics and pharmacodynamics of vincristine. Cancer Chemother Pharmacol 71:555–564. https://doi.org/10.1007/s00280-012-2042-4
Umsumarng S, Pitchakarn P, Sastraruji K, Yodkeeree S, Ung AT, Pyne SG, Limtrakul P (2015) Reversal of human multi-drug resistance leukaemic cells by stemofoline derivatives via inhibition of P-glycoprotein function. Basic Clin Pharmacol Toxicol 116:390–397. https://doi.org/10.1111/bcpt.12331
Styczynski J, Kurylak A, Wysocki M (2005) Cytotoxicity of cortivazol in childhood acute lymphoblastic leukemia. Anticancer Res 25:2253–2258
He B, Zhang N, Zhao R (2016) Dexamethasone downregulates SLC7A5 expression and promotes cell cycle arrest, autophagy and apoptosis in BeWo cells. J Cell Physiol 231:233–242. https://doi.org/10.1002/jcp.25076
Kullmann MK, Grubbauer C, Goetsch K, Jakel H, Podmirseg SR, Trockenbacher A, Ploner C, Cato AC, Weiss C, Kofler R, Hengst L (2013) The p27-Skp2 axis mediates glucocorticoid-induced cell cycle arrest in T-lymphoma cells. Cell Cycle 12:2625–2635. https://doi.org/10.4161/cc.25622
Wang HY, Zhang Y, Zhou Y, Lu YY, Wang WF, Xin M, Guo XL (2016) Rosiglitazone elevates sensitization of drug-resistant oral epidermoid carcinoma cells to vincristine by G2/M-phase arrest, independent of PPAR-gamma pathway. Biomed Pharmacother 83:349–361. https://doi.org/10.1016/j.biopha.2016.06.047
Sayed-Ahmed MM, Al-Shabanah OA, Hafez MM, Aleisa AM, Al-Rejaie SS (2010) Inhibition of gene expression of heart fatty acid binding protein and organic cation/carnitine transporter in doxorubicin cardiomyopathic rat model. Eur J Pharmacol 640:143–149. https://doi.org/10.1016/j.ejphar.2010.05.002
Tamai I, Ohashi R, Nezu J, Yabuuchi H, Oku A, Shimane M, Sai Y, Tsuji A (1998) Molecular and functional identification of sodium ion-dependent, high affinity human carnitine transporter OCTN2. J Biol Chem 273:20378–20382
Acknowledgements
We would like to thank Ms. Michiko Anzai (Fukushima Medical University, Fukushima, Japan) for providing technical assistance.
Funding
This study was funded by grants from the Japanese Society for the Promotion of Science Grants-in-Aid for Scientific Research (C) MO23591400 to Y.S. and MO24590325 to J.K.
Author information
Authors and Affiliations
Contributions
MA analyzed cytotoxicity, expression of transporters, effects of siRNA, and YS designed and integrated the study. TO and YM contributed to flow cytometric analyses and cytotoxicity assay. JK and MH supervised the study design and data analyses.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
In this study, neither human subjects nor animals were used.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Akaihata, M., Shikama, Y., Matsumoto, Y. et al. Glucocorticoids attenuate the sensitivity of glucocorticoid-resistant lymphoid cells to doxorubicin via reduction in OCTN2. Mol Cell Biochem 459, 49–59 (2019). https://doi.org/10.1007/s11010-019-03549-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-019-03549-0