Abstract
Purpose
Hyper Immunoglobulin M (HIgM) syndrome is a heterogeneous group of primary immunodeficiency disorders, characterized by recurrent infections and associated with decreased serum IgG and IgA, but normal or increased IgM. The aim of the present study was to evaluate respiratory manifestations in patients with HIgM syndrome.
Methods
A total number of 62 patients, including 46 males and 16 females were included in the present study. To investigate the respiratory complications among HIgM patients, we evaluated the clinical hospital records, immunologic and molecular diagnostic assays, pulmonary function tests (PFT), and high-resolution computed tomography (HRCT) scans.
Results
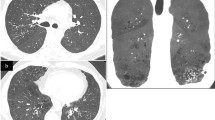
Pneumonia was the most common respiratory manifestation (n = 35, 56.4%), followed by otitis media (45.1%), sinusitis (33.8%), and bronchiectasis (14.5%). 52.1% of the patients had abnormal PFT results, with a predominant restrictive pattern of changes. HRCT scans demonstrated abnormal findings in 85.7% of patients with found mutations. Ten cases had hilar lymphadenopathy and para-hilar infiltrates in their HRCT findings. Genetic diagnosis was confirmed in 29 HIgM patients (72.4% CD40 ligand (CD40L) and 24.1% activation-induced cytidine deaminase (AICDA/AID) deficiencies). Majority of patients with CD40L (71.4%) and AID (57.1%) deficiencies had missense mutations. Pneumonia and abnormal high-resolution computed tomography (HRCT) findings were more frequent among patients with CD40L mutation. Respiratory failure constituted the major cause of mortality (37.5%) with majority of cases occurring in CD40L-deficient patients (50%).
Conclusions
Respiratory complications are common in patients with HIgM syndrome. A proper awareness of respiratory manifestations in patients with HIgM may result in improved management, reduced morbidity and mortality, and an improvement in the quality of life of the patients.



Similar content being viewed by others
References
Conley ME, Larche M, Bonagura VR, Lawton AR 3rd, Buckley RH, Fu SM, et al. Hyper IgM syndrome associated with defective CD40-mediated B cell activation. J Clin Invest. 1994;94(4):1404–9. https://doi.org/10.1172/jci117476.
Notarangelo LD, Duse M, Ugazio AG. Immunodeficiency with hyper-IgM (HIM). Immunodefic Rev. 1992;3(2):101–21.
Qamar N, Fuleihan RL. The hyper IgM syndromes. Clin Rev Allergy Immunol. 2014;46(2):120–30. https://doi.org/10.1007/s12016-013-8378-7.
Winkelstein JA, Marino MC, Ochs H, Fuleihan R, Scholl PR, Geha R, et al. The X-linked hyper-IgM syndrome: clinical and immunologic features of 79 patients. Medicine. 2003;82(6):373–84. https://doi.org/10.1097/01.md.0000100046.06009.b0.
Durandy A, Kracker S. Immunoglobulin class-switch recombination deficiencies. Arthritis Res Ther. 2012;14(4):218. https://doi.org/10.1186/ar3904.
Aghamohammadi A, Parvaneh N, Rezaei N, Moazzami K, Kashef S, Abolhassani H, et al. Clinical and laboratory findings in hyper-IgM syndrome with novel CD40L and AICDA mutations. J Clin Immunol. 2009;29(6):769–76. https://doi.org/10.1007/s10875-009-9315-7.
Hirbod-Mobarakeh A, Aghamohammadi A, Rezaei N. Immunoglobulin class switch recombination deficiency type 1 or CD40 ligand deficiency: from bedside to bench and back again. Expert Rev Clin Immunol. 2014;10(1):91–105.
Abolhassani H, Parvaneh N, Rezaei N, Hammarstrom L, Aghamohammadi A. Genetic defects in B-cell development and their clinical consequences. J Investig Allergol Clin Immunol. 2014;24(1):6–22 quiz 2 p following.
Peron S, Metin A, Gardes P, Alyanakian MA, Sheridan E, Kratz CP, et al. Human PMS2 deficiency is associated with impaired immunoglobulin class switch recombination. J Exp Med. 2008;205(11):2465–72. https://doi.org/10.1084/jem.20080789.
Leven EA, Maffucci P, Ochs HD, Scholl PR, Buckley RH, Fuleihan RL, et al. Hyper IgM Syndrome: a report from the USIDNET Registry. J Clin Immunol. 2016;36(5):490–501. https://doi.org/10.1007/s10875-016-0291-4.
Noordzij JG, Wulffraat NM, Haraldsson A, Meyts I, van't Veer LJ, Hogervorst FB, et al. Ataxia-telangiectasia patients presenting with hyper-IgM syndrome. Arch Dis Child. 2009;94(6):448–9. https://doi.org/10.1136/adc.2008.149351.
Picard C, Bobby Gaspar H, Al-Herz W, Bousfiha A, Casanova JL, Chatila T, et al. International union of immunological societies: 2017 primary mmunodeficiency diseases committee report on inborn errors of immunity. J Clin Immunol. 2018;38(1):96–128. https://doi.org/10.1007/s10875-017-0464-9.
Levy J, Espanol-Boren T, Thomas C, Fischer A, Tovo P, Bordigoni P, et al. Clinical spectrum of X-linked hyper-IgM syndrome. J Pediatr. 1997;131(1 Pt 1):47–54.
Revy P, Muto T, Levy Y, Geissmann F, Plebani A, Sanal O, et al. Activation-induced cytidine deaminase (AID) deficiency causes the autosomal recessive form of the hyper-IgM syndrome (HIGM2). Cell. 2000;102(5):565–75.
Minegishi Y, Lavoie A, Cunningham-Rundles C, Bedard PM, Hebert J, Cote L, et al. Mutations in activation-induced cytidine deaminase in patients with hyper IgM syndrome. Clin Immunol (Orlando, Fla). 2000;97(3):203–10. https://doi.org/10.1006/clim.2000.4956.
Azizi G, Abolhassani H, Rezaei N, Aghamohammadi A, Asgardoon MH, Rahnavard J, et al. The use of immunoglobulin therapy in primary immunodeficiency diseases. Endocr Metab Immune Disord Drug Targets. 2016;24(77293):EPUB-77293.
de la Morena MT. Clinical phenotypes of hyper-IgM syndromes. J Allergy Clin Immunol Pract. 2016;4(6):1023–36. https://doi.org/10.1016/j.jaip.2016.09.013.
Dosanjh A. Chronic pediatric pulmonary disease and primary humoral antibody based immune disease. Respir Med. 2011;105(4):511–4. https://doi.org/10.1016/j.rmed.2010.11.013.
Abolhassani H, Akbari F, Mirminachi B, Bazregari S, Hedayat E, Rezaei N, et al. Morbidity and mortality of Iranian patients with hyper IgM syndrome: a clinical analysis. Iran J Immunol. 2014;11(2):123–33.
de la Morena MT, Leonard D, Torgerson TR, Cabral-Marques O, Slatter M, Aghamohammadi A, et al. Long-term outcomes of 176 patients with X-linked hyper-IgM syndrome treated with or without hematopoietic cell transplantation. J Allergy Clin Immunol. 2017;139(4):1282–92.
Abolhassani H, Aghamohammadi A, Fang M, Rezaei N, Jiang C, Liu X, et al. Clinical implications of systematic phenotyping and exome sequencing in patients with primary antibody deficiency. Genet Med. 2018. https://doi.org/10.1038/s41436-018-0012-x.
Abolhassani H, Chou J, Bainter W, Platt CD, Tavassoli M, Momen T, et al. Clinical, immunologic, and genetic spectrum of 696 patients with combined immunodeficiency. J Allergy Clin Immunol. 2018;141(4):1450–8. https://doi.org/10.1016/j.jaci.2017.06.049.
Aghamohammadi A, Mohammadinejad P, Abolhassani H, Mirminachi B, Movahedi M, Gharagozlou M, et al. Primary immunodeficiency disorders in Iran: update and new insights from the third report of the national registry. J Clin Immunol. 2014;34(4):478–90. https://doi.org/10.1007/s10875-014-0001-z.
Abolhassani H, Kiaee F, Tavakol M, Chavoshzadeh Z, Mahdaviani SA, Momen T, et al. Fourth Update on the Iranian national registry of primary immunodeficiencies: integration of molecular diagnosis. J Clin Immunol. 2018;38(7):816–32. https://doi.org/10.1007/s10875-018-0556-1.
Garner JS, Jarvis WR, Emori TG, Horan TC, Hughes JM. CDC definitions for nosocomial infections, 1988. Am J Infect Control. 1988;16(3):128–40.
Bhalla M, Turcios N, Aponte V, Jenkins M, Leitman BS, McCauley DI, et al. Cystic fibrosis: scoring system with thin-section CT. Radiology. 1991;179(3):783–8.
Grenier P, Cordeau MP, Beigelman C. High-resolution computed tomography of the airways. J Thorac Imaging. 1993;8(3):213–29.
Hansell DM, Wells AU, Rubens MB, Cole PJ. Bronchiectasis: functional significance of areas of decreased attenuation at expiratory CT. Radiology. 1994;193(2):369–74. https://doi.org/10.1148/radiology.193.2.7972745.
Gharagozlou M, Ebrahimi FA, Farhoudi A, Aghamohammadi A, Bemanian MH, Chavoshzadeh Z, et al. Pulmonary complications in primary hypogammaglobulinemia: a survey by high resolution CT scan. Monaldi Arch Chest Dis. 2006;65(2):69–74.
Rusconi F, Panisi C, Dellepiane RM, Cardinale F, Chini L, Martire B, et al. Pulmonary and sinus diseases in primary humoral immunodeficiencies with chronic productive cough. Arch Dis Child. 2003;88(12):1101–5.
van Zeggeren L, van de Ven AA, Terheggen-Lagro SW, Mets OM, Beek FJ, van Montfrans JM, et al. High-resolution computed tomography and pulmonary function in children with common variable immunodeficiency. Eur Respir J. 2011;38(6):1437–43. https://doi.org/10.1183/09031936.00173410.
Serra G, Milito C, Mitrevski M, Granata G, Martini H, Pesce AM, et al. Lung MRI as a possible alternative to CT scan for patients with primary immune deficiencies and increased radiosensitivity. Chest. 2011;140(6):1581–9. https://doi.org/10.1378/chest.10-3147.
van de Ven AA, van Montfrans JM, Terheggen-Lagro SW, Beek FJ, Hoytema van Konijnenburg DP, Kessels OA, et al. A CT scan score for the assessment of lung disease in children with common variable immunodeficiency disorders. Chest. 2010;138(2):371–9. https://doi.org/10.1378/chest.09-2398.
Pereira FF, Ibiapina Cda C, Alvim CG, Camargos PA, Figueiredo R, Pedrosa JF. Correlation between Bhalla score and spirometry in children and adolescents with cystic fibrosis. Rev Assoc Med Bras (1992). 2014;60(3):216–21.
Standardization of spirometry--1987 update. Statement of the American Thoracic Society. Am Rev Respir Dis. 1987;136(5):1285–98. https://doi.org/10.1164/ajrccm/136.5.1285.
Polgar G, Promadhat V. Pulmonary function testing in children : techniques and standards. Philadelphia: Saunders; 1971.
Cabral-Marques O, Klaver S, Schimke LF, Ascendino EH, Khan TA, Pereira PV, et al. First report of the hyper-IgM syndrome Registry of the Latin American Society for Immunodeficiencies: novel mutations, unique infections, and outcomes. J Clin Immunol. 2014;34(2):146–56. https://doi.org/10.1007/s10875-013-9980-4.
Lougaris V, Badolato R, Ferrari S, Plebani A. Hyper immunoglobulin M syndrome due to CD40 deficiency: clinical, molecular, and immunological features. Immunol Rev. 2005;203:48–66. https://doi.org/10.1111/j.0105-2896.2005.00229.x.
Lopes AJ, Camilo GB, de Menezes SL, Guimaraes FS. Impact of different etiologies of bronchiectasis on the pulmonary function tests. Clin Med Res. 2015;13(1):12–9. https://doi.org/10.3121/cmr.2014.1236.
Feydy A, Sibilia J, De Kerviler E, Zagdanski AM, Chevret S, Fermand JP, et al. Chest high resolution CT in adults with primary humoral immunodeficiency. Br J Radiol. 1996;69(828):1108–16. https://doi.org/10.1259/0007-1285-69-828-1108.
Jesenak M, Banovcin P, Jesenakova B, Babusikova E. Pulmonary manifestations of primary immunodeficiency disorders in children. Front Pediatr. 2014;2:77. https://doi.org/10.3389/fped.2014.00077.
de Miranda NF, Bjorkman A, Pan-Hammarstrom Q. DNA repair: the link between primary immunodeficiency and cancer. Ann N Y Acad Sci. 2011;1246:50–63. https://doi.org/10.1111/j.1749-6632.2011.06322.x.
Yazdani R, Abolhassani H, Asgardoon M, Shaghaghi M, Modaresi M, Azizi G, et al. Infectious and noninfectious pulmonary complications in patients with primary immunodeficiency disorders. J Investig Allergol Clin Immunol. 2017;27(4):213–24. https://doi.org/10.18176/jiaci.0166.
Howard V, Greene JM, Pahwa S, Winkelstein JA, Boyle JM, Kocak M, et al. The health status and quality of life of adults with X-linked agammaglobulinemia. Clin Immunol (Orlando, Fla). 2006;118(2-3):201–8. https://doi.org/10.1016/j.clim.2005.11.002.
Resnick ES, Moshier EL, Godbold JH, Cunningham-Rundles C. Morbidity and mortality in common variable immune deficiency over 4 decades. Blood. 2012;119(7):1650–7. https://doi.org/10.1182/blood-2011-09-377945.
Brower KS, Del Vecchio MT, Aronoff SC. The etiologies of non-CF bronchiectasis in childhood: a systematic review of 989 subjects. BMC Pediatr. 2014;14:4. https://doi.org/10.1186/s12887-014-0299-y.
Haidopoulou K, Calder A, Jones A, Jaffe A, Sonnappa S. Bronchiectasis secondary to primary immunodeficiency in children: longitudinal changes in structure and function. Pediatr Pulmonol. 2009;44(7):669–75. https://doi.org/10.1002/ppul.21036.
Wood P, Stanworth S, Burton J, Jones A, Peckham DG, Green T, et al. Recognition, clinical diagnosis and management of patients with primary antibody deficiencies: a systematic review. Clin Exp Immunol. 2007;149(3):410–23. https://doi.org/10.1111/j.1365-2249.2007.03432.x.
Quartier P, Debre M, De Blic J, de Sauverzac R, Sayegh N, Jabado N, et al. Early and prolonged intravenous immunoglobulin replacement therapy in childhood agammaglobulinemia: a retrospective survey of 31 patients. J Pediatr. 1999;134(5):589–96.
Tarzi MD, Grigoriadou S, Carr SB, Kuitert LM, Longhurst HJ. Clinical immunology review series: an approach to the management of pulmonary disease in primary antibody deficiency. Clin Exp Immunol. 2009;155(2):147–55. https://doi.org/10.1111/j.1365-2249.2008.03851.x.
Jain A, Ma CA, Liu S, Brown M, Cohen J, Strober W. Specific missense mutations in NEMO result in hyper-IgM syndrome with hypohydrotic ectodermal dysplasia. Nat Immunol. 2001;2(3):223–8. https://doi.org/10.1038/85277.
Yazdani R, Abolhassani H, Kiaee F, Habibi S, Azizi G, Tavakol M, et al. Comparison of common monogenic defects in a large predominantly antibody deficiency cohort. J Allergy Clin Immunol Pract. 2018. https://doi.org/10.1016/j.jaip.2018.09.004.
Acknowledgments
We would like to thank Dr. Zamani for her contribution in the radiologic assessment of our patients.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
This study was approved by the Ethics Committee of the Tehran University of the Medical Sciences and informed consents were obtained from all patients and/or their parents.
Conflict of Interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic Supplementary Material
ESM 1
(DOCX 55 kb)
Rights and permissions
About this article
Cite this article
Moazzami, B., Yazdani, R., Azizi, G. et al. Respiratory Complications in Patients with Hyper IgM Syndrome. J Clin Immunol 39, 557–568 (2019). https://doi.org/10.1007/s10875-019-00650-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10875-019-00650-3