Abstract
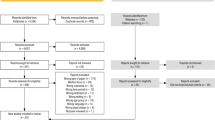
This mixed method study examined factors associated with parents not attending their child’s mental health treatment after initially seeking help for their 2–5 year old child. It was part of a larger study comparing two evidence-based treatments among low-income racial/ethnic minority families seeking child mental health services. Of 123 parents who initiated mental health treatment (71 % African American or multi-racial; 97.6 % low-income), 36 (29.3 %) never attended their child’s first treatment session. Socio-demographic characteristics, parenting stress, depression, severity of child behavior problems, and length of treatment delay from intake to first scheduled treatment session were compared for families who did and did not attend their first treatment session. Parents who never attended their child’s first treatment session were more likely to live with more than four adults and children (p = .007) and have more depressive symptoms (p = .003). Median length of treatment delay was 80 days (IQR = 55) for those who attended and 85 days (IQR = 67.5) for those who did not attend their child’s first treatment session (p = .142). Three themes emerged from caregiver interviews: (a) expectations about the treatment, (b) delays in getting help, and (c) ambivalence about research participation. Findings suggest the need to develop better strategies for addressing risk factors early in the treatment process and reducing the length of time families with adverse psychosocial circumstances must wait for child mental health treatment.
Similar content being viewed by others
References
Abidin, R. (1995). Parenting stress index: Professional manual. 3rd edn. Odessa, FL: Psychological Assessment Resources.
Achenbach, T. M., & Rescorla, L. A. (2000). Manual for the ASEBA preschool forms & profiles. Burlington, VT: University of Vermont, Research Center for Children, Youth, and Families.
Acri, M. C., Bornheimer, L. A., O’Brien, K., Sezer, S., Little, V., Cleek, A. F., & McKay, M. M. (2016). A model of integrated health care in a poverty-impacted community in New York City: Importance of early detection and addressing potential barriers to intervention implementation. Social Work in Health Care, 55(4), 314–327. doi:10.1080/00981389.2015.1137256.
Ammerman, R. T., Peugh, J. L., Teeters, A. R., Putnam, F. W., & Van Ginkel, J. B. (2016). Child maltreatment history and response to CBT treatment in depressed mothers participating in home visiting. Journal of Interpersonal Violence, 31(5), 774–791. doi:10.1177/0886260514556769.
Anderson, L. E., Chen, M. L., Perrin, J. M., & Cleave, J. V. (2015). Outpatient visit and medication prescribing for US children with mental health conditions. Journal of the American Academy of Pediatrics. doi:10.1542/peds.2015-0807.
Becker, K. D., Lee, B. R., Daleiden, E. L., Lindsey, M., Brandt, N. E., & Chorpita, B. F. (2015). The common elements of engagement in children’s mental health services: Which elements for which outcomes? Journal of Clinical Child and Adolescent Psychology, 44(1), 30–43. doi:10.1080/15374416.2013.814543.
Breland-Noble, A. M., Bell, C., & Nicolas, G. (2006). Family first: The development of an evidence-based family intervention for increasing participation in psychiatric clinical care research in depressed African American adolescents. Family Process, 45, 153–169.
Brown, S., Parker, J., & Godding, P. (2002). Administrative, clinical and ethical issues surrounding the use of waiting lists in the delivery of mental health services. Journal of Behavioral Health Services & Research, 29, 217–228.
Children’s Hospital Association Survey (2012). Pediatric specialist physician shortages affect access to care. https://www.childrenshospitals.org/issues-andadvocacy/graduate-medical-education/fact-sheets/2012/pediatric-specialistphysicianshortages-affect-access-to-care.
Clemente, C., McGrath, R., Stevenson, C., & Barnes, J. (2006). Evaluation of a waiting list initiative in a child and adolescent mental health service. Child and Adolescent Mental Health, 11(2), 98–103.
Coker, A. D., Huang, H., & Kashubeck-West, S. (2009). Research with African Americans: Lessons learned about recruiting African American women. Journal of Multicultural Counseling and Development, 37(3), 153–165. doi:10.1002/j.2161-1912.2009.tb00099.x.
Creswell, J. W., & Plano Clark, V. L. (2010). Designing and conducting mixed methods research. 2nd edn. Thousand Oaks, CA: Sage Publications.
Davis, D. W., Myers, J., Logsdon, M. C., & Bauer, N. S. (2015). The relationship among caregiver depressive symptoms, parenting behavior, and family-centered care. Journal of Pediatric Health Care. doi:10.1016/j.pedhc.2015.06.004.
Dempster, R., Davis, D. W., Faye Jones, V., Keating, A., & Wildman, B. (2015). The role of stigma in parental help-seeking for perceived child behavior problems in urban, low-income African American parents. Journal of Clinical Psychology in Medical Settings. doi:10.1007/s10880-015-9433-8.
Dempster, R., Wildman, B., & Keating, A. (2013). The role of stigma in parental help-seeking for child behavior problems. Journal of Clinical Child and Adolescent Psychology, 42, 56–67.
Edin, K. J., & Schaefer, H. L. (2015). $2.00 a day: Living on almost nothing in America. New York: Houghton Mifflin Harcourt Publishing Company.
Ell, K., Katon, W., Xie, B., Lee, P. J., Kapetanovic, S., Guterman, J., & Chou, C. P. (2010). Collaborative care management of major depression among low-income, predominantly Hispanic subjects with diabetes: A randomized controlled trial. Diabetes Care, 33, 706–713.
Giorgi, A., & Giorgi, B. (2003). The descriptive phenomenological psychological method. In P. M. Camic, J. E. Rhodes, & L. Yardley (Eds.), Qualitative research in psychology: Expanding perspectives in methodology and design (pp. 243–273). Washington, DC: American Psychological Association.
Gopalan, G., Goldstein, L., Klingenstein, K., Sicher, C., Blake, C., & McKay, M. M. (2010). Engaging families in child mental health treatment: Updates and special considerations. Journal of the Canadian Academy of Child & Adolescent Psychiatry, 19(3), 182–196.
Gordon, M., Antshel, K. M., Lewandowski, L., & Seigers, D. (2010). Predictors of missed appointments over the course of child mental health treatment. Psychiatric Services, 61(7), 657–659.
Gross, D. A., Belcher, H. M. E., Ofonedu, M. E., Breitenstein, S., Frick, K. D., & Budhathoki, C. (2014). Study protocol for a comparative effectiveness trial of two parent training programs in a fee-for-service mental health clinic: Can we improve mental health services to low-income families? Trials, 15, 70 doi:10.1186/1745-6215-15-70.
Gross, D., Fogg, L., Young, M., Ridge, A., Cowell, J. M., Richardson, R., & Sivan, A. (2006). The equivalence of the child behavior checklist/1½ across parent race/ethnicity, income level, and language. Psychological Assessment, 18(3), 313–323.
Haine-Schlagel, R., & Walsh, N. E. (2015). A review of parent participate engagement in child and family mental health treatment. Clinical Child and Family Psychological Review, 18, 133–150.
Harrison, M. E., McKay, M. M., & Bannon, W. J. (2004). Inner-city child mental health service use: The real question is why youth and families do not use services. Community Mental Health Journal, 40(2), 119–131. doi:10.1023/B:COMH.0000022732.80714.8b.
Hay, D. F., Pawlby, S., Waters, C. S., & Sharp, D. (2008). Antepartum and postpartum exposure to maternal depression: Different effects on different adolescent outcomes. Journal of Child Psychology and Psychiatry, 49(10), 1079–1088.
Ho, C. P., Zinski, A., Fogger, S. A., Peters, J. D., Westfall, A. O., Mugavero, M. J., Lawrence, S. T., et al. (2015). Factors associated with missed psychiatry visits in an urban HIV clinic. AIDS and Behavior, 19(8), 1423–1429.
Hodgkinson, S., Beers, L., Southammakosane, C., & Lewin, A. (2014). Addressing the mental health needs of pregnant and parenting adolescents. Pediatrics, 133(1), 114–122. doi:10.1542/peds.2013-0927.
Husserl, E. (1900/1970). Logical Investigation (trans: Findlay, J. N.). New York: Humanities Press.
Ingoldsby, E. M. (2010). Review of interventions to improve family engagement and retention in parent and child mental health programs. Journal of Child and Family Studies, 19, 629–645.
Institute of Medicine. (2015a). Transforming health care scheduling and access: getting to now. Washington, DC: National Academy Press.
Institute of Medicine. (2015b). Opportunities to promote children’s behavioral health: Health care reform and beyond. Washington, DC: National Academy Press.
Larson, J., dosReis, S., Stewart, M., Kushner, R., Frosch, E., & Solomon, B. (2013). Barriers to mental health care for urban, lower income families referred from pediatric primary care. Administration and Policy in Mental Health and Mental Health Services Research, 40, 159–167.
Lindsey, M. A., Brandt, N. E., Becker, K. D., Lee, B. R., Barth, R. P., Daleiden, E. L., & Chorpita, B. F. (2014). Identifying the common elements of treatment engagement interventions in children’s mental health services. Clinical Child and Family Psychology Review, 17(3), 283–298. doi:10.1007/s10567-013-0163-x.
Lindsey, M. A., Chambers, K., Pohle, C., Beall, P., & Lucksted, A. (2013). Understanding the behavioral determinants of mental health service use by urban, under-resourced Black youth: Adolescent and caregiver perspectives. Journal of Child and Family Studies, 22(1), 107–121. doi:10.1007/s10826-012-9668-z.
McGurran, J., & Noseworthy, T. (2002). Improving the management of waiting lists for elective health care service: public perspectives on proposed solutions. Hospital Quarterly, 5(3), 28–32.
McKay, M. M., & Bannon, W. J. (2004). Engaging families in child mental health services. Child and Adolescent Psychiatric Clinics of North America, 13(4), 905–921. doi:10.1016/j.chc.2004.04.001.
McKay, M. M., Lynn, C. J., & Bannon, W. M. (2005). Understanding inner city child mental health need and trauma exposure: Implications for preparing urban service providers. American Journal of Orthopsychiatry, 75(2), 201–210. doi:10.1037/0002-9432.75.2.201.
McKay, M. M., McCadam, K., & Gonzales, J. J. (1996). Addressing the barriers to mental health services for inner city children and their caretakers. Community Mental Health Journal, 32(4), 353–361.
Mendez, J. L., Carpenter, J. L., LaForett, D. R., & Cohen, J. S. (2009). Parental engagement and barriers to participation in a community-based preventive intervention. American Journal of Community Psychology, 44, 1–14.
Murphy, S. M., Zweifach, J., & Hoffman, L. (2012). The everyday concerns of mothers of young children and the motivation to seek ongoing parenting support from experts. Early Child Development and Care, 182(9), 1125–1137. doi:10.1080/03004430.2011.597505.
Nock, M. K., & Ferriter, C. (2005). Parent management of attendance and adherence in child and adolescent therapy: A conceptual and empirical review. Clinical Child and Family Psychology Review, 8(2), 149–166. doi:10.1007/s10567-005-4753-0.
Nock, M. K., & Kazdin, A. E. (2005). Randomized controlled trial of a brief intervention for increasing participation in parent management training. Journal of Consulting and Clinical Psychology, 73, 872–879.
Ofonedu, M. E., Percy, W. H., Harris-Britt, A., & Belcher, H. M. (2013). Depression in inner city African American youth: a phenomenological study. Journal of Child and Family Studies, 22(1), 96–106. doi:10.1007/s10826-012-9583-3.
Oslin, D. W., Ross, J., Sayers, S., Murphy, J., Kane, V., & Katz, I. R. (2006). Screening, assessment, and management of depression in VA primary care clinics: the behavioral health laboratory. Journal of General Internal Medicine, 21, 46–50.
Paterson, W. G., Depew, W. T., Pare, P., Petrunia, D., Switzer, C., Veldhuyzen van Zanten, S. J., & Daniels, S. (2006). Canadian consensus on medically acceptable wait times for digestive health care. Canadian Journal of Gastroenterology, 20(6), 411–423.
Pawlby, S., Hay, D., Sharp, D., Waters, C. S., & Pariante, C. M. (2011). Antenatal depression and offspring psychopathology: The influence of childhood maltreatment. British Journal of Psychiatry, 199(2), 106–112. doi:10.1192/bjp.bp.110.087734.
Popp, T. K., Spinrad, T. L., & Smith, C. L. (2008). The relation of cumulative demographic risk to mothers’ responsivity and control: Examining the role of toddler temperament. Infancy, 13(5), 496–518. doi:10.1080/15250000802329446.
Reitman, D., Currier, R. O., & Stickle, T. R. (2002). A critical evaluation of the parenting stress index-short form (PSI-SF) in a head start population. Journal of Clinical Child and Adolescent Psychology, 31(3), 384–392.
Satcher, D. (2001). Mental health: culture, race, and ethnicity—a supplement to mental health: a report of the surgeon general. Rockville, MD: U.S. Department of Health and Human Services, Substance Abuse and Mental Health Services Administration, Center for Mental Health Services.
Staudt, M. (2007). Treatment engagement with caregivers of at-risk children: Gaps in research and conceptualization. Journal of Child and Family Studies, 16(2), 183–196. doi:10.1007/s10826-006-9077-2.
Staudt, M., Lodato, G., & Hickman, C. R. (2012). Therapists talk about the engagement process. Community Mental Health Journal, 48(2), 212–218. doi:10.1007/s10597-011-9377-x.
Swartz, H. A., Shear, M. K., Greeno, C., Wren, F. J., Sales, E., Sullivan, B. K., & Ludewig, D. P. (2005). Depression and anxiety among mothers bringing their children to a pediatric mental health clinic. Psychiatric Services, 56, 1077–1083.
Swartz, H. A., Zuckoff, A., Frank, E., Spielvogle, H. N., Shear, M. K., Fleming, M. D., & Scott, J. (2006). An open-label trial of enhanced brief interpersonal psychotherapy in depressed mothers whose children are receiving psychiatric treatment. Depression and Anxiety, 23(7), 398–404. doi:10.1002/da.20212.
Thompson, R., Dancy, B. L., Wiley, T. A., Najdowski, C. J., Perry, S. P., Wallis, J., & Knafl, K. A. (2013). African American families’ expectations and intentions for mental health services. Administration and Policy in Mental Health and Mental Health Services Research, 40(5), 371–383. doi:10.1007/s10488-012-0429-5.
Van Dam, N. T., & Earleywine, M. (2011). Validation of the center for epidemiologic studies depression scale-revised (CESD-R): Pragmatic depression assessment in the general population. Psychiatry Research, 186(1), 128–132. doi:10.1016/j.psychres.2010.08.018.
Weissman, M. M., Pilowsky, D. J., Wickramaratne, P. J., Talati, A., Wisniewski, S. R., Fava, M., & Hughes, C. W. (2006). Remissions in maternal depression and child psychopathology: A STAR*D-child report. Journal of the American Medical Association, 295, 1389–1398.
Westin, A. M. L., Barksdale, C. L., & Stephan, S. H. (2014). The effect of waiting time on youth engagement to evidence based treatments. Community Mental Health Journal, 50, 221–228.
Wilcox, H. C., Rains, M., Belcher, H., Kassam-Adams, N., Kazak, A., Lee, R., et al. (2016). Behavioral problems and service utilization in children with chronic illnesses referred for trauma-related mental health services. Journal of Developmental and Behavioral Pediatrics, 37(1), 62–70. doi:10.1097/DBP.0000000000000236.
Williams, M., Latta, J., & Conversano, P. (2008). Eliminating the wait for mental health services. The Journal of Behavioral Health Services and Research, 35(1), 107–114.
Acknowledgments
Research reported in this publication was supported by the National Institute of Nursing Research of the National Institutes of Health under award #R01 NR012444. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health. The authors give special thanks to the families and children who participated in this study, Jasmine Gilmore for her assistance with the qualitative data analysis, and Melissa Kurtz and Kellie Miller for their assistance with data collection.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Ofonedu, M.E., Belcher, H.M.E., Budhathoki, C. et al. Understanding Barriers to Initial Treatment Engagement among Underserved Families Seeking Mental Health Services. J Child Fam Stud 26, 863–876 (2017). https://doi.org/10.1007/s10826-016-0603-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10826-016-0603-6