Abstract
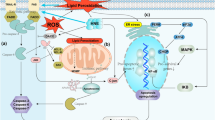
Among the properties of lactoferrin (LF) are bactericidal, antianemic, immunomodulatory, antitumour, antiphlogistic effects. Previously we demonstrated its capacity to stabilize in vivo HIF-1-alpha and HIF-2-alpha, which are redox-sensitive multiaimed transcription factors. Various tissues of animals receiving recombinant human LF (rhLF) responded by expressing the HIF-1-alpha target genes, hence such proteins as erythropoietin (EPO), ceruloplasmin, etc. were synthesized in noticeable amounts. Among organs in which EPO synthesis occurred were brain, heart, spleen, liver, kidneys and lungs. Other researchers showed that EPO can act as a protectant against severe brain injury and status epilepticus in rats. Therefore, we tried rhLF as a protector against the severe neurologic disorders developed in rats, such as the rotenone-induced model of Parkinson’s disease and experimental autoimmune encephalomyelitis as a model of multiple sclerosis, and observed its capacity to mitigate the grave symptoms. Moreover, an intraperitoneal injection of rhLF into mice 1 h after occlusion of the medial cerebral artery significantly diminished the necrosis area measured on the third day in the ischaemic brain. During this period EPO was synthesized in various murine tissues. It was known that EPO induces nuclear translocation of Nrf2, which, like HIF-1-alpha, is a transcription factor. In view that under conditions of hypoxia both factors demonstrate a synergistic protective effect, we suggested that LF activates the Keap1/Nrf2 signaling pathway, an important link in proliferation and differentiation of normal and malignant cells. J774 macrophages were cultured for 3 days without or in the presence of ferric and ferrous ions (RPMI-1640 and DMEM/F12, respectively). Then cells were incubated with rhLF or Deferiprone. Confocal microscopy revealed nuclear translocation of Nrf2 (the key event in Keap1/Nrf2 signaling) induced by apo-rhLF (iron-free, RPMI-1640). The reference compound Deferiprone (iron chelator) had the similar effect. Upon iron binding (in DMEM/F12) rhLF did not activate the Keap1/Nrf2 pathway. Added to J774, apo-rhLF enhanced transcription of Nrf2-dependent genes coding for glutathione S-transferase P and heme oxygenase-1. Western blotting revealed presence of Nrf2 in mice brain after 6 days of oral administration of apo-rhLF, but not Fe-rhLF or equivalent amount of PBS. Hence, apo-LF, but not holo-LF, induces the translocation of Nrf2 from cytoplasm to the nucleus, probably due to its capacity to induce EPO synthesis.







Similar content being viewed by others
Abbreviations
- ARE:
-
Anti-oxidant response element
- BLOTTO-T:
-
3% solution of dry skimmed milk in PBS containing 0.05% Tween 20
- CS:
-
Clinical score
- DFP:
-
Deferriprone
- EAE:
-
Experimental autoimmune encephalomyelitis
- EGM:
-
Encephalitogenic mixture
- EPO:
-
Erythropoietin
- GA:
-
Glatiramer acetate
- Gstp1:
-
Glutathione S-transferase P
- HIF:
-
Hypoxia-inducible factor
- HO-1:
-
Heme oxygenase-1
- Keap 1:
-
Kelch-like ECH-associated protein 1
- LF:
-
Lactoferrin
- MCAO:
-
Medial cerebral artery occlusion
- Nrf2:
-
Nuclear factor erythroid 2-related factor 2
- rhLF:
-
Recombinant human lactoferrin
- TTC:
-
Tri-phenyltetrasolium-2,3,5 chloride
- PBS:
-
Phosphate buffered saline i.e., 150 mM NaCl, 10 mM Na-phosphate buffer, pH 7.4
References
Abdurasulova IN, Serdyuk SE, Gmiro VE (2007) Comparative study of preventive and therapeutic effects of IEM-1966 and memantine in rats with experimental allergic encephalomyelitis. Bull Exp Biol Med 144(2):217–220. https://doi.org/10.1007/s10517-007-0293-6
Agnello D, Bigini P, Villa P, Mennini T, Cerami A, Brines ML, Ghezzi P (2002) Erythropoietin exerts an anti-inflammatory effect on the CNS in a model of experimental autoimmune encephalomyelitis. Brain Res 952(1):128–134. https://doi.org/10.1016/S0006-8993(02)03239-0
Alnaeeli M, Raaka BM, Gavrilova O, Teng R, Chanturiya T, Noguchi CT (2014) Erythropoietin signaling: a novel regulator of white adipose tissue inflammation during diet-induced obesity. Diabetes 63(7):2415–2431. https://doi.org/10.2337/db13-0883
Amini AA, Nair LS (2011) Lactoferrin: a biologically active molecule for bone regeneration. Curr Med Chem 18(8):1220–1229. https://doi.org/10.2174/092986711795029744
Amini AA, Nair LS (2013) Evaluation of the bioactivity of recombinant human lactoferrins toward murine osteoblast-like cells for bone tissue engineering. Tissue Eng Part A 19(9–10):1047–1055. https://doi.org/10.1089/ten.TEA.2012.0227
Amini AA, Nair LS (2014) Recombinant human lactoferrin as a biomaterial for bone tissue engineering: mechanism of antiapoptotic and osteogenic activity. Adv Healthc Mater 3(6):897–905. https://doi.org/10.1002/adhm.201300496
Ammarguellat F, Gogusev J, Drüeke TB (1996) Direct effect of erythropoietin on rat vascular smooth-muscle cell via a putative erythropoietin receptor. Nephrol Dial Transplant 11(4):687–692. https://doi.org/10.1093/ndt/11.4.687
Anagnostou A, Liu Z, Steiner M, Chin K, Lee ES, Kessimian N, Noguchi CT (1994) Erythropoietin receptor mRNA expression in human endothelial cells. Proc Natl Acad Sci USA 91:3974–3978. http://www.jstor.org/stable/2364574
Anderson NL, Nance SL, Pearson TW, Anderson NG (1982) Specific antiserun staining of two-dimensional electrophoretic patterns of human plasma proteins immobilized on nitricellulose. Electrophoresis 3:135–142. https://doi.org/10.1002/elps.1150030304
Appelhoff RJ, Tian YM, Raval RR, Turley H, Harris AL, Pugh CW, Ratcliffe PJ, Gleadle JM (2004) Differential function of the prolyl hydroxylases PHD1, PHD2, and PHD3 in the regulation of hypoxia-inducible factor. J Biol Chem 279:38458–38465. https://doi.org/10.1074/jbc.M406026200
Ayton S, Lei P, Mclean C, Bush AI, Finkelstein DI (2016) Transferrin protects against Parkinsonian neurotoxicity and is deficient in Parkinson’s substantia nigra. Signal Transduct Target Ther 1:16015. https://doi.org/10.1038/sigtrans.2016.15
Bartels C, Späte K, Krampe H, Ehrenreich H (2008) Recombinant human erythropoietin: novel strategies for neuroprotective/neuro-regenerative treatment of multiple sclerosis. Ther Adv Neurol Disord 1(3):193–206. https://doi.org/10.1177/1756285608098422
Bond WS, Rex TS (2014) Evidence that erythropoietin modulates neuroinflammation through differential action on neurons, astrocytes, and microglia. Front Immunol 5:523. https://doi.org/10.3389/fimmu.2014.00523
Bradford MM (1976) A rapid and sensitive method for the quantitation of microgram quantities of protein utilizing the principle of protein-dye binding. Anal Biochem 72:248–254. https://doi.org/10.1016/0003-2697(76)90527-3
Brines M, Cerami A (2005) Emerging biological roles for erythropoietin in the nervous system. Nat Rev Neurosci 6:484–494. https://doi.org/10.1038/nrn1687
Brines M, Cerami A (2006) Discovering erythropoietin’s extra-hematopoietic functions: biology and clinical promise. Kidney Int 70:246–250. https://doi.org/10.1038/sj.ki.5001546
Brines M, Cerami A (2008) Erythropoietin-mediated tissue protection: reducing collateral damage from the primary injury response. J Intern Med 264(5):405–432. https://doi.org/10.1111/j.1365-2796.2008.02024.x
Brines M, Cerami A (2013) Erythropoietin and engineered innate repair activators. Methods Mol Biol 982:1–11. https://doi.org/10.1007/978-1-62703-308-4_1
Bruick RK, McKnight SL (2001) A conserved family of prolyl-4-hydroxylases that modify HIF. Science 294(5545):1337–1340. https://doi.org/10.1126/science.1066373
Buemi M, Cavallaro E, Floccari F, Sturiale A, Aloisi C, Trimarchi M, Grasso G, Corica F, Frisina N (2002) Erythropoietin and the brain: from neurodevelopment to neuroprotection. Clin Sci 103:275–282. https://doi.org/10.1042/cs1030275
Chavez JC, Baranova O, Lin J, Pichiule P (2006) The transcriptional activator hypoxia inducible factor 2 (HIF-2/EPAS-1) regulates the oxygen-dependent expression of erythropoietin in cortical astrocytes. J Neurosci 26(37):9471–9481. https://doi.org/10.1523/JNEUROSCI.2838-06.2006
Chen X, Wang CC, Song SM, Wei SY, Li JS, Zhao SL, Li B (2015a) The administration of erythropoietin attenuates kidney injury induced by ischemia/reperfusion with increased activation of Wnt/β-catenin signaling. J Formos Med Assoc 114(5):430–437. https://doi.org/10.1016/j.jfma.2015.01.007
Chen Y, Zheng Z, Zhu X, Shi Y, Tian D, Zhao F, Liu N, Hüppi PS, Troy FA 2nd, Wang B (2015b) Lactoferrin promotes early neurodevelopment and cognition in postnatal piglets by upregulating the BDNF signaling pathway and polysialylation. Mol Neurobiol 52(1):256–269. https://doi.org/10.1007/s12035-014-8856-9
Choi M, Son H (2013) Effects of serotonin on erythropoietin expression in mouse hippocampus. Exp Neurobiol 22:45–50. https://doi.org/10.5607/en.2013.22.1.45
Choi D, Schroer SA, Lu SY, Wang L, Wu X, Liu Y, Zhang Y, Gaisano HY, Wagner KU, Wu H, Retnakaran R, Woo M (2010) Erythropoietin protects against diabetes through direct effects on pancreatic beta cells. J Exp Med 207(13):2831–2842. https://doi.org/10.1084/jem.20100665
Chong Z, Kang J-Q, Maiese K (2003) Erythropoietin: cytoprotection in vascular and neuronal cells. Curr Drug Targets 3:141–154. https://doi.org/10.2174/1568006033481483
Chong ZZ, Li F, Maiese K (2005) Erythropoietin requires NF-kappaB and its nuclear translocation to prevent early and late apoptotic neuronal injury during beta-amyloid toxicity. Curr Neurovasc Res 2(5):387–399. https://doi.org/10.2174/156720205774962683
Cornish J, Naot D (2010) Lactoferrin as an effector molecule in the skeleton. Biometals 23(3):425–430. https://doi.org/10.1007/s10534-010-9320-6
Cutone A, Frioni A, Berlutti F, Valenti P, Musci G, Bonaccorsi di Patti MC (2014) Lactoferrin prevents LPS-induced decrease of the iron exporter ferroportin in human monocytes/macrophages. Biometals 27(5):807–813. https://doi.org/10.1007/s10534-014-9742-7
Diaz Z, Assaraf MI, Miller WH Jr, Schipper HM (2005) Astroglial cytoprotection by erythropoietin pre-conditioning: implications for ischemic and degenerative CNS disorders. J Neurochem 93(2):392–402. https://doi.org/10.1111/j.1471-4159.2005.03038.x
Engelmayer J, Blezinger P, Varadhachary A (2008) Talactoferrin stimulates wound healing with modulation of inflammation. J Surg Res 149(2):278–286. https://doi.org/10.1016/j.jss.2007.12.754
Erbaş O, Çınar BP, Solmaz V, Çavuşoğlu T, Ateş U (2015) The neuroprotective effect of erythropoietin on experimental Parkinson model in rats. Neuropeptides 49:1–5. https://doi.org/10.1016/j.npep.2014.10.003
Fling SP, Gregerson DS (1986) Peptide and protein molecular weight determination by electrophoresis using a high-molarity tris buffer system without urea. Anal Biochem 155:83–88. https://doi.org/10.1016/0003-2697(86)90228-9
Garcia P, Speidel V, Scheuer C, Laschke MW, Holstein JH, Histing T, Pohlemann T, Menger MD (2011) Low dose erythropoietin stimulates bone healing in mice. J Orthop Res 29(2):165–172. https://doi.org/10.1002/jor.21219
García-Montoya IA, Cendón TS, Arévalo-Gallegos S, Rascón-Cruz Q (2012) Lactoferrin a multiple bioactive protein: an overview. Biochim Biophys Acta 1820(3):226–236. https://doi.org/10.1016/j.bbagen.2011.06.018
Genc S, Kuralay F, Genc K, Akhisaroglu M, Fadiloglu S, Yorukoglu K, Fadiloğlu M, Gure A (2001) Erythropoietin exerts neuroprotection in 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine-treated C57/BL mice via increasing nitric oxide production. Neurosci Lett 298:139–141. https://doi.org/10.1016/S0304-3940(00)01716-X
Genc S, Koroglu TF, Genc K (2003) Erythropoietin as a novel neuroprotectant. Restor Neurol Neurosci 22:105–119
Genc K, Genc S, Baskin H, Semin I (2006) Erythropoietin decreases cytotoxicity and nitric oxide formation induced by inflammatory stimuli in rat oligodendrocytes. Physiol Res 55(1):33–38
Genc K, Egrilmez MY, Genc S (2010) Erythropoietin induces nuclear translocation of Nrf2 and heme oxygenase-1 expression in SH-SY5Y cells. Cell Biochem Funct 28:197–201. https://doi.org/10.1002/cbf.1639
Ghezzi P, Brines M (2004) Erythropoietin as an antiapoptotic, tissue-protective cytokine. Cell Death Differ 11:S37–S44. https://doi.org/10.1038/sj.cdd.4401450
Ginet V, van de Looij Y, Petrenko V, Toulotte A, Kiss J, Hüppi PS, Sizonenko SV (2016) Lactoferrin during lactation reduces lipopolysaccharide-induced brain injury. BioFactors 42(3):323–336. https://doi.org/10.1002/biof.1278
Grabe DW (2007) Update on clinical practice recommendations and new therapeutic modalities for treating anemia in patients with chronic kidney disease. Am J Health Syst Pharm 64(13 Suppl 8):S8–S14. https://doi.org/10.2146/ajhp070182 Quiz S23–S25
Guo C, Yang ZH, Zhang S, Chai R, Xue H, Zhang YH, Li JY, Wang ZY (2017) Intranasal lactoferrin enhances α-secretase-dependent amyloid precursor protein processing via the ERK1/2-CREB and HIF-1α pathways in an Alzheimer’s disease mouse model. Neuropsychopharmacology 42(13):2504–2515. https://doi.org/10.1038/npp.2017.8
Haase VH (2010) Hypoxic regulation of erythropoiesis and iron metabolism. Am J Physiol Renal Physiol 299:F1–F13. https://doi.org/10.1152/ajprenal.00174.2010
Hand CC, Brines M (2011) Promises and pitfalls in erythopoietin-mediated tissue protection: are nonerythropoietic derivatives a way forward? J Investig Med 59:1073–1082. https://doi.org/10.2310/JIM.0b013e3181ed30bf
Holstein JH, Orth M, Scheuer C, Tami A, Becker SC, Garcia P, Histing T, Mörsdorf P, Klein M, Pohlemann T, Menger MD (2011) Erythropoietin stimulates bone formation, cell proliferation, and angiogenesis in a femoral segmental defect model in mice. Bone 49(5):1037–1045. https://doi.org/10.1016/j.bone.2011.08.004
Huang R, Han L, Li J, Ren F, Ke W, Jiang C, Pei Y (2009) Neuroprotection in a 6-hydroxydopamine-lesioned Parkinson model using lactoferrin-modified nanoparticles. J Gene Med 11(9):754–763. https://doi.org/10.1002/jgm.1361
Huang R, Ke W, Liu Y, Wu D, Feng L, Jiang C, Pei Y (2010) Gene therapy using lactoferrin-modified nanoparticles in a rotenone-induced chronic Parkinson model. J Neurol Sci 290(1–2):123–130. https://doi.org/10.1016/j.jns.2009.09.032
Ivan M, Kondo K, Yang H, Kim W, Valiando J, Ohh M, Salic A, Asara JM, Lane WS, Kaelin WG Jr (2001) HIFalpha targeted for VHL-mediated destruction by proline hydroxylation: implications for O2 sensing. Science 292(5516):464–468. https://doi.org/10.1126/science.1059817
Jang W, Park J, Shin KJ, Kim JS, Kim JS, Youn J, Cho JW, Oh E, Ahn JY, Oh KW, Kim HT (2014) Safety and efficacy of recombinant human erythropoietin treatment of non-motor symptoms in Parkinson’s disease. J Neurol Sci 337(1–2):47–54. https://doi.org/10.1016/j.jns.2013.11.015
Jaquet K, Krause K, Tawakol-Khodai M, Geidel S, Kuck KH (2002) Erythropoietin and VEGF exhibit equal angiogenic potential. Microvasc Res 64(2):326–333. https://doi.org/10.1006/mvre.2002.2426
Jia Z, Xue R, Ma S, Xu J, Guo S, Li S, Zhang E, Wang J, Yang J (2016) Erythropoietin attenuates the memory deficits in aging rats by rescuing the oxidative stress and inflammation and promoting BDNF releasing. Mol Neurobiol 53(8):5664–5670. https://doi.org/10.1007/s12035-015-9438-1
Jiang R, Lönnerdal B (2014) Transcriptomic profiling of intestinal epithelial cells in response to human, bovine and commercial bovine lactoferrins. Biometals 27(5):831–841. https://doi.org/10.1007/s10534-014-9746-3
Juul S (2002) Erythropoietin in the central nervous system, and its use to prevent hypoxic-ischemic brain damage. Acta Paediatr Suppl 91:36–42. https://doi.org/10.1111/j.1651-2227.2002.tb02904.x
Kamalinia G, Khodagholi F, Atyabi F, Amini M, Shaerzadeh F, Sharifzadeh M, Dinarvand R (2013) Enhanced brain delivery of deferasirox-lactoferrin conjugates for iron chelation therapy in neurodegenerative disorders: in vitro and in vivo studies. Mol Pharm 10(12):4418–4431. https://doi.org/10.1021/mp4002014
Kapitsinou PP, Liu Q, Unger TL, Rha J, Davidoff O, Keith B, Epstein JA, Moores SL, Erickson-Miller CL, Haase VH (2010) Hepatic HIF-2 regulates erythropoietic responses to hypoxia in renal anemia. Blood 116(16):3039–3048. https://doi.org/10.1182/blood-2010-02-270322
Kensler TW, Wakabayashi N, Biswal S (2007) Cell survival responses to environmental stresses via the Keap1-Nrf2-ARE pathway. Annu Rev Pharmacol Toxicol 47:89–116. https://doi.org/10.1146/annurev.pharmtox.46.120604.141046
Kim DJ, Kim YM, Yun YS, Ahn CW, Cha BS, Song YD, Lim SK, Kim KR, Hahn JS, Huh KB, Lee HC (2003) Therapeutic effect of recombinant human erythropoietin on anaemia with erythropoietin deficiency in diabetic patients. Diabet Med 20(8):661–664. https://doi.org/10.1046/j.1464-5491.2003.01012.x
Knowles HJ, Raval RR, Harris AL, Ratcliffe PJ (2003) Effect of ascorbate on the activity of hypoxia-inducible factor in cancer cells. Cancer Res 63:1764–1768
Kostevich VA, Sokolov AV, Kozlov SO, Vlasenko AY, Kolmakov NN, Zakharova ET, Vasilyev VB (2016) Functional link between ferroxidase activity of ceruloplasmin and protective effect of apo-lactoferrin: studying rats kept on a silver chloride diet. Biometals 29(4):691–704. https://doi.org/10.1007/s10534-016-9944-2
Kruzel ML, Actor JK, Radak Z, Bacsi A, Saavedra-Molina A, Boldogh I (2010) Lactoferrin decreases LPS-induced mitochondrial dysfunction in cultured cells and in animal endotoxemia model. Innate Immun 16(2):67–79. https://doi.org/10.1177/1753425909105317
Kuhrt D, Wojchowski DM (2015) Emerging EPO and EPO receptor regulators, and signal transducers. Blood 125:3536–3541. https://doi.org/10.1182/blood-2014-11-575357
Kumral A, Genc S, Ozer E, Yilmaz O, Gokmen N, Koroglu TF, Duman N, Genc K, Ozkan H (2006) Erythropoietin downregulates bax and DP5 proapoptotic gene expression in neonatal hypoxic-ischemic brain injury. Biol Neonat 89:205–210. https://doi.org/10.1159/000089951
Lappin TR, Maxwell AP, Johnston PG (2002) EPO’s alter ego: erythropoietin has multiple actions. Stem Cells 20:485–492. https://doi.org/10.1634/stemcells.20-6-485
Lee JW, Bae SH, Jeong JW, Kim SH, Kim KW (2004) Hypoxia-inducible factor (HIF-1)alpha: its protein stability and biological functions. Exp Mol Med 36:1–12. https://doi.org/10.1038/emm.2004.1
Lee ST, Chu K, Park JE, Jung KH, Jeon D, Lim JY, Lee SK, Kim M, Roh JK (2012) Erythropoietin improves memory function with reducing endothelial dysfunction and amyloid-beta burden in Alzheimer’s disease models. J Neurochem 120(1):115–124. https://doi.org/10.1111/j.1471-4159.2011.07534.x
Legrand D (2012) Lactoferrin, a key molecule in immune and inflammatory processes. Biochem Cell Biol 90(3):252–268. https://doi.org/10.1139/o11-056
Lewczuk P, Hasselblatt M, Kamrowski-Kruck H, Heyer A, Unzicker C, Sirén AL, Ehrenreich H (2000) Survival of hippocampal neurons in culture upon hypoxia: effect of erythropoietin. NeuroReport 11(16):3485–3488. https://doi.org/10.1097/00001756-200011090-00017
Li X, Gonias SL, Campana WM (2005) Schwann cells express erythropoietin receptor and represent a major target for Epo in peripheral nerve injury. Glia 51:254–265. https://doi.org/10.1002/glia.20202
Li W, Zhu S, Hu J (2015) Bone regeneration is promoted by orally administered bovine lactoferrin in a rabbit tibial distraction osteogenesis model. Clin Orthop Relat Res 473(7):2383–2393. https://doi.org/10.1007/s11999-015-4270-5
Lim J, Kim HI, Bang Y, Seol W, Choi HS, Choi HJ (2015) Hypoxia-inducible factor-1α upregulates tyrosine hydroxylase and dopamine transporter by nuclear receptor ERRγ in SH-SY5Y cells. NeuroReport 26(6):380–386. https://doi.org/10.1097/WNR.0000000000000356
Lin TY, Chiou SH, Chen M, Kuo CD (2005) Human lactoferrin exerts bi-directional actions on PC12 cell survival via ERK1/2 pathway. Biochem Biophys Res Commun 337(1):330–336. https://doi.org/10.1016/j.bbrc.2005.09.056
Lyons TE, Miller MS, Serena T, Sheehan P, Lavery L, Kirsner RS, Armstrong DG, Reese A, Yankee EW, Veves A (2007) Talactoferrin alfa, a recombinant human lactoferrin promotes healing of diabetic neuropathic ulcers: a phase 1/2 clinical study. Am J Surg 193(1):49–54. https://doi.org/10.1016/j.amjsurg.2006.07.010
Ma C, Cheng F, Wang X, Zhai C, Yue W, Lian Y, Wang Q (2016) Erythropoietin pathway: a potential target for the treatment of depression. Int J Mol Sci 17:677. https://doi.org/10.3390/ijms17050677
Marti HH, Bernaudin M, Petit E, Bauer C (2000) Neuroprotection and angiogenesis: dual role of erythropoietin in brain ischemia. News Physiol Sci 15:225–229. https://doi.org/10.1152/physiologyonline.2000.15.5.225
Masuda S, Okano M, Yamagishi K, Nagao M, Ueda M, Sasaki R (1994) A novel site of erythropoietin production. Oxygen-dependent production in cultured rat astrocytes. J Biol Chem 269:19488–19493
Mayeur S, Spahis S, Pouliot Y, Levy E (2016) Lactoferrin, a pleiotropic protein in health and disease. Antioxid Redox Signal 24(14):813–836. https://doi.org/10.1089/ars.2015.6458
Meloni BP, Tilbrook PA, Boulos S, Arthur PG, Knuckey NW (2006) Erythropoietin preconditioning in neuronal cultures: signaling, protection from in vitro ischemia, and proteomic analysis. J Neurosci Res 83(4):584–593. https://doi.org/10.1002/jnr.20755
Meng R, Zhu D, Bi Y, Yang D, Wang Y (2013) Erythropoietin inhibits gluconeogenesis and inflammation in the liver and improves glucose intolerance in high-fat diet-fed mice. PLoS ONE 8(1):e53557. https://doi.org/10.1371/journal.pone.0053557
Mikati MA, El Hokayem JA, El Sabban ME (2007) Effects of a single dose of erythropoietin on subsequent seizure susceptibility in rats exposed to acute hypoxia at P10. Epilepsia 48(1):175–181. https://doi.org/10.1111/j.1528-1167.2006.00900.x
Minnerup J, Heidrich J, Rogalewski A, Schäbitz WR, Wellmann J (2009) The efficacy of erythropoietin and its analogues in animal stroke models: a meta-analysis. Stroke 40(9):3113–3120. https://doi.org/10.1161/STROKEAHA.109.555789
Montesi M, Panseri S, Iafisco M, Adamiano A, Tampieri A (2015) Coupling hydroxyapatite nanocrystals with lactoferrin as a promising strategy to fine regulate bone homeostasis. PLoS ONE 10(7):e0132633. https://doi.org/10.1371/journal.pone.0132633
Morishita S, Tomita K, Ono T, Murakoshi M, Saito K, Sugiyama K, Nishino H, Kato H (2015) Lactoferrin attenuates fatty acid-induced lipotoxicity via Akt signaling in hepatocarcinoma cells. Biochem Cell Biol 93(6):566–573. https://doi.org/10.1139/bcb-2015-0014
Morishita S, Kawaguchi H, Ono T, Miura N, Murakoshi M, Sugiyama K, Kato H, Tanimoto A, Nishino H (2016) Enteric lactoferrin attenuates the development of high-fat and high-cholesterol diet-induced hypercholesterolemia and atherosclerosis in Microminipigs. Biosci Biotechnol Biochem 80(2):295–303. https://doi.org/10.1080/09168451.2015.1091713
Mulligan P, White NR, Monteleone G, Wang P, Wilson JW, Ohtsuka Y, Sanderson IR (2006) Breast milk lactoferrin regulates gene expression by binding bacterial DNA CpG motifs but not genomic DNA promoters in model intestinal cells. Pediatr Res 59(5):656–661. https://doi.org/10.1203/01.pdr.0000214958.80011.e1
Nagai A, Nakagawa E, Choi HB, Hatori K, Kobayashi S, Kim SU (2001) Erythropoietin and erythropoietin receptors in human CNS neurons, astrocytes, microglia, and oligodendrocytes grown in culture. J Neuropathol Exp Neurol 60:386–392. https://doi.org/10.1093/jnen/60.4.386
Nairz M, Sonnweber T, Schroll A, Theurl I, Weiss G (2012) The pleiotropic effects of erythropoietin in infection and inflammation. Microbes Infect 14:238–246. https://doi.org/10.1016/j.micinf.2011.10.005
Nakajima K, Kanno Y, Nakamura M, Gao XD, Kawamura A, Itoh F, Ishisaki A (2011) Bovine milk lactoferrin induces synthesis of the angiogenic factors VEGF and FGF2 in osteoblasts via the p44/p42 MAP kinase pathway. Biometals 24(5):847–856. https://doi.org/10.1007/s10534-011-9439-0
Nguyen DN, Jiang P, Stensballe A et al (2016) Bovine lactoferrin regulates cell survival, apoptosis and inflammation in intestinal epithelial cells and preterm pig intestine. J Proteom 139:95–102. https://doi.org/10.1016/j.jprot.2016.03.020
Norrby K (2004) Human apo-lactoferrin enhances angiogenesis mediated by vascular endothelial growth factor A in vivo. J Vasc Res 41(4):293–304. https://doi.org/10.1159/000078927
Ochoa TJ, Sizonenko SV (2016) Lactoferrin and prematurity: a promising milk protein? Biochem Cell Biol 95(1):22–30. https://doi.org/10.1139/bcb-2016-0066
Ono T, Murakoshi M, Suzuki N, Iida N, Ohdera M, Iigo M, Yoshida T, Sugiyama K, Nishino H (2010) Potent anti-obesity effect of enteric-coated lactoferrin: decrease in visceral fat accumulation in Japanese men and women with abdominal obesity after 8-week administration of enteric-coated lactoferrin tablets. Br J Nutr 104(11):1688–1695. https://doi.org/10.1017/S0007114510002734
Ono T, Fujisaki C, Ishihara Y, Ikoma K, Morishita S, Murakoshi M, Sugiyama K, Kato H, Miyashita K, Yoshida T, Nishino H (2013) Potent lipolytic activity of lactoferrin in mature adipocytes. Biosci Biotechnol Biochem 77(3):566–571. https://doi.org/10.1271/bbb.120817
Ono T, Murakoshi M, Suzuki N, Iida N, Ohdera M, Iigo M, Yoshida T, Sugiyama K, Nishino H (2015) Potent anti-obesity effect of enteric-coated lactoferrin: decrease in visceral fat accumulation in Japanese men and women with abdominal obesity after 8-week administration of enteric-coated lactoferrin tablets—CORRIGENDUM. Br J Nutr 114(1):159. https://doi.org/10.1017/S0007114515001853
Paesano R, Pietropaoli M, Gessani S, Valenti P (2009) The influence of lactoferrin, orally administered, on systemic iron homeostasis in pregnant women suffering of iron deficiency and iron deficiency anaemia. Biochimie 91(1):44–51. https://doi.org/10.1016/j.biochi.2008.06.004
Paesano R, Berlutti F, Pietropaoli M, Pantanella F, Pacifici E, Goolsbee W, Valenti P (2010) Lactoferrin efficacy versus ferrous sulfate in curing iron deficiency and iron deficiency anemia in pregnant women. Biometals 23(3):411–417. https://doi.org/10.1007/s10534-010-9335-z
Paesano R, Pacifici E, Benedetti S, Berlutti F, Frioni A, Polimeni A, Valenti P (2014) Safety and efficacy of lactoferrin versus ferrous sulphate in curing iron deficiency and iron deficiency anaemia in hereditary thrombophilia pregnant women: an interventional study. Biometals 27(5):999–1006. https://doi.org/10.1007/s10534-014-9723-x
Park Y-G, Moon J-H, Park S-Y (2014) Lactoferrin from bovine colostrum regulates prolyl hydroxylase 2 activity and prevents prion protein-mediated neuronal cell damage via cellular prion protein. Neuroscience 274:187–197. https://doi.org/10.1016/j.neuroscience.2014.05.030
Plzak L, Fried W, Jacobson L, Bethard W (1955) Demonstration of stimulation of erythropoiesis by plasma from anemic rats using Fe59. J Lab Clin Med 46:671–678
Puddu P, Valenti P, Gessani S (2009) Immunomodulatory effects of lactoferrin on antigen presenting cells. Biochimie 91:11–18. https://doi.org/10.1016/j.biochi.2008.05.005
Puddu P, Latorre D, Carollo M, Catizone A, Ricci G, Valenti P, Gessani S (2011) Bovine lactoferrin counteracts Toll-like receptor mediated activation signals in antigen presenting cells. PLoS ONE 6:e22504. https://doi.org/10.1371/journal.pone.0022504
Pulina MO, Sokolov AV, Zakharova ET, Kostevich VA, Vasilyev VB (2010) Effect of lactoferrin on consequences of acute experimental hemorrhagic anemia in rats. Bull Exp Biol Med 149(2):219–222. https://doi.org/10.1007/s10517-010-0911-6
Qi C, Xu M, Gan J, Yang X, Wu N, Song L, Yuan W, Liu Z (2014) Erythropoietin improves neurobehavior by reducing dopaminergic neuron loss in a 6-hydroxydopamine-induced rat model. Int J Mol Med 34(2):440–450. https://doi.org/10.3892/ijmm.2014.1810
Qi W, Shen Q, Zhang L, Han LP, Wang S (2016) Study on the inflammatory intervention of erythropoietin on NEC. Exp Ther Med 11(6):2221–2224. https://doi.org/10.3892/etm.2016.3199
Qin YJ, Zhang XL, Yu YQ, Bian XH, Dong SM (2013) Cardioprotective effect of erythropoietin on sepsis-induced myocardial injury in rats. World J Emerg Med 4(3):215–222. https://doi.org/10.5847/wjem.j.1920-8642.2013.03.011
Qiu Z, Strickland DK, Hyman BT, Rebeck GW (1999) Alpha2-macroglobulin enhances the clearance of endogenous soluble beta-amyloid peptide via low-density lipoprotein receptor-related protein in cortical neurons. J Neurochem 73(4):1393–1398. https://doi.org/10.1046/j.1471-4159.1999.0731393.x
Rankin EB, Biju MP, Liu Q, Unger TL, Rha J, Johnson RS, Simon MC, Keith B, Haase VH (2007) Hypoxia-inducible factor-2 (HIF-2) regulates hepatic erythropoietin in vivo. J Clin Invest 117(4):1068–1077. https://doi.org/10.1172/JCI30117
Rankin EB, Wu C, Khatri R, Wilson TL, Andersen R, Araldi E, Rankin AL, Yuan J, Kuo CJ, Schipani E, Giaccia AJ (2012) The HIF signaling pathway in osteoblasts directly modulates erythropoiesis through the production of EPO. Cell 149(1):63–74. https://doi.org/10.1016/j.cell.2012.01.051
Reissmann KR (1950) Studies on the mechanism of erythropoietic stimulation in parabiotic rats during hypoxia. Blood 5:372–380. https://doi.org/10.1182/blood-2015-12-686386
Ribatti D, Vacca A, Roccaro AM, Crivellato E, Presta M (2003) Erythropoietin as an angiogenic factor. Eur J Clin Invest 33(10):891–896. https://doi.org/10.1046/j.1365-2362.2003.01245.x
Rong R, Xijun X (2015) Erythropoietin pretreatment suppresses inflammation by activating the PI3K/Akt signaling pathway in myocardial ischemia-reperfusion injury. Exp Ther Med 10(2):413–418. https://doi.org/10.3892/etm.2015.2534
Rosa L, Cutone A, Lepanto MS, Paesano R, Valenti P (2017) Lactoferrin: a natural glycoprotein involved in iron and inflammatory homeostasis. Int J Mol Sci 18:1985. https://doi.org/10.3390/ijms18091985
Rousseau E, Michel PP, Hirsch EC (2013) The iron-binding protein lactoferrin protects vulnerable dopamine neurons from degeneration by preserving mitochondrial calcium homeostasis. Mol Pharmacol 84(6):888–898. https://doi.org/10.1124/mol.113.087965
Samygina VR, Sokolov AV, Bourenkov G, Petoukhov MV, Pulina MO, Zakharova ET, Vasilyev VB, Bartunik H, Svergun DI (2013) Ceruloplasmin: macromolecular assemblies with iron-containing acute phase proteins. PLoS ONE 8:e67145. https://doi.org/10.1371/journal.pone.0067145
Saray A, Ozakpinar R, Koc C, Serel S, Sen Z, Can Z (2003) Effect of chronic and short-term erythropoietin treatment on random flap survival in rats: an experimental study. Laryngoscope 113(1):85–99. https://doi.org/10.1097/00005537-200301000-00016
Semenza GL (2012) Hypoxia-inducible factors in physiology and medicine. Cell 148(3):399–408. https://doi.org/10.1016/j.cell.2012.01.021
Semenza GL, Wang GL (1992) A nuclear factor induced by hypoxia via de novo protein synthesis binds to the human erythropoietin gene enhancer at a site required for transcriptional activation. Mol Cell Biol 12(12):5447–5454. https://doi.org/10.1128/MCB.12.12.5447
Sifringer M, Genz K, Brait D, Brehmer F, Löber R, Weichelt U, Kaindl AM, Gerstner B, Felderhoff-Mueser U (2009) Erythropoietin attenuates hyperoxia-induced cell death by modulation of inflammatory mediators and matrix metalloproteinases. Dev Neurosci 31(5):394–402. https://doi.org/10.1159/000232557
Sifringer M, Brait D, Weichelt U, Zimmerman G, Endesfelder S, Brehmer F, von Haefen C, Friedman A, Soreq H, Bendix I, Gerstner B, Felderhoff-Mueser U (2010) Erythropoietin attenuates hyperoxia-induced oxidative stress in the developing rat brain. Brain Behav Immun 24(5):792–799. https://doi.org/10.1016/j.bbi.2009.08.010
Sirén AL, Ehrenreich H (2001) Erythropoietin–a novel concept for neuroprotection. Eur Arch Psychiatry Clin Neurosci 251(4):179–184. https://doi.org/10.1007/s004060170038
Sirén AL, Fratelli M, Brines M, Goemans C, Casagrande S, Lewczuk P, Keenan S, Gleiter C, Pasquali C, Capobianco A, Mennini T, Heumann R, Cerami A, Ehrenreich H, Ghezzi P (2001) Erythropoietin prevents neuronal apoptosis after cerebral ischemia and metabolic stress. Proc Natl Acad Sci USA 98(7):4044–4049. https://doi.org/10.1073/pnas.051606598
Sokolov AV, Solovyov KV, Kostevich VA, Chekanov AV, Pulina MO, Zakharova ET, Shavlovski MM, Panasenko OM, Vasilyev VB (2012) Protection of ceruloplasmin by lactoferrin against hydroxyl radicals is pH dependent. Biochem Cell Biol 90(3):397–404. https://doi.org/10.1139/o2012-004
Sokolov AV, Zakharova ET, Kostevich VA, Samygina VR, Vasilyev VB (2014) Lactoferrin, myeloperoxidase, and ceruloplasmin: complementary gearwheels cranking physiological and pathological processes. Biometals 27:815–828. https://doi.org/10.1007/s10534-014-9755-2
Somm E, Larvaron P, van de Looij Y, Toulotte A, Chatagner A, Faure M, Métairon S, Mansourian R, Raymond F, Gruetter R, Wang B, Sizonenko SV, Hüppi PS (2014) Protective effects of maternal nutritional supplementation with lactoferrin on growth and brain metabolism. Pediatr Res 75(1–1):51–61. https://doi.org/10.1038/pr.2013.199
Stoyanoff TR, Todaro JS, Aguirre MV, Zimmermann MC, Brandan NC (2014) Amelioration of lipopolysaccharide-induced acute kidney injury by erythropoietin: involvement of mitochondria-regulated apoptosis. Toxicology 318:13–21. https://doi.org/10.1016/j.tox.2014.01.011
Sun ZK, Yang HQ, Pan J, Zhen H, Wang ZQ, Chen SD, Ding JQ (2008) Protective effects of erythropoietin on tau phosphorylation induced by beta-amyloid. J Neurosci Res 86(13):3018–3027. https://doi.org/10.1002/jnr.21745
Sytkowski AJ (2011) The neurobiology of erythropoietin. Cell Mol Neurobiol 31:931–937. https://doi.org/10.1007/s10571-011-9695-0
Tamura A, Graham DI, McCulloch J, Teasdale GM (1981) Focal cerebral ischaemia in the rat: 1. description of technique and early neuropathological consequences following middle cerebral artery occlusion. J Cereb Blood Flow Metab 1(1):53–60. https://doi.org/10.1038/jcbfm.1981.6
Teng R, Gavrilova O, Suzuki N, Chanturiya T, Schimel D, Hugendubler L, Mammen S, Yver DR, Cushman SW, Mueller E, Yamamoto M, Hsu LL, Noguchi CT (2011) Disrupted erythropoietin signalling promotes obesity and alters hypothalamus proopiomelanocortin production. Nat Commun 2:520. https://doi.org/10.1038/ncomms1526
Togawa J, Nagase H, Tanaka K, Inamori M, Umezawa T, Nakajima A, Naito M, Sato S, Saito T, Sekihara H (2002) Lactoferrin reduces colitis in rats via modulation of the immune system and correction of cytokine imbalance. Am J Physiol Gastrointest Liver Physiol 283(1):G187–G195. https://doi.org/10.1152/ajpgi.00331.2001
Tramontano AF, Muniyappa R, Black AD, Blendea MC, Cohen I, Deng L, Sowers JR, Cutaia MV, El-Sherif N (2003) Erythropoietin protects cardiac myocytes from hypoxia-induced apoptosis through an Akt-dependent pathway. Biochem Biophys Res Commun 308(4):990–994. https://doi.org/10.1016/S0006-291X(03)01503-1
Valenti P, Antonini G (2005) Lactoferrin: an important host defence against microbial and viral attack. Cell Mol Life Sci 62:2576–2587. https://doi.org/10.1007/s00018-005-5372-0
van de Looij Y, Chatagner A, Quairiaux C, Gruetter R, Hüppi PS, Sizonenko SV (2014a) Multi-modal assessment of long-term erythropoietin treatment after neonatal hypoxic-ischemic injury in rat brain. PLoS ONE 9(4):e95643. https://doi.org/10.1371/journal.pone.0095643
van de Looij Y, Ginet V, Chatagner A, Toulotte A, Somm E, Hüppi PS, Sizonenko SV (2014b) Lactoferrin during lactation protects the immature hypoxic-ischemic rat brain. Ann Clin Transl Neurol 1(12):955–967. https://doi.org/10.1002/acn3.138
Vogel HJ (2012) Lactoferrin, a bird’s eye view. Biochem Cell Biol 90(3):233–244. https://doi.org/10.1139/o2012-016
Wang GL, Semenza GL (1995) Purification and characterization of hypoxia-inducible factor 1. J Biol Chem 270(3):1230–1237. https://doi.org/10.1074/jbc.270.3.1230
Wang J, Bi M, Liu H, Song N, Xie J (2015) The protective effect of lactoferrin on ventral mesencephalon neurons against MPP+ is not connected with its iron binding ability. Sci Rep 5:10729. https://doi.org/10.1038/srep10729
Xue YQ, Zhao LR, Guo WP, Duan WM (2007) Intrastriatal administration of erythropoietin protects dopaminergic neurons and improves neurobehavioral outcome in a rat model of Parkinson’s disease. Neuroscience 146(3):1245–1258. https://doi.org/10.1016/j.neuroscience.2007.02.004
Yatsiv I, Grigoriadis N, Simeonidou C, Stahel PF, Schmidt OI, Alexandrovitch AG, Tsenter J, Shohami F (2005) Erythropoietin is neuroprotective, improves functional recovery, and reduces neuronal apoptosis and inflammation in a rodent model of experimental closed head injury. FASEB J 12:1701–1703. https://doi.org/10.1096/fj.05-3907fje
Youssoufian H, Longmore G, Neumann D, Yoshimura A, Lodish H (1993) Structure, function, and activation of the erythropoietin receptor. Blood 81:2223
Yu Y, Shiou SR, Guo Y, Lu L, Westerhoff M, Sun J, Petrof EO, Claud EC (2013) Erythropoietin protects epithelial cells from excessive autophagy and apoptosis in experimental neonatal necrotizing enterocolitis. PLoS ONE 8(7):e69620. https://doi.org/10.1371/journal.pone.0069620
Yuan RR, Maeda Y, Li W, Lu W, Cook S, Dowling P (2008) Erythropoietin: a potent inducer of peripheral immuno/inflammatory modulation in autoimmune EAE. PLoS ONE 3(4):e1924. https://doi.org/10.1371/journal.pone.0001924
Zakharova ET, Shavlovski MM, Bass MG, Gridasova AA, Pulina MO, De Filippis V, Beltramini M, Di Muro P, Salvato B, Fontana A, Vasilyev VB, Gaitskhoki VS (2000) Interaction of lactoferrin with ceruloplasmin. Arch Biochem Biophys 374:222–228. https://doi.org/10.1006/abbi.1999.1559
Zakharova ET, Sokolov AV, Kostevich VA, Vasilyev VB (2012) Human apo-lactoferrin as a physiological mimetic of hypoxia stabilizes hypoxia-inducible factor-1 alpha. Biometals 25:1247–1259. https://doi.org/10.1007/s10534-012-9586-y
Zenkov NK, Kozhin PM, Chechushkov AV, Martinovich GG, Kandalintseva NV, Menshchikova EB (2017) Mazes of Nrf2 regulation. Biochemistry 82(5):556–564. https://doi.org/10.1134/S0006297917050030
Zhang T, Wang Y, Ban R, Tong L, Qiao H, Lao H, Zhao H, Jiang X, Sun X, Zhang F (2012a) Oral administration of lactoferrin attenuates intestinal ischemia-reperfusion injury in rats. Eur Surg Res 49(2):99–106. https://doi.org/10.1159/000342633
Zhang X, Li QY, Xiao BG (2012b) Anti-inflammatory effect of erythropoietin therapy on experimental autoimmune encephalomyelitis. Int J Neurosci 122(5):255–262. https://doi.org/10.3109/00207454.2011.648761
Zimecki M, Artym J, Chodaczek G, Kocieba M, Kuryszko J, Houszka M, Kruzel ML (2007a) Immunoregulatory function of lactoferrin in immunosuppressed and autoimmune animals. Postepy Hig Med Dosw 61:283–287
Zimecki M, Kocieba M, Chodaczek G, Houszka M, Kruzel ML (2007b) Lactoferrin ameliorates symptoms of experimental encephalomyelitis in Lewis rats. J Neuroimmunol 182(1–2):160–166. https://doi.org/10.1016/j.jneuroim.2006.10.008
Acknowledgements
The study was supported by RFBR Grant 18-015-00241 and Grants MK-5874.2018.4, MD-5133.2018.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zakharova, E.T., Sokolov, A.V., Pavlichenko, N.N. et al. Erythropoietin and Nrf2: key factors in the neuroprotection provided by apo-lactoferrin. Biometals 31, 425–443 (2018). https://doi.org/10.1007/s10534-018-0111-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10534-018-0111-9