Abstract
Purpose
Potential risk of adverse obstetrical outcomes has been shown among breast cancer survivors. Therefore, the aim of this systematic review and meta-analysis was to evaluate the relationship between history of breast cancer (BC) and obstetrical outcomes.
Methods
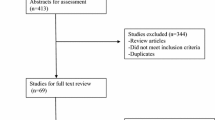
PubMed, EMBASE, and Medline were searched from the inception of each database to April 2019. Selection criteria included prospective and retrospective cohort studies of BC pregnant survivors. The meta-analysis was performed by computing odds ratios (ORs) using both fixed and random-effects models. Quality assessment of the included studies was performed using the Newcastle–Ottawa Scale and the review was registered with PROSPERO number CRD42019127716.
Results
Four studies, including 1466 cases of BC survivors and 6,912,485 controls, were included. Compared with controls, a higher incidence of obstetrical complication was found in women with history of BC. The incidence of preterm birth (PTB) in the study group was 11.05% compared with 7.79% in the control group (1.68, 95% confidence interval 1.43–1.99). Breast cancer history was also associated with low birth weight (LBW) (study group: 9.26% vs. control group: 5.54%, 1.88, CI 95% 1.55–2.27), cesarean section (CS) (study group: 19.76% vs. control group 10.81%, 1.78, CI 95% 1.39–2.27), intrauterine fetal death (IUFD) (study group: 0.004% vs. control group 0.36%, of 1.25 CI 95% 0.36–4.35), and fetal anomalies (study group: 5.8% vs. control group: 4.26%, 1.45 CI 95% 1.01–2.09).
Conclusions
History of BC was associated with adverse obstetrical outcomes.






Similar content being viewed by others
Abbreviations
- BC:
-
Breast cancer
- PTB:
-
Preterm birth
- LBW:
-
Low birth weight
- CS:
-
Cesarean section
- IUFD:
-
Intrauterine fetal death
- NOS:
-
Newcastle–Ottawa Scale
- ORs:
-
Odds ratios
- CIs:
-
Confidence intervals
- MeSH:
-
Relevant medical subject heading
References
World Cancer Research Fund International (2015) Breast cancer statistics [Internet]. http://www.wcrf.org. Accessed 3 March 2019
Ferlay J, Soerjomataram I, Ervik M, Dikshit R, Eser S, Mathers C, Rebelo M, Parkin DM, Forman D, Bray F (2013) GLOBOCAN 2012 v1.0, Cancer Incidence and Mortality Worldwide: IARC CancerBase No. 11 [Internet]. International Agency for Research on Cancer, Lyon. http://globocan.iarc.fr. Accessed 2 March 2019
Torre LA, Siegel RL, Ward EM, Jemal A (2016) Global cancer incidence and mortality rates and trends—an update. Cancer Epidemiol Biomarkers Prev 25(1):16–27
Ginsburg O, Bray F, Coleman MP et al (2016) The global burden of women’s cancers: a grand challenge in global health. Lancet 389:847–860. https://doi.org/10.1016/S0140-6736(16)31392-7
DeSantis CE, Fedewa SA, Goding Sauer A, Kramer JL, Smith RA, Jemal A (2016) Breast cancer statistics, 2015: convergence of incidence rates between black and white women. Cancer J Clin 66(1):31–42. https://doi.org/10.3322/caac.21320
Howlader NNA, Krapcho M, Miller D, Bishop K, Altekruse SF, Kosary CL, Yu M, Ruhl J, Tatalovich Z, Mariotto A, Lewis DR, Chen HS, Feuer EJ, Cronin KA (2016) Cancer Statistics Review, 1975^2013çSEER Statistics. Based on November 2015 SEER data submission. https://seer.cancer.gov/csr/1975_2013/. Accessed 3 February 2019
Estimated Number of New Cases for the Four Major Cancers by Sex and Age Group (2018) American Cancer Society, Surveillance Research. https://www.cancer.org/content/dam/cancer-org/research/cancer-facts-and-statistics/annual-cancer-facts-and-figures/2018/estimated-number-of-new-cases-for-the-four-major-cancers-by-sex-and-age-group-2018.pdf. Accessed 13 Dec 2018
Kroman N, Jensen M-B, Wohlfahrt J, Ejlertsen B, Danish Breast Cancer Cooperative Group (2008) Pregnancy after treatment of breast cancer—a population-based study on behalf of Danish Breast Cancer Cooperative Group. Acta Oncol Stockh Swed 47:545–549. https://doi.org/10.1080/02841860801935491
Shah NM, Scott DM, Kandagatla P, Moravek MB, Cobain EF, Burness ML et al (2019) Young women with breast cancer: fertility preservation options and management of pregnancy-associated breast cancer. Ann Surg Oncol. https://doi.org/10.1245/s10434-019-07156-7
Langagergaard V, Gislum M, Skriver MV et al (2006) Birth outcome in women with breast cancer. Br J Cancer 94:142–146. https://doi.org/10.1038/sj.bjc.6602878
Dalberg K, Eriksson J, Holmberg L (2006) Birth outcome in women with previously treated breast cancer—a population-based cohort study from Sweden. PLoS Med 3:e336. https://doi.org/10.1371/journal.pmed.0030336
Langagergaard V (2010) Birth outcome in women with breast cancer, cutaneous malignant melanoma, or Hodgkin’s disease: a review. Clin Epidemiol 3:7–19. https://doi.org/10.2147/CLEP.S12190
Ramírez-Torres N, Robles-Robles AG, Villafaña-Vázquez VH et al (2010) Breast cancer and subsequent pregnancy. Infertility, death risk and survival [in Spanish]. Ginecol Obstet Mex 78:85–93
Henderson LK, Craig JC, Willis NS, Tovey D, Webster AC (2010) How to write a Cochrane systematic review. Nephrology (Carlton) 15:617–624. https://doi.org/10.1111/j.1440-1797.2010.01380.x
NHS Centre for Reviews and Dissemination (2009) Systematic reviews: CRD’s guidance forundertaking reviews in health care. University of York, York. https://www.york.ac.uk/media/crd/Systematic_Reviews.pdf. Retrieved from 3 Dec 2016
Welch V, Petticrew M, Petkovic J et al (2016) Extending the PRISMA statement to equity-focused systematic reviews (PRISMA-E 2012): explanation and elaboration. J Clin Epidemiol 70:68–89. https://doi.org/10.1016/j.jclinepi.2015.09.001
Stewart LA, Clarke M, Rovers M et al (2015) Preferred reporting items for systematic review and meta-analyses of individual participant data: the PRISMA-IPD statement. JAMA 313:1657–1665. https://doi.org/10.1001/jama.2015.3656
Wells GA, Shea B, O’Connell D, et al (2018) The Newcastle-Ottawa Scale (NOS) for assessing the quality of non randomised studies in meta-analyses. Ottawa Hospital Research Institute, Ottawa. http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp. Accessed 27 Feb 2018
Higgins JPT, Thompson SG, Deeks JJ, Altman DJ (2003) Measuring inconsistency in meta-analyses. BMJ 327:557–560. https://doi.org/10.1136/bmj.327.7414.557
Egger M, Smith GD, Phillips AN (1997) Meta-analysis: principles and procedures. BMJ 315(7121):1533–1537. https://doi.org/10.1136/bmj.315.7121.1533
Begg CB, Mazumdar M (1994) Operating characteristics of a rank correlation test for publication bias. Biometrics 50:1088–1101
Jacob L, Kalder M, Arabin B, Kostev K (2017) Impact of prior breast cancer on mode of delivery and pregnancy-associated disorders: a retrospective analysis of subsequent pregnancy outcomes. J Cancer Res Clin Oncol 143:1069–1074. https://doi.org/10.1007/s00432-017-2352-3
Hartnett KP, Ward KC, Kramer MR, Lash TL, Mertens AC, Spencer JB, Fothergill A, Howards PP (2017) The risk of preterm birth and growth restriction in pregnancy after cancer. Int J Cancer 141(11):2187–2196. https://doi.org/10.1002/ijc.30914
Iqbal J, Amir E, Rochon PA, Giannakeas V, Sun P, Narod SA (2017) Association of the timing of pregnancy with survival in women with breast cancer. JAMA Oncol 3(5):659–665. https://doi.org/10.1001/jamaoncol.2017.0248
Azim HA Jr, Kroman N, Paesmans M et al (2013) Prognostic impact of pregnancy after breast cancer according to estrogen receptor status: a multicenter retrospective study. J Clin Oncol 31:73. https://doi.org/10.1200/JCO.2012.44.2285
Black KZ, Nichols HB, Eng E, Rowley DL (2017) Prevalence of preterm, low birthweight, and small for gestational age delivery after breast cancer diagnosis: a population-based study. Breast Cancer Res 19(1):11. https://doi.org/10.1186/s13058-017-0803-z
Romero R, Espinoza J, Goncalves LF, Kusanovic JP, Friel L, Hassan S (2007) The role of inflammation and infection in preterm birth. Semin Reprod Med 25(1):21–39. https://doi.org/10.1055/s-2006-956773
Hakim FT, Cepeda R, Kaimei S et al (1997) Constraints on CD4 recovery postchemotherapy in adults: thymic insufficiency and apoptotic decline of expanded peripheral CD4 cells. Blood 90(9):3789–3798
Wiser I, Orr N, Kaufman B et al (2010) Immunosuppressive treatments reduce long-term immunity to smallpox among patients with breast cancer. J Infect Dis 201(10):1527–1534. https://doi.org/10.1086/651950
Signorello LB, Mulvihill JJ, Green DM et al (2010) Stillbirth and neonatal death in relation to radiation exposure before conception: a retrospective cohort study. Lancet 376:624. https://doi.org/10.1016/S0140-6736(10)60752-0
Winther JF, Olsen JH, Wu H et al (2012) Genetic disease in the children of Danish survivors of childhood and adolescent cancer. J Clin Oncol 30:27. https://doi.org/10.1200/JCO.2011.35.0504
Signorello LB, Mulvihill JJ, Green DM et al (2012) Congenital anomalies in the children of cancer survivors: a report from the childhood cancer survivor study. J Clin Oncol 30:239. https://doi.org/10.1200/JCO.2011.37.2938
Green DM, Peabody EM, Nan B et al (2002) Pregnancy outcome after treatment for Wilms tumor: a report from the National Wilms Tumor Study Group. J Clin Oncol 20:2506. https://doi.org/10.1200/jco.2002.07.159
Ståhl O, Boyd HA, Giwercman A et al (2011) Risk of birth abnormalities in the offspring of men with a history of cancer: a cohort study using Danish and Swedish national registries. J Natl Cancer Inst 103:398. https://doi.org/10.1093/jnci/djq550
Witt KL, Bishop JB (1996) Mutagenicity of anticancer drugs in mammalian germ cells. Mutat Res 355(1–2):209–234
Braems G, Denys H, De Wever O, Cocquyt V, Van den Broecke R (2011) Use of tamoxifen before and during pregnancy. Oncologist 16(11):1547–1551
Momen NC, Ernst A, Arendt LH et al (2017) Maternal cancer and congenital anomalies in children—a Danish nationwide cohort study. PLoS ONE 12(3):e0173355
Funding
No specific funding was obtained.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
D’Ambrosio, V., Vena, F., Di Mascio, D. et al. Obstetrical outcomes in women with history of breast cancer: a systematic review and meta-analysis. Breast Cancer Res Treat 178, 485–492 (2019). https://doi.org/10.1007/s10549-019-05408-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10549-019-05408-4