Abstract
Purpose
To determine the recurrence risk and risk factors for monozygotic splitting after elective single-embryo transfers (eSET).
Methods
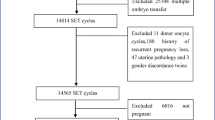
A retrospective cohort study was performed investigating 65,664 eSET cycles that resulted in a clinical pregnancy as reported in the Society for Assisted Reproductive Technology (SART) Clinical Outcomes Reporting System (CORS) between 2004 and 2017. Monozygosity was defined as more than one fetal heart tone by the first-trimester ultrasound and concordant sex at live birth. The primary outcome was recurrence risk, with recurrence defined as one patient having two or more cycles of eSET resulting in monozygotic multiples. The secondary objective was to identify factors associated with smonozygotic splitting, using a multivariable logistic regression model and a stepwise purposeful model selection.
Results
There were 1355 (2.05%) pregnancies that resulted in two or more fetal heart tones after SET, including 840 monozygotic twins and triplets at birth. Recurrence occurred in two cases—0.0001% of patients with multiple eSET cycles. One case resulted from embryos created from a single cohort with intracytoplasmic sperm injection (ICSI), assisted hatching (AH), and blastocyst transfers. The second case resulted from donor egg embryos with ICSI and blastocyst transfers. Risk factors associated with monozygotic live birth were blastocyst transfer (OR 1.23, 95% CI 1.04–1.47, P = 0.0176) and AH (OR 1.23, 95% CI 1.05–1.44, P = 0.0081).
Conclusion
Recurrence of monozygotic live births in eSET was very rare. Blastocyst transfer and AH were confirmed to be risk factors for monozygotic live births, while ICSI, PGT, and FET do not appear to be associated.

Similar content being viewed by others
References
Ryan GL, Zhang SH, Dokras A, Syrop CH, Van Voorhis BJ. The desire of infertile patients for multiple births. Fertil Steril. 2004;81(3):500–4.
Gleicher N, Barad D. Twin pregnancy, contrary to consensus, is a desirable outcome in infertility. Fertil Steril. 2009;91(6):2426–31.
Child TJ, Henderson AM, Tan SL. The desire for multiple pregnancy in male and female infertility patients. Hum Reprod. 2004;19(3):558–61.
Knopman JM, Krey LC, Oh C, Lee J, McCaffrey C, Noyes N. What makes them split? Identifying risk factors that lead to monozygotic twins after in vitro fertilization. Fertil Steril. 2014;102(1):82–9.
Glazebrook C, Sheard C, Cox S, Oates M, Ndukwe G. Parenting stress in first-time mothers of twins and triplets conceived after in vitro fertilization. Fertil Steril. 2004;81(3):505–11.
Ellison MA, Hotamisligil S, Lee H, Rich-edwards JW, Pang SC, Hall JE. Psychosocial risks associated with multiple births resulting from assisted reproduction. Fertil Steril. 2005;83(5):1422–8.
Practice Committee of the American Society for Reproductive Medicine and the Practice Committee for the Society for Assisted Reproductive Technologies. Electronic address: ASRM@asrm.org. Guidance on the limits to the number of embryos to transfer: a committee opinion. Fertil Steril. 2021;116(3):651–654.
Centers for Disease Control and Prevention, American Society for Reproductive Medicine, Society for Assisted Reproductive Technology. 2015 Assisted Reproductive Technology National Summary Report. Atlanta (GA): US Dept of Health and Human Services. 2017
Kanter JR, Boulet SL, Kawwass JF, Jamieson DJ, Kissin DM. Trends and correlates of monozygotic twinning after single embryo transfer. Obstet Gynecol. 2015;125(1):111–7.
Vega M, Zaghi S, Buyuk E, Jindal S. Not all twins are monozygotic after elective single embryo transfer: analysis of 32,600 elective single embryo transfer cycles as reported to the Society for Assisted Reproductive Technology. Fertil Steril. 2018;109(1):118–22.
Vitthala S, Gelbaya TA, Brison DR, Fitzgerald CT, Nardo LG. The risk of monozygotic twins after assisted reproductive technology: a systematic review and meta-analysis. Hum Reprod Update. 2009;15(1):45–55.
Fellman J, Eriksson AW. Weinberg’s differential rule reconsidered. Hum Biol. 2006;78(3):253–75.
Chang HJ, Lee JR, Jee BC, Suh CS, Kim SH. Impact of blastocyst transfer on offspring sex ratio and the monozygotic twinning rate: a systematic review and meta-analysis. Fertil Steril. 2009;91(6):2381–90.
Knopman J, Krey LC, Lee J, Fino ME, Novetsky AP, Noyes N. Monozygotic twinning: an eight-year experience at a large IVF center. Fertil Steril. 2010;94(2):502–10.
Shapiro LR, Zemek L, Shulman MJ. Genetic etiology for monozygotic twinning. Birth Defects Orig Artic Ser. 1978;14(6A):219–22.
Ikemoto Y, Kuroda K, Ochiai A, et al. Prevalence and risk factors of zygotic splitting after 937 848 single embryo transfer cycles. Hum Reprod. 2018;33(11):1984–91.
Blickstein I, Jones C, Keith LG. Zygotic-splitting rates after single-embryo transfers in in vitro fertilization. N Engl J Med. 2003;348(23):2366–7.
Nakasuji T, Saito H, Araki R, et al. The incidence of monozygotic twinning in assisted reproductive technology: analysis based on results from the 2010 Japanese ART national registry. J Assist Reprod Genet. 2014;31(7):803–7.
Osianlis T, Rombauts L, Gabbe M, Motteram C, Vollenhoven V. Incidence and zygosity of twin births following transfers using a single fresh or frozen embryo. Hum Reprod. 2014;29(7):1438–43.
Fellman J, Eriksson AW. Weinberg’s differential rule reconsidered. Hum Biol. 2006;78(3):253–75.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
This study was reviewed by the Institutional Review Board of the University of Rochester and determined to be not human subject research; therefore, the IRB review and approval were not required.
Conflict of interest
The authors declare no competing interests. WV is a consultant for Turtle Health and Siemens Diagnostics. DL’s time at the University of Rochester is supported in part by the University of Rochester CTSA award number UL1 TR002001 from the National Center for Advancing Translational Sciences of the National Institutes of Health.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Chu, C.S., Li, D., Olson-Chen, C. et al. Recurrence risk and risk factors for monozygotic twin and triplet birth in over 65,000 single-embryo transfers. J Assist Reprod Genet 40, 851–855 (2023). https://doi.org/10.1007/s10815-023-02737-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-023-02737-8