Abstract
Purpose
Proliferative diabetic retinopathy (PDR) can be treated by retinal photocoagulation, but in some cases, the treatment is initiated too late or is insufficient so that the disease advances to a stage requiring vitrectomy. There is a need to identify risk factors that can predict if patients with PDR will develop complications in need for vitrectomy.
Methods
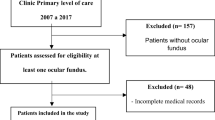
Survival analysis with death as competing risk was used to study systemic risk factors for PDR progression to a complication in need for vitrectomy in right eyes of all 1288 diabetic patients from the Aarhus area, Denmark, who had developed proliferative retinopathy in the right eye during the 25 years period from 1 July 1994 until 1 July 2019.
Results
The overall cumulative incidence of reaching a vitrectomy end point in the right eye was 24.1% (n = 311). In 9.3% (n = 120) of the patients where vitrectomy had been performed together with the first photocoagulation, the age of onset of diabetes was significantly higher (p < 0.0001), the diabetes duration longer (p < 0.035) and BMI higher (p < 0.01) than in the patients who had been vitrectomized later than the first photocoagulation. The risk for vitrectomy was significantly increased by high variability of HbA1c before the development of PDR (p < 0.0001), but not by other parameters known to increase the risk for developing PDR.
Conclusion
Increasing variability of HbA1c before the development of PDR increases the risk for progression to a complication in need of vitrectomy. The need for vitrectomy is unaffected by other risk factors known to increase the risk for developing PDR.

Similar content being viewed by others
References
Fong DS, Aiello L, Gardner TW et al (2004) Retinopathy in diabetes. Diabetes Care 10:2540–2553
Wong TY, Sun J, Kawasaki R et al (2018) Guidelines on diabetic eye care: the international council of ophthalmology recommendations for screening, follow-up, referral, and treatment based on resource settings. Ophthalmology 125(10):1608–1622
The diabetic retinopathy vitrectomy study research group (1988) Early vitrectomy for severe proliferative diabetic retinopathy in eyes with useful vision. Results of a randomized trial–diabetic retinopathy vitrectomy study report 3. Ophthalmology 95:1307–1320
The diabetic retinopathy vitrectomy study research group (1988) Early vitrectomy for severe proliferative diabetic retinopathy in eyes with useful vision. Clinical application of results of a randomized trial–diabetic retinopathy vitrectomy study report 4. Ophthalmology 95:1321–1334
Ostri C, la Cour M, Lund-Andersen H (2014) Diabetic vitrectomy in a large type 1 diabetes population: long-term incidence and risk factors. Acta Ophthalmol 92(5):439–443
Parikh R, Shah RJ, VanHouten JP et al (2014) Ocular findings at initial panretinal photocoagulation for proliferative diabetic retinopathy predict the need for future pars plana vitrectomy. Retina 34(10):1977–2000
Khan R, Surya J, Rajalakshmi R et al (2020) Need for vitreous surgeries in proliferative diabetic retinopathy in 10 years follow-up: India retinal disease study (IRDS) group report no2. Ophthalmic Res 64(3):432–439. https://doi.org/10.1159/000512767
Bek T (2020) Systemic risk factors contribute differently to the development of proliferative diabetic retinopathy and clinically significant macular oedema. Diabetologia 63(11):2462–2470
Bek T, Erlandsen M (2006) Visual prognosis after panretinal photocoagulation for proliferative diabetic retinopathy. Acta Ophthalmol 84(1):16–20
Bek T, Møller F, Klausen B (2000) Short term visual prognosis after retinal laser photocoagulation for diabetic maculpathy. Acta Ophthalmol 78(5):539–542
Jackson TL, Nicod E, Angelis A et al (2017) Pars plana vitrectomy for diabetic macular edema: a systematic review, meta-analysis, and synthesis of safety literature. Retina 37(5):886–895
Holladay JT (2004) Visual acuity measurements. J Cat Refract Surg 30:287–290
Silva PS, Diala PA, Haman R et al (2014) Visual outcomes from pars plana vitrectomy versus combined pars plana vitrectomy, phacoemulsification, and intraocular lens implantation in patients with diabetes. Retina 34(10):1960–1968
Wu L, Berrocal MH, Rodriquez FJ et al (2014) Intraocular pressure elevation after uncomplicated pars plana vitrectomy: results of the pan americal collaborative retina study group. Retina 34(10):1985–1989
Bek T, Stefánsson E, Hardarson SH (2019) Retinal oxygen saturation is an independent risk factor for the severity of diabetic retinopathy. Br J Ophthalmol 103(8):1167–1172
Song YS, Nagaoka T, Omae T et al (2016) Systemic risk factors in bilateral proliferative diabetic retinopathy requiring vitrectomy. Retina 36(7):1309–1313
Ometto G, Assheton P, Calivas F et al (2017) Spatial distribution of early red lesions is a risk factor for development of vision-threatening diabetic retinopathy. Diabetologia 60:2361–2367
Yorston D, Wickham L, Benson S et al (2008) Predictive clinical features and outcomes of vitrectomy for proliferative diabetic retinopathy. Br J Ophthalmol 92(3):365–368
Huang CT, Hsieh YT, Yang CM (2017) Vitrectomy for complications of proliferative diabetic retinopathy in young adults: clinical features and surgical outcomes. Graefes Arch Clinc Exp Ophthalmol 255(5):863–871
Hove M, Kristensen JK, Lauritzen T et al (2004) The prevalence of retinopathy in an unselected population of type 2 diabetes patients from Aarhus County Denmark. Acta Ophthalmol 82(4):443–448
Voigt M, Schmidt S, Legmann T et al (2018) Prevalence and progression rate of diabetic retinopathy in type 2 diabetes patients in correlation with the duration of diabetes. Exp Clin Endocrinol Diabetes 126(9):570–576
Slieker RC, van der Heijden AAWH, Nijpels G et al (2019) Visit-to-visit variability of glycemia and vascular complications: the hoorn diabetes care system cohort. Cardiovasc Diabetol 18(1):170. https://doi.org/10.1186/s12933-019-0975-1
Bek T (2020) Incidence and risk for developing proliferative diabetic retinopathy after photocoagulation for diabetic maculopathy. Curr Eye Res 45(8):986–991
Jørgensen CM, Bek T (2016) The systemic blood pressure and oxygen saturation in retinal arterioles predict the effect of intravitreal anti-VEGF treatment on diabetic maculopathy. Invest Ophthalmol Vis Sci 57:5429–5434
Mehlsen J, Erlandsen M, Poulsen PL et al (2011) Identification of independent risk factors for the development of diabetic retinopathy requiring treatment. Acta Ophthalmol 89(6):515–521
Sivaprasad S, Pearce E (2019) The unmet need for better risk stratification of non-proliferative diabetic retinopathy. Diabet Med 36(4):424–433
Cruickshanks KJ, Moss SE, Klein R et al (1995) Physical activity and the risk of progression of retinopathy or the development of proliferative diabetic retinopathy. Ophthalmology 102(8):1177–1182
Praidou A, Harris M, Niakas D et al (2017) Physical activity and its correlations to diabetic retinopathy. Diabetes Complicat 31(2):456–461
Hainsworth DP, Bebu I, Aiello LP et al (2019) Risk factors for retinopathy in type 1 diabetes: the DCCT/EDIC study. Diabetes Care 42(5):875–882
Aiello LP, Cahill MT, Wong JS (2001) Systemic considerations in the management of diabetic retinopathy. Am J Ophthalmol 132(5):760–766
Noor AKCM, Tai ELM, Kueh YC et al (2020) Survival time of visual gains after diabetic vitrectomy and its relationship with ischemic heart disease. Int J Environ Res Public Health 17(1):310
Acknowledgements
The skillful assistance of nurse photographers Helle Hedegaard and Tina Bjerre is gratefully acknowledged.
Funding
None.
The material is not available because this would imply the delivery of material that might identify individual patients.
Author information
Authors and Affiliations
Contributions
Toke Bek conceived the study, performed the statistical analyses and wrote the draft manuscript. All authors contributed to the data collection, interpretation of results and commented on previous versions of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interest to disclose.
Institutional board approvals
At request, the medical ethics committee stated that the reporting of anonymized data in the present study does not require consent from patients or ethical approval.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Bek, T., Nielsen, M.S., Klug, S.E. et al. Increasing metabolic variability increases the risk for vitrectomy in proliferative diabetic retinopathy. Int Ophthalmol 42, 757–763 (2022). https://doi.org/10.1007/s10792-021-02041-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-021-02041-3