Abstract
Background
Hepatic ischemia reperfusion (HIR) leads to a lung inflammatory response and subsequent pulmonary barrier dysfunction. The gap junction communication protein connexin 32 (Cx32), which is widely expressed in the lungs, participates in intercellular signaling. This study determined whether the communication protein Cx32 could affect pulmonary inflammation caused by HIR.
Methods
Mice were randomly allocated into four groups (n = 8/group): (i) Cx32+/+ sham group; (ii) Cx32+/+ HIR model group; (iii) Cx32−/− sham group; and (iv) Cx32−/− HIR model group. Twenty-four hours after surgery, lung tissues were collected for bright field microscopy, western blot (Cx32, JAK2, p-JAK2, STAT3, p-STAT3), and immunofluorescence (ZO-1, 8-OHDG) analyses. The collected bronchoalveolar fluid was tested for levels of interleukin-6 (IL-6), matrix metalloproteinase 12 (MMP-12), and antitrypsin (α1-AT). Lung mmu-miR-26a/b expression was detected using a PCR assay.
Results
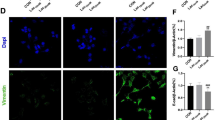
Increased expression of Cx32 mRNA and protein was noted in the lungs after HIR. Cx32 deletion significantly aggravated pulmonary function from acute lung injury induced by HIR. In addition, Cx32 deletion decreased the protein level of ZO-1 (pulmonary function) and increased the level of the oxidative stress marker 8-OHDG in the lungs. Moreover, in the Cx32−/− HIR model group, the levels of IL-6 and MMP-12 in bronchoalveolar lavage fluid were significantly increased leading to activation of the JAK2/STAT3 pathway, and decreased α1-AT levels. Furthermore, we found mmu-miR-26a/b was significantly downregulated in the Cx32−/− HIR model group.
Conclusion
HIR leads to acute lung inflammatory injury. Cx32 deletion aggravates hepatic-derived lung inflammation, partly through blocking the transferring of mmu-miR-26a/b and leading to IL-6-related JAK2/STAT3 pathway activation.









Similar content being viewed by others
References
Douzinas EE, Livaditi O, Tasoulis MK, et al. Nitrosative and oxidative stresses contribute to post-ischemic liver injury following severe hemorrhagic shock: the role of hypoxemic resuscitation. PLoS ONE. 2012;7:e32968.
Darnis B, Mohkam K, Schmitt Z, et al. Subtotal hepatectomy in swine for studying small-for-size syndrome and portal inflow modulation: is it reliable? HPB (Oxford). 2015;17:881–888.
Madadi-Sanjani O, Kuebler JF, Dippel S, et al. Long-term outcome and necessity of liver transplantation in infants with biliary atresia are independent of cytokine milieu in native liver and serum. Cytokine. 2018;111:382–388.
Ulger BV, Erbis H, Turkcu G, et al. Nebivolol ameliorates hepatic ischemia/reperfusion injury on liver but not on distant organs. J Invest Surg. 2015;28:245–252.
Mikrou A, Kalimeris KA, Lilis I, et al. Molecular studies of the immunological effects of the sevoflurane preconditioning in the liver and lung in a rat model of liver ischemia/reperfusion injury. Mol Immunol. 2016;72:1–8.
Lepere V, Vanier A, Loncar Y, et al. Risk factors for pulmonary complications after hepatic resection: role of intraoperative hemodynamic instability and hepatic ischemia. BMC Anesthesiol. 2017;17:84.
Li GZ, Sloane JL, Lidsky ME, et al. Simultaneous diaphragm and liver resection: a propensity-matched analysis of postoperative morbidity. J Am Coll Surg. 2013;216:402–411.
Li X, Wei X, Chen C, et al. N-Acetylcysteine inhalation improves pulmonary function in patients received liver transplantation. Biosci Rep. 2018;38:pii: BSR20180858.
Ge M, Chen C, Yao W, et al. Overexpression of Brg1 alleviates hepatic ischemia/reperfusion-induced acute lung injury through antioxidative stress effects. Oxid Med Cell Longev. 2017;2017:8787392.
Sperber J, Lipcsey M, Larsson A, et al. Evaluating the effects of protective ventilation on organ-specific cytokine production in porcine experimental postoperative sepsis. BMC Pulm Med. 2015;15:60.
Coulon P, Landisman CE. The potential role of gap junctional plasticity in the regulation of state. Neuron. 2017;93:1275–1295.
Freund-Michel V, Muller B, Marthan R, et al. Expression and role of connexin-based gap junctions in pulmonary inflammatory diseases. Pharmacol Ther. 2016;164:105–119.
Losa D, Chanson M, Crespin S. Connexins as therapeutic targets in lung disease. Expert Opin Ther Targets. 2011;15:989–1002.
Okamoto T, Akiyama M, Takeda M, et al. Connexin32 is expressed in vascular endothelial cells and participates in gap-junction intercellular communication. Biochem Biophys Res Commun. 2009;382:264–268.
Okamoto T, Akiyama M, Takeda M, et al. Connexin32 protects against vascular inflammation by modulating inflammatory cytokine expression by endothelial cells. Exp Cell Res. 2011;317:348–355.
Zhang Y, Yuan D, Yao W, et al. Hyperglycemia aggravates hepatic ischemia reperfusion injury by inducing chronic oxidative stress and inflammation. Oxid Med Cell Longev. 2016;2016:3919627.
Yao W, Li H, Luo G, et al. SERPINB1 ameliorates acute lung injury in liver transplantation through ERK1/2-mediated STAT3-dependent HO-1 induction. Free Radic Biol Med. 2017;108:542–553.
He Y, Ye ZQ, Li X, et al. Alpha7 nicotinic acetylcholine receptor activation attenuated intestine-derived acute lung injury. J Surg Res. 2016;201:258–265.
Miyajima A, Ohashi H, Fujishiro A, et al. Effects of all trans-retinoic acid on alveolar regeneration in dexamethasone-induced emphysema models and its relationship to exposure in ICR and FVB mice. Biol Pharm Bull. 2016;39:927–934.
Li H, Yao W, Liu Z, et al. Hyperglycemia abrogates ischemic postconditioning cardioprotection by impairing AdipoR1/Caveolin-3/STAT3 signaling in diabetic rats. Diabetes. 2015;65:942–955.
Zhao W, Zhou S, Yao W, et al. Propofol prevents lung injury after intestinal ischemia-reperfusion by inhibiting the interaction between mast cell activation and oxidative stress. Life Sci. 2014;108:80–87.
Chi X, Yao W, Zhang A, et al. Downregulation of lung toll-like receptor 4 could effectively attenuate liver transplantation-induced pulmonary damage at the early stage of reperfusion. Mediators Inflamm. 2015;2015:383907.
Yao W, Luo G, Zhu G, et al. Propofol activation of the Nrf2 pathway is associated with amelioration of acute lung injury in a rat liver transplantation model. Oxid Med Cell Longev. 2014;2014:258567.
Luo G, Zhu G, Yuan D, et al. Propofol alleviates acute lung injury following orthotopic autologous liver transplantation in rats via inhibition of the NADPH oxidase pathway. Mol Med Rep. 2015;11:2348–2354.
Luo GJ, Yao WF, He Y, et al. Ulinastatin prevents acute lung injury led by liver transplantation. J Surg Res. 2015;193:841–848.
Colletti LM, Kunkel SL, Walz A, et al. Chemokine expression during hepatic ischemia/reperfusion-induced lung injury in the rat. The role of epithelial neutrophil activating protein. J Clin Invest. 1995;95:134–141.
Nastos C, Kalimeris K, Papoutsidakis N, et al. Global consequences of liver ischemia/reperfusion injury. Oxid Med Cell Longev. 2014;2014:906965.
Yu Z, Tong Y, Zhang R, et al. Saquinavir ameliorates liver warm ischemia-reperfusion-induced lung injury via HMGB-1- and P38/JNK-Mediated TLR-4-dependent signaling pathways. Mediators Inflamm. 2017;2017:7083528.
Schulz R, Gorge PM, Gorbe A, et al. Connexin 43 is an emerging therapeutic target in ischemia/reperfusion injury, cardioprotection and neuroprotection. Pharmacol Ther. 2015;153:90–106.
O’Donnell JJ III, Birukova AA, Beyer EC, et al. Gap junction protein connexin43 exacerbates lung vascular permeability. PLoS One. 2014;9:e100931.
Rignault S, Haefliger JA, Waeber B, et al. Acute inflammation decreases the expression of connexin 40 in mouse lung. Shock. 2007;28:78–85.
Duffy HS, Iacobas I, Hotchkiss K, et al. The gap junction protein connexin32 interacts with the Src homology 3/hook domain of discs large homolog 1. J Biol Chem. 2007;282:9789–9796.
Proboszcz M, Paplinska-Goryca M, Nejman-Gryz P, et al. A comparative study of sTREM-1, IL-6 and IL-13 concentration in bronchoalveolar lavage fluid in asthma and COPD: a preliminary study. Adv Clin Exp Med. 2017;26:231–236.
Ruwanpura SM, Mcleod L, Miller A, et al. Interleukin-6 promotes pulmonary emphysema associated with apoptosis in mice. Am J Respir Cell Mol Biol. 2011;45:720–730.
Chen M, Liu Y, Yi D, et al. Tanshinone IIA promotes pulmonary artery smooth muscle cell apoptosis in vitro by inhibiting the JAK2/STAT3 signaling pathway. Cell Physiol Biochem. 2014;33:1130–1138.
Fujimoto E, Sato H, Shirai S, et al. Connexin32 as a tumor suppressor gene in a metastatic renal cell carcinoma cell line. Oncogene. 2005;24:3684–3690.
Hong X, Sin WC, Harris AL, et al. Gap junctions modulate glioma invasion by direct transfer of microRNA. Oncotarget. 2015;6:15566–15577.
Yang X, Liang L, Zhang XF, et al. MicroRNA-26a suppresses tumor growth and metastasis of human hepatocellular carcinoma by targeting interleukin-6-Stat3 pathway. Hepatology. 2013;58:158–170.
Funding
The study was supported in part by grants from Natural Science Foundation of China (No.81974081 and No.81601724 for Weifeng Yao; No.81974296 and No.81772127 and No. 81571926 for Ziqing Hei; No.81770649 for Gangjian Luo) and the Science and Technology Project of Guangdong Province (No. 2019A1515011852 to Weifeng Yao) the Young Teacher Training Program of Sun Yat-sen University, China (Grant no. 19ykpy23 for Weifeng Yao).
Author information
Authors and Affiliations
Contributions
Zheng Zhang and Weifeng Yao participated in research design, data collection, and data analysis and wrote the manuscript. Ziqing Hei and Gangjian Luo participated in research design, data collection, and data analysis. Dongdong Yuan, Fei Huang, Yue Liu participated in data collection and data analysis. All authors participated meaningfully in the study and have seen and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Zhang, Z., Yao, W., Yuan, D. et al. Effects of Connexin 32-Mediated Lung Inflammation Resolution During Liver Ischemia Reperfusion. Dig Dis Sci 65, 2914–2924 (2020). https://doi.org/10.1007/s10620-019-06020-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-019-06020-8