Abstract
Objectives
We sought to identify the most common diagnostic categories linked to dispensed opioid prescriptions among children 1–36 months old and changes in patterns over the years 2000 to 2017.
Methods
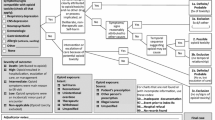
This study used South Carolina’s Medicaid claims data of pediatric dispensed outpatient opioid prescriptions between 2000 and 2017. The major opioid-related diagnostic category (indication) for each prescription was identified using visit primary diagnoses and the Clinical Classification System (AHRQ-CCS) software. The variables of interest were the rate of opioid prescriptions per 1,000 visits for each diagnostic category and the relative percentage of opioid prescriptions assigned to each category compared to all categories.
Results
Six major diagnostic categories were identified; Diseases of the respiratory system (RESP), Congenital anomalies (CONG), Injury (INJURY), Diseases of the nervous system and sense organs (NEURO), Diseases of the digestive system (GI), and Diseases of the genitourinary system (GU). The overall rate of dispensed opioid prescriptions per category declined significantly for four diagnostic categories throughout the study period, RESP by 15.13, INJURY by 8.49, NEURO by 7.33, and GI by 5.93. Two categories increased during the same time, CONG (by 9.47) and GU (by 6.98). RESP was the most prevalent category linked to a dispensed opioid prescription within 2010–2012 (almost 25%) but CONG was the most prevalent by 2014 (17.77%).
Conclusions for practice
Among Medicaid children 1–36 months old, annual dispensed opioid prescription rates declined for most major diagnostic categories (RESP, INJURY, NEURO, and GI). Future studies should explore alternatives to current opioid dispensing practices for GU and CONG cases.
Significance
Eventhough opioid is a high-risk medication for children, it is continued to be prescribed to pediatric population. A little is known about the diagnoses associated with opioid prescribing among children 1–36 months old and their trends. This study demonstrates that opioid prescriptions linked to respiratory diagnosis have become less prevalent, surpassed by opioids prescribed for surgical conditions.


Similar content being viewed by others
Data Availability
‘Not applicable’.
Code Availability
‘Not applicable’.
Abbreviations
- AHRQ:
-
Agency for Healthcare Research and Quality
- SC:
-
South Carolina
- CCS:
-
Clinical Classifications Software
- CONG:
-
Congenital anomalies
- GI:
-
Diseases of the digestive system
- GU:
-
Diseases of the genitourinary system
- INJURY:
-
Injury
- NEURO:
-
Diseases of the nervous system and sense organs
- RESP:
-
Diseases of the respiratory system
References
Anandarajan, D., Talwar, D., & Wells, L. (2019). Significant nationwide variation exists in opioid prescription Rates Amongst Pediatric patients with ACL injuries: a Restrospective Cohort Study. Orthopaedic Journal of Sports Medicine, 7(3 Suppl), 2325967119S0008. https://doi.org/10.1177/2325967119S00084.
Basco, W. T., McCauley, J. L., Zhang, J., Mauldin, P. D., Simpson, K. N., Heidari, K., Marsden, J. E., & Ball, S. J. (2021). Trends in dispensed opioid analgesic prescriptions to children in South Carolina: 2010–2017. Pediatrics, 147(3), 2010–2017. https://doi.org/10.1542/PEDS.2020-0649/-/DCSUPPLEMENTAL/.
Basco, W. T., Roberts, J. R., Ebeling, M., Garner, S. S., Hulsey, T. C., & Simpson, K. (2018). Indications for Use of Combination Acetaminophen/Opioid Drugs in Infants < 6 months old. Clinical Pediatrics, 57(6), 741. https://doi.org/10.1177/0009922817730349.
Berlin, J., McCarver-May, D. G., Notterman, D. A., Ward, R. M., Weismann, D. N., Wilson, G. S., Wilson, J. T., March, J., Bennett, D. R., Hoskins, I. A., Mulinare, J., Kaufman, P., Mithani, S., MacLeod, S. M., Troendle, G., Yaffe, S. J., Cote, C. J., & Szefler, S. J. (1997). Use of Codeine- and dextromethorphan-containing cough remedies in children. Pediatrics, 99(6), 918–920. https://doi.org/10.1542/PEDS.99.6.918.
Centers for Disease Control and Prevention (2018). CDC’s Opioid Overdose Indicator Support Toolkit: Guidance for building and reporting on opioid-related mortality, morbidity, and PDMP indicators (Versions 2.0). Atlanta, GA.
Chidambaran, V., Sadhasivam, S., & Mahmoud, M. (2017). Codeine and Opioid metabolism – implications and Alternatives for Pediatric Pain Management. Current Opinion in Anaesthesiology, 30(3), 349. https://doi.org/10.1097/ACO.0000000000000455.
Chua, K. P., Shrime, M. G., & Conti, R. M. (2017). Effect of FDA investigation on opioid prescribing to children after tonsillectomy/adenoidectomy. Pediatrics, 140(6), https://doi.org/10.1542/PEDS.2017-1765/38185.
Chung, C. P., Callahan, S. T., Cooper, W. O., Dupont, W. D., Murray, K. T., Franklin, A. D., Hall, K., Dudley, J. A., Stein, C. M., & Ray, W. A. (2018). Outpatient opioid prescriptions for children and opioid-related adverse events. Pediatrics, 142(2), https://doi.org/10.1542/PEDS.2017-2156/-/DCSUPPLEMENTAL.
Coffin, P., & Banta-Green, C. (2014). The dueling obligations of opioid stewardship. Annals of Internal Medicine, 160(3), 207–208. https://doi.org/10.7326/M13-2781.
Conradt, E., Flannery, T., Aschner, J. L., Annett, R. D., Croen, L. A., Duarte, C. S., Friedman, A. M., Guille, C., Hedderson, M. M., Hofheimer, J. A., Jones, M. R., Ladd-Acosta, C., McGrath, M., Moreland, A., Neiderhiser, J. M., Nguyen, R. H. N., Posner, J., Ross, J. L., Savitz, D. A., & Lester, B. M. (2019). Prenatal opioid exposure: neurodevelopmental Consequences and Future Research Priorities. Pediatrics, 144(3), https://doi.org/10.1542/PEDS.2019-0128.
Cramer, J. D., Barnett, M. L., Anne, S., Bateman, B. T., Rosenfeld, R. M., Tunkel, D. E., & Brenner, M. J. (2021). Nonopioid, Multimodal Analgesia as First-line Therapy after Otolaryngology Operations: primer on nonsteroidal anti-inflammatory drugs (NSAIDs). Otolaryngology - Head and Neck surgery. (United States), 164(4), 712–719. https://doi.org/10.1177/0194599820947013.
Creswell, P. D., Gibson, C., Theobald, J., & Meiman, J. G. (2019). Exposures to Opioids among Wisconsin Children and Adolescents, 2002–2016. WMJ: Official Publication of the State Medical Society of Wisconsin, 118(1), 9–15.
Defalco, F. J., Ryan, P. B., & Soledad Cepeda, M. (2013). Applying standardized drug terminologies to observational healthcare databases: a case study on opioid exposure. Health Services and Outcomes Research Methodology, 13(1), 58–67. https://doi.org/10.1007/s10742-012-0102-1.
FDA Drug Safety Communication: FDA requires labeling changes for prescription opioid cough and cold medicines to limit their use to adults 18 years and older | FDA. (n.d.). https://www.fda.gov/drugs/drug-safety-and-availability/fda-drug-safety-communication-fda-requires-labeling-changes-prescription-opioid-cough-and-cold.
Galinkin, J. L. (2011). It’s time to rethink use of codeine in pediatric patients. American Academy of Pediatrics.
Groenewald, C. B. (2019). Opioid prescribing patterns for pediatric patients in the USA. The Clinical Journal of Pain, 35(6), 515. https://doi.org/10.1097/AJP.0000000000000707.
Haffajee, R. L., Mello, M. M., Zhang, F., Zaslavsky, A. M., Larochelle, M. R., & Wharam, J. F. (2018). States with overall robust prescription drug monitoring programs experienced reductions in Opioids prescribed to commercially-insured individuals. Health Affairs (Project Hope), 37(6), 964. https://doi.org/10.1377/HLTHAFF.2017.1321.
Hudgins, J. D., Porter, J. J., Monuteaux, M. C., & Bourgeois, F. T. (2019). Trends in opioid prescribing for adolescents and young adults in ambulatory care settings. Pediatrics, 143(6), https://doi.org/10.1542/PEDS.2018-1578/76823.
IBM ® Micromedex ® RED BOOK ® Data Sheet Comprehensive drug pricing and product information. (n.d)https://www.ibm.com/products/micromedex-red-book/resources
Jones, C. M., Lurie, P., & Woodcock, J. (2014). Addressing Prescription Opioid Overdose: Data Support a Comprehensive PolicyApproach. JAMA, 312(17),1733–1734. https://doi.org/10.1001/JAMA.2014.13480
Kang, A. M., & Brooks, D. E. (2016). US poison control center calls for infants 6 months of age and younger. Pediatrics, 137(2), https://doi.org/10.1542/PEDS.2015-1865/52753.
Kelley-Quon, L. I., Kirkpatrick, M. G., Ricca, R. L., Baird, R., Harbaugh, C. M., Brady, A., Garrett, P., Wills, H., Argo, J., Diefenbach, K. A., Henry, M. C. W., Sola, J. E., Mahdi, E. M., Goldin, A. B., Peter, S., Downard, S. D., Azarow, C. D., Shields, K. S., T., & Kim, E. (2021). Guidelines for opioid prescribing in children and adolescents after surgery: an Expert Panel Opinion. JAMA Surgery, 156(1), 76–90. https://doi.org/10.1001/JAMASURG.2020.5045.
Kuehn, B. M. (2013). FDA Committee: more restrictions needed on Hydrocodone Combination Products. Journal Of The American Medical Association, 309(9), 862–862. https://doi.org/10.1001/JAMA.2013.1609.
Kuehn, B. M. (2014). CDC: Major Disparities in Opioid Prescribing among States: some States Crack down on excess prescribing. Journal Of The American Medical Association, 312(7), 684–686. https://doi.org/10.1001/JAMA.2014.9253.
Phang, K. G., Roberts, J. R., Ebeling, M., Garner, S. S., & Basco, W. T. (2020). Opioids or steroids for pneumonia or sinusitis. Pediatrics, 146(2), https://doi.org/10.1542/peds.2019-3690.
Poonai, N., Datoo, N., Ali, S., Cashin, M., Drendel, A. L., Zhu, R., Lepore, N., Greff, M., Rieder, M., & Bartley, D. (2017). Oral morphine versus ibuprofen administered at home for postoperative orthopedic pain in children: a randomized controlled trial. CMAJ: Canadian Medical Association Journal, 189(40), E1252. https://doi.org/10.1503/CMAJ.170017.
Renny, M. H., Yin, H. S., Jent, V., Hadland, S. E., & Cerdá, M. (2021). Temporal Trends in Opioid Prescribing Practices in children, adolescents, and younger adults in the US from 2006 to 2018. JAMA Pediatrics, 10016. https://doi.org/10.1001/jamapediatrics.2021.1832.
Tan, G. X., & Tunkel, D. E. (2017). Control of Pain after Tonsillectomy in Children: a review. JAMA Otolaryngology–Head & Neck Surgery, 143(9), 937–942. https://doi.org/10.1001/JAMAOTO.2017.0845.
Tierney, W. M. (2014). The dueling obligations of opioid stewardship. Annals of Internal Medicine, 161(4), 307. https://doi.org/10.7326/L14-5016-7.
Tobias, J. D., Green, T. P., & Coté, C. J. (2016). Codeine: time to say no. Pediatrics, 138(4), https://doi.org/10.1542/PEDS.2016-2396/52374.
Tomaszewski, D. M., Arbuckle, C., Yang, S., & Linstead, E. (2018). Trends in Opioid Use in Pediatric Patients in US Emergency Departments from 2006 to 2015. JAMA Network Open, 1(8), e186161–e186161. https://doi.org/10.1001/JAMANETWORKOPEN.2018.6161.
Walker, M. (2016). Kids and Pain: FDA Considers Rules for Pediatric Opioid Trials. MedPageToday. http://www.medpagetoday.com/PainManagement/PainManagement/60261
Winkelman, T. N. A., Villapiano, N., Kozhimannil, K. B., Davis, M. M., & Patrick, S. W. (2018). Incidence and costs of neonatal abstinence syndrome among infants with Medicaid: 2004–2014. Pediatrics, 141(4), https://doi.org/10.1542/PEDS.2017-3520/-/DCSUPPLEMENTAL.
Zhang, H., Kilaru, A. S., Meisel, Z. F., & Bao, Y. (2021). Prescription Drug Monitoring Program Mandates and Opioids Dispensed Following Emergency Department Encounters for Patients With Sickle Cell Disease or Cancer With Bone Metastasis. JAMA. https://doi.org/10.1001/JAMA.2021.10161
Zhu, A., Benzon, H. A., & Anderson, A., T (2017). Evidence for the efficacy of systemic opioid-sparing analgesics in Pediatric Surgical populations: a systematic review. Anesthesia and Analgesia, 125(5), 1569–1587. https://doi.org/10.1213/ANE.0000000000002434.
Acknowledgements
‘Not Applicable”.
Funding
The authors received no specific funding for this work.
Author information
Authors and Affiliations
Contributions
All authors have made substantial contributions to the conception or design of the work, including the acquisition, analysis, or interpretation of data for the work; drafting the work and revising it critically for important intellectual content; and final approval of the version to be published.
Corresponding author
Ethics declarations
Conflict of Interest
The authors in this study declare no conflict of interest.
Ethics Approval
This study was waivered as “not human research” by the IRB of the Medical University of South Carolina and Clemson University because the data were de-identified.
Consent to Participate
‘Not applicable’.
Consent for Publication
‘Not applicable’.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic Supplementary Material
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Sivaraj, L., Basco, W., Heavner, S. et al. Outpatient Opioid Dispensing Patterns for SC Medicaid Children 1–36 Months Old. Matern Child Health J 27, 1043–1050 (2023). https://doi.org/10.1007/s10995-023-03621-8
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10995-023-03621-8